This article has been
cited by other articles in ScienceCentral.
Abstract
Background
A family approach and obtaining consent from the families of potential brain-dead donors is the most important step of organ procurement in countries where an opt-in policy applies to organ donation. Health care staff’s communication skills and ability to have conversations about donation under circumstances of grief and emotion play a crucial role in families’ decision-making process and, consequently, the consent rate.
Methods
A new training course, called the Iranian family approach-specific course (IrFASC), was designed with the aim of improving interviewers’ skills and knowledge, sharing experiences, and increasing coordinators’ confidence. The IrFASC was administered to three groups of coordinators. The family consent rate of participants in the same intervals (12 months for group 1, 6 months for group 2, and 3 months for group 3) was measured before and after the training course. The Wilcoxon signed-rank test was used to make comparisons.
Results
The family consent rate was significantly different for all participants before and after the training, increasing from 50.0% to 62.5% (P=0.037). Furthermore, sex (P=0.005), previous training (P=0.090), education (P=0.068), and duration of work as a coordinator (P=0.008) had significant effects on the difference in families’ consent rates before and after IrFASC.
Conclusions
This study showed that the IrFASC training method could improve the success of coordinators in obtaining family consent.
Go to :

Keywords: Tissue and organ procurement, Education, Organ transplantation
|
HIGHLIGHTS |
Family approach and obtaining consent from brain-dead families is the most important step of organ procurement. The Iranian family approach-specific course has a significant effect on the success of coordinators in obtaining family consent. The sex, experience and previous training courses have an effect on the success of the coordinators.
|
Go to :

INTRODUCTION
Obtaining consent from the families of eligible deceased organ donors, known as the family approach, is the most important step of organ procurement in countries where an opt-in policy applies to organ donation [
1]. A large proportion of the gap between supply and demand for organs is attributed to the low rate of family consent and the high family refusal rate [
2]. It is well known that family refusal is the most important factor affecting organ donation [
3]. In recent years, a reduction in the refusal rate has been seen in European countries, specifically in Spain [
4], but the rate of family refusal in Iran remains high. According to latest report of the International Registry in Organ Donation and Transplantation, the rate of actual deceased organ donors in Iran over 2021 was 11.72 per million population (PMP), representing an increase of 3.92% compared to 2020 [
5]. Despite this slight improvement since 2020, the donation rate in Iran remains below the worldwide average, with a donation rate of 41.88 PMP in USA or 40.2 PMP in Spain [
6].
Multiple socio-demographic characteristics, such as ethnicity, culture, religion, and education, influence public perceptions of organ donation [
7,
8]. It has been reported that inadequate knowledge about donation and negative attitudes are the main reasons for refusal to donate organs and tissue [
9,
10]. The donation system is built on a foundation of continuing education and training to ensure the presence of highly qualified professionals in transplant teams. Health care staff’s communication skills and ability to have conversations about donation under circumstances of grief and emotion play a crucial role in families’ decision-making process and, consequently, the consent rate [
2]. To enhance family satisfaction and donation, it is necessary to provide specific communication training for health care professionals to establish a foundation for effective conversations about donation [
11]. Although training has been prioritized for health care professionals, it still seems essential to follow a well-designed approach to education, incorporate all staff members, and use experimental learning.
According to the data from the latest report of 2019 by the National Transplant Organization, the majority of donations occur after brain death (DBD) [
12]. Identifying all obstacles to DBD and moving towards overcoming them are priorities during the process of organ donation. Since public beliefs about brain death in Iran play a critical role in the family refusal rate after brain death [
13], the involvement of coordinators who can provide reasonable responses to family members’ questions would be essential for obtaining family consent. The importance of transplant coordinators, who play a robust and independent role as a crucial element of the multidisciplinary transplant team, is well acknowledged. Transplant coordinators are responsible for facilitating patient care throughout the entirety of the transplantation process to ensure ethical practices in nursing and transplant coordination [
14]. The purpose of the present study was to examine the effects of the Iranian family approach-specific course (IrFASC) on deceased organ donors’ families’ consent and satisfaction rates. Additionally, the effects of coordinators’ characteristics, such as education, sex, and training status at baseline, on family consent were investigated.
Go to :

