Abstract
SUPPLEMENTARY MATERIALS
Supplementary Table 1.
Notes
CONFLICTS OF INTEREST
Lee-Ling Lim has been international editorial board members of the Diabetes & Metabolism Journal since 2022. She was not involved in the review process of this article. Otherwise, there was no conflict of interest.
Ying-Guat Ooi and Shireene R. Vethakkan report no conflict of interest; Tharsini Sarvanandan reports receiving honoraria for giving lectures from Novo Nordisk; Nicholas Ken Yoong Hee reports receiving honoraria for giving lectures from AstraZeneca, Novo Nordisk and Zuellig Pharma; Quan-Hziung Lim reports receiving honoraria for giving lectures from AstraZeneca, Boehringer Ingelheim, Novo Nordisk and Zuellig Pharma; Sharmila S. Paramasivam reports receiving honoraria for consultancy or giving lectures from Abbott, Amgen, AstraZeneca, Boehringer Ingelheim, Merck, Novo Nordisk and Zuellig Pharma; Jeyakantha Ratnasingam reports receiving honoraria for consultancy or giving lectures from Abbott, Amgen, AstraZeneca, Boehringer Ingelheim, Novo Nordisk, Sanofi, Servier, Novartis, Ipsen and Zuellig Pharma; Soo-Kun Lim reports receiving grants and/or honoraria for consultancy or giving lectures from Abbott, AstraZeneca, Astellas, Baxter, Boehringer Ingelheim, Duopharma, Fresenius-Kabi, MSD, Novartis, Novo Nordisk, Roche, Sanofi and Taisho; Lee-Ling Lim reports receiving grants and/or honoraria for consultancy or giving lectures from Abbott, Amgen, AstraZeneca, Boehringer Ingelheim, Novartis, Novo Nordisk, Roche, Sanofi, Servier and Zuellig Pharma.
REFERENCES
Fig. 2.
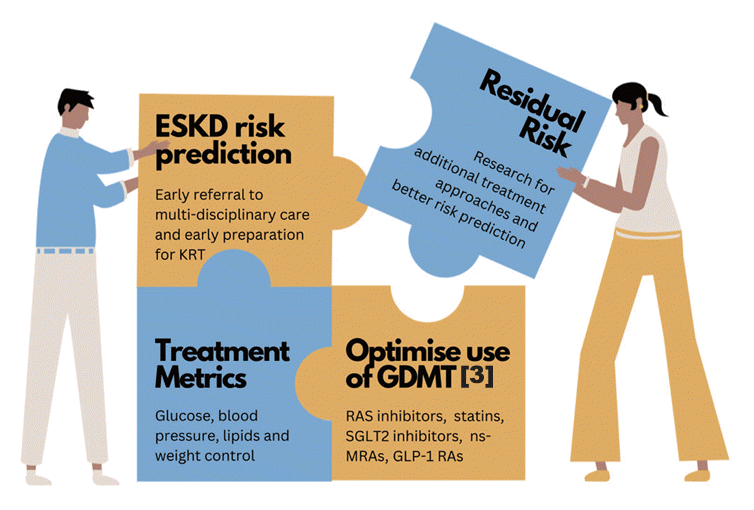
Table 1.
