Abstract
Preservation of the recurrent laryngeal nerve (RLN) is a priority for surgeons during thyroidectomy in patients with papillary thyroid carcinoma (PTC). RLN invasion by PTC in a patient presenting with preoperative vocal fold paralysis may require resection of the nerve with the tumor. However, the decision should be made regarding whether to preserve or sacrifice a functioning RLN invaded by PTC. Under certain conditions, preservation of the nerve with incomplete tumor resection could be considered. An RLN that has been resected due to PTC invasion may be managed by various reinnervation techniques to improve vocal outcomes. This article reviews clinical considerations and rationales for surgical decisions related to patients with PTC invasion of the RLN.
Recurrent laryngeal nerve (RLN) invasion by papillary thyroid carcinoma (PTC) can occur either from the primary tumor or the lymph node metastasis. Invasion of the RLN may be identified in 33% to 61% of patients with local invasion of PTC into surrounding organs [1-3]. Since the RLN may be difficult to identify on preoperative imaging studies, the anatomy of the RLN should be considered when the primary PTC or metastatic lymph node is located along the tracheoesophageal groove. The right RLN comes from the vagus nerve looping more laterally at the subclavian artery. Hence, a tumor located in the right posterior lower lobe could also have invasion of the RLN [4].
Up to 68% of patients with RLN invasion might have normal vocal fold movement [4,5]. Therefore, clinical suspicion based on preoperative imaging studies and preparation for possible RLN injury/resection and patient counseling is mandatory if nerve invasion is predicted. A surgical strategy on whether to preserve or sacrifice a functioning RLN invaded by PTC needs to be established before the surgery. The decision may be controversial because previous studies have reported that invasion of the RLN showed no independent impact on survival outcomes in patients with PTC [1]. In addition, there have been controversial outcomes regarding the survival benefit of RLN resection in patients with locally invasive PTC [6-8]. Moreover, the feasibility and oncologic safety of incomplete tumor removal (R2 resection) to preserve the RLN with local invasion has been reported [9,10].
Therefore, patients with PTC invasion of the RLN require a thorough preoperative evaluation and preparation followed by an appropriate intraoperative decision for both oncologic safety and functional outcomes. In this article, clinical considerations and rationales for surgical decisions related to patients with PTC invasion to the RLN will be reviewed.
Preoperative laryngoscopy to examine the vocal function is recommended to identify any vocal fold paresis or paralysis [2,11]. It has been reported that 70% of patients with preoperative vocal fold paralysis (VFP) undergoing thyroidectomy were diagnosed with invasive thyroid cancer [12]. On the other hand, almost one-third of patients with VFP after thyroidectomy showed normal vocal function, thereby showing the necessity of a laryngoscope exam to detect neural dysfunction [13,14]. Moreover, Newman et al. [4] reported that almost one-third of patients had normal vocal fold mobility despite gross invasion of the RLN. Thus, laryngeal examination may be mandatory to check preoperative vocal fold function. Ultrasonography could be considered as an alternative method to examine the vocal function [15].
Ultrasound image presenting a tumor with protrusion into the tracheoesophageal groove was reported to have a diagnostic accuracy of 96.3% to predict RLN invasion by thyroid cancer [16]. Loss of normal thyroid tissue between cancer and the tracheoesophageal groove may also be an ultrasonographic finding of thyroid cancer with RLN invasion (Fig. 1). Seo et al. [17] reported that computerized tomography (CT) showed a sensitivity, specificity, and accuracy of 78.2%, 89.8%, and 85.5%, respectively, for invasion of the RLN. The kappa value presenting the interobserver variability was 0.7546, showing a substantial agreement. The CT findings suggesting RLN invasion were completely effaced fatty tissue in the tracheoesophageal groove, greater than 25% of the circumference of the tumor abutting the capsule at the posterior portions of the thyroid [18]. Magnetic resonance imaging could also suggest findings for suspected invasion to the RLN [19]. However, another study found that imaging studies may predict extension of thyroid cancer to the RLN in only one-quarter (26.7%) of patients [4].
Meticulous preoperative evaluation and imaging may suggest possible invasion of the RLN by thyroid cancer. Potential risk of RLN invasion should be explained to the patient with possible temporary/permanent VFP from traction injury or permanent VFP due to resection of the nerve invaded by the tumor [2,11]. Possibility of bilateral VFP (with tracheostomy) and staging the surgery to prevent such complication should be included in the informed consent. In the case of RLN resection, the reinnervation procedure, postoperative rehabilitation and expected outcomes need to be explained. In the case of a patient with a functioning RLN potentially invaded by cancer, preservation of the nerve even with microscopic or macroscopic residual tumor could be discussed with the patient considering the age, occupation, and personal preference of the patient [10,11].
