Abstract
Purpose
Polydactyly of the foot is a common congenital anomaly. The goal of surgery for polydactyly is to increase similarity to the contralateral foot, with a well-aligned arcade of toes that allows patients to wear normal footwear and ambulate painlessly. Foot appearance is especially important in Asian countries where people remove their shoes indoors. This study reviewed the surgical results in patients who underwent surgery for correction of untreated foot polydactyly after the age of 18 years.
Methods
We retrospectively analyzed the data of 11 patients who underwent surgery between 2006 and 2019. The forefoot width, angulation difference, and toe length ratios between the affected and unaffected feet were compared before and after the operation. In addition, the purpose of the surgery and postoperative cosmetic satisfaction were collected for each patient.
Results
The median age at the time of the operation was 25 years (interquartile range, 22–32 years) and most patients presented with postaxial polydactyly. The primary reasons to undergo surgery were both functional and cosmetic. The forefoot width and angle difference ratios became significantly more similar to the contralateral side postoperatively (p<0.05). No significant difference was found in the toe length ratio. Postoperative Global Aesthetic Improvement Scale scores showed satisfactory results.
Polydactyly of the foot is a common congenital anomaly [1]. Surgical methods and prognosis vary depending on the degree and type of polydactyly. Simple deformities require excision of the extra digit, which is possible as early as postnatal period. For cases in which the bones, joints, and ligaments are intricately connected, surgery is performed when general anesthesia is possible [2-4]. In several Asian countries, people take off their shoes before going indoors and rarely wear shoes inside. Therefore, parents from these cultures prefer their children to undergo foot surgery to treat even minor problems as early as possible [5].
The treatment of polydactyly of the foot has been less highlighted than that of the hand because it causes fewer functional problems. However, when left untreated, it can cause developmental delay related to footwear difficulties, psychological problems related to cosmesis [2,6,7]. In this study, we gathered patients with untreated polydactyly of the foot to obtain reasons for deciding to receive treatment as an adult and also investigate the functional and cosmetic results.
Ethics statement: This study was approved by the Institutional Review Board of Seoul National University College of Medicine (No. 2201-065-1290). Written informed consent was obtained for publication of this article and accompanying images.
Between 2006 and 2019, a total of 361 patients underwent surgery for polydactyly of the foot in our institute. A total of 11 patients with polydactyly of the foot who underwent their first treatment procedure after the age of 18 years were included. Patients who underwent secondary operations (contracture release, 5; soft tissue rearrangement, 4; wedge osteotomy, 4), who could not be reached (n=9), or under the age of 18 years (n=328) were excluded from the study. Demographic information, family history, and treatment details were retrospectively gathered. Cases were classified according to the SAM (syndactylism, axis deviation, metatarsal extension) system [8]. SAM system consists of three categories to classify foot polydactyly: presence of syndactyly, presence of any axis deviation, and extent of metatarsal involvement based on preoperative physical and radiologic examination.
Pre- and postoperative values of forefoot width, angle difference, and toe length were measured on anteroposterior (AP) foot radiographs and compared with each patient’s contralateral, unaffected side [9]. Forefoot width was evaluated by measuring the largest distance between soft tissue margins of the first and fifth (or sixth) metatarsophalangeal joints (Fig. 1A). The orderly alignment of the arcade of the toes was evaluated by comparing the angle difference in the alignment of the toes before and after surgery (Fig. 1B). Two lines connecting the midpoints of the tips of the affected toe and the adjacent toes were drawn on the AP foot radiographs. The angle between the two lines was measured. Preserved toe lengths were measured as the distance between the tips of the distal phalanx and the base of the proximal phalanx (Fig. 1C). Results were evaluated in ratios of affected to unaffected sides for each category. The closer the ratio was to 1, the greater the similarity between the affected and unaffected sides.
Subjective evaluation of the surgical results was defined with a Global Aesthetic Improvement Scale (GAIS) score and used as a reference parameter by the patient. The GAIS is a 5-point scale rating global aesthetic improvement in appearance compared to pretreatment [10]. The rating categories are worse (5 points), no change (4 points), improved (3 points), much improved (2 points), and very much improved (1 point). Also, each patient was asked short answer questions about the purpose of the surgery, and the authors sorted them into ‘functional’ or ‘cosmetic.’
