Abstract
Backgrounds/Aims
Pancreaticoduodenectomy is the most common procedure for the management of duodenal pathologies. However, it is associated with substantial morbidity and a low risk of mortality. Pancreas-preserving limited duodenal resection (PPLDR) can be performed under specific scenarios. We share our experience with PPLDR and its outcome.
Methods
We retrospectively analyzed a prospectively maintained database of patients undergoing limited duodenal resection in the form of wedge (sleeve) resection or segmental resection of one or more duodenal segments from March 2016 to March 2021 at a tertiary care center in North India.
Results
During the study period, 10 patients (including 9 males) underwent PPLDR. Five of these 10 patients showed primary duodenal or proximal jejunal pathology, while the remaining five had duodenal pathology involving an adjacent organ tumor. Four patients underwent wedge (sleeve) resection, while the remaining six underwent segmental duodenal resection of one or more duodenal segments. Mean hospital stay was 6 days (range, 3-11 days) without 30-day mortality. Morbidity occurred in 4 patients (Grade I-II, n = 3; Grade III, n = 1). All patients were alive and disease-free at the time of last follow-up. The mean follow-up duration was 23 months (range, 2-48 months).
Duodenum is a complex organ based on its anatomical location, proximity to the ampulla of Vater, the pancreas and major vessels. Pancreaticoduodenectomy is the most common procedure for the management of duodenal pathologies. However, it is associated with morbidity in the range of 30%–50% and mortality of approximately 5% in most of the large series. Advances in diagnostics and refinement of surgical techniques have led to the development of pancreas-preserving limited duodenal resection (PPLDR) either as a wedge (sleeve) resection or segmental resection as an alternative to pancreaticoduodenectomy in certain pathologies and tumor locations. Due to the rarity of such tumors, it has been difficult to formulate a standard algorithm for their management. We share our experience for this not so common but technically challenging procedure, describe various reconstruction options and their outcomes and suggest an algorithm for appropriate option for limited duodenal resection.
We retrospectively analyzed a prospectively maintained database of all patients undergoing limited duodenal resection in the form of wedge (sleeve) or segmental resection of one or more duodenal segments from March 2016 to March 2021 at a tertiary care center in North India. The study was approved by the institutional ethics committee of Mahatma Gandhi University of Medical Science and Technology (no. 20/00164). Written informed consent was obtained from all participants. Ten patients who underwent PPLDR were identified and their records were analyzed for preoperative presentation, evaluation, per-operative details, postoperative hospital stay, complications (with Clavien-Dindo grading), 30-day mortality and histopathology. Patients with periampullary pathologies who underwent pancreaticoduodenectomy were excluded. All procedures were performed by a trained gastrointestinal and hepatobiliary surgeon (AS).
An extended kocherization of the duodenum was performed in all patients; patients requiring resection of D3 and D4 segments underwent Cattell-Braasch maneuver, followed by mobilization of the ligament of Treitz. Further technique depended upon the type of pathology and tumor location. Small and benign tumors were managed via wedge (sleeve) resection of the duodenum (Fig. 1). A minor defect in the duodenal wall was closed primarily while a larger defect was closed with a jejunal serosal patch (loop). Prior to segmental resection of the duodenum, the whole of the small bowel, ascending colon and the proximal transverse colon were retracted cranially to expose the duodeno-jejunal junction. The third part of the duodenum was separated from the uncinate process of the pancreas. Additional procedures as described in the Table 1 were performed in a standard maneuver. The jejunum was divided to ensure adequate length, and the jejunal limb was passed to the right posterior to the superior mesenteric vessels. All duodeno-jejunal anastomoses were performed in a side-to-side or end-to-end manner with continuous monofilament sutures (polydioxanone PDS 3-0) in a single layer. Air leak test was performed in all patients by insufflating air via a nasogastric (Ryles) tube inserted orally during surgery. A feeding jejunostomy (modified Witzel technique) was added at approximately 30 cm distal to the anastomosis in all patients except those in whom primary closure of the duodenal defect was performed after a small wedge (sleeve) duodenal resection. Drain was placed. Patients who underwent primary repair were administered oral methylene blue on postoperative day (POD) 1 and patients who underwent anastomosis on POD 2 before starting oral feeds.
Patients’ demographic and clinical details are listed in Table 1. The mean age of patients at presentation was 54 years (range, 40–67 years). Nine out of 10 patients were male and one patient was female. Five patients had primary duodenal or proximal jejunal pathology, including jejunal adenocarcinoma (2/5) (Fig. 2), duodenal gastro-intestinal stromal tumor (GIST) (2/5) and lymphoma (1/5). Out of the remaining 5, two had retroperitoneal sarcoma (Fig. 3), one patient carried a mesenteric tumor (GIST), another carcinoma hepatic flexure (Fig. 4) and carcinoma gall bladder was detected in the remaining patient. Chief presenting complaints of the patients having duodenal or jejunal pathology was melena (4/5). Six patients underwent segmental resection of one or more duodenal segments, while remaining four patients had wedge (sleeve) excision of the lateral part of the duodenum (D2 and D3). Patients carrying other pathologies involving the duodenum underwent surgery based on the primary tumor location as described in Table 1. One patient (case no. 6) had two large recurrent retroperitoneal tumors, which were treated via segmental duodenal resection and excision, segmental transverse colon resection and proximal gastrectomy with colo-colic and esophagogastric anastomosis. One to two drains (passive) were placed in the abdominal cavity of all patients. Feeding jejunostomy was done in seven out of ten patients. Mean operative time was 190 minutes (range, 60–350 minutes) and the mean blood loss was 214 mL (range, 0–500 mL).