In patients presenting preoperative VFP due to gross invasion of thyroid cancer, resection of the nerve with removal of the tumor should be considered [2,11]. However, the decision to preserve or sacrifice a functioning RLN invaded by PTC is controversial. This may be due to the lesser impact of RLN invasion on oncologic outcome compared to invasion of other organs categorized as T4a. Some authors have even suggested that it may be more appropriate to consider RLN invasion as the T3b category [11]. Invasion of RLN does lead to higher risk of recurrence, but to a lesser degree than tracheal or esophageal invasion [20]. In addition, RLN invasion showed no significant impact on survival of patients with PTC [1]. Moreover, resection of a RLN invaded by PTC had no advantage to improve recurrence-free survival [5,6,9], disease-specific survival [21], and overall survival [22].
Accordingly, the consensus of the American Head and Neck Society (AHNS) states that PTC may be shaved off to preserve a functioning RLN if all gross tumors are removed [2]. Macroscopic completeness of tumor resection may be achieved if tumor involvement of the nerve is confined to the epineurium [11]. However, preservation of the RLN may be impossible if the tumor involves the perineurium and endoneurium. Wu et al. [11] proposed that there may be factors to consider in favor of preserving the RLN even if the tumor undergoes incomplete resection with small remnant followed by adjuvant therapy: (1) young patients and voice professionals or those with preference to preserve their vocal function; (2) elderly patients and those with reduced pulmonary function leading to higher risk of aspiration pneumonia; (3) patients with contralateral VFP at risk of bilateral VFP; (4) active distant metastasis; and (5) generally iodine-avid patients when efficiency of adjuvant treatment is judged to be good.
Lee et al. [10] recently reported that shaving the tumor with gross residual tumor (incomplete tumor resection) smaller than 1 cm in length and 4 mm in thickness followed by high-dose radioactive iodine ablation (RAI) led to acceptable oncologic and functional outcomes. All the patients underwent more than one RAI treatment (>100 mCi), and 61.7% underwent two RAI treatments. Among the 47 patients with isolated invasion of the RLN (excluding patients with invasion of the trachea or esophagus), 10.6% showed recurrence with lymph node metastasis with no death or distant metastasis. The nerve was resected only in one case (2.1%) due to progression of the residual tumor. There were no patients with permanent VFP, with six cases (12.8%) of temporary VFP. The final non-stimulated serum thyroglobulin was 0.7±1.8 ng/mL. On the other hand, partial resection of the RLN has been suggested by Kihara et al. [23]. They applied this technique to patients with the thickness of the preserved RLN less than half of its original size. Among 18 patients, 83% of the patients had functioning vocal folds 1 year after surgery presenting nearly normal phonation. Based on these studies and alternate adjuvant treatments such as RAI, T3 suppression, radiotherapy, and tyrosine kinase inhibitors, attempts to spare a functioning RLN invaded by PTC could be considered, and its oncologic safety should be confirmed in further studies [11].
The AHNS recommended intraoperative neuromonitoring (IONM) in all cases of invasive differentiated thyroid carcinoma [2]. IONM is helpful for identification and preservation the RLN during thyroidectomy [24]. It may predict postoperative vocal fold function, prevent bilateral VFP or predict the necessity for tracheostomy [11]. The International Neural Monitoring Study Group [11] introduced a management algorithm in patients with ipsilateral preoperative VFP. They suggested performing contralateral RLN dissection first and proceeding to the invaded side if the nerve is well preserved (no loss of signal). The proximal electromyogram data could be considered for decisions on preservation or sacrifice of the RLN in patients with preoperative VFP. Since one-third of patients with abnormal laryngoscope findings may maintain stimulability with IONM, resecting an RLN with proximal stimulability may lead to deterioration of dysphonia and dysphagia [11].
In patients with anticipated resection of the RLN, reinnervation should be prepared before surgery [2]. Reinnervation of the RLN also should be considered for patients with preoperative VFP due to PTC invasion since it led to improved vocal outcomes and spared the need for laryngeal framework surgery [25]. Methods of reinnervation include direct anastomosis, free nerve grafting, ansa cervicalis to RLN anastomosis, and vagus to RLN anastomosis [2,25-27]. Reinnervation can restore the muscle tone of the paralyzed vocal fold and thereby improve vocal outcomes [25-27]. The reinnervated vocal fold is fixed at the median, but may restore its tension and recover from atrophy, leading to reduced vocal gap and enhanced tension between vocal folds [26].