METHODS
Institutional review board approval for this study was waived because this study does not involve the use of any animal or human data or tissue.
A new training course (IrFASC) was designed with the aim of improving interviewers’ skills and knowledge, sharing experiences, and increasing coordinators’ confidence for use in Iran. IrFASC was held as an intensive course by the Iranian Society of Organ Donation in collaboration with the Health Ministry's Management Center for Transplantation and Special Diseases.
This 60-hour training course with participants from organ procurement units all over Iran was performed virtually (on the Adobe Connect platform) for 5 days. In this course, 21 topics related to methods of obtaining consent from families of patients with brain death were taught by organ donation specialists (
Table 1).
Table 1
The topics that were taught in the IrFASC training course
|
Topic |
|
Organ donation status in Iran |
|
Basic topics |
|
Communication skills |
|
Reasons for family refusal |
|
Data gathering and infrastructure |
|
Not knowing what the deceased believed about donation or the deceased having declared himself or herself unwilling to donate organs during life |
|
Families’ worries about mutilation and delay of funeral arrangements |
|
Financial expectations |
|
Distrust of the allocation system |
|
Dissatisfaction with health system |
|
Request for time |
|
Tribal and social problems |
|
Support of family |
|
Fear of blame |
|
Lack of access to family |
|
Guilty feelings |
|
Miracles |
|
Breaking bad news and acute reaction |
|
Negative influential people |
|
Fear of social position |
|
Refusal with no reasons |

This course included different components to increase the impact of training. The general class was held in a teacher-centered manner, important points about each topic were presented, and short videos related to each section were used to enhance understanding. In addition, 18 “brainstorming sessions” were designed to implement discussion-based learning [
15] and thinking-based learning [
16]. Think tanks were provided in order to support interactions between participants in online learning. Participants were divided into separate teams, and members of each team consulted with each other. The performance of the teams was assessed according to summaries of the opinions of the team members on the subject.
Four scenarios were also designed to simulate interviews with families of brain-dead patients. Simulation-based learning provides a situation similar to a real experience, thereby improving people's skills, attitudes, and knowledge [
17,
18]. In each simulation, a number of participants simulated the family communication process based on a pre-prepared scenario. Then, the members of the teams entered the think tanks and shared their opinions on how coordinators could behave to satisfy the families of brain-dead potential donors. This course taught coordinators how to identify families’ concerns through interviews and what techniques are available to resolve these concerns.
In order to improve focus and accuracy, four games were planned for the participants during the course. The games were played in teams with the participation of all team members in a limited time. The main factors in determining the top team were the speed of action and accuracy. As examinations, at the end of each training day, participants were asked to answer some related questions about the topics of that training day. Finally, on the last day, a comprehensive examination including the topics of the entire course was held. Additionally, to evaluate participants’ alertness and accuracy, 4-choice questions were asked at various time points.
Three groups of coordinators, with 8, 17, and 20 participants, were trained using the IrFASC and were assessed 12, 6, and 3 months after training, respectively. The family consent rate of participants who were assessed at the same intervals (12 months for group 1, 6 months for group 2, and 3 months for group 3) was measured before and after the training course.
Statistical Analysis
The data were analyzed using IBM SPSS ver. 26 (IBM Corp., Armonk, NY, USA) and Graph Pad version 8 (GraphPad Software, San Diego, CA, USA). The categorical variables are expressed as proportions and frequencies. The quantitative variables with normal distribution are summarized as mean±standard deviation (SD). Non-normal quantitative variables are presented as median and interquartile range. The Kolmogorov-Smirnov test was applied to test the normality distribution. To explore the impacts of categorical independent variables, the chi-square test was used.
Mean values were compared between two groups using the independent or paired t-test, as well as using non-parametric tests, such as the Mann-Whitney U-test or the Wilcoxon signed-rank test. Analysis of variance, the Kruskal-Wallis test, and the Friedman test were applied for comparisons of mean values among more than two groups (
Table 2). The data were modeled using generalized estimating equation (GEE) model because of their longitudinal and correlated structure (
Table 3). P-values less than 0.05 were considered to indicate statistical significance.
Table 2
Comparison of the family consent rate
|
Variable |
Before |
After |
P-value |
|
Family consent rate (%) |
|
|
|
Sex |
|
|
|
|
Male |
64 (50–100) |
69 (50–80) |
0.334 |
|
Female |
44 (0–100) |
57 (38.3–75.4) |
0.005a)
|
|
Time elapsed since training (mo) |
|
|
|
12 |
58.6 (37.5–91.7) |
66.3 (51–85.02) |
0.237 |
|
6 |
50.0 (20–91.7) |
65.6 (36.7–76.4) |
0.149 |
|
3 |
54.4 (0–100) |
58.2 (50–78.8) |
0.195 |
|
Training experience |
|
|
|
Yes |
51.7 (20–79.2) |
62.2 (40–76.3) |
0.090b)
|
|
No |
50.0 (25–100) |
66.0 (50–100) |
0.169 |
|
Education level of the coordinator |
|
|
|
PhD |
26.7 (5–48.3) |
72.8 (66.9–78.8) |
0.068b)
|
|
MSc |
40.0 (0–83.3) |
50.0 (10–72.2) |
0.715 |
|
BSc |
57.1 (25–100) |
58.7 (44.6–79.1) |
0.147 |
|
Working duration as coordinator (mo) |
|
|
|
<25 |
53.03 (10–100) |
50.0 (36.7–68.6) |
0.616 |
|
≥25 |
50.0 (20.6–93.7) |
72.5 (51.1–80) |
0.008a)
|
|
Total |
50.0 (20–100) |
62.5 (46.4–77.2) |
0.037a)
|

