Abstract
Objectives
An association between dietary patterns and mental health in children has been suggested in a series of studies, yet detailed analyses of dietary patterns and their effects on ADHD (attention deficit hyperactivity disorder) are limited.
Methods
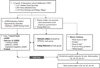
We included 4569 children who had dietary intake data as part of the CHEER (Children's Health and Environmental Research) study conducted nationwide from 2005 to 2010. We assessed ADHD (Attention Deficit Hyperactivity Disorder) by the DuPaul's ADHD Rating Scales and dietary intake by a semi-quantitative food frequency questionnaire. Using intake data, we constructed five dietary patterns: “Plant foods & fish,” “Sweets,” “Meat & fish,” “Fruits & dairy products,” and “Wheat based.”
Results
The overall proportion of ADHD was 12.3%. Boys (17.8%) showed a higher rate of ADHD than girls (6.5%). The total intake of calories (85 kcal) and plant fat (2g) in the ADHD group was significantly higher than that of the normal group. ADHD was significantly negatively associated with dietary habits such as having breakfast and meal frequency, and positively associated with eating speed, unbalanced diet, overeating, and rice consumption. Regarding dietary patterns, the “Sweets” category was relevant to high ADHD risk (OR 1.59, 95% CI: 1.18, 2.15 for Q5 vs. Q1) in a linear relationship. An inverse, non-linear association was found between “Fruits & dairy products” and ADHD (OR 0.55, 95% CI: 0.39, 0.76 for Q4 vs. Q1).
Conclusions
Our study confirms both positive and negative associations between diet and ADHD in elementary school age children. Moreover, linear or nonlinear associations between diet and ADHD draw attention to the possible threshold role of nutrients. Further studies may consider characteristics of diet in more detail to develop better intervention or management in terms of diet and health.
Figures and Tables
Table 2
Percentage of children who diagnosed with attention deficit hyperactivity disorder (ADHD) and the subtypes of ADHD

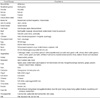
Table 6
Factor loadings1) for the five dietary patterns derived from semi-food frequency questionnaire (SFFQ)

References
1. Sarris J, Kean J, Schweitzer I, Lake J. Complementary medicines (herbal and nutritional products) in the treatment of Attention Deficit Hyperactivity Disorder (ADHD): A systematic review of the evidence. Complement Ther Med. 2011; 19(4):216–227.

2. Korean Academy of Child and Adolescent Psychiatry. The prevalence of ADHD in Korea [internet]. Korean Academy of Child and Adolescent Psychiatry;2017. cited 2018 Jul 12. Available from: http://adhd.or.kr/adhd/adhd02.php.
3. Heilskov Rytter MJ, Andersen LB, Houmann T, Bilenberg N, Hvolby A, Molgaard C. Diet in the treatment of ADHD in children: a systematic review of the literature. Nord J Psychiatry. 2015; 69(1):1–18.
4. Rowland AS, Lesesne CA, Abramowitz AJ. The epidemiology of attention-deficit/hyperactivity disorder (ADHD): a public health view. Ment Retard Dev Disabil Res Rev. 2002; 8(3):162–170.

5. Sung HS. Our elementary education. In; to understand children who have excessive distraction. Atten Defic Hyperact Disord. 2005; 3:38–39.
6. Song MR, Ha EH. The effects of children's executive function impairments and ADHD symptoms on self-directed learning capability. Korean J Play Ther. 2014; 17(2):193–207.
7. Kim SY. Attentional functions and dysfunctions in ADHD. Korean J Cogn Biol Psychol. 2014; 26(2):67–94.
8. Koo HJ, Choi JS. Language and cognitive development of preschool children from multicultural families and mono-Korean families in rural areas. Korean J Early Child Educ. 2012; 32(4):115–136.
9. Lee JR, Jae KS, Yoon CY. ADHD and substance abuse. Korean J East West Sci. 2004; 7(1):151–166.
10. Chen JR, Hsu SF, Hsu CD, Hwang LH, Yang SC. Dietary patterns and blood fatty acid composition in children with attention-deficit hyperactivity disorder in Taiwan. J Nutr Biochem. 2004; 15(8):467–472.

11. Kim HY, Choi EY, Kong MR. A study on the correlation between symptoms of ADHD, problem behaviors and emotional regulation ability of adolescents. J Spec Educ Rehabil Sci. 2013; 52(4):339–358.
12. Kwon HJ, Ha M, Kim BN, Lim MH. Harmful environmental factors leading to attention-deficit hyperactivity disorder. J Korean Acad Child Adolesc Psychiatry. 2016; 27(4):267–277.

13. Landrigan PJ, Schechter CB, Lipton JM, Fahs MC, Schwartz J. Environmental pollutants and disease in American children: estimates of morbidity, mortality, and costs for lead poisoning, asthma, cancer, and developmental disabilities. Environ Health Perspect. 2002; 110(7):721–728.

14. Choi WY. A study on regulation of mobile phone radiation: Necessity and content. J Leg Stud. 2013; 21(2):499–527.
15. Choi JO. Influence of youth internet fame addiction on ADHD and academic achievement: Focusing on elementary school students in Seoul, Incheon, and Gyeonggi region. J Korea Inst Youth Facil Environ. 2014; 12(2):19–28.
16. Han JY, Kim HJ, Ha MN, Paik KC, Lim MH, Lee SG. The effects of prenatal exposure to alcohol and environmental tobacco smoke on risk for ADHD: A large population-based study. Psychiatry Res. 2015; 225(1-2):164–168.

