Abstract
Objective
This cross-sectional study aimed to investigate the characteristics of malocclusions in scoliotic patients through clinical examinations.
Methods
Fifty-eight patients with idiopathic scoliosis (IS) and 48 patients with congenital scoliosis (CS) participated in the study. A randomly selected group of 152 orthopedically healthy children served as the control group. Standardized orthodontic and orthopedic examination protocols were used to record the occlusal patterns and type of scoliosis. Assessments were made by three experienced orthodontists and a spinal surgery team. The differences in the frequency distribution of occlusal patterns were evaluated by the chi-squared test.
Results
In comparison with patients showing IS, patients with CS showed a higher incidence of Cobb angle ≥ 45° (p = 0.020) and included a higher proportion of patients receiving surgical treatments (p < 0.001). The distribution of the Angle Class II subgroup was significantly higher in the IS (p < 0.001) and CS (p = 0.031) groups than in the control group. In comparison with the healthy controls, the CS and IS groups showed significantly higher (p < 0.05) frequencies of asymmetric molar and asymmetric canine relationships, upper and lower middle line deviations, anterior deep overbite, unilateral posterior crossbite, and canted occlusal plane, with the frequencies being especially higher in CS patients and to a lesser extent in IS patients.
Scoliosis is a three-dimensional deviation of the spinal axis and an orthopedic condition characterized by postural abnormalities,1,2 with the most common type in adolescents in China being idiopathic scoliosis (IS).3 The possible relationship between abnormal body posture and disorders in the oral and maxillofacial systems has been investigated in previous studies.4,5 Hitchcock6 conducted a case study to provide evidence for a possible causal relationship between occlusion and scoliosis. Motoyoshi et al.7 used finite-element analysis to confirm that the distribution of occlusal stress might be related to changes in head and neck posture. A study of scoliosis and spinal deformities suggested that patients with a spinal deformities develop a high incidence of temporomandibular disorder, Angle Class II malocclusion, deep overbite, and deep overjet.8 Lippold et al.9 found that the incidence of Angle Class II malocclusion was higher in preschool children with scoliosis. A subsequent literature review confirmed the increased prevalence of malocclusions in children with scoliosis.10 Identification of the anatomical and functional relationships between the masticatory system and the body posture regulating system led to several hypotheses of correlations between occlusion and postural disturbances.11 Patients with IS always show a coronal curvature of the spine, which grows progressively curved.12 While the majority of cases of IS manifested in adolescence,13 early-onset scoliosis develops before adolescence and is categorized as a subclass of IS, presenting as a developmental disorder of malformation or faulty segmentation of the vertebrae and often occurring in combination with other abnormalities.14,15
Most of the recent research on this topic involved cross-sectional studies that focused on the morphological and functional abnormalities of the stomatognathic system in patients with IS.16,17 However, the dental-occlusal features in patients with congenital scoliosis (CS) have been rarely reported. Therefore, in the present study, we included cases of IS and CS and hypothesized that IS and CS patients have different patterns of malocclusions in comparison with healthy children.
All patients involved in this cross-sectional study received detailed information on orthodontic and orthopedic examinations beforehand. They (or their guardians) provided written consent to participate in the study. The examinations complied with the requirements set by the Ethics Committee of the Seventh Medical Center of PLA General Hospital (study approval number: 2018106).
The study involved patients who were diagnosed with scoliosis from April 2013 to April 2018. The patients underwent clinical examinations by spinal surgeons and orthodontists, who took radiographic images of the entire spine and computed tomography (CT) images for further diagnoses. Twenty patients were excluded because of a history of orthodontic treatment, cleft lip and palate, maxillofacial fracture, trauma, infection, or severe dental crowding. Healthy volunteers were recruited from the local junior and senior middle schools as the control group under the following selection criteria: natural complete dentition; orthopedically healthy; no history of orthodontic treatment; and no maxillofacial deformities. The incidence of malocclusion patterns was indicated as frequency or percentage values.
The occlusion variables for each individual were evaluated by three orthodontists. To ensure the accuracy of examination results, orthodontists who had undergone training in advance and had > 5 years of experience conducted the evaluations. In cases involving inconsistencies in the dental examination findings recorded by the orthodontists, the majority opinion was determined as the final record, or a case discussion was conducted to reach an agreement, and thereby address potential sources of bias.
The following issues were considered and included in the data records:
