Abstract
Anterior communicating artery (ACoA) aneurysms sometimes present with visual symptoms when they rupture or directly compress the optic nerve. Giant or large ACoA aneurysms producing bitemporal hemianopsia are extremely rare. Here we present an unusual case of bitemporal hemianopsia caused by a large intracranial aneurysm of the ACoA. A 41-year-old woman was admitted to our neurosurgical department with a sudden-onset bursting headache and visual impairment. On admission, her vision was decreased to finger counting at 30 cm in the left eye and 50 cm in the right eye, and a severe bitemporal hemianopsia was demonstrated on visual field testing. A brain computed tomography scan revealed a subarachnoid hemorrhage at the basal cistern, and conventional cerebral catheter angiography of the left internal carotid artery demonstrated an 18×8 mm dumbbell-shaped aneurysm at the ACoA. Microscopic aneurysmal clipping was performed. An ACoA aneurysm can produce visual field defects by compressing the optic chiasm or nerves. We emphasize that it is important to diagnose an aneurysm through cerebrovascular study to prevent confusing it with pituitary apoplexy.
Aneurysms of the internal carotid artery and the anterior communicating artery (ACoA) are close to the optic nerve and chiasm. However, they rarely produce visual symptoms and signs in spite of their proximity to the visual pathways. Although ACoA aneurysms are the most frequent site of subarachnoid hemorrhage (SAH), they only infrequently cause visual disturbances. Most aneurysms presenting with visual disturbances are large or giant aneurysms, and the mechanism of visual loss and field defect has been attributed to either compression of the optic nerve or chiasm by the aneurysm itself or by an associated hematoma or vasospasm. We present a case of a ruptured large ACoA aneurysm presenting with a sudden onset of bitemporal hemianopsia.
A 41-year-old woman suddenly developed a bursting headache and bilateral visual disturbance. There was no alteration of her level of consciousness. Three days later she visited a local hospital because the headache continued and her vision had not improved. She was diagnosed with SAH and transferred to our hospital. On admission to our department, the patient had no abnormal finding on neurological examination except for visual disturbance. Her vision was decreased to finger counting at 30 cm in the left eye and 50 cm in the right eye, and a bitemporal hemianopsia was demonstrated. A non-contrast-enhanced computed tomography (CT) scan showed diffuse blood in the basal cistern and the Sylvian fissure of the left side of the brain (Fig. 1A). A contrast-enhanced CT scan showed a well-defined area of increased density above the sella (Fig. 1B). A brain MRI showed the optic chiasm to be deviated upward by a mass-like lesion in the sella (Fig. 1C). Cerebral catheter angiography through the left internal carotid artery revealed a downward and caudally-projecting ACoA aneurysm with a well-defined neck measuring 18×8 mm in diameter (Fig. 1D).
The patient immediately underwent a pterional craniotomy on the left side. A small amount of subarachnoid clot was observed around the chiasmal region. Under microscope magnification, a large aneurysm was found protruding forward and bending around the optic chiasm, curving down below it, and thus causing it to elevate and stretch (Fig. 2A). The aneurysmal neck was dissected and clipped with a Yasargil clip. We opened the aneurysm and removed clots and thrombi. The immediate post-operative period was uncomplicated. A post-operative angiogram showed complete clipping of the aneurysm (Fig. 2B).
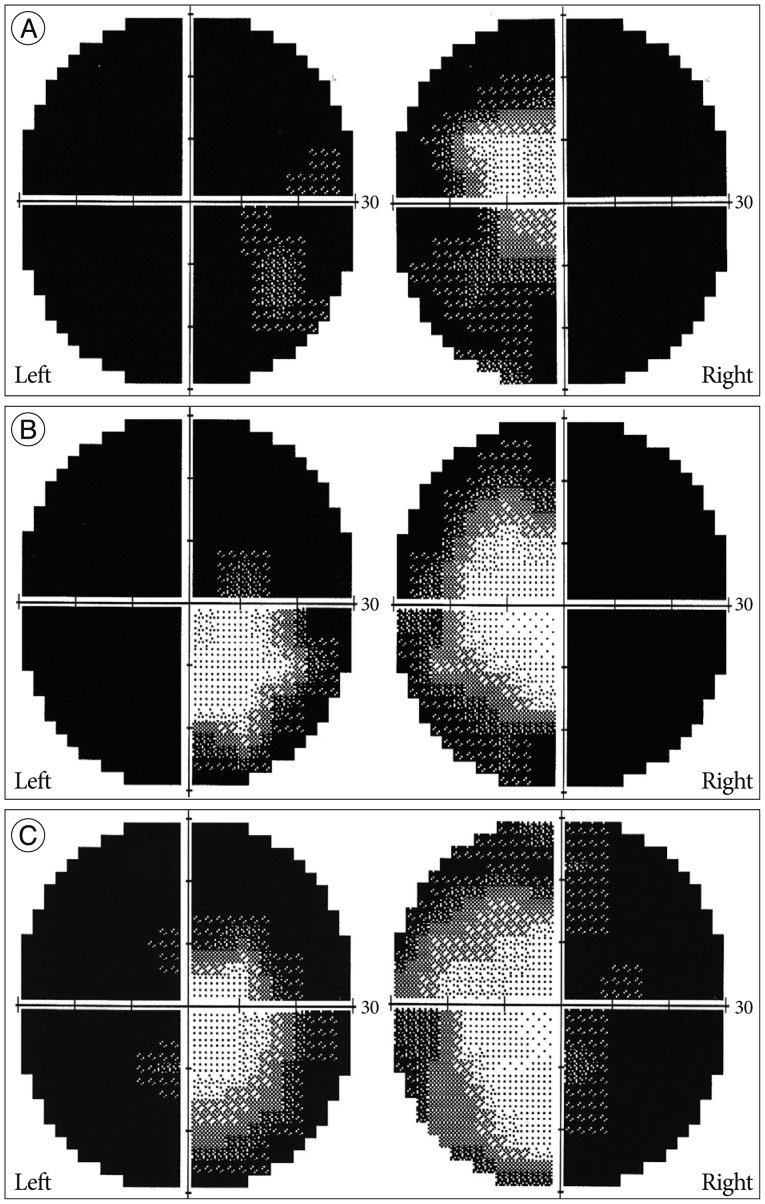
Three days later, the patient's visual disturbance had not improved and a severe bitemporal hemianopsia persisted (Fig. 3A) on perimetry (Humphrey field analyzer, Carl Zeiss Meditec Inc., Dublin, CA, USA). However, no vitreous hemorrhage in association with SAH was found in either eyes. Follow-up ophthalmological examination, 15 days after SAH (Fig. 3B), revealed that visual acuity had improved to 0.1 in both eyes. However, nine months after SAH, the patient continued to complain of diminished visual acuity and fields in both eyes, even though visual acuity improved to 0.25 in the left and 0.63 in the right. Also, perimetry testing revealed improved bitemporal hemianopsia (Fig. 3C).