Table 3
GEE model results for family consent by binomial distribution and logit function
|
Variable |
β |
Standard error |
95% Wald CI |
P-value |
|
|
Lower |
Upper |
|
Intercept |
0.498 |
0.311 |
–0.113 |
1.108 |
0.110 |
|
Male sex |
0.629 |
0.297 |
0.061 |
1.197 |
0.030a)
|
|
Training experience=yes |
–0.487 |
0.400 |
–1.273 |
0.298 |
0.224 |
|
Education level of coordinator=PhD |
–0.202 |
0.237 |
–0.666 |
0.263 |
0.395 |
|
Education level of coordinator=MSc |
–0.371 |
0.420 |
–1.196 |
0.454 |
0.378 |
|
Time=after |
0.763 |
0.154 |
0.461 |
1.064 |
<0.001a)
|
|
Working duration as a coordinator |
0 |
0.003 |
–0.008 |
0.007 |
0.915 |

Go to :

RESULTS
In total, 150 coordinators attended the IrFASC training course. Among them, 45 coordinators (men, 19 [42.2%]; women, 26 [57.8%]) were included in this study because their information was complete, without missing data. Of the study participants, 8 (17.8%), 17 (37.8%), and 20 (44.4%) were assessed at 12, 6, and 3 months after the training, respectively. The mean age was 36.9±6.8 years (36.1±5.9 and 38.4±6.5 years for men and women, respectively, without a statistically significant difference; P=0.104). Twenty-eight of the participants (62.2%) had attended other training courses previously, while 17 (37.8%) had no training experience.
Four (8.9%), 5 (11.1%), and 36 (80%) coordinators had PhD, MSc, and BSc degrees, respectively. The mean±SD and median (interquartile range) values for coordinator experience were 30.7±30.4 months and 25 months (10–41 months), respectively. One of the key variables of this study was the family consent rate, which was calculated by dividing the number of family consents by the number of family approaches for each coordinator.
Table 2 shows a comparison of the family consent rate before and after training by sex, the time elapsed since training, experience of a previous training course, and education.
The Wilcoxon signed-rank test was used to compare the results shown in
Table 2. The Spearman correlation coefficient between the family consent rate and age was –0.053 (P=0.728) and –0.006 (P=0.967) before and after training, respectively, and those relationships were not significant. The correlation coefficient between the duration of experience as a coordinator and the family consent rate was estimated as –0.46 (P=0.766) and 0.289 (P=0.054) before and after training, respectively.