(1) Dentition development stage: primary, transitional, or permanent dentition
(2) Sagittal dimension: canine relationship, molar relationship, and Angle’s classification, which was categorized as Class I occlusion (a centric occlusion in which the mesiobuccal cusp of the maxillary first molar occludes the buccal groove of the mandibular first molar) or Class II occlusion (a retrognathic positional relationship in which the mesiobuccal cusp of the maxillary first molar occludes anterior to the mesial buccal groove of the mandibular first molar). The Angle Class II subgroups included cases with Angle Class II on one side and Angle Class I or III on the other side. Angle Class III occlusion referred to a prognathic positional relationship in which the mesiobuccal cusp of the maxillary first molar occluded posterior to the buccal groove of the mandibular first molar.
(3) Transverse dimension: upper midline deviation, lower midline deviation, posterior crossbite
(4) Vertical dimension: occlusal plane inclination, anterior and posterior overbite
(5) Other evaluations: spacing, crowding, loss of tooth, oral habits, or caries, which may influence inter-arch relationships.
Orthopedic examinations and diagnoses were performed by a team of spinal surgeons, who conducted physical examinations and X-ray assessments of the spine and recorded the patients’ medical history. The following parameters were primarily determined in this epidemiological study.
(1) Type of scoliosis. CS or IS was diagnosed by orthopedists based on the full-length anteroposterior and lateral X-ray spine images, 3-dimensional CT spine reconstructions, and clinical manifestations. In addition, the patients’ medical history was evaluated to determine when they developed symptoms, whether they were diagnosed at birth or before their preschool stage (CS cases), or whether they developed symptoms and were diagnosed in the preadolescent period (IS cases). Patients diagnosed with neuromuscular scoliosis or Scheuermann’s disease and conditions other than IS and CS were excluded.
A total of 106 patients with scoliosis, including 58 patients with IS and 48 patients with CS, participated in this study. The proportion of female patients in the IS and CS groups was 87.9% and 60.4%, respectively. The mean ages of patients during the study were 14 years and 8 months in the IS group and 15 years and 3 months in the CS group. Severity was significantly higher in the CS patients, which reflected a greater surgical treatment rate in this group (Table 1). A total of 152 healthy volunteers (mean age: 15 years and 2 months; range, 12 years and 2 months to 18 years and 6 months) served as the controls.
Individual normal occlusion and Class I malocclusion distribution ratio in the CS group was 45.8%, which was significantly lower than that in the control group (p < 0.05), but no significant difference was found between the IS and control groups. However, the Class II subdivision distribution ratio was significantly higher in both the IS (17.2%) and CS (29.2%) groups in the control group (7.2%) (p < 0.05) (Table 2). The high proportion of patients showing Class II subdivisions indicated sagittal asymmetry of bilateral occlusion in patients with scoliosis.
In assessments performed in the sagittal dimension, the incidences of asymmetry in the molar relationship (29.2%) and canine relationship (29.8%) were significantly higher in the CS group (p < 0.05). Moreover, the proportion of asymmetric molar relationships in the IS group was 17.2%, which was significantly higher than that (7.9%) in the control group. Two cases in the IS group, one case in the CS group, and four cases in the control group were excluded from the statistical data on canine relationships, because the orthodontists were unable to obtain accurate records due to embedded or lost canines.
In assessments performed in the transverse dimension, the incidence of lower midline deviation in the IS and CS groups was 39.7% and 45.8% respectively, and they were both higher than the value in the control group (25.7%; p < 0.05). In contrast, a significant difference in the proportion of upper midline deviations was found only between the CS and control groups (p = 0.034). The incidence of upper midline deviations in the IS group was 25.9% compared to 17.1% in the control group (p = 0.152). Moreover, unilateral posterior crossbite was more frequent in both the IS (19.0%, p = 0.034) and CS (27.1%, p = 0.001) groups in comparison with the control group (8.6%).
In assessments performed in the vertical dimension, the proportions of cases showing a canted occlusal plane in both the IS (20.7%, p = 0.036) and CS (27.1%, p = 0.003) groups were higher than those in the control group (9.9%). Anterior deep overbite appeared more frequently in the CS group, but its incidence did not differ significantly between the IS and control groups. Figure 1 presents the X-ray and dental images of an 18-year-old female patient with severe CS, whose thoracic spine was severely deformed and twisted. The patient also showed a unilateral (right side) Angle Class II subgroup occlusion.
The sex and severity distributions highlighted in this study were similar to those reported previously.15,20 The Class II subdivision distribution ratio was significantly higher in both the IS and CS groups in comparison with the control group, indicating sagittal asymmetry of bilateral occlusion in patients with scoliosis (Table 2).