The anterior communicating artery is the most common site of intracranial aneurysm, accounting for 26–38% of all cerebral aneurysms913). Usually, patients with a ruptured intracranial aneurysm causing SAH present symptoms of a sudden headache and mental status changes. Although ACoA aneurysms can be located close to the visual pathways, they rarely induce visual disturbances4). Several previous reports of ACoA aneurysms causing visual disturbance involve large or giant aneurysms17121416). However, small aneurysms of the ACoA rarely produce visual disturbance if they ruptured and presented with SAH before becoming large enough to induce significant pressure on the chiasm or optic nerves7). In our case, the aneurysm was large (18×8 mm) and ruptured. We hypothesize that the mechanism of visual disturbance is related to direct compression of the visual pathways either by the aneurysm itself or by an associated hematoma. ACoA aneurysms typically compress the superior chiasmal surface and produce macular loss and bilateral inferior field defects78). As in our case, a large aneurysm can grow forward and downward in front of the anterior edge of the chiasm and then elevate the chiasm and optic nerves upward and backward. This is in accordance with the hypothesis that the development of a bitemporal hemianopsia is caused by mechanical pressure on the chiasm10). Also, when the aneurysm ruptures, the pressure from arterial blood flow can damage the optic chiasm and nerves as much as the presence of a hematoma2315).
In our case, the patient's vision continued to deteriorate for three days after the onset of a severe headache. It is also possible that the visual disturbance was produced by ischemic damage resulting from poor blood circulation to the anterior visual pathways secondary to vasospasm or abnormality in the vessels to the optic pathway. For giant intracranial aneurysms, visual disturbance can occur with compression of the optic pathway caused by the aneurysm itself and, also, from poor blood circulation caused by pressure on the vessels around the optic pathway. Moreover, hematoma around a ruptured intracranial aneurysm can form an adhesion to the surrounding brain tissue and might compress microvessels on or around the optic pathway, causing poor blood circulation6).
Usually, the preferred treatment of an intracranial aneurysm with visual disturbance is to clip the neck of the aneurysm and remove the aneurysmal sac or intra-saccular hematoma and thrombus that compress the optic pathways. In most cases, clip ligation of the neck has a good prognosis, even for the patients with poor fundus conditions13). Some authors report that it is necessary to follow patients for up to two years after surgery to observe recovery from the visual disturbance511). In our case, ophthalmologic findings nine months after surgery indicated that visual acuity and field defects were gradually improving. Additional follow-up may be necessary to observe further recovery from the visual disturbance.
A ruptured large ACoA aneurysm can produce visual disturbance by direct compression of the aneurysm itself, by hematoma around the optic pathways, or by ischemic injury of the optic pathway caused by poor blood circulation by vasospasm or microvessel compression. Although the aneurysm was successfully clipped in the presented case, the visual symptoms were not completely resolved after surgery. This case demonstrates that ischemia resulting from poor blood circulation, as well as direct compression of the visual pathways, might play a role in visual disturbances.
References
1. Aoki N. Partially thrombosed aneurysm presenting as the sudden onset of bitemporal hemianopsia. Neurosurgery. 1988; 22:564–566. PMID: 3362325.