| Study; Region | Study characteristics | Study design and aim | Key findings | KFRE, C statistic (95% CI) |
|---|---|---|---|---|
| Tangri et al. (2016) [59]; North America & Europe | a) 721,357 adults (40% had diabetes) | a) Meta-analysis | a) Excellent discrimination and appropriate cali-bration (death not treated as competing risk) | a) 4- and 8-variable 2-year score: 0.90 (0.89–0.92) |
| b) Multinational cohorts from Chronic Kidney Disease Prognosis Consortium (CKD-PC) | b) Validation and recalibration for non-USA/Canada cohorts | |||
| c) Mean±SD eGFR: 46±11 mL/min/1.73 m2 | b) Addition of a recalibration factor optimized performance in non-USA/Canada populations | b) 4- and 8-variable 5-year: 0.88 (0.86–0.90) | ||
| d) 40% has baseline urinary ACR of ≥30 mg/g | ||||
| e) Mean±SD age: 74±10 years | ||||
| f) Men 77% | ||||
| Lennartz et al. (2016) [60]; Germany | a) 403 adults | a) Prospective cohorts | a) Excellent discrimination and calibration | a) 4-variable 3-year score: 0.91 (0.83–0.99) |
| b) Referral to tertiary nephrology care center | b) Validation | b) Addition of ultrasound markers did not improve performance | ||
| c) Mean±SD eGFR: 55.7±32 mL/min/1.73 m2 | c) Addition of ultrasound markers: RRI or DI-RISK | |||
| d) Median urinary ACR: 44 mg/g (IQR, 15–204) | ||||
| e) Mean±SD age: 60±15 years | ||||
| f) Men 58% | ||||
| g) Mean±SD RRI: 72±9 | ||||
| h) Mean±SD DI-RISK: 8±5 | ||||
| Major et al. (2019) [61]; United Kingdom | a) 35,539 adults (31.5% had diabetes) | a) Retrospective cohort | a) Excellent discrimination (death not treated as competing risk) | a) 4-variable 2-year score: 0.93 (0.91–0.96) |
| b) Primary care CKD population | b) Validation in primary care setting and clinical utility | |||
| c) Median eGFR: 51 mL/min/1.73 m2 (IQR, 43–56) | b) Referral criteria based on 5-year risk of ≥5% and/or an urinary ACR of ≥70 mg/mmol is time and cost-effective | b) 4-variable 5-year score: 0.93 (0.91–0.94) | ||
| d) Median urinary ACR: 3.2 mg/mmol (IQR, 1.2–8.0) | ||||
| e) Mean±SD age: 76±10 years | ||||
| f) Men 43% | ||||
| Hallan et al. (2019) [62]; USA | a) 1,188 elderly (17% had diabetes) | a) Retrospective cohort | a) Well calibrated with excellent discrimination | a) 4-variable 5-year score: 0.88 (0.86–0.90) |
| b) General population-based data | b) Validation of both KFRE and MREK in elderly | b) Recommend using both MREK and KFRE to decide whether to prepare for RRT in elderly people with advanced CKD | ||
| c) Mean±SD eGFR: 36±8 mL/min/1.73 m2 | ||||
| d) Mean±SD urinary ACR: 7.1±18.7 mg/mmol | ||||
| e) Mean±SD age: 80±6.8 years | ||||
| f) Men 47% | ||||
| Wang et al. (2019) [63]; Singapore | a) 17,271 adults (59% had T2DM) | a) Retrospective cohort | a) The Recalibrated Pooled KFRE SEA has similar discrimination with slightly improved precision. | Original KFRE: |
| b) Primary care CKD population | b) Validation | a) 4-variable 2-year score: 0.96 (0.95–0.97) | ||
| c) 89% CKD stage 3 | c) Recalibration in Singapore population | b) The effect of competing mortality risk is unlikely to affect the ESKD prediction. | b) 4-variable 5-year score: 0.94 (0.93–0.95) | |
| d) Urinary ACR data not included | d) Clinical utility | Recalibrated Pooled KFRE SEA: | ||
| e) Mean±SD age: 75±9 years | c) Using calculated 5-year risk >10%–16% to guide dialysis planning and calculated 2-year risk >45% to guide nephrologist referral would facilitate more efficient care and accurate risk stratification. | a) 4-variable 2-year score: 0.96 (0.95–0.97) | ||
| f) Men 49% | b) 4-variable 5-year score: 0.94 (0.93–0.95) | |||