Seven parameters21 were applied to represent the asymmetric occlusal patterns in three dimensions in this research. The incidence of all of these asymmetric occlusal patterns was significantly higher in the CS group than in the control group. In the IS group, incidences of these asymmetric occlusal patterns, except the canine relationship, upper middle line deviation, and deep overbite, were statistically higher, which indicated that idiopathic patients suffered less occlusal asymmetric deformity compared to patients with CS to some extent. These findings were presumably related to the minor spinal deformity and a shorter course of IS. Another possibility contributing to these findings was the small number of cases evaluated in the study.
Although bilateral asymmetries are accepted to be a common feature of occlusions,16,17,21 opinions about the etiology of occlusal asymmetries differ. A cross-sectional study by Lewandowska et al.16 confirmed bilateral dentoalveolar asymmetries in patients with adolescent IS. However, another IS study17 reported a functional lateral mandibular displacement in two individuals. At present, methods to evaluate dental/facial asymmetric features in scoliotic patients include clinical dental examination and measurements of full-mouth dental casts or posterior-anterior cephalograms. The authors believe that further studies should focus on the 3-dimensional asymmetry of the maxillofacial skeleton, since its growth and developmental tendency vary with the progress of scoliosis. To investigate the changes in the degree of malocclusion with age in patients with scoliosis, participants should be grouped by age in future studies.
Several authors have tried to establish possible connections among the location, direction, and severity of scoliosis and dentofacial anomalies. One study demonstrated a correlation between the left proximal thoracic curve of scoliosis and the anterior partial open bite.17 Another study evaluating patients with mandibular deviation also confirmed that the direction of mandibular deviation was the same as the lateral bending of the thoracolumbar vertebrae, which was opposite to the lateral bending of the cervical vertebrae.22 However, hypotheses describing the correlations between scoliosis and occlusion have varied in recent decades.10,23-26 This correlation was assumed to be based on the anatomic and functional connections between the stomatognathic complex and the cervical vertebra. An anatomic connection refers to the muscular and ligament attachments between the craniofacial complex and the cervical vertebra, while functional connections among the cranium, mandible, and cervical vertebra are adjusted by visual balance and a gravity effect. Muscular balance between the neck and masticatory system has been demonstrated to play an essential role in the relationship between asymmetric malocclusion and scoliosis.27,28 Kondo29 found that early improvement in occlusion, combined with physiotherapy to achieve muscular balance of the neck and masticatory system, was effective for improvement of muscular function asymmetry. Thus, early correction of muscular torticollis should be considered to prevent the progression of facial asymmetry in congenital muscular torticollis patients.30 These findings indicate the possibility of an interaction effect between the masticatory system and body posture.
However, this study had a number of limitations. Although 16 adolescents with scoliosis were excluded because of severe crowding, even mild crowding can potentially influence occlusal patterns, resulting in a systematic error. Moreover, the exclusion of orthodontic patients with scoliosis may have introduced bias to the results. Despite these limitations, the conclusions remain reliable since only two patients with scoliosis were excluded in this study.
The results of this cross-sectional study partially confirmed the findings of previous studies that reported a higher frequency of dentofacial deviations in adolescents with various orthopedic problems. Both IS and CS groups showed significant differences in the severity and frequency of asymmetric occlusions in comparison with the control group. In addition, more severe dentofacial deviations were observed in CS than in IS patients, indicating that asymmetric malocclusions in adolescents may serve as a reminder for both parents and medical staff to evaluate patients for potential orthopedic problems, thereby facilitating early detection and treatment of these problems.
ACKNOWLEDGEMENTS
This work was financially supported by grants from the Open Project of State Key Laboratory of Military Stomatology (grant no. 2020KB04) and the Clinical Technology Project of AFMU (grant no. LX2021-312). We appreciate the assistance provided by the staff in the Department of Orthopedics, Xijing Hospital for collection and diagnosis of scoliosis cases. We would also like to thank Dr. Liang Fei for assisting with the statistical analyses.
REFERENCES
1. Karimi MT, Rabczuk T. 2018; Scoliosis conservative treatment: a review of literature. J Craniovertebr Junction Spine. 9:3–8.
2. Shakil H, Iqbal ZA, Al-Ghadir AH. 2014; Scoliosis: review of types of curves, etiological theories and conservative treatment. J Back Musculoskelet Rehabil. 27:111–5. DOI: 10.3233/BMR-130438. PMID: 24284269.