According to the results shown in
Table 2, the family consent rate significantly improved after training for all participants, with an increase from 50.0% to 62.5% (P=0.037). The family consent rate in women showed a statistically significant difference before and after training at a significance level of 10%, while for men, this comparison did not yield significant results (P=0.334). The difference in the family consent rate before and after the IrFASC for those who had previously attended other training courses was significant at the level of 10% (51.7% vs. 62.2%, P=0.090). However, a similar result was not seen for coordinators who had not received previous training (
Fig. 1).
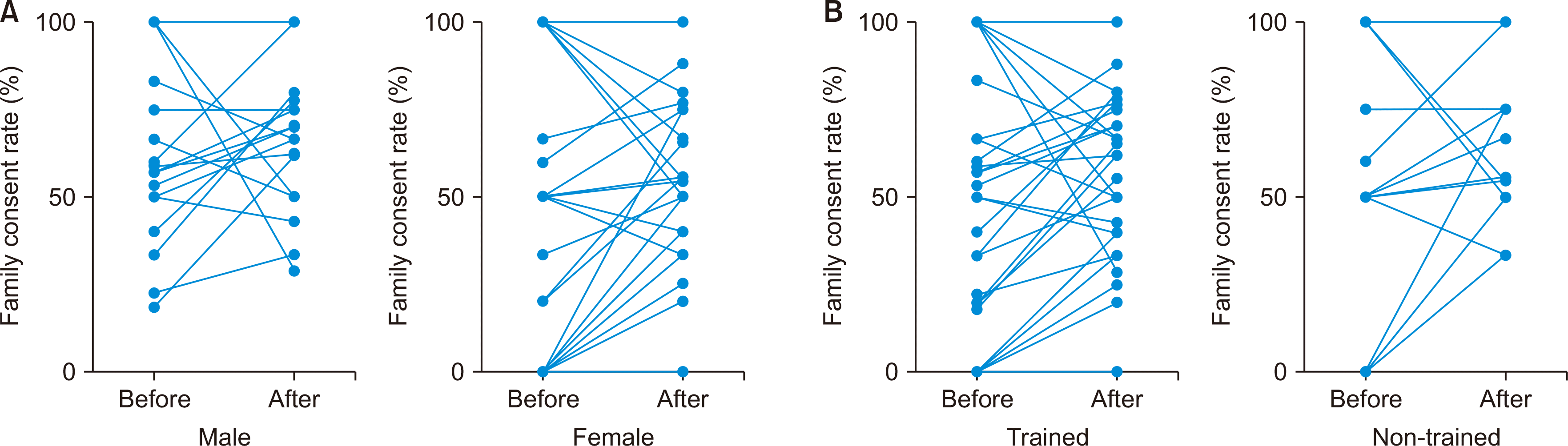 | Fig. 1Family consent rate change by (A) sex and (B) training status. 
|
Furthermore, the comparison of family consent rates according to the time elapsed after training (12, 6, or 3 months) did not show any significant differences. The family consent rate of coordinators with PhD degrees, compared to those with other degrees, increased after training (26.7% vs. 72.8%, P=0.068). The rate of obtaining family consent was compared before and after the training course according to the duration of experience as a transplant coordinator (more or less than the average value of 25 months) (
Table 2). The family consent rate significantly improved after the IrFASC in coordinators with more than 25 months of experience (50% vs. 72.5%, P=0.008).
Table 3 shows the results of fitting the GEE model to examine the simultaneous effects of sex, previous training, education, duration of experience, and time since training on the family consent rate. Since the family consent rate was calculated by dividing the number of family consents by the total number of family approaches, a binomial distribution with a logit link function was used to fit the number of family consents. In this model, the number of family consents was considered as “successes,” and the number of family approaches was considered as the number of trials. The following reference groups were used for comparisons: female sex, no training experience, a BSc degree, and the “before” time point. Among the studied variables, only two (sex and time) showed a statistically significant effect on the family consent rate (
Table 3).
Go to :