Postoperative morbidity was graded according to the Clavien-Dindo classification (grade I, minor deviation from normal postoperative course; grade II complications, requiring therapeutic drugs outside of those allowed in grade I; grade III, requiring surgical, endoscopic or radiological intervention; and grade IV, life threatening complications) [1]. Four patients experienced morbidity in the postoperative period. Two patients—one undergoing jejunal patch repair and one with end-to-end duodeno-jejunal anastomosis showed delayed gastric emptying (DGE)—required the use of one or more prokinetics to prevent grade II morbidity. One patient had superficial surgical site infection that was managed with wound dressings (grade I). High-grade morbidity occurred in one patient (case no. 6) who had an intra-abdominal collection and pleural effusion due to a leak from the esophago-gastric anastomosis, which was confirmed by a computed tomography (CT) scan with oral contrast. The collection was drained with an ultrasound-guided pigtail catheter (Grade IIIA). The patient also developed cardiac arrhythmias postoperatively, which required specific medication and feeding jejunostomy for continued enteral feeding. The patient was discharged on POD 11.
All patients underwent R0 resection. None of the 10 patients experienced 30-day mortality. Two patients with duodenal GIST had low-grade GIST and did not receive adjuvant biological therapy, while the patient with mesenteric GIST received adjuvant tyrosine kinase inhibitor (imatinib). Both patients with retroperitoneal sarcoma were discussed in the multidisciplinary tumor board and were not recommended any adjuvant treatment. Patients with adenocarcinoma (jejunum, colon and gall bladder) received adjuvant chemotherapy as per the institute protocol. One patient diagnosed with jejunal adenocarcinoma also had an isolated rib metastasis for which wide local excision of the metastasis was performed after one month. The patient diagnosed with lymphoma of the duodenum also received chemotherapy during the post-operative period. All patients were alive and disease-free at the time of last follow-up. The mean follow-up duration was 23 months (range, 2–48 months).
Pancreaticoduodenectomy is the standard procedure for the management of duodenal malignancies, especially when D2 is involved. It is also indicated when the duodenum is associated with a tumor involving an adjacent organ, such as cholangiocarcinoma, gall bladder cancer, stomach cancer, colon cancer, and renal cell carcinoma. Nevertheless, pancreaticoduodenectomy is associated with substantial morbidity and small but significant mortality. PPLDR is indicated for benign or low-grade malignant lesions but is technically challenging because of the location of the ampulla of Vater in the second part of the duodenum, and the head and the uncinate process of the pancreas related to the first three segments of duodenum. Combined with the rarity of such tumors, PPLDR is performed quite infrequently even at specialized gastrointestinal or hepato-pancreatico-biliary units. Few studies have described only elective primary limited duodenal resections [2-6] for primary duodenal pathology, while/however non-duodenal pathologies requiring limited duodenal resection are very rarely reported [7]. A series from Japan classified pancreas-preserving duodenectomy into proximal (D1 and D2) and distal (D3 and D4) categories [8]. Herein, we have described PPLDR in 10 patients with good outcomes.
Whenever duodenal involvement is suspected or duodenal resection is anticipated, a comprehensive pre-operative work-up is required in the form of upper gastrointestinal endoscopy and/or endoscopic ultrasound (EUS) combined with cross-sectional imaging in the form of CT or MRI abdomen. When the duodenal involvement is encountered intraoperatively, the decision to perform pancreaticoduodenectomy, which is often considered as the only viable option, should not be rushed into immediately; rather, the operating surgeon should take a time-out and re-assess whether a PPLDR can be performed safely without compromising the oncological adequacy and radicality. This depends upon tumor location and the extent of involvement of the duodenal circumference. A wedge (sleeve) resection can be done if the tumor is located in D1-D3 and less than one-third of the circumference is involved. Tumors in D3, D4 and the proximal jejunum require segmental resection of one or more duodenal segments with anastomosis (Fig. 5).
Reconstruction after PPLDR depends upon the type of resection. A small defect in the duodenal wall after a wedge (sleeve) duodenal resection can be closed primarily without a risk of stricture. A large defect in the duodenal wall can be covered with a jejunal serosal patch (loop) (without mucosal anastomosis). Jejunal patch has been well described for large/giant duodenal perforations but has been rarely used after limited wedge (sleeve) duodenal resection. It prevents the formation of a circulating loop in mucosal anastomosis and also avoids a formal Roux-en-Y anastomosis.
End-to-end, end-to-side, and side-to-side duodeno-jejunal anastomoses are the various types of reconstruction that can be performed after segmental duodenal resection. We preferred a side-to-side duodeno-jejunal anastomosis (Fig. 6) in a majority of our patients because it is technically easy to perform, without the need for sutures on the mesenteric side, and provides a wide stoma. Dorcaratto et al. [9], in their series of 11 patients reported additional complications and longer postoperative stay in patients with end-to-side compared with end-to-end anastomoses, while another series of side-to-side duodeno-jejunal anastomoses reported from India [7] did not encounter any leak-related morbidity, similar to our results. It is not possible to comment on the relative superiority of reconstruction techniques because of the limited number of studies including small number of patients investigated.