17. Mattes JA. The Feingold diet: a current reappraisal. J Learn Disabil. 1983; 16(6):319–323.
18. Kim WK, Cho SS. Sugar and cognitive performance. J Nutr Health. 2007; 40(sup):50–65.
19. Chung SH. Sugar and children's behavior. J Nonviol. 2010; 4:121–132.
20. Millichap JG, Yee MM. The diet factor in attention-deficit/hyperactivity disorder. Pediatrics. 2012; 129(2):330–337.

21. Kim KM, Lim MH, Kwon HJ, Yoo SJ, Kim EJ, Kim JW. Associations between attention-deficit/hyperactivity disorder symptoms and dietary habits in elementary school children. Appetite. 2018; 127(1):274–279.

22. Howard AL, Robinson M, Smith GJ, Ambrosini GL, Piek JP, Oddy WH. ADHD is associated with a "Western" dietary pattern in adolescents. J Atten Disord. 2011; 15(5):403–411.

23. Woo HD, Kim DW, Hong YS, Kim YM, Seo JH, Choe BM. Dietary patterns in children with Attention Deficit/Hyperactivity Disorder (ADHD). Nutrients. 2014; 6(4):1539–1553.

24. Azadbakht L, Esmaillzadeh A. Dietary patterns and attention deficit hyperactivity disorder among Iranian children. Nutrition. 2012; 28(3):242–249.

25. Kwon HJ. Korean environmental health survey for children. Ministry of Environment. National Institute of Environmental Research;2010 Report No. VI.
26. Shin MS, Cho SJ, Chun SY, Hong KE. A study of the development and standardization of ADHD diagnostic system. J Child Adolesc Psychiatry. 2000; 11(1):91–99.
27. Lim Y, Oh SY. Development of a semi-quantitative food questionnaire for pre-school children in Korea. Korean J Community Nutr. 2002; 7(1):58–66.
28. Connolly A, Vance A. Psychosocial factors associated with parent and teacher reports of aggression in children and adolescents with attention deficit hyperactivity disorder. Aust New Zealand J Psychiatry. 2010; 44(7):667–675.

29. Gungor S, Celiloglu OS, Raif SG, Ozcan OO, Selimoglu MA. Malnutrition and obesity in children with ADHD. J Atten Disord. 2016; 20(8):647–652.

30. Ptacek R, Kuzelova H, Stefano GB, Raboch J, Sadkova T, Goetz M. Disruptive patterns of eating behaviors and associated lifestyles in males with ADHD. Med Sci Monit. 2014; 20:608–613.

31. Durá-Travé T, Gallinas-Victoriano F. Caloric and nutrient intake in children with attention deficit hyperactivity disorder treated with extended-release methylphenidate: analysis of a cross-sectional nutrition survey. JRSM Open. 2014; 5(2):2042533313517690.

32. Cho SC, Kim BN, Kim JW, Rohde LA, Hwang JW, Chung DS. Full syndrome and subthreshold attention-deficit/ hyperactivity disorder in a Korean community sample: comorbidity and temperament findings. Eur Child Adolesc Psychiatry. 2009; 18(7):447–457.
33. Kim DW, Lee JE, Jung WC, Nam KC, Bang YW, Kim SJ. Cross sectional study on the prevalence of attention deficit hyperactivity disorder and associated factors among elementary school students living nearby Shihwa-Banwol industrial complex. Korean J Occup Environ Med. 2012; 24(3):252–262.

34. Pastor P, Reuben C, Duran C, Hawkins L. Association between diagnosed ADHD and selected characteristics among children aged 4-17 years: United States, 2011-2013. NCHS Data Brief. 2015; 4(5):4–17.
35. Han JY, Kim HJ, Ha MN, Paik KC, Lim MH, Lee SG. The effects of prenatal exposure to alcohol and environmental tobacco smoke on risk for ADHD: A large population-based study. Psychiatry Res. 2015; 225(1-2):164–168.

36. Choi JY, Lee SS. Relation between dietary habit and nutrition knowledge, and Attention Deficit Hyperactivity Disorder (ADHD) in the middle school students in Seoul. Korean J Nutr. 2009; 42(8):682–690.

37. Jang CB, Kim HY. The relationship between attention deficit hyperactivity disorder, dietary habit and caffeine intake in uppergrade elementary school children. Korean J Nutr. 2012; 45(6):522–530.

38. Reinblatt SP, Mahone EM, Tanofsky Kraff M, Lee Winn AE, Yenokyan G, Leoutsakos JMS. Pediatric loss of control eating syndrome: Association with attention deficit/hyperactivity disorder and impulsivity. Int J Eat Disord. 2015; 48(6):580–588.
39. Merkt J, Gawrilow C. Health, dietary habits, and achievement motivation in college students with self-reported ADHD diagnosis. J Atten Disord. 2016; 20(9):727–740.





 PDF
PDF ePub
ePub Citation
Citation Print
Print









 XML Download
XML Download