Surgery was performed under tourniquet application. For postaxial polydactyly, the toe to be excised was decided based on the toe length, angular deviation, and arcade of toes. In cases with syndactylism, two toes were separated by an interdigital zigzag incision, taking care not to disrupt the neurovascular bundle. Wedge osteotomy was performed at the proximal phalanx if the toe deviated more than 15° [9]. For skin defects between the toes, full-thickness skin was applied which was harvested from the inguinal area.
Data are presented as median and interquartile range. For the continuous variables, Wilcoxon signed-rank test was applied to compare between pre- and postoperative status. All statistical analyses were performed using the PASW Statistics ver. 18 (IBM Corp., Armonk, NY, USA), and a p-value of <0.05 was considered statistically significant.
The clinical features of the patients and GAIS scores are shown in Table 1. Ten patients had postaxial type polydactyly, among which seven patients had syndactylism. The median age of the operation conducted was 25 years. Patients reported no other underlying diseases except one who had right-hand postaxial syndactyly. Another patient reported a family history of polydactyly of the hand.
The main complaints due to untreated polydactyly of foot were 36.7% functional (n=4) and 63.6% cosmetic (n=7). Functional complaints included discomfort when wearing shoes and recurrent callus formation on the first or fifth toe. Patients who had social consequences of cosmetic problems mainly reported social isolation and the need to hide their feet due to disfiguration. The specific answers of the patients are listed in Table 1.
Of the 10 cases of postaxial polydactyly, six underwent excision of the sixth toe and four of the fifth toe. Seven patients required skin grafting (for S1 and S2) and six required wedge osteotomies of the proximal phalanx. Objective postoperative values are shown in Table 2. Forefoot width and angle difference became significantly similar to the contralateral side postoperatively (p<0.05). There was no significant difference in preserved toe length.
The follow-up period was a median of 7 months. There were no postoperative complications, including wound dehiscence, infection, or graft failure (Figs. 2, 3). However, one case appeared with a hypertrophic scar. No cases revealed any varus or valgus deformities, functional disturbances, or foot pain after surgery until the last follow-up session. The patients’ postoperative GAIS ratings demonstrated overall satisfaction with the treatment.
Polydactyly of the foot is defined as the presence of six or more toes. Duplication occurs at any level from the midfoot to the distal phalanges. Most cases are of the postaxial type with duplicated fifth rays constituting 80% of duplications, and syndactyly is often present [1,5]. Polydactyly of the foot may be present as part of a collection of abnormalities, or it may exist by itself, inherited as an autosomal dominant trait. The most commonly associated condition is polydactyly of the hand, with an incidence of 33% [6].
Polydactyly of the foot can cause both functional and cosmetic abnormalities. Functional abnormalities include difficulty in wearing customary shoes and occasional pain while walking [11]. However, in polydactyly without the involvement of the metatarsal bone, problems are considered more cosmetic than functional. It is a different matter when the metatarsal is involved, as the fifth toe metatarsal head plays a significant role; it sustains the transverse arch of the foot, which functions as a spring and allows smooth walking with weight transfer [12]. Patients in our study were mostly classified as M0 (without metatarsal bone involvement, 64%), and for this group, the focus of the surgery was more cosmetic than functional.
Many studies have reported the importance of appearance as a patient-reported outcome in surgery for congenital differences [13-15]. Normalizing appearance clearly offers benefits, and the success of surgical treatment should not be underestimated. Most studies reported enhanced self-esteem, more positive appearance ratings, and improvements in social confidence following surgery [16,17]. Even without much functional impairment, the affected patients experienced improvements in the GAIS rating. The difficulties most frequently reported by people who are visibly different relate to negative self-perceptions and challenges with social interaction [18]. It has been suggested that the earlier the surgery, the greater the psychological benefit to the child [19,20]. Although this study included cases of foot polydactyly, interviews hint that under the current culture of taking off shoes indoors, patients felt discomfort and isolation due to foot appearance.
The limitations of this study were a small number of cases with no control group, and the results were self-evaluated. However, this study presented postoperative outcomes with objective values and parameters. Measurements showed that forefoot width and alignment of the toe arcade were significantly similar to those of the contralateral foot postoperatively. In addition, through surveys with the adults, opinions on the inconvenience of congenital deformity and the reasons for surgery were clearly conveyed.
The deformities may have been neglected until adulthood because this group of patients had no functional problems. However, patients experienced social issues arising from being different and eventually sought treatment.
References
1. Kelly DM, Mahmoud K, Mauck BM. Polydactyly of the foot: a review. J Am Acad Orthop Surg. 2021; 29:361–9.