| Tangri et al. (2020) [64]; Canada | a) 3,659 kidney transplant recipients | a) Retrospective cohort | a) Accurately predicts graft failure in kidney transplant recipients with even better discrimination when eGFR is <45 mL/min/1.73 m2 (death was not treated as a competing risk). | a) 4-variable 2-year score: 0.81 (0.72–0.91) |
| b) Transplant database from multiple transplant centers in Canada | b) Validation among kidney transplant recipients 1 year post-transplant | |||
| c) 26% had eGFR <45 mL/min/1.73 m2 | b) 4-variable 5-year score: 0.73 (0.67–0.80) | |||
| d) Median urinary ACR: 2.2–9.8 mg/mmol across 4 cohorts | ||||
| e) Mean age: 47–53 years across 4 cohorts | ||||
| f) Men 60%–66% across 4 cohorts | ||||
| Kang et al. (2020) [65]; Korea | a) 13,244 adults (29% had diabetes) | a) Retrospective cohort | a) 28.0% subjects developed ESKD during the mean follow-up period of 4.1 years. | a) 4-variable 2-year score: 0.86 (0.86–0.87) |
| b) Nephrology clinic in 2 tertiary centers | b) Validation in Korean population and recalibration | b) 6-variable 2-year score: 0.87 (0.86–0.88) | ||
| c) Mean±SD eGFR: 36.1±17.1 mL/min/1.73 m2 | b) Excellent discrimination | c) 8-variable 2-year score: 0.88 (0.86–0.88) | ||
| d) Mean±SD urinary ACR: 992.9±2,325.6 mg/g | c) No need for recalibration | d) 4-variable 5-year score: 0.83 (0.82–0.85) | ||
| e) Mean±SD age: 60±14 years | e) 6-variable 5-year score: 0.83 (0.82–0.84) | |||
| f) Men 58% | f) 8-variable 5-year score: 0.83 (0.82–0.85) | |||
| Chu et al. (2020) [66]; USA | a) 2,889 kidney transplant recipients (43% living donor graft, 39.3% had diabetes) | a) Retrospective cohort | a) 2.4% developed graft loss by 2 years, 8.7% by 5 years | a) 4-variable 2-year score: 0.85 (0.81–0.88) |
| b) Multi-center cohort-majority from the USA, few from Canada and Brazil | b) Validation among kidney transplant recipients with eGFR ≤60 mL/min/1.73 m2 6 months post-transplant | b) Accurate calibration and discrimination (death treated as a competing risk) | b) 4-variable 5-year score: 0.81 (0.78–0.84) | |
| c) Mean±SD eGFR: 41±11 mL/min/1.73 m2 | c) Well calibrated for both deceased donor and living donor grafts | |||
| d) Median urinary ACR 28 mg/g (IQR, 10–119) | d) Poor calibration for subgroups of less than 2 years post-transplantation | |||
| e) Mean±SD age: 52±9 years | ||||
| f) Men 61% | ||||
| Hundemer et al. (2020) [67]; Canada | a) 1,293 adults (49% had diabetes) | a) Retrospective cohort | a) Excellent discrimination & adequate calibra-tion across CKD etiologies (death was not treated as a competing risk) | a) 4-variable 2-year score: 0.83 (0.81–0.85) |
| b) Specialty nephrology clinic at single academic tertiary center | b) Validation across different CKD etiologies | |||
| c) Median eGFR: 15 mL/min/1.73 m2 (IQR, 12–19) | b) Underestimation of risk for ADPKD subgroup | b) 4-variable 2-year score: 0.81 (0.77–0.84) | ||
| d) Median urinary ACR: 1,277 mg/g (IQR, 322–2,903) | ||||
| e) Median age: 68 years (IQR, 58–78) | ||||
| f) Men 61% | ||||
| Ali et al. (2021) [68]; United Kingdom | a) 743 adults (40% had diabetes) | a) Retrospective cohort | a) Good discrimination with similar predictive accuracy | a) 4- and 8-variable 2-year score: 0.79 (0.76–0.83) |
| b) Advanced kidney care service clinic at single tertiary care center | b) Validation & clinical utility across different etiologies of CKD | b) Underestimation of risk for ADPKD subgroup | ||
| c) Median eGFR: 16 mL/min/1.73 m2 (IQR, 13–18) | d) Better for guiding further intervention compared to using eGFR cut-offs | b) 4- and 8-variable 5-year score: 0.77 (0.74–0.81) | ||