We did not encounter any anastomotic (duodeno-jejunal) leak-related morbidity in our series. Two patients had DGE, which was also managed without any significant increase in the hospital stay. One major complication in our series was due to a leak from the esophago-gastric anastomosis (case no. 6) requiring percutaneous intervention. None of our patients required reoperation. Dorcaratto et al. [9] reported major complications in two out of 9 patients following primary anastomosis (end-to-end and end-to-side). In contrast, we and another series from a high-volume center in India did not encounter any morbidity related to side-to-side duodeno-jejunal anastomosis [7], thus emphasizing that side-to-side anastomosis is comparable to other techniques. Notably, a feeding jejunostomy was performed in the majority of the patients in our study except those who had primary closure after wedge (sleeve) resection. This approach ensured early enteral feeding, thus providing crucial nutritional support in the early postoperative period, despite leak-related morbidity. Feeding jejunostomy is recommended in any patient with a precarious duodenal suture line and is performed routinely in pancreaticoduodenectomy.
Surgical resection is the mainstay of treatment for duodenal GIST diagnosed pre-operatively. A wide local excision with negative margins is sufficient as these tumors are well-encapsulated and rarely show lymphatic spread. Hence, routine lymphadenectomy is not recommended unless the lymph nodes are grossly enlarged on preoperative imaging or during surgery [10,11]. Studies have shown similar long-term outcome and survival with limited duodenal resection when compared with pancreaticoduodenectomy for duodenal GIST [9,12].
Limited duodenal resection for colon carcinoma with direct infiltration or malignant colo-duodenal fistula has been extensively described in literature with good outcome and equivalent survival as compared to more radical resections such as pancreaticoduodenectomy along with colonic resection [13-16]. In a series by Gupta et al. [17], five out of nine patients with malignant colo-duodenal fistula underwent sleeve resection of duodenum with R0 resection status and good outcome. However, the data related to gall bladder cancer with duodenal involvement is limited. A large series from India reported sleeve resection of the duodenum in 16 out of 26 patients (61.5%) with gall bladder cancer with duodenal involvement and concluded that duodenal infiltration in gall bladder cancer is not an indicator of unresectability or pancreaticoduodenectomy [18].
It is difficult to identify duodenal involvement preoperatively in case of a large retroperitoneal tumor as most often such large tumors generate pressure and symptoms of upper gastrointestinal obstruction. Limited duodenal resection can be safely performed when the duodenal involvement is found intra-operatively, depending upon the duodenal length, segments and the circumference involved. A case series of 15 patients from Italy describing the short-term outcome of duodenal resection for retroperitoneal sarcoma, however, concluded that segmental resection of duodenum was frequently associated with anastomotic leak-related morbidity (21% vs. 0%) than wedge (sleeve) resection [19].
Primary adenocarcinoma of the fourth segment of the duodenum and the proximal jejunum can also be safely resected with limited (distal) duodenal resection, especially when the tumor is small and the small bowel mesentery and the head of the pancreas/uncinate process are not involved. Many studies comparing pancreaticoduodenectomy with limited duodenal resection have reported equivalent long-term outcome and overall survival with less morbidity [20,21]. A recent propensity-matched analysis of 2,487 patients comparing radical resection with partial resection for duodenal adenocarcinoma concluded that adjuvant therapy in addition to surgery improved survival regardless of the type of surgery and played a significant role in survival [22]. R0 resection was achieved in all of our patients with duodenal adenocarcinoma who underwent PPLDR. Hence these series and our experience corroborate the feasibility and oncological adequacy of PPLDR for such tumors.
A major limitation of our study is the small number of patients and heterogeneity of primary (benign and malignant) tumors. Unfortunately, the paucity of resectable duodenal tumors even in high-volume and specialized gastrointestinal/oncology units limit the possibility of a large series or any future randomized study. Meanwhile, series such as ours and others [8,9] represent high-quality evidence. Future studies are also required to explore the outcomes of PPLDR with a minimally invasive (laparoscopic/robotic) approach. In patients with benign or low-grade malignant primary tumors of the duodenum and cancers of adjacent organs or the retroperitoneum involving the duodenum, PPLDR is an easier and safer but oncologically adequate alternative to pancreaticoduodenectomy. We did not compare the results of PPLDR with those of pancreaticoduodenectomy due to the differences in the indications for PPLDR and pancreaticoduodenectomy, as described above. Our median follow-up was only 23 months but it is well known that most recurrences occur in the first 24 months. Further, we recommend PPLDR for benign tumors or tumors with low malignancy potential.
ACKNOWLEDGEMENTS
Authors would like to acknowledge Mr. Deepak Sharma for his perennial support in obtaining and maintaining patient records.
REFERENCES
1. Dindo D, Demartines N, Clavien PA. 2004; Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 240:205–213. DOI: 10.1097/01.sla.0000133083.54934.ae. PMID: 15273542. PMCID: PMC1360123.
2. Nakayama Y, Konishi M, Gotohda N, Kato Y, Aizawa H, Kudo M, et al. 2017; Comparison of postoperative early and late complications between pancreas-sparing duodenectomy and pancreatoduodenectomy. Surg Today. 47:705–711. DOI: 10.1007/s00595-016-1418-1. PMID: 27654454.

