Introduction
Rationale
Objectives
Methods
Ethics statement
Study design
Eligibility criteria
Information sources/search
Study selection
Data collection process and data items
Risk of bias assessment
Results
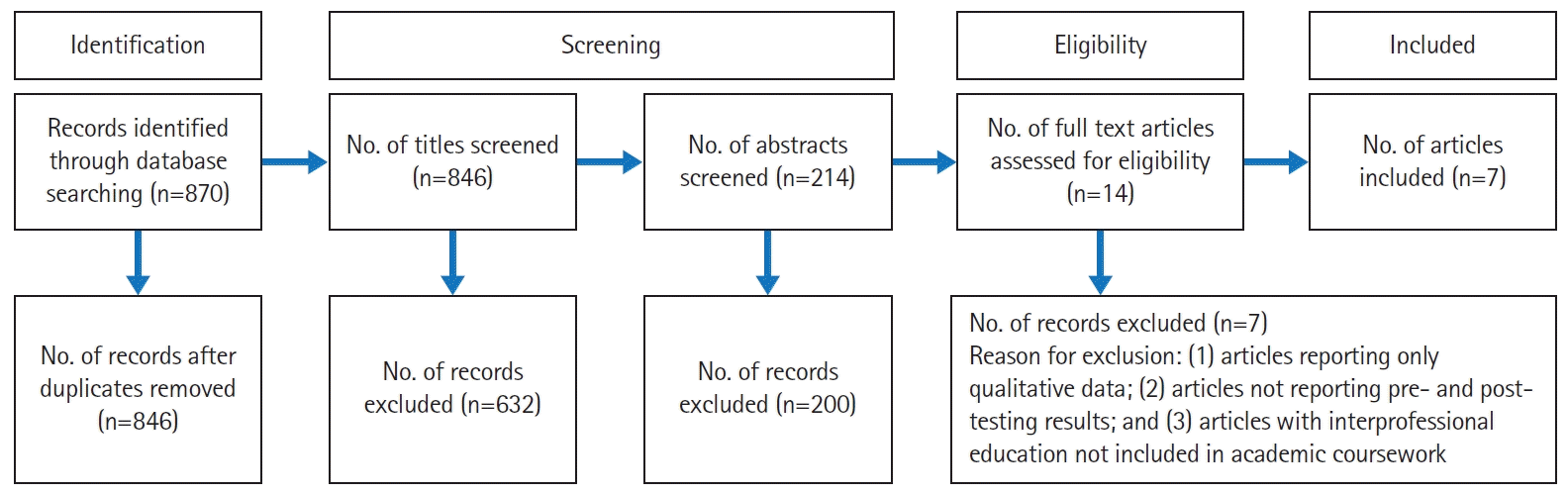
Study selection
Study characteristics
Table 1.
| References | Student type (no. of participants) | Intervention | Outcome measures | Results |
|---|---|---|---|---|
| Cino et al. [5] (2018) | Dental hygiene (10); nursing (37); medical laboratory technician (28) | Students participated in a questionnaire determining self-efficacy for IPE before and after participation in an interprofessional ethics activity. | Self-efficacy for interprofessional learning | Six questions yielded significant improvements in self-efficacy for IPE learning |
| Teamwork (P=0.023) | ||||
| Multiple professions roles (P=0.031) | ||||
| Patient benefits of team care (P=0.043) | ||||
| Objectives of interprofessional learning (P=0.019) | ||||
| Quality of interprofessional team work (P=0.008) | ||||
| Interprofessional learning goal achievement (P=0.012) | ||||
| Leithead et al. [8] (2018) | Medical (70 IPT/43 RIPLS); undergraduate nursing (40 IPT/27 RIPLS); nurse anesthesia (42 IPT/29 RIPLS) | Students participated in IPE involving a high-fidelity simulation of the operating room over the course of 3 years. | IPT | Significant improvement overall was reported on IPT following the intervention (P<0.001) |
| RIPLS | Significant improvement overall was reported on RIPLS following the intervention (P<0.001) | |||
| Paige et al. [9] (2014) | Nursing (18); certified registered nurse anesthetist (20); medical (28) | Students participated in IPE involving a high-fidelity simulation of the operating room. | Likert-type items measuring self-efficacy and team performance | Eleven out of the 15 items showed significant improvement following the intervention including items related to individual task responsibilities, communication, and teamwork (P<0.001) |
| Pinto et al. [10] (2018] | Medical (70); occupational therapy (34); physical therapy (28); physician assistant (12); nursing (44) | Students completed a stroke simulation activity along with pre- and post-test questionnaires regarding the IPE. | IPE collaborative competency self-assessment tool | Following the intervention, overall results indicated significant improvement in interprofessional values and interprofessional interactions |
| Values domain (P<0.0001) | ||||
| Interactions domain (P=0.0003) | ||||
| Renschler et al. [3] (2016) | Osteopathic medicine (1st 19/2nd 21); nursing (1st 30/2nd 41); health science (1st 7/2nd 6); speech-language (1st 18/2nd 17); athletic training (1st 4/2nd 0); exercise sciences (1st 3/2nd 0) | Student participation in an interprofessional geriatric home visit program for a 1-sem versus a 2-sem IPE activity. | Attitudes Towards Health Care Teams Scale | 1st sem: led to significant improvements following the intervention (P=0.00) |
| 2nd sem: showed no significant improvements | ||||
| Team Skills Scale | 1st sem: showed significant improvement in team skills (P=0.00) | |||
| 2nd sem: reported significant improvements (P=0.01) | ||||