2. Cetik O, Uslu M, Cirpar M, Eksioglu F. Experience with the surgical treatment of radial polydactyly in adults. Ann Plast Surg. 2005; 55:363–6.

3. Light T, Buck-Gramcko D. Polydactyly: terminology and classification. In : Buck-Gramcko D, editor. Congenital malformations of the hand and forearm. London: Churchill Livingstone;1998. p. 217–24.
4. Dobyns JH, Wood VE, Bayne LG, et al. Congenital hand deformities. In : Green DP, editor. Operative hand surgery, Vol. 2. 2nd ed. New York: Churchill Livingstone;1988. p. 255–536.
5. Kim JH, Kim BJ, Kwon ST. Foot syndactyly: a clinical and demographic analysis. Arch Plast Surg. 2016; 43:559–63.

7. Cowan RJ. Surgical problems associated with congenital malformations of the forefoot. Can J Surg. 1965; 8:29–41.
8. Seok HH, Park JU, Kwon ST. New classification of polydactyly of the foot on the basis of syndactylism, axis deviation, and metatarsal extent of extra digit. Arch Plast Surg. 2013; 40:232–7.

9. Woo SJ, Kim BJ, Kwon ST. Case-control study of the treatment of postaxial polysyndactyly of the foot: comparison of surgical results after removal of the fifth or sixth toe. Arch Plast Surg. 2021; 48:91–7.

10. Narins RS, Brandt F, Leyden J, Lorenc ZP, Rubin M, Smith S. A randomized, double-blind, multicenter comparison of the efficacy and tolerability of Restylane versus Zyplast for the correction of nasolabial folds. Dermatol Surg. 2003; 29:588–95.

11. Uda H, Sugawara Y, Niu A, Sarukawa S. Treatment of lateral ray polydactyly of the foot: focusing on the selection of the toe to be excised. Plast Reconstr Surg. 2002; 109:1581–91.

12. Chan CW, Rudins A. Foot biomechanics during walking and running. Mayo Clin Proc. 1994; 69:448–61.

13. Johnson SP, Sebastin SJ, Rehim SA, Chung KC. The importance of hand appearance as a patient-reported outcome in hand surgery. Plast Reconstr Surg Glob Open. 2015; 3:e552.

14. McDougall L, Kennedy J, Coombs C, Penington A. The psychosocial impact of congenital hand and upper limb differences on children: a qualitative study. J Hand Surg Eur Vol. 2021; 46:391–7.

15. Andersson GB, Gillberg C, Fernell E, Johansson M, Nachemson A. Children with surgically corrected hand deformities and upper limb deficiencies: self-concept and psychological well-being. J Hand Surg Eur Vol. 2011; 36:795–801.