3. Nagai H, Hyodo M, Kurihara K, Ohki J, Yasuda T, Kasahara K, et al. 1999; Pancreas-sparing duodenectomy: classification, indication and procedures. Hepatogastroenterology. 46:1953–1958. PMID: 10430376.
4. Eisenberger CF, Knoefel WT, Peiper M, Yekebas EF, Hosch SB, Busch C, et al. 2004; Pancreas-sparing duodenectomy in duodenal pathology: indications and results. Hepatogastroenterology. 51:727–731. PMID: 15143902.
5. Burasakarn P, Higuchi R, Nunobe S, Kanaji S, Eguchi H, Okada KI, et al. 2021; Limited resection vs. pancreaticoduodenectomy for primary duodenal adenocarcinoma: a systematic review and meta-analysis. Int J Clin Oncol. 26:450–460. DOI: 10.1007/s10147-020-01840-5. PMID: 33386555.

6. Maher MM, Yeo CJ, Lillemoe KD, Roberts JR, Cameron JL. 1996; Pancreas-sparing duodenectomy for infra-ampullary duodenal pathology. Am J Surg. 171:62–67. DOI: 10.1016/S0002-9610(99)80075-0. PMID: 8554153.

7. Golhar A, Mangla V, Mehrotra S, Lalwani S, Mehta N, Nundy S. 2018; Limited distal duodenal resection: surgical approach and outcomes. A case series. Ann Med Surg (Lond). 30:36–41. DOI: 10.1016/j.amsu.2018.04.005. PMID: 30013770. PMCID: PMC6019849.

