Abstract
Acute ruptures of flexor tendons in patients with distal radius fractures are very rare complications. The majority of reported cases, flexor tendon rupture associated with distal radius fracture, is chronic flexor tendon ruptures, which are caused by implants for fixation or rough surfaces of malunited distal radius. We experienced an unusual case of an acute rupture of the flexor digitorum profundus tendon in a patient with a distal radius fracture, in addition to providing an auxiliary review of the literature.
References
1. Soong M, van Leerdam R, Guitton TG, Got C, Katarincic J, Ring D. Fracture of the distal radius: risk factors for complications after locked volar plate fixation. J Hand Surg Am. 2011; 36:3–9.

2. Kato N, Nemoto K, Arino H, Ichikawa T, Fujikawa K. Ruptures of flexor tendons at the wrist as a complication of fracture of the distal radius. Scand J Plast Reconstr Surg Hand Surg. 2002; 36:245–8.

3. McMaster PE. Late ruptures of extensor and flexor pollicis longus tendons following Colles' fracture. J Bone Joint Surg Am. 1932; 14:93–101.
4. Bonatz E, Kramer TD, Masear VR. Rupture of the extensor pollicis longus tendon. Am J Orthop (Belle Mead NJ). 1996; 25:118–22.
5. Drobetz H, Kutscha-Lissberg E. Osteosynthesis of distal radial fractures with a volar locking screw plate system. Int Orthop. 2003; 27:1–6.

6. Roberts JO, Regan PJ, Roberts AH. Rupture of flexor pollicis longus as a complication of Colles' fracture: a case report. J Hand Surg Br. 1990; 15:370–2.

