INTRODUCTION
Since its introduction, hypoglossal-facial nerve anastomosis (HFNA) has been used as a favorable option for injured facial nerve (FN) reanimation. However, this operation results in donor nerve deficits, such as hemiglossal atrophy. Several modified surgical techniques, including anastomosis from the split hypoglossal nerve (HGN) or descending branch of the HGN to the FN, have been designed to reduce hemiglossal atrophy. Moreover, other modifications have also been made, such as hemihypoglossal-facial anastomosis and hypoglossal-facial nerve interpositional jump graft to overcome complications caused by classical methods
6,
8,
18,
22).
First, a detailed understanding of the anatomy of the submandibular region, including the route of the HGN and useful anatomical landmarks for HFNA and surrounding structures, is important to reduce procedural complications and the risk of nerve damage. It is difficult to define the proximal part of the HGN located immediately beneath the base of the skull, as the HGN in this area is readily confused with accessory nerves or the vagus nerve. Thus, it is necessary to dissect the submandibular region for identification of the HGN. Several anatomical studies of the submandibular region have been reported
3,
16,
17,
23), but there have been no previous reports of such studies in Korean subjects. This study focused mainly on the relationships among the FN, HGN, and surgical landmarks such as the mastoid process tip (MPT), the digastric muscle posterior belly (DMPB), and the common carotid artery (CCA), which can be easily identified during surgery. The anatomical data on the relationships between the anatomical landmarks, FN, and HGN may be helpful to find the FN and HGN more easily and to reduce the risk of procedural complications.
MATERIALS AND METHODS
Fifteen adult cadavers (9 males and 6 females) with a mean age of 62.2 years (range : 48-81) were fixed with formalin solution. A total of 29 specimens were obtained from 15 cadavers. Due to the anatomical destruction of the left submandibular region in one male cadaver (No. 15), the left specimen of this cadaver was excluded.
First, suboccipital and neck muscles were removed carefully, and the FN, digastric muscle, carotid artery, and nerve trunks were exposed. The mastoid process was dissected, and the FN was identified. After identification of the FN beneath the mastoid process, the FN was further dissected in the direction of the stylomastoid foramen (SMF). The SMF was located in the dorsal portion of the styloid process, which was the exit point of the FN. Subsequently, the FN was dissected and traced distally to the posterior part of the parotid gland. The parotid gland was removed almost completely for FN dissection.
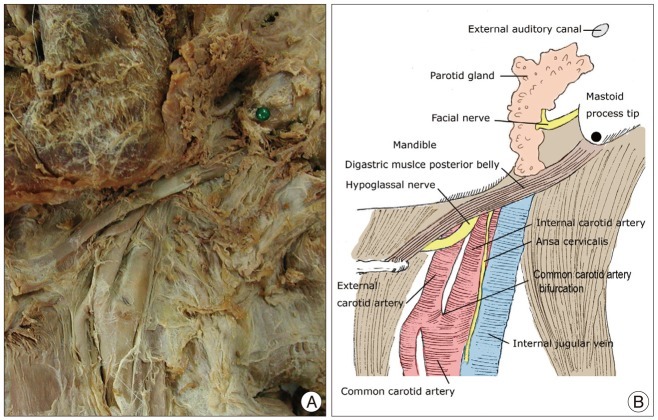
To determine the relationships among the FN, HGN, and surrounding structures, the MPT, the bifurcation of CCA, and the DMPB were designated as the anatomical landmarks of the submandibular area (
Fig. 1).
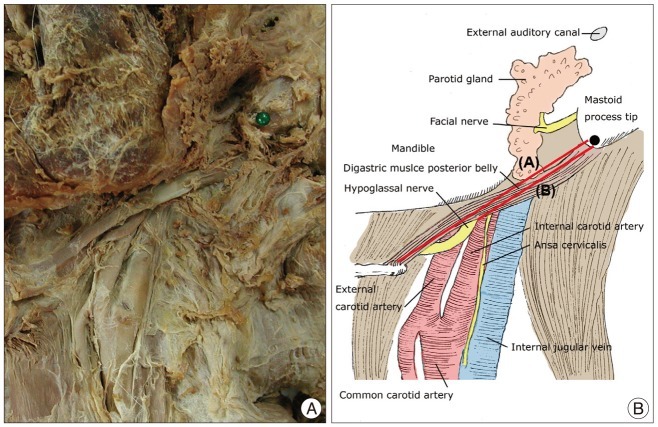