8. Konishi M, Kinoshita T, Nakagohri T, Takahashi S, Gotohda N, Ryu M. 2007; Pancreas-sparing duodenectomy for duodenal neoplasms including malignancies. Hepatogastroenterology. 54:753–757. PMID: 17591055.
9. Dorcaratto D, Heneghan HM, Fiore B, Awan F, Maguire D, Geoghegan J, et al. 2015; Segmental duodenal resection: indications, surgical techniques and postoperative outcomes. J Gastrointest Surg. 19:736–742. DOI: 10.1007/s11605-015-2744-0. PMID: 25595309.

10. Zhou B, Zhang M, Wu J, Yan S, Zhou J, Zheng S. 2013; Pancreaticoduodenectomy versus local resection in the treatment of gastrointestinal stromal tumors of the duodenum. World J Surg Oncol. 11:196. DOI: 10.1186/1477-7819-11-196. PMID: 23945012. PMCID: PMC3751193.

11. Chung JC, Chu CW, Cho GS, Shin EJ, Lim CW, Kim HC, et al. 2010; Management and outcome of gastrointestinal stromal tumors of the duodenum. J Gastrointest Surg. 14:880–883. DOI: 10.1007/s11605-010-1170-6. PMID: 20140534.

12. Liang X, Yu H, Zhu LH, Wang XF, Cai XJ. 2013; Gastrointestinal stromal tumors of the duodenum: surgical management and survival results. World J Gastroenterol. 19:6000–6010. DOI: 10.3748/wjg.v19.i36.6000. PMID: 24106400. PMCID: PMC3785621.

13. Koea JB, Conlon K, Paty PB, Guillem JG, Cohen AM. 2000; Pancreatic or duodenal resection or both for advanced carcinoma of the right colon: is it justified? Dis Colon Rectum. 43:460–465. DOI: 10.1007/BF02237187. PMID: 10789739.

14. Hakimi AN, Rosing DK, Stabile BE, Petrie BA. 2007; En bloc resection of the duodenum for locally advanced right colon adenocarcinoma. Am Surg. 73:1063–1066. DOI: 10.1177/000313480707301031. PMID: 17983082.