| d) Median urinary ACR: 409 mg/g (IQR, 85–1,356) | ||||
| e) Median age: 69 years (IQR, 57–77) | ||||
| f) Men 62% | ||||
| Ramspek et al. (2021) [38]; Europe | a) 15,069 adults (21% had diabetes) | a) Retrospective cohorts | a) Excellent calibration and good discrimination | EQUAL cohort |
| b) Multi-center cohorts | b) Validation | b) 5-year KFRE overpredicted risk by 10%–18% (death as competing risk) | a) 4-variable 2-year score: 0.76 (0.72–0.80) | |
| c) Mean±SD eGFR: (EQUAL cohort) 18.5±4.7 mL/min/1.73 m2 (SRR cohort) 21.9±5.7 mL/min/1.73 m2 | b) 8-variable 2-year score: 0.78 (0.75–0.81) | |||
| c) 4-variable 5-year score: 0.75 (0.71–0.78) | ||||
| d) Median urinary ACR: (EQUAL cohort) 40 mg/mmol (IQR, 8–165) (SRR cohort) 36 mg/mmol (IQR, 7–155) | d) 8-variable 5-year score: 0.76 (0.73–0.79) | |||
| SRS cohort | ||||
| e) Mean age: 74–76 years across 2 cohorts | a) 4- and 8-variable 2-year score: 0.84 (0.83–0.85) | |||
| f) Men 61%–65% | b) 4- and 8-variable 5-year score: 0.81 (0.80–0.82) | |||
| Ali (2021) [69]; United Kingdom | a) 415 transplant recipients (18.9% living donor graft, 12% had diabetes) | a) Retrospective cohort | a) Adequate discrimination for predicting graft failure, especially in those with an eGFR <45 mL/min/1.73 m2 with poor calibration (likely due to lack of transplant related variables) | a) 4-variable 5-year score: 0.74 (0.61–0.88) |
| b) Single renal transplant center | b) Validation among kidney transplant recipients 1-year post-transplant | b) 8-variable 5-year score: 0.75 (0.63–0.87) | ||
| c) Median eGFR: 54.1 mL/min/1.73 m2 (IQR, 41.6–70.5) | ||||
| d) Median urinary ACR: 22.1 mg/g (IQR, 11.5–65.4) | ||||
| e) Median age: 50 years (IQR, 40–60) | ||||
| f) Men 59% | ||||
| Kwek et al. (2022) [70]; Singapore | a) 1,128 adults (64.6% had diabetes) | a) Retrospective cohort | a) Excellent discrimination (death not taken as a competing risk) | a) 4-variable 2-year score: 0.87 (0.85–0.90) |
| b) Nephrology clinic, single tertiary center | b) Validation | b) 8-variable 2-year score: 0.87 (0.85–0.89) | ||
| c) Median eGFR: 31.9 mL/min/1.73 m2 (IQR, 22.4–44.8) | ||||
| d) Median urinary ACR: 243 mg/g (range, 63–868) | ||||
| e) Mean±SD age: 67±12 years | ||||
| f) Men 58% | ||||
| Irish et al. (2023) [71]; Australia | a) 12,861 adults (54.9% had diabetes) | a) Retrospective cohort | a) Excellent discrimination and adequately calibrated (death not taken as a competing risk) | a) 4-variable 2-year score: 0.98 (0.97–0.99) |
| b) Multiple national registries | b) Validation among Australian cohort | b) 6-variable 2-year score: 0.97 (0.96–0.99) | ||
| c) Mean±SD eGFR: 50.3±9.3 mL/min/1.73 m2 | c) 8-variable 2-year score: 0.96 (0.94–0.98) | |||
| d) Median urinary ACR: 1.4 mg/g (IQR, 0.6–5.0) | d) 4-variable 5-year score: 0.96 (0.95–0.97) | |||
| e) Mean±SD age: 70±10 years | e) 6-variable 5-year score: 0.96 (0.95–0.97) | |||
| f) Men 48% | f) 8-variable 5-year score: 0.95 (0.93–0.96) |
KFRE, Kidney Failure Risk Equation; CI, confidence interval; SD, standard deviation; eGFR, estimated glomerular filtration rate; ACR, albumin-creatinine ratio; IQR, interquartile range; RRI, renal resistive index; DI-RISK, difference of resistive indices in spleen and kidney; CKD, chronic kidney disease; MREK, mortality risk equation for kidney disease; RRT, renal replacement therapy; T2DM, type 2 diabetes mellitus; SEA, South East Asia; ESKD, end-stage kidney disease; ADPKD, autosomal dominant polycystic kidney disease; EQUAL, European Quality Study; SRR, Swedish Renal Registry.




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download