A 60-year-old woman reported a 2-week history of dyspnea. She had a history of radiation therapy of the chest wall due to Hodgkin’s lymphoma 40 years prior, and a history of cardiac tamponade 1-year prior (Figure 1A and B). A hemorrhagic pericardial effusion (PE) was drained at that time. There were no atypical cells in pericardial fluid cytology. Serum tumor markers such as SCC (TA4) and CYFRA 21-1 were elevated, but computed tomography (CT), positron emission tomography (PET)-CT, and endoscopic evaluation findings were negative for malignancy (Figure 1C and D). Also, there was no evidence of infection or autoimmune disease in the pericardial fluid analysis and laboratory test. She was treated with steroids for 3 months and was doing well without any symptoms. Follow-up transthoracic echocardiography (TTE) showed resolved PE (Supplementary Video 1). However, she complained of new-onset dyspnea symptoms. TTE revealed minimal PE and more aggravated pericardial adhesion with septal bouncing and respiratory variation of mitral inflow (36%) (Figure 1E and F, Supplementary Videos 2 and 3). CT demonstrated diffused pericardial thickening with enhancement and newly developed necrotic masses at the left atrium and right atrioventricular grove (Figure 1G and H). PET-CT revealed multiple hyper-metabolic masses at the pericardium (Figure 1I and J). An open biopsy was performed and the patient was diagnosed with epithelioid angiosarcoma (Figure 1K and L). The patient was administered chemotherapy with doxorubicin. Cardiac malignancy is a rare disease, but it should be considered in patients with unexplained PE and constrictive pericarditis. For these patients, multimodality imaging is helpful for diagnosis.
Written informed consent was obtained from the patient.
Notes
Funding: The authors received no financial support for the research, authorship, and/or publication of this article.
SUPPLEMENTARY MATERIALS
Supplementary Video 1
TTE showed resolution of PE, but a pericardial adhesion was suspected after 3-month steroid therapy.
Supplementary Video 2
The apical 4-chamber view of TTE showed pericardial adhesion with abnormal septal motion in this visit (after 1 year).
Supplementary Video 3
The subcostal view of TTE showed pericardial thickening and adhesion of the right ventricular free wall in this visit (after 1 year).
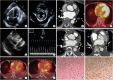
Figure 1
Multimodality images with TTE, CT, PET-CT. (A-D) Image 1-year prior, (E-J) Image in this time, and (K and L) Histopathologic findings.
(A, B) Large amount of PE with pericardial tamponade was shown on the apical 4-chamber view and the parasternal short-axis view of mid-left ventricular level of TTE; (C) Heart CT showed normal heart structure without pericardial thickening or pericardial masses; (D) PET-CT showed mild hyper-metabolic activity along the pericardium that suggested pericarditis. (E) The subcostal view of TTE showed pericardial thickening with aggravated pericardial adhesion (yellow arrow); (F) Mitral peak E-wave of 1.27 m/s (expiration) and 0.81m/s (inspiration), 36% drop in mitral E-wave velocity; (G, H) Heart CT showed not only diffuse pericardial enhancement and thickening combined with small amount of PE but also newly developed multiple necrotic pericardial masses around left atrium and right atrioventricular groove that suggested malignant tumor, such as angiosarcoma (yellow arrows); (I, J) Hyper-metabolic multiple masses at pericardium suggested pericardial malignancy were shown on PET-CT (yellow arrows); (K, L) Histopathologic finding showed atypical spindle cell infiltration and immune-histochemical staining showed the positive for vimentin, which were consistent with an epithelioid feature of high-grade sarcoma that suggested epithelioid angiosarcoma.
CT = computed tomography; PE = pericardial effusion; PET = positron emission tomography; TTE = transthoracic echocardiography.




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download