16. Hughes MJ. The social consequences of facial disfigurement. Milton: Routledge;2019.
17. Franzblau LE, Chung KC, Carlozzi N, Chin AY, Nellans KW, Waljee JF. Coping with congenital hand differences. Plast Reconstr Surg. 2015; 135:1067–75.

18. Rumsey N, Harcourt D. Body image and disfigurement: issues and interventions. Body Image. 2004; 1:83–97.

19. Bradbury E. Psychological issues for children and their parents. In : Buck-Gramcko D, editor. Congenital malformations of the hand and forearm. London: Churchill Livingstone;1998. p. 48–56.
Fig. 1.
Measurements performed using anteroposterior foot X-rays preoperatively and postoperatively. (A) Forefoot width was measured at the widest length of the soft tissue margins between the first and fifth (or sixth) metatarsophalangeal joints. (B) The angle difference was assessed by drawing two linear lines that connected the midpoint of the tips of the outermost two adjacent toes and measuring the angle between the two lines. (C) Toe length was measured as the distance between the tips of the distal phalanx to the base of the proximal phalanx.

Fig. 2.
Case 1 with left foot postaxial foot polydactyly. (A) Preoperative photograph and X-ray of a 35-year-old female patient with left postaxial polysyndactyly, type S0A2M2 (S, syndactylism; A, axis deviation; M, metatarsal extension). The forefoot width, angle difference, and toe length ratios of the affected to unaffected feet were measured as 1.06, 10.34, and 1.03, respectively. (B) Postoperative X-ray after 15 years. The postoperative forefoot width, angle difference, and toe length ratios were measured as 0.97, 7.83, and 1.06, respectively. The Global Aesthetic Improvement Scale score was 2.
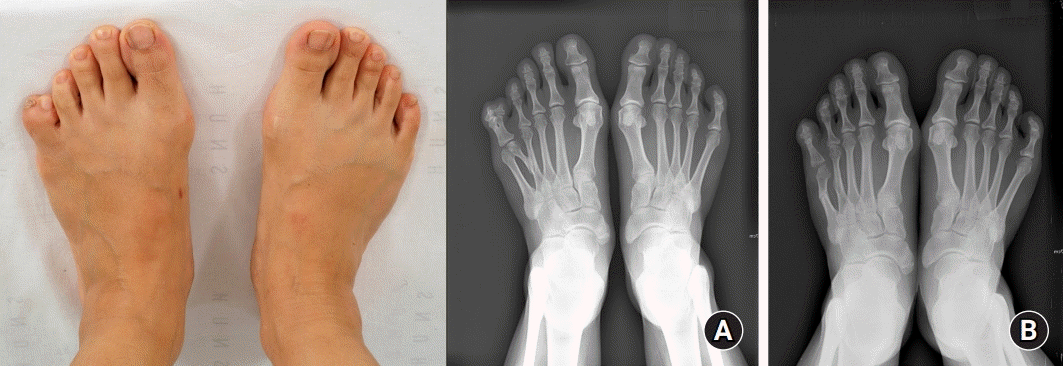
Fig. 3.
Case 10 with left foot second toe polydactyly. (A) Preoperative photograph and X-ray of a 21-year-old female patient with left foot second toe, type S1A1M0 (S, syndactylism; A, axis deviation; M, metatarsal extension). The forefoot width, angle difference, and toe length ratios of the affected to unaffected feet were measured as 0.99, 1.41, and 1.05, respectively. (B) Postoperative X-ray after 2 months. The postoperative forefoot width, angle difference, and toe length ratios were measured as 0.96, 1.22, and 0.99, respectively. The Global Aesthetic Improvement Scale score was 1.