15. Kamath AS, Iqbal CW, Pham TH, Wolff BG, Chua HK, Donohue JH, et al. 2011; Management and outcomes of primary coloduodenal fistulas. J Gastrointest Surg. 15:1706–1711. DOI: 10.1007/s11605-011-1630-7. PMID: 21826549.

16. Lianwen Y, Jianping Z, Guoshun S, Dongcai L, Jiapeng Z. 2009; Surgical treatment for right colon cancer directly invading the duodenum. Am Surg. 75:385–388. DOI: 10.1177/000313480907500507. PMID: 19445288.

17. Gupta V, Kurdia KC, Kumar P, Yadav TD, Gulati A, Sinha SK, et al. 2018; Malignant colo-duodenal fistula: management based on proposed classification. Updates Surg. 70:449–458. DOI: 10.1007/s13304-018-0570-0. PMID: 30054817.

18. Agarwal AK, Mandal S, Singh S, Sakhuja P, Puri S. 2007; Gallbladder cancer with duodenal infiltration: is it still resectable? J Gastrointest Surg. 11:1722–1727. DOI: 10.1007/s11605-007-0320-y. PMID: 17906907.

19. Cananzi FCM, Ruspi L, Samà L, Sicoli F, Gentile D, Minerva EM, et al. 2019; Short-term outcomes after duodenal surgery for mesenchymal tumors: a retrospective analysis from a single tertiary referral center. Updates Surg. 71:451–456. DOI: 10.1007/s13304-019-00667-8. PMID: 31270684.

20. Bakaeen FG, Murr MM, Sarr MG, Thompson GB, Farnell MB, Nagorney DM, et al. 2000; What prognostic factors are important in duodenal adenocarcinoma? Arch Surg. 135:635–641. discussion 641–642. DOI: 10.1001/archsurg.135.6.635. PMID: 10843358.

21. Mitchell WK, Thomas PF, Zaitoun AM, Brooks AJ, Lobo DN. 2017; Pancreas preserving distal duodenectomy: a versatile operation for a range of infra-papillary pathologies. World J Gastroenterol. 23:4252–4261. DOI: 10.3748/wjg.v23.i23.4252. PMID: 28694665. PMCID: PMC5483499.

22. Platoff RM, Kellish AS, Hakim A, Gaughan JP, Atabek UM, Spitz FR, et al. 2021; Simple versus radical resection for duodenal adenocarcinoma: a propensity score matched analysis of National Cancer Database. Am Surg. 87:266–275. DOI: 10.1177/0003134820951432. PMID: 32927979.

Fig. 1
Diagrammatic representation of surgical procedures. (A) Primary repair of a minor defect in duodenal wall. (B) Jejunal serosal (loop) patch repair of large defect in the duodenal wall. (C) End-toend duodenojejunostomy. (D) Side-to-side duodenojejunostomy.