| - | Between-group comparisons showed more significant improvements in the 1-sem program than in the 2-sem program (P<0.05) | |||
| Ruebling et al. [11] (2014) | Athletic training (15); clinical laboratory (9); cytotechnology (2); health information management (2); investigative medical sciences (15); nuclear medicine (4); nursing (115); nutrition and dietetics (18); occupational therapy (20); physical therapy (83); Radiation therapy (8) | Questionnaire completed by students who participated in a sem-long IPE course in interdisciplinary teams. | RIPLS | Significant improvements after the introductory IPE course (P=0.05) |
| Significant improvements after the IPE course (P<0.001) | ||||
| University of West England Interprofessional Questionnaire | Improvements were noted after the IPE course (P=0.01) | |||
| Significant improvements after the IPE course (P<0.001) | ||||
| Stubbs et al. [12] (2017) | Dentistry; dietetics; divinity; medicine; nursing; occupational therapy; pharmacy; public health; social work; speech and hearing science (30) | Students completed a questionnaire before the IPE program, after IPE training and upon completion of the IPE consisting of didactic and community service work. | ISVS | The ISVS contained 3 sub-scales: SPA, CWO, VWO |
| SPA: After completion significant improvements were reported (P=0.005) | ||||
| CWO: After completion significant improvements were reported (P<0.0001) | ||||
| VWO: After completion significant improvements were reported (P=0.001) |
IPE, interprofessional education; IPT, Interprofessional Teamwork Scale; RIPLS, Readiness for Interprofessional Learning Scale; Sem, semester; ISVS, Interprofessional Socialization & Valuing Scale. SPA, self-perceived ability to work with others; CWO, comfort working with others; VWO, value of working with others.
Risk of bias
Table 2.
| Quality assessment tool | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | Total |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Cino et al. [5] | Yes | No | NR | NR | Yes | Yes | Yes | No | Yes | Yes | No | Yes | 7 |
| Leithead et al. [8] | Yes | Yes | Yes | No | Yes | No | Yes | No | Yes | Yes | Yes | Yes | 9 |
| Paige et al. [9] | Yes | No | Yes | No | No | Yes | Yes | No | Yes | Yes | Yes | Yes | 8 |
| Pinto et al. [10] | Yes | Yes | Yes | Yes | Yes | No | Yes | No | Yes | Yes | No | Yes | 9 |
| Renschler et al. [3] | Yes | Yes | Yes | Yes | Yes | Yes | Yes | Yes | NR | Yes | No | Yes | 10 |
| Ruebling et al. [11] | Yes | Yes | Yes | Yes | Yes | Yes | Yes | No | No | Yes | No | Yes | 9 |
| Stubbs et al. [12] | Yes | No | Yes | Yes | No | Yes | Yes | No | Yes | Yes | Yes | Yes | 9 |
Criteria: 1: study question; 2: eligibility criteria and study population; 3: study participants representative of clinical populations of interest; 4: all eligible participants enrolled; 5: sample size; 6: intervention clearly described; 7: outcome measures clearly described, valid, and reliable; 8: blinding of outcome assessors; 9: follow-up rate; 10: statistical analysis; 11: multiple outcome measures; 12: group-level interventions and individual-level outcome efforts.
NR, not reported.




 PDF
PDF Citation
Citation Print
Print




 XML Download
XML Download