Abstract
Purpose
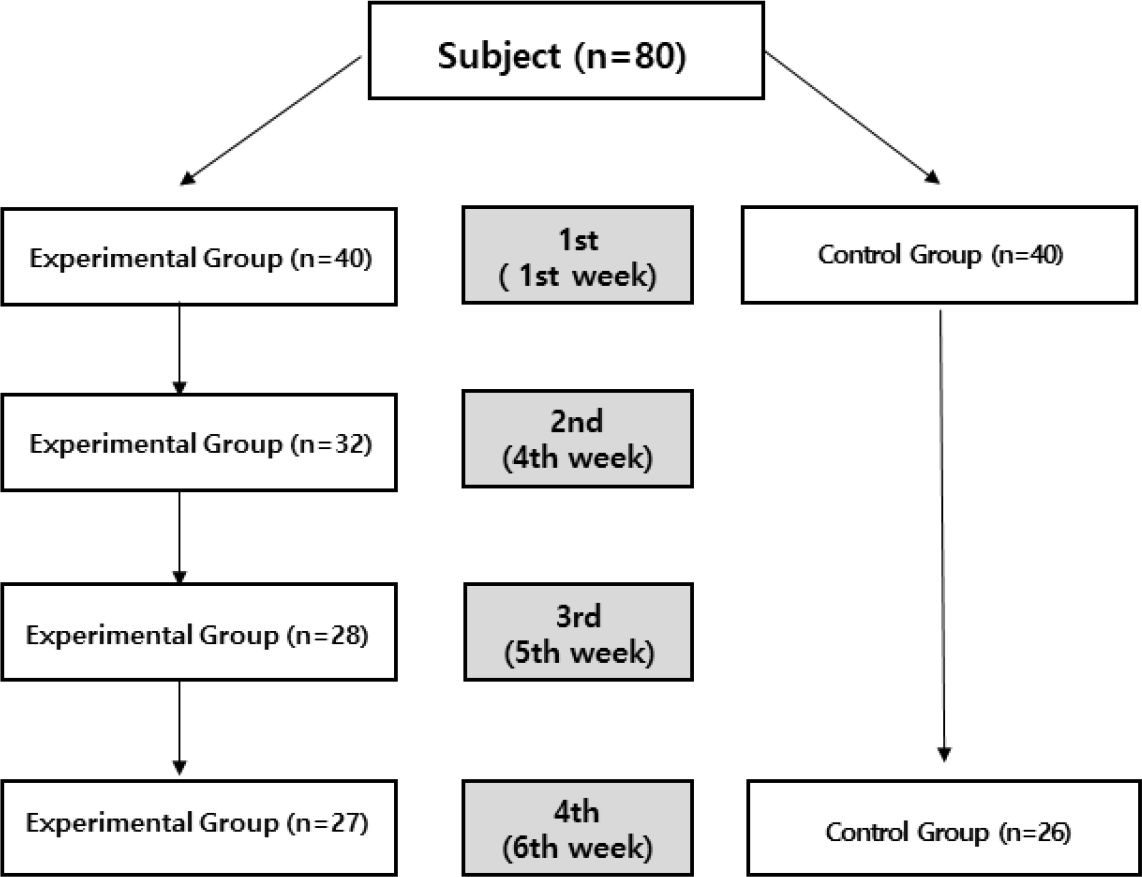
Changes in eating habits and malnutrition due to dysphagia are important health problems for older adults. This study investigated the effects of an educational program aimed at improving diet quality in community-dwelling older adults at risk for dysphagia in South Korea. Methods: We assessed 27 individuals in the experimental group and 26 individuals in the control group between September and October 2015. All participants were aged 65 years or older and were at risk for dysphagia. A combined diet and exercise program was applied to the experimental group (n=27) for six weeks. We examined changes in participants' eating habits and their knowledge and attitudes concerning dysphagia risk. The nutrition intake of all participants was measured before and after the intervention using 24-hr dietary recall. Results: There was a significant increase in knowledge of dysphagia risk in the experimental group, with scores increasing from 3.7 to 7.1, out of 10 points (p<0.001). There were also significant improvements in eating habits after the intervention in the experimental group, with scores increasing from 21.9 to 28.3, out of 36 points (p<0.001). The attitude score of participants in the experimental group increased significantly, from 15.2 to 16.7, out of 20 points (p=0.016). Conclusion: Developing educational programs can help older adults living in the community lead a healthier lifestyle and improve their ability to manage their diet.
Go to : 
References
1. Statistics Korea. Report of older adults statistics in 2017. Daejeon: Statistics Korea;2017.
2. Miura H, Kariyasu M, Yamasaki K, Arai Y. Evaluation of chewing and swallowing disorders among frail community-dwelling elderly individuals. J Oral Rehabil. 2007; 34(6):422–427.