Fig. 2
(A, B) Computed tomography image of primary jejunal adenocarcinoma (arrows). (C) Intra-operative image showing jejunal tumor after mobilization of duodeno-jejunal flexure. (D, E) Resected specimen showing jejunal tumor.
Fig. 3
(A, B) Computed tomography images of large retroperitoneal sarcoma. (C, D) Intra-operative image showing large retroperitoneal sarcoma with focal duodenal involvement (arrows).
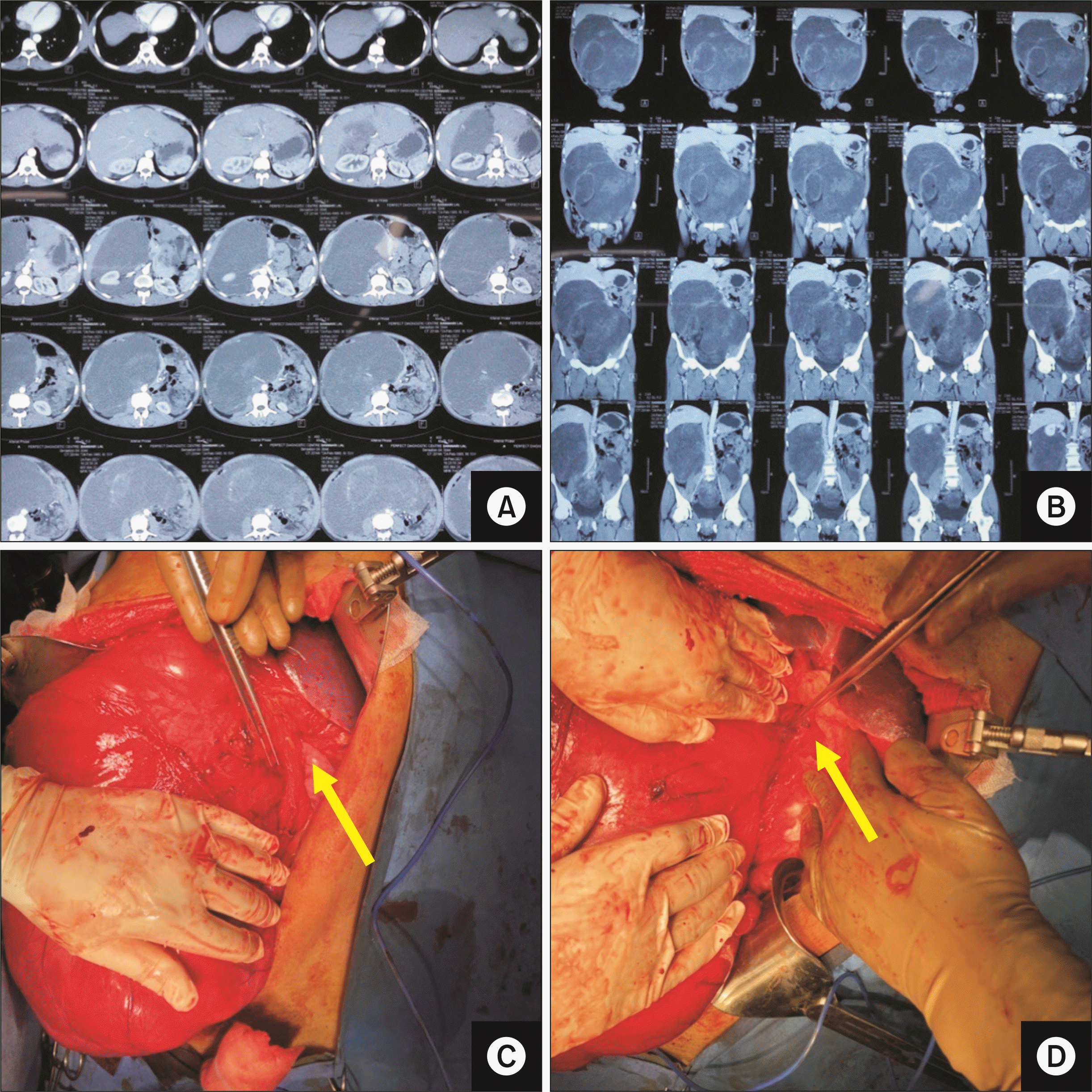
Fig. 4
(A) Computed tomography (CT) image showing hepatic flexure growth with colo-duodenal fistula (arrow). (B) Coronal section of CT scan showing