3. Qiu GX. 2017; Scoliosis in China: history and present status. Chin Med J (Engl). 130:2521–3. DOI: 10.4103/0366-6999.217081. PMID: 29067948. PMCID: PMC5678247.
4. Korbmacher H, Koch L, Eggers-Stroeder G, Kahl-Nieke B. 2007; Associations between orthopaedic disturbances and unilateral crossbite in children with asymmetry of the upper cervical spine. Eur J Orthod. 29:100–4. DOI: 10.1093/ejo/cjl066. PMID: 17290022.

5. Shakeel A, Asim HM, Ahmad N, Aziz A. 2018; Idiopathic scoliosis in secondary school girls: a screening programme. J Coll Physicians Surg Pak. 28:726. DOI: 10.29271/jcpsp.2018.09.726. PMID: 30158047.

6. Hitchcock HP. 1969; Treatment of a malocclusion associated with scoliosis. Angle Orthod. 39:64–8. DOI: 10.1043/0003-3219(1969)039<0064:TOAMAW>2.0.CO;2. PMID: 5250527.
7. Motoyoshi M, Shimazaki T, Sugai T, Namura S. 2002; Biomechanical influences of head posture on occlusion: an experimental study using finite element analysis. Eur J Orthod. 24:319–26. DOI: 10.1093/ejo/24.4.319. PMID: 12198861.

8. Segatto E, Lippold C, Végh A. 2008; Craniofacial features of children with spinal deformities. BMC Musculoskelet Disord. 9:169. DOI: 10.1186/1471-2474-9-169. PMID: 19102760. PMCID: PMC2637865.

9. Lippold C, van den Bos L, Hohoff A, Danesh G, Ehmer U. 2003; Interdisciplinary study of orthopedic and orthodontic findings in pre-school infants. J Orofac Orthop. 64:330–40. DOI: 10.1007/s00056-003-0236-4. PMID: 14692047.

10. Saccucci M, Tettamanti L, Mummolo S, Polimeni A, Festa F, Tecco S. 2011; Scoliosis and dental occlusion: a review of the literature. Scoliosis. 6:15. DOI: 10.1186/1748-7161-6-15. PMID: 21801357. PMCID: PMC3162939.

11. Hong JY, Suh SW, Modi HN, Yang JH, Hwang YC, Lee DY, et al. 2011; Correlation between facial asymmetry, shoulder imbalance, and adolescent idiopathic scoliosis. Orthopedics. 34:187. DOI: 10.3928/01477447-20110427-14. PMID: 21667906.

12. He C, Wong MS. 2018; Spinal flexibility assessment on the patients with adolescent idiopathic scoliosis: a literature review. Spine (Phila Pa 1976). 43:E250–8. DOI: 10.1097/BRS.0000000000002276. PMID: 28604491.
13. Shen J, Parent S, Wu J, Aubin CÉ, Mac-Thiong JM, Kadoury S, et al. 2020; Towards a new 3D classification for adolescent idiopathic scoliosis. Spine Deform. 8:387–96. DOI: 10.1007/s43390-020-00051-2. PMID: 32026444.