Preoperative imaging and laryngoscopy should be reviewed thoroughly to identify possible RLN invasion by PTC. Informed consent should be obtained for possible resection/reinnervation of the RLN or preservation of the nerve with microscopic/macroscopic residual tumor and necessity of adjuvant treatment. IONM may be helpful to preserve the nerve during tumor dissection and aid in intraoperative decisions regarding surgical extent. The limited impact of isolated RLN invasion by PTC on oncologic outcomes and the uncertain benefit of resecting the RLN due to tumor invasion should be considered by clinicians when facing the decision of whether to preserve or sacrifice the nerve.
Notes
References
1. McCaffrey TV, Bergstralh EJ, Hay ID. Locally invasive papillary thyroid carcinoma: 1940-1990. Head Neck. 1994; 16:165–72.
2. Shindo ML, Caruana SM, Kandil E, McCaffrey JC, Orloff LA, Porterfield JR, et al. Management of invasive well-differentiated thyroid cancer: an American Head and Neck Society consensus statement. AHNS consensus statement. Head Neck. 2014; 36:1379–90.
3. Kowalski LP, Filho JG. Results of the treatment of locally invasive thyroid carcinoma. Head Neck. 2002; 24:340–4.
4. Newman SK, Harries V, Wang L, McGill M, Ganly I, Girshman J, et al. Invasion of a recurrent laryngeal nerve from small well-differentiated papillary thyroid cancers: patient selection implications for active surveillance. Thyroid. 2022; 32:164–9.
5. Na HS, Kwon HK, Shin SC, Cheon YI, Seo M, Lee JC, et al. Clinical outcomes of T4a papillary thyroid cancer with recurrent laryngeal nerve involvement: a retrospective analysis. Sci Rep. 2021; 11:6707.
6. Nishida T, Nakao K, Hamaji M, Kamiike W, Kurozumi K, Matsuda H. Preservation of recurrent laryngeal nerve invaded by differentiated thyroid cancer. Ann Surg. 1997; 226:85–91.
7. Falk SA, McCaffrey TV. Management of the recurrent laryngeal nerve in suspected and proven thyroid cancer. Otolaryngol Head Neck Surg. 1995; 113:42–8.
8. Chan WF, Lo CY, Lam KY, Wan KY. Recurrent laryngeal nerve palsy in well-differentiated thyroid carcinoma: clinicopathologic features and outcome study. World J Surg. 2004; 28:1093–8.
9. Lee HS, Kim SW, Park T, Nam GY, Hong JC, Lee KD. Papillary thyroid carcinoma with exclusive involvement of a functioning recurrent laryngeal nerve may be treated with shaving technique. World J Surg. 2015; 39:969–74.
10. Lee HS, Kim Y, Kim SB, Choi DG, Cha HK, Park JS, et al. Shaving papillary thyroid carcinoma involving functioning recurrent laryngeal nerve: safety of incomplete tumor resection and nerve sparing. Ann Surg Oncol. 2023; 30:7157–64.
11. Wu CW, Dionigi G, Barczynski M, Chiang FY, Dralle H, Schneider R, et al. International neuromonitoring study group guidelines 2018: Part II: Optimal recurrent laryngeal nerve management for invasive thyroid cancer-incorporation of surgical, laryngeal, and neural electrophysiologic data. Laryngoscope. 2018; 128 Suppl 3:S18–27.
12. Randolph GW, Kamani D. The importance of preoperative laryngoscopy in patients undergoing thyroidectomy: voice, vocal cord function, and the preoperative detection of invasive thyroid malignancy. Surgery. 2006; 139:357–62.
13. Sittel C, Stennert E, Thumfart WF, Dapunt U, Eckel HE. Prognostic value of laryngeal electromyography in vocal fold paralysis. Arch Otolaryngol Head Neck Surg. 2001; 127:155–60.
14. Chandrasekhar SS, Randolph GW, Seidman MD, Rosenfeld RM, Angelos P, Barkmeier-Kraemer J, et al. Clinical practice guideline: improving voice outcomes after thyroid surgery. Otolaryngol Head Neck Surg. 2013; 148(6 Suppl):S1–37.