7. Vaughan-Jackson OJ. Rheumatoid hand deformities considered in the light of tendon imbalance. J Bone Joint Surg Br. 1962; 44:764–75.
8. Bell JS, Wollstein R, Citron ND. Rupture of flexor pollicis longus tendon: a complication of volar plating of the distal radius. J Bone Joint Surg Br. 1998; 80:225–6.
Fig. 1.
(A) Initial radiographs of the wrist showing a comminuted and displaced distal radius fracture with dorsal angulation and ulnar styloid process fracture. Note the bony beak at the proximal fractured end and the obvious deformity of the wrist. (B) Computed tomography scan showing simple intra-articular and simple metaphysic fractures of the distal radius.The bony beak at the proximal fractured end is prominently shown (white arrow).
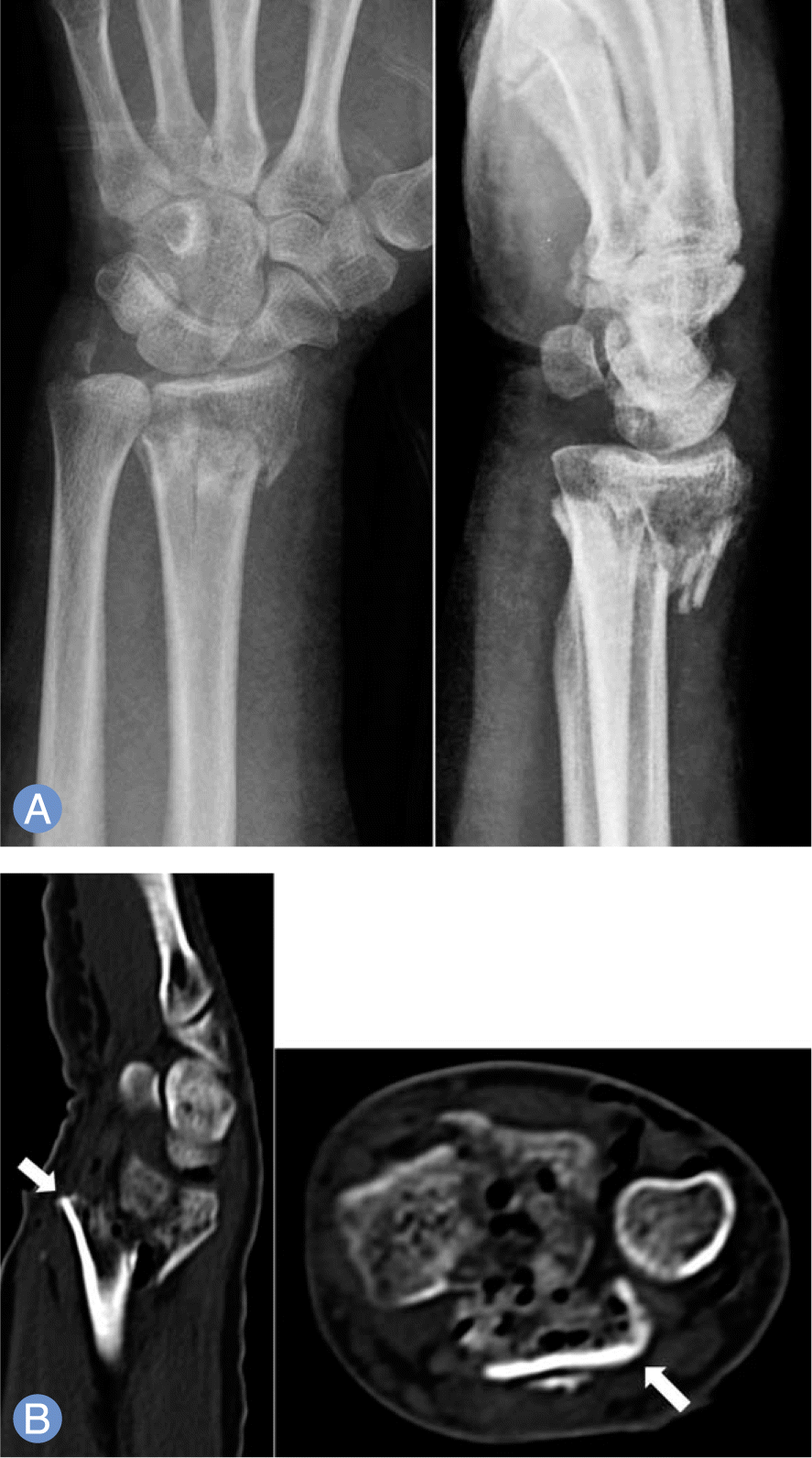
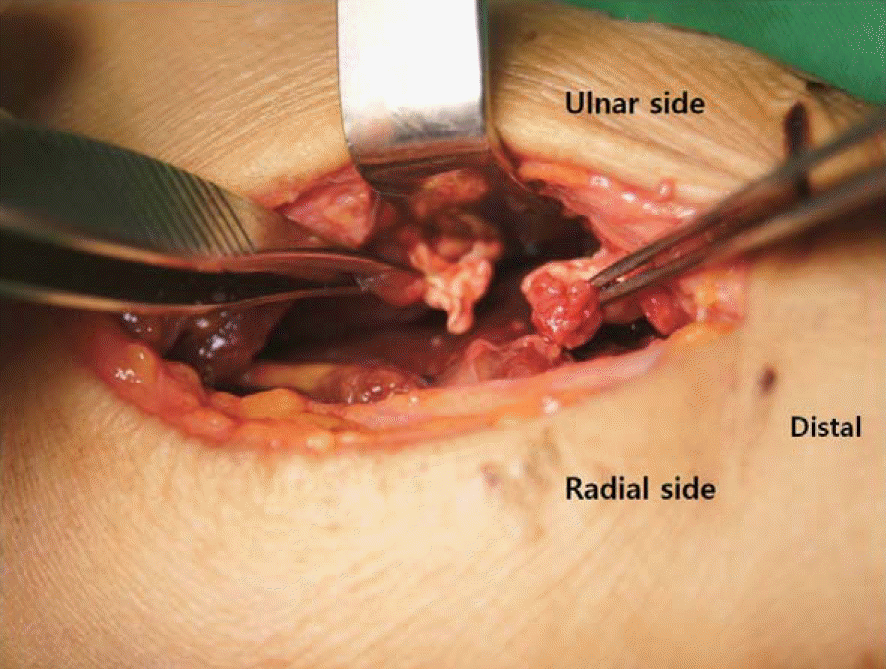
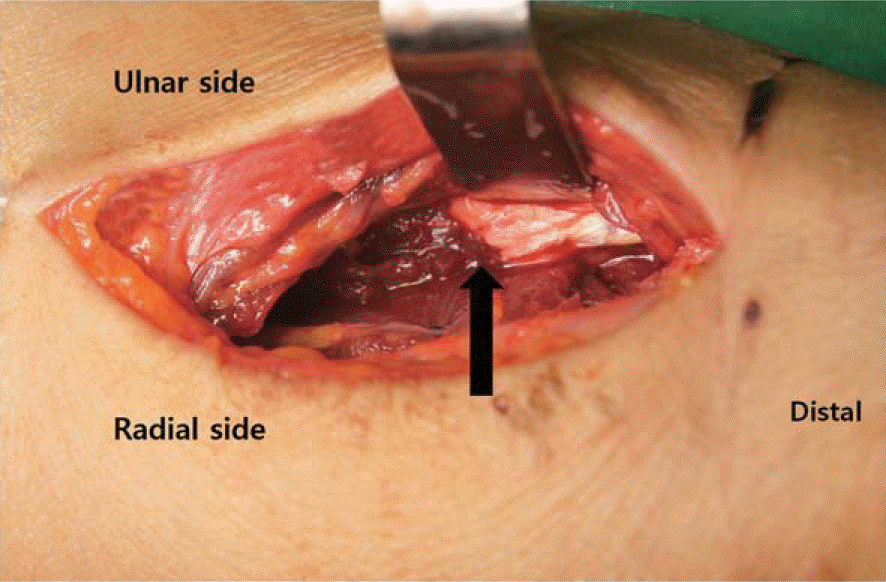
Fig. 2.
Intraoperative gross picture showing ruptured third flexor digitorum profundus tendon at the musculotendinous junction in flexor tendon zone V.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download