DISCUSSION
The primary aim of this study was to investigate the effects of the IrFASC on deceased organ donors’ families’ consent rate. The secondary aim of this study was to examine the impact of the personal characteristics of coordinators, such as sex, education level, previous training history, and experience working as a transplant coordinator. The training course improved the success of coordinators in obtaining family consent. A sub-analysis showed that the training course more effectively led to improvements in women, participants with a history of training, participants with a PhD degree, and those who had worked as a transplant coordinator for more than 25 months than their counterparts. Furthermore, men and trained coordinators also became more successful in eliciting a high level of satisfaction from the families of patients with brain death.
A major obstacle to organ donation remains the inability to obtain consent [
3,
19]. Family refusal is the most important factor affecting organ donation and is responsible for a large gap between organ supply and demand [
3]. An estimated 73% of Iranian brain-dead patients' families refused organ donation in 2009 [
20]. The family members of patients with brain death are in a stressful and dramatic position in the hospital, where they are concerned about the patient's condition and are faced for the first time with the need to make a decision about organ donation. In these circumstances, the presence of a well-educated and experienced coordinator can improve dialogues and increase the rate of family consent [
21,
22].
Based on the findings of this study, the training course increased the success of family consent coordinators. Training conditions were directly and significantly related to the families’ consent rate (β=0.76, P<0.001). In a study of a training course, coordinators reported being more comfortable talking to family members of patients with brain death and answering questions related to donation following training. Furthermore, after completing the training, coordinators spent a more significant amount of time discussing donations and donation-related topics with families of eligible donors [
23]. Training courses and educational programs lead to behavioral changes in coordinators and new learning transfers to the clinical setting and increase the rate of family consent [
23,
24]. Training courses may also increase coordinators' confidence in their ability to communicate when offering organ donation, resulting in increased consent rates [
24].
Although there are many strategies for training coordinators, a review showed that one-day training programs that used role-playing with simulated participants and group discussions alongside feedback were effective for learning [
11]. Furthermore, this study found that a combination of passive learning techniques, such as written information or oral presentations with experiential learning techniques, such as role-playing with feedback, also yielded promising results [
11].
The present study showed that, in general, male coordinators were more successful during the process of obtaining a high level of satisfaction from the families of patients with brain death, but the effect of education on increasing this success rate for women was significant. A possible explanation for this is that women might apply educational content more than men in the family consent process. We suggest using combined educational methods to make the educational program attractive for both sexes.
A study by Baughn et al. [
25], published in 2010, examined how coordinators and families interacted during organ donation discussions, paying particular attention to the influence of the coordinator's sex and race and the race of the potential donor's family. That study observed that male coordinators displayed more affiliative and friendly behaviors toward a simulated white family than toward an African American family, whereas female coordinators exhibited slightly less affiliative behavior toward the white family. Other studies showed that female coordinators were more successful at obtaining family consent [
26,
27]. In this regard, cultural issues or the sex match between the coordinator and decision-maker may be influential.
This study has several strengths and limitations. One of the strengths of this study is that it considered the effects of a training course at different time points since course completion on the rate of family consent. It also analyzed coordinators’ individual characteristics and their effects on the effectiveness of the training course. One of the limitations of this study is the limited number of participants. The low number of family interviews among some coordinators after the training course is another limitation. Furthermore, because of the combination of educational strategies in this training course, the effectiveness of each strategy could not be analyzed individually. In conclusion, this study shows the beneficial effects of a training course for coordinators on their rate of family consent. More interventional studies with a larger sample size can provide more robust information on this issue.
Go to :





 PDF
PDF Citation
Citation Print
Print




 XML Download
XML Download