14. Alsiddiky AM. 2015; An insight into early onset of scoliosis: new update information- a review. Eur Rev Med Pharmacol Sci. 19:2750–65. PMID: 26241527.
15. Mackel CE, Jada A, Samdani AF, Stephen JH, Bennett JT, Baaj AA, et al. 2018; A comprehensive review of the diagnosis and management of congenital scoliosis. Childs Nerv Syst. 34:2155–71. DOI: 10.1007/s00381-018-3915-6. PMID: 30078055.

16. Lewandowska J, Opydo-Szymaczek J, Mehr K, Głowacki J. 2019; Bilateral dentoalveolar asymmetries in female patients with adolescent idiopathic scoliosis. Acta Bioeng Biomech. 21:53–62. DOI: 10.37190/ABB-01457-2019-01. PMID: 32022798.

17. Laskowska M, Olczak-Kowalczyk D, Zadurska M, Czubak J, Czubak-Wrzosek M, Walerzak M, et al. 2019; Evaluation of a relationship between malocclusion and idiopathic scoliosis in children and adolescents. J Child Orthop. 13:600–6. DOI: 10.1302/1863-2548.13.190100. PMID: 31908677. PMCID: PMC6924124.

18. Dubousset J. 2020; Past, present, and future in pediatric spinal surgery. Ann Transl Med. 8:36. DOI: 10.21037/atm.2019.08.13. PMID: 32055627. PMCID: PMC6995910.

19. Kuznia AL, Hernandez AK, Lee LU. 2020; Adolescent idiopathic scoliosis: common questions and answers. Am Fam Physician. 101:19–23.
20. Yaman O, Dalbayrak S. 2014; Idiopathic scoliosis. Turk Neurosurg. 24:646–57. DOI: 10.5137/1019-5149.JTN.8838-13.0. PMID: 25269032.

21. Ben-Bassat Y, Yitschaky M, Kaplan L, Brin I. 2006; Occlusal patterns in patients with idiopathic scoliosis. Am J Orthod Dentofacial Orthop. 130:629–33. DOI: 10.1016/j.ajodo.2005.01.032. PMID: 17110260.

22. Zhou S, Yan J, Da H, Yang Y, Wang N, Wang W, et al. 2013; A correlational study of scoliosis and trunk balance in adult patients with mandibular deviation. PLoS One. 8:e59929. DOI: 10.1371/journal.pone.0059929. PMID: 23555836. PMCID: PMC3612109. PMID: 1d06faeef8544b1abde7d6ea3a84a043.

23. Michelotti A, Manzo P, Farella M, Martina R. 1999; [Occlusion and posture: is there evidence of correlation?]. Minerva Stomatol. 48:525–34. Italian. PMID: 10768011.
24. Kim TH, Kim JH, Kim YJ, Cho IS, Lim YK, Lee DY. 2014; The relation between idiopathic scoliosis and the frontal and lateral facial form. Korean J Orthod. 44:254–62. DOI: 10.4041/kjod.2014.44.5.254. PMID: 25309865. PMCID: PMC4192527.

25. Jeong KY, Min KJ, Woo J, Yim SY. 2015; Craniofacial asymmetry in adults with neglected congenital muscular torticollis. Ann Rehabil Med. 39:440–50. DOI: 10.5535/arm.2015.39.3.440. PMID: 26161351. PMCID: PMC4496516.

26. Végh A, Fábian G, Jianu R, Segatto E. 2012; Orofacial characteristics of adolescents with diagnosed spinal disorders. Biomed Tech (Berl). 57:65–9. DOI: 10.1515/bmt-2011-0036. PMID: 22718594.

27. Tecco S, Mummolo S, Marchetti E, Tetè S, Campanella V, Gatto R, et al. 2011; sEMG activity of masticatory, neck, and trunk muscles during the treatment of scoliosis with functional braces. A longitudinal controlled study. J Electromyogr Kinesiol. 21:885–92. DOI: 10.1016/j.jelekin.2011.08.004. PMID: 21889363.

28. Saifuddin M, Miyamoto K, Ueda HM, Shikata N, Tanne K. 2003; An electromyographic evaluation of the bilateral symmetry and nature of masticatory muscle activity in jaw deformity patients during normal daily activities. J Oral Rehabil. 30:578–86. DOI: 10.1046/j.1365-2842.2003.00991.x. PMID: 12787454.