15. Fukuhara T, Donishi R, Matsuda E, Koyama S, Fujiwara K, Takeuchi H. A novel lateral approach to the assessment of vocal cord movement by ultrasonography. World J Surg. 2018; 42:130–6.
16. Chung SR, Baek JH, Choi YJ, Sung TY, Song DE, Kim TY, et al. Sonographic assessment of the extent of extrathyroidal extension in thyroid cancer. Korean J Radiol. 2020; 21:1187–95.
17. Seo YL, Yoon DY, Lim KJ, Cha JH, Yun EJ, Choi CS, et al. Locally advanced thyroid cancer: can CT help in prediction of extrathyroidal invasion to adjacent structures? AJR Am J Roentgenol. 2010; 195:W240–4.
18. Agha FP. Recurrent laryngeal nerve paralysis: a laryngographic and computed tomographic study. Radiology. 1983; 148:149–55.
19. Takashima S, Takayama F, Wang J, Kobayashi S, Kadoya M. Using MR imaging to predict invasion of the recurrent laryngeal nerve by thyroid carcinoma. AJR Am J Roentgenol. 2003; 180:837–42.
20. Ito Y, Kihara M, Takamura Y, Kobayashi K, Miya A, Miyauchi A. Prognosis and prognostic factors of patients with papillary thyroid carcinoma requiring resection of recurrent laryngeal nerve due to carcinoma extension. Endocr J. 2012; 59:247–52.
21. Lang BH, Lo CY, Wong KP, Wan KY. Should an involved but functioning recurrent laryngeal nerve be shaved or resected in a locally advanced papillary thyroid carcinoma? Ann Surg Oncol. 2013; 20:2951–7.
22. Brooks JA, Abdelhamid Ahmed AH, Al-Qurayshi Z, Kamani D, Kyriazidis N, Hammon RJ, et al. Recurrent laryngeal nerve invasion by thyroid cancer: laryngeal function and survival outcomes. Laryngoscope. 2022; 132:2285–92.
23. Kihara M, Miyauchi A, Yabuta T, Higashiyama T, Fukushima M, Ito Y, et al. Outcome of vocal cord function after partial layer resection of the recurrent laryngeal nerve in patients with invasive papillary thyroid cancer. Surgery. 2014; 155:184–9.
24. Randolph GW, Dralle H; International Intraoperative Monitoring Study Group, Abdullah H, Barczynski M, Bellantone R, et al. Electrophysiologic recurrent laryngeal nerve monitoring during thyroid and parathyroid surgery: international standards guideline statement. Laryngoscope. 2011; 121 Suppl 1:S1–16.
25. Iwaki S, Maeda T, Saito M, Otsuki N, Takahashi M, Wakui E, et al. Role of immediate recurrent laryngeal nerve reconstruction in surgery for thyroid cancers with fixed vocal cords. Head Neck. 2017; 39:427–31.
26. Masuoka H, Miyauchi A. Intraoperative management of the recurrent laryngeal nerve transected or invaded by thyroid cancer. Front Endocrinol (Lausanne). 2022; 13:884866.
27. Yumoto E, Sanuki T, Kumai Y. Immediate recurrent laryngeal nerve reconstruction and vocal outcome. Laryngoscope. 2006; 116:1657–61.
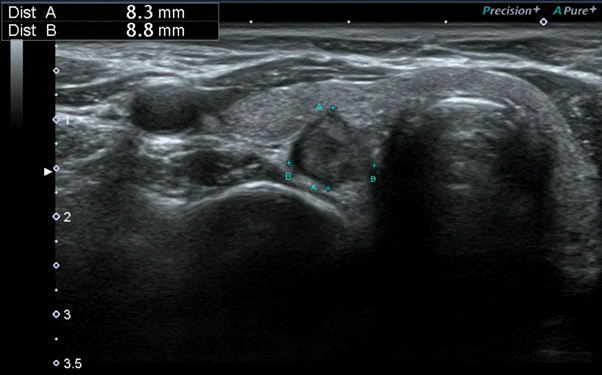
Fig. 1.
Ultrasound image of a patient with suspected invasion of the recurrent laryngeal nerve by a papillary thyroid carcinoma. Protrusion of the tumor into the right tracheoesophageal groove and partial loss of normal thyroid tissue between cancer and the tracheoesophageal groove can be seen. The photograph was provided by the author, Hyoung Shin Lee.




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download