3. Roy N, Stemple J, Merrill RM, Thomas L. Dysphagia in the elderly: preliminary evidence of prevalence, risk factors, and socioemotional effects. Ann Otol Rhinol Laryngol. 2007; 116(11):858–865.

4. Chen PH, Golub JS, Hapner ER, Johns MM 3rd. Prevalence of perceived dysphagia and quality-of-life impairment in a geriatric population. Dysphagia. 2009; 24(1):1–6.
5. Holland G, Jayasekeran V, Pendleton N, Horan M, Jones M, Hamdy S. Prevalence and symptom profiling of oropharyngeal dysphagia in a community dwelling of an elderly population: a self-reporting questionnaire survey. Dis Esophagus. 2011; 24(7):476–480.

6. Ministry of Health and Welfare, Korea Centers for Disease Control and Prevention. Korea Health Statistics 2012: Korea National Health and Nutrition Examination Survey (KNHANES V-3). Cheongju: Korea Centers for Disease Control and Prevention;2013.
7. Won YS, Kim JH, Kim SK. Relationship of subjective oral health status to subjective oral symptoms for the elderly in some Seoul area. J Dent Hyg Sci. 2009; 9(4):375–380.
8. Lee SM, Cho EP, Hwang YS, Kang BW. The change of oral function before and after practicing program for oral function improving. J Dent Hyg Sci. 2011; 11(6):497–503.
9. Yun OJ, Lee YH. The effect of singing intervention for women elderly with dysphagia risk. Korean J Adult Nurs. 2012; 24(4):380–389.

10. Bang HL, Park YH. The effect of an exercise-based swallowing training program for nursing home residents with stroke. J Muscle Joint Health. 2014; 21(2):85–96.

11. Fukada J, Kamakura Y, Manzai T, Kitaike T. Development of dysphagia risk screening system for elderly persons. Jpn J Dysphagia Rehabil. 2006; 10(1):31–42.
12. Choi YH. Relationship between number of residual teeth and masticatory function [dissertation]. Cheonnan: Dankook university;2008.
13. Kang JH, Park RY, Lee SJ, Kim JY, Yoon SR, Jung KI. The effect of bedside exercise program on stroke patients with dysphagia. Ann Rehabil Med. 2012; 36(4):512–520.

14. Turley R, Cohen S. Impact of voice and swallowing problems in the elderly. Otolaryngol Head Neck Surg. 2009; 140(1):33–36.

15. Cohen J. Statistical power analysis for the behavioral sciences. Cambridge (MA): Academic press;2013.
16. Kim YJ, Choi YH, Kim JY, Lee HK. The effect of orophysical exercise for the elderly on oral function and nutrient intake. J Korean Acad Oral Health. 2011; 35(4):414–422.
17. Sura L, Madhavan A, Carnaby G, Crary MA. Dysphagia in the elderly: management and nutritional considerations. Clin Interv Aging. 2012; 7:287–298.
18. Yang SO, Jeong G, Kim SJ, Kim K, Lee SH, Saung S, Baik S. The effects of oral function improving exercise on the UWS, oral function and OHIP in elderly. J Korean Public Health Nurs. 2012; 26(3):478–490.

19. Ministry of Health and Welfare. Demonstration project of hub-health centers' health promotion programs for elderly people. Seoul: Ministry of Health and Welfare;2007.
Go to : 
 | Fig. 2.Contents of the educational program for improving the dietary quality: Dietary guide and exercise guide |
Table 1.
Schedule of the educational program for improving the dietary quality
Table 2.
General character of the respondents before program (n (%) or mean ± SD)
Table 3.
The knowledge1) change between before and after the educational program1) (n (%) or mean ± SD)
Table 4.
The change of eating habits related to chewing and swallowing between before and after the educational program1) (mean ± SD)
Table 5.
The change of the attitude related to chewing and swallowing between before and after the educational program1) (mean ± SD)
Table 6.
The change of dietary consumption between before and after educational program1) (mean ± SD)




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download