2. Chan JW, Hoyt WF, Ellis WG, Gress D. Pathogenesis of acute monocular blindness from leaking anterior communicating artery aneurysms : report of six cases. Neurology. 1997; 48:680–683. PMID: 9065547.

3. Claes C, Milea D, Bodaghi B, Tran TH, LeHoang P, Blanc R. Acute retrobulbar optic neuropathy due to rupture of an anterior communicating artery aneurysm. Acta Ophthalmol Scand. 2006; 84:145–146. PMID: 16445456.

4. Date I, Akioka T, Ohmoto T. Penetration of the optic chiasm by a ruptured anterior communicating artery aneurysm. Case report. J Neurosurg. 1997; 87:324–326. PMID: 9254100.

5. Ferguson GG, Drake CG. Carotid-ophthalmic aneurysms : visual abnormalities in 32 patients and the results of treatment. Surg Neurol. 1981; 16:1–8. PMID: 7280963.

6. Hara N, Mukuno K, Ohtaka H, Shimizu K. Ischemic optic neuropathy associated with subarachnoid hemorrhage after rupture of anterior communicating artery aneurysm. Ophthalmologica. 2003; 217:79–84. PMID: 12566879.

7. Højer-Pedersen E, Haase J. Giant anterior communicating artery aneurysm with bitemporal hemianopsia : case report. Neurosurgery. 1981; 8:703–706. PMID: 7279157.

8. Jefferson G. Further concerning compression of the optic pathways by intracranial aneurysms. Clin Neurosurg. 1953; 1:55–103. PMID: 14379465.

9. Koo SK, Song YJ, Huh JT. Surgically treated anterior communicating artery aneurysm. J Korean Neurosurg Soc. 2005; 37:405–409.
10. Moller PM, Hvid-Hansen O. Chiasmal visual fields. Acta Ophthalmol (Copenh). 1970; 48:678–684. PMID: 5536714.
11. Nishino A, Sakurai Y, Arai H, Nishimura S, Suzuki S, Uenohara H. Clinical manifestations, character of aneurysms, and surgical results for unruptured cerebral aneurysms presenting with ophthalmic symptoms. Acta Neurochir Suppl. 2002; 82:47–49. PMID: 12378990.

12. Norwood EG, Kline LB, Chandra-Sekar B, Harsh GR 3rd. Aneurysmal compression of the anterior visual pathways. Neurology. 1986; 36:1035–1041. PMID: 3736868.

13. Park JH, Park SK, Kim TH, Shin JJ, Shin HS, Hwang YS. Anterior communicating artery aneurysm related to visual symptoms. J Korean Neurosurg Soc. 2009; 46:232–238. PMID: 19844624.

14. Peiris JB, Ross Russell RW. Giant aneurysms of the carotid system presenting as visual field defect. J Neurol Neurosurg Psychiatry. 1980; 43:1053–1064. PMID: 7217950.

15. Ruben S, Afshar F. Visual failure following subarachnoid haemorrhage from rupture of an anterior communicating artery aneurysm. J Neurol Neurosurg Psychiatry. 1991; 54:1017–1018. PMID: 1800651.

16. Schisano G. Large anterior communicating artery aneurysm with temporal hemianopsia. Case report. J Neurosurg Sci. 1985; 29:267–271. PMID: 3831272.
Fig. 1
Brain computed tomography scan shows a subarachnoid hemorrhage at the basal cistern (A) and a oval lesion with contrast filling at the sellar region (B). Brain magnetic resonance imaging shows the optic chiasm (arrow heads) deviating upward by the aneurysm (arrow) (C). Cerebral catheter angiography in the left internal carotid artery demonstrates an 18×8 mm dumbbell-shaped aneurysm at the anterior communicating artery (D).
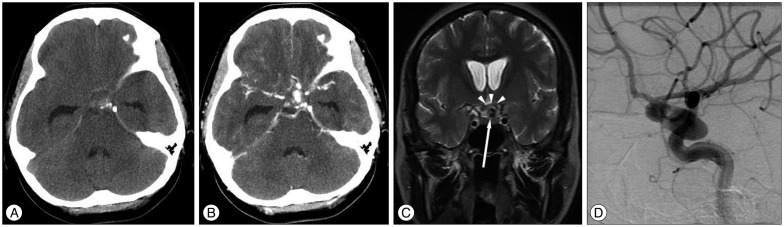
Fig. 2
Intra-operative view shows an aneurysmal sac on the anterior border of the optic chiasm (A). A large aneurysm grows forward and downward in the front of the free edge of the chiasm and pushes the chiasm upward and backward (*). Postoperative cerebral catheter angiography demonstrates complete occlusion of the aneurysmal sac by a clip (B). AN : aneurysm, ICA : internal carotid artery, ON : optic nerve.





 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download