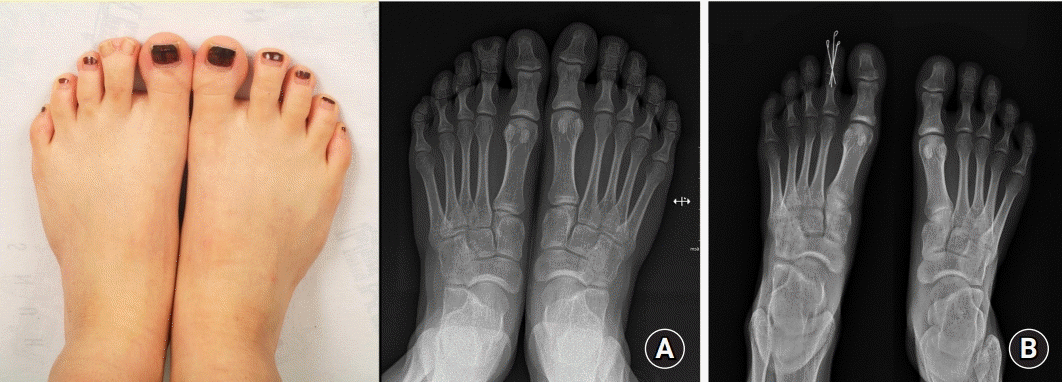
Table 1.
Clinical features, verbatim quotes from the patients on the purpose of surgery, and GAIS scores
| Case No. | Sex | Age at time of surgery (yr) | Location | SAM classification | Other anomalies | Family history | Main purpose of surgerya) | GAIS score at the last follow-upb) |
|---|---|---|---|---|---|---|---|---|
| 1 | Female | 35 | Left 5th toe | S0A2M2 | No | No | F: Pain upon wearing customized shoes | 2 |
| 2 | Female | 25 | Right 5th toe | S1A1M0 | No | No | C: Embarrassed to expose the foot | 2 |
| 3 | Female | 24 | Right 5th toe | S0A1M0 | No | Yes | C: Ashamed to wear open toe heels | 3 |
| 4 | Female | 27 | Left 5th toe | S0A1M0 | No | No | C: Ashamed of exposing the foot indoors without socks | 1 |
| 5 | Female | 56 | Right 5th toe | S1A0M1 | No | No | F: Discomfort upon wearing customized shoes for a long time | 1 |
| 6 | Female | 20 | Left 5th toe | S2A1M0 | No | No | C: Embarrassed to expose the foot | 1 |
| 7 | Male | 22 | Right 5th toe | S0A1M2 | Yes | No | F: Callus formation when wearing customized shoes | 3 |
| 8 | Male | 22 | Left 5th toe | S2A1M2 | No | No | F: Pain when wearing customized shoes | 1 |
| 9 | Female | 29 | Right 5th toe | S2A0M0 | No | No | C: Embarrassed and think the foot is ugly | 2 |
| 10 | Female | 21 | Left 2nd toe | S1A1M0 | No | No | C: Tired of people talking about the shape of the toe | 1 |
| 11 | Female | 53 | Right 5th toe | S1A0M0 | No | No | C: Embarrassed to expose the foot | 1 |
Table 2.
Comparison of preoperative and postoperative measurements of forefoot width, angle difference, and toe length ratio
| Measurement |
Preoperative |
Postoperative |
p-value | ||||
|---|---|---|---|---|---|---|---|
| Affected | Unaffected | Affected/unaffected | Affected | Unaffected | Affected/unaffected | ||
| Forefoot width (mm) | 99.22 (93.79–104.91) | 90.46 (89.22–93.1) | 1.10 | 89.35 (84.75–94.80) | 90.00 (87.83–93.29) | 0.99 | 0.005* |
| Angle difference (°) | 21.40 (15.46–33.29) | 13.76 (3.62–14.77) | 1.56 | 10.38 (7.40–18.73) | 6.76 (4.63–14.86) | 1.54 | 0.021* |
| Toe length (mm) | 35.07 (33.57–37.25) | 34.00 (31.78–35.14) | 1.03 | 34.03 (32.09–38.00) | 34.00 (31.80–35.21) | 1.00 | 0.083 |




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download