29. Kondo E. 2004; Features and treatment of skeletal class III malocclusion with severe lateral mandibular shift and asymmetric vertical dimension. World J Orthod. 5:9–24. PMID: 15615138.
30. Seo SJ, Yim SY, Lee IJ, Han DH, Kim CS, Lim H, et al. 2013; Is craniofacial asymmetry progressive in untreated congenital muscular torticollis? Plast Reconstr Surg. 132:407–13. DOI: 10.1097/PRS.0b013e3182959e30. PMID: 23584628.

Figure 1
X-ray and dental images of an 18-year-old female patient with congenital scoliosis and an Angle Class II subgroup classification. A, Full-length anteroposterior spine X-ray image showing a severely deformed and twisted spine. B, Dental image showing normal mandibular occlusion on the right side. C, Dental image showing an oblique occlusal plane. D, Dental image showing mandibular deviation on the left side.
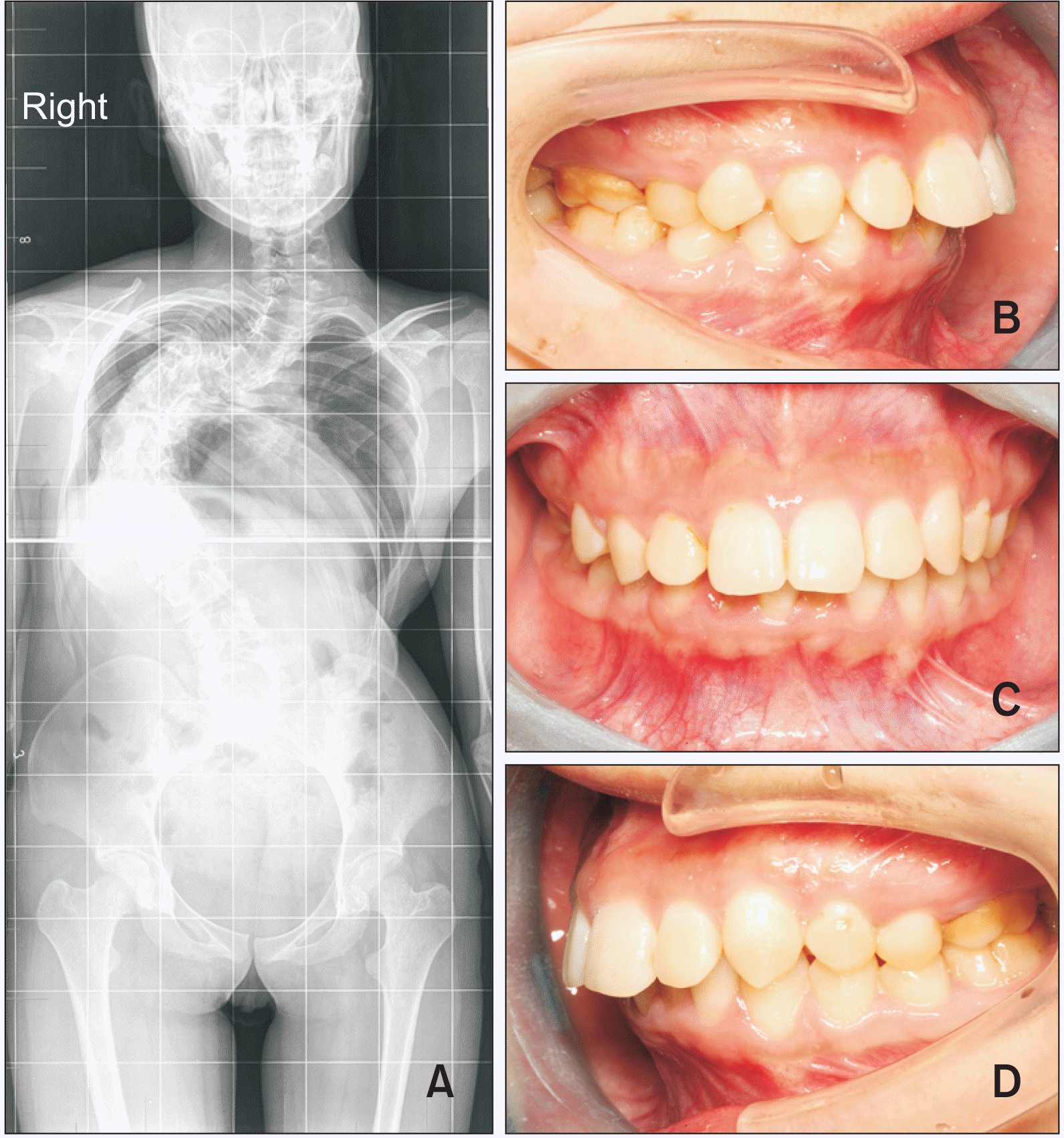
Table 1
Sex distribution, age, severity distribution, and treatment method distribution in patients with scoliosis
| Variable | IS group (n = 58) | CS group (n = 48) | p-value |
|---|---|---|---|
| Sex distribution | 0.001** | ||
| Male | 7 (12.1) | 19 (39.6) | |
| Female | 51 (87.9) | 29 (60.4) | |
| Age | - | ||
| Mean | 14Y8M | 15Y3M | |
| Min–max | 12Y4M–20Y2M | 10Y5M–23Y6M | |
| Severity distribution | 0.020* | ||
| Cobb angle ≥ 45° | 22 (37.9) | 31 (64.6) | |
| Cobb angle < 45° | 36 (62.1) | 17 (35.4) | |
| Treatment method distribution | < 0.001** | ||
| Surgical treatment | 20 (34.5) | 42 (87.5) | |
| Physical therapy | 38 (65.5) | 6 (12.5) |
Table 2
Distribution of angle classification in the idiopathic scoliosis, congenital scoliosis, and control groups