colo-duodenal fistula (arrow). (C) Intra-operative image showing duodenal involvement (specimen retracted by the first assistant). (D) Jejunal patch in progress (side-to-side loop). (E) Resected specimen showing hepatic flexure colonic growth with duodenal fistula.
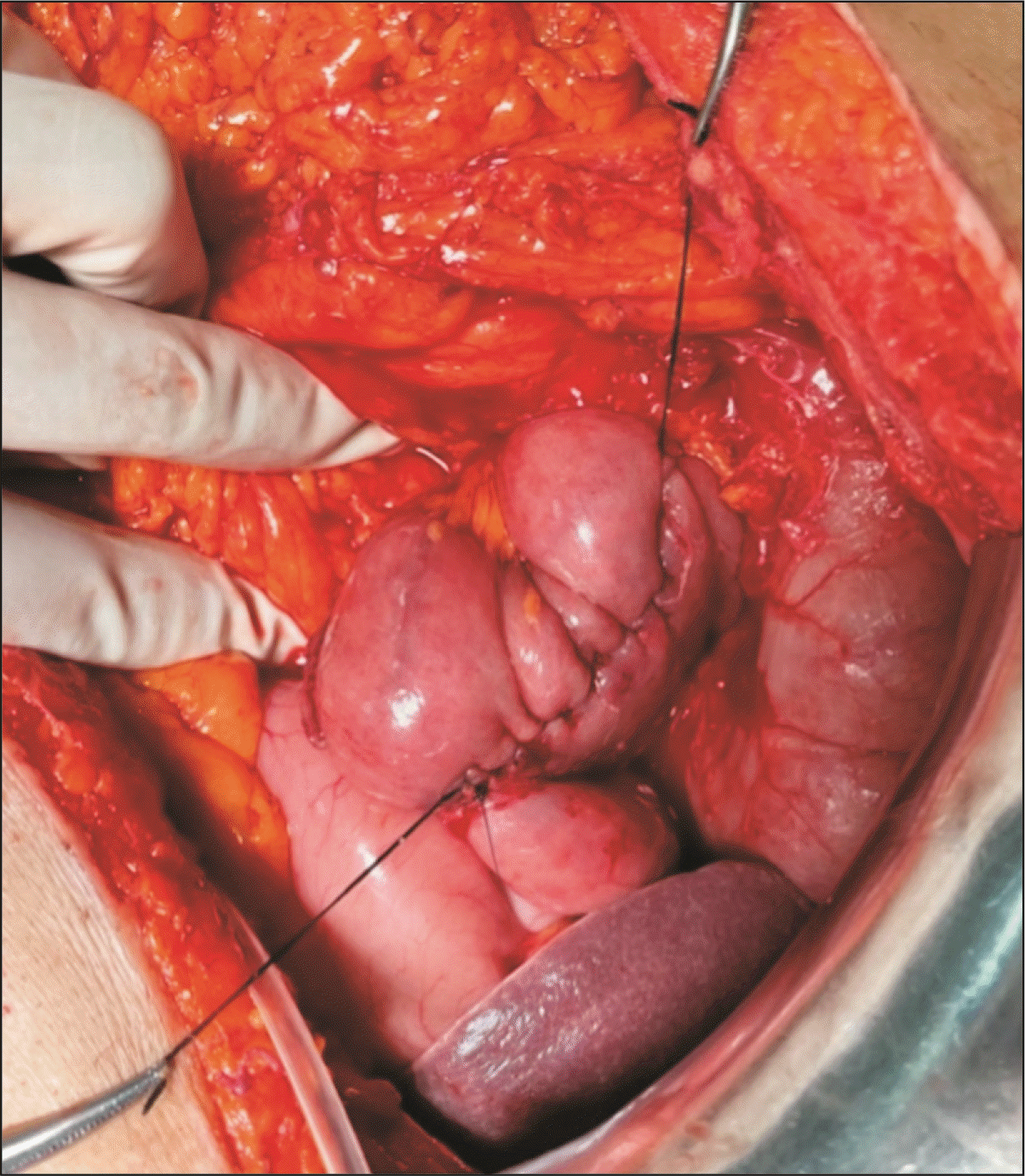
Fig. 5
Algorithm for management of duodenal pathologies requiring pancreas-preserving limited duodenal resection (PPLDR).

Table 1
Characteristics of patients who underwent pancreas-preserving limited duodenal resection (PPLDR)




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download