| Angle classification |
IS group (n = 58) |
CS group (n = 48) |
Control group (n = 152) |
p-value (IS vs. control) |
p-value (CS vs. control) |
p-value (IS vs. CS) |
|||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | ||||||
| Normocclusion and Class I | 34 | 58.6 | 22 | 45.8 | 103 | 67.8 | 0.311 | 0.006** | 0.136 | ||
| Class II | 13 | 22.4 | 10 | 20.8 | 24 | 15.8 | 0.260 | 0.417 | 1.000 | ||
| Class II subgroup | 10 | 17.2 | 14 | 29.2 | 11 | 7.2 | 0.031* | < 0.001** | 0.144 | ||
| Class III | 1 | 1.7 | 2 | 4.2 | 14 | 9.2 | 0.060 | 0.261 | 0.450 | ||
Table 3
Occlusal patterns in the idiopathic scoliosis, congenital scoliosis, and control groups
| Occlusal pattern |
IS group (n = 58) |
CS group (n = 48) |
Control group (n = 152) |
p-value (IS group vs. control) |
p-value (CS group vs. control) |
p-value (IS vs. CS) |
|||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | ||||||
| Asymmetric molar relationship | 10 | 17.2 | 14 | 29.2 | 12 | 7.9 | 0.048** | < 0.001** | 0.144 | ||
| Asymmetric canine relationship | 11 | 19.6 | 14 | 29.8 | 14 | 9.5 | 0.094 | 0.001** | 0.232 | ||
| Deviation of the upper middle line | 15 | 25.9 | 15 | 31.3 | 26 | 17.1 | 0.152 | 0.034* | 0.540 | ||
| Deviation of the lower middle line | 23 | 39.7 | 22 | 45.8 | 39 | 25.7 | 0.047** | 0.008** | 0.522 | ||
| Anterior deep overbite | 21 | 36.2 | 19 | 39.6 | 36 | 23.7 | 0.068 | 0.003** | 0.721 | ||
| Unilateral posterior crossbite | 11 | 19.0 | 13 | 27.1 | 13 | 8.6 | 0.034 | 0.001** | 0.320 | ||
| Canted occlusal plane | 12 | 20.7 | 13 | 27.1 | 15 | 9.9 | 0.036 | 0.003** | 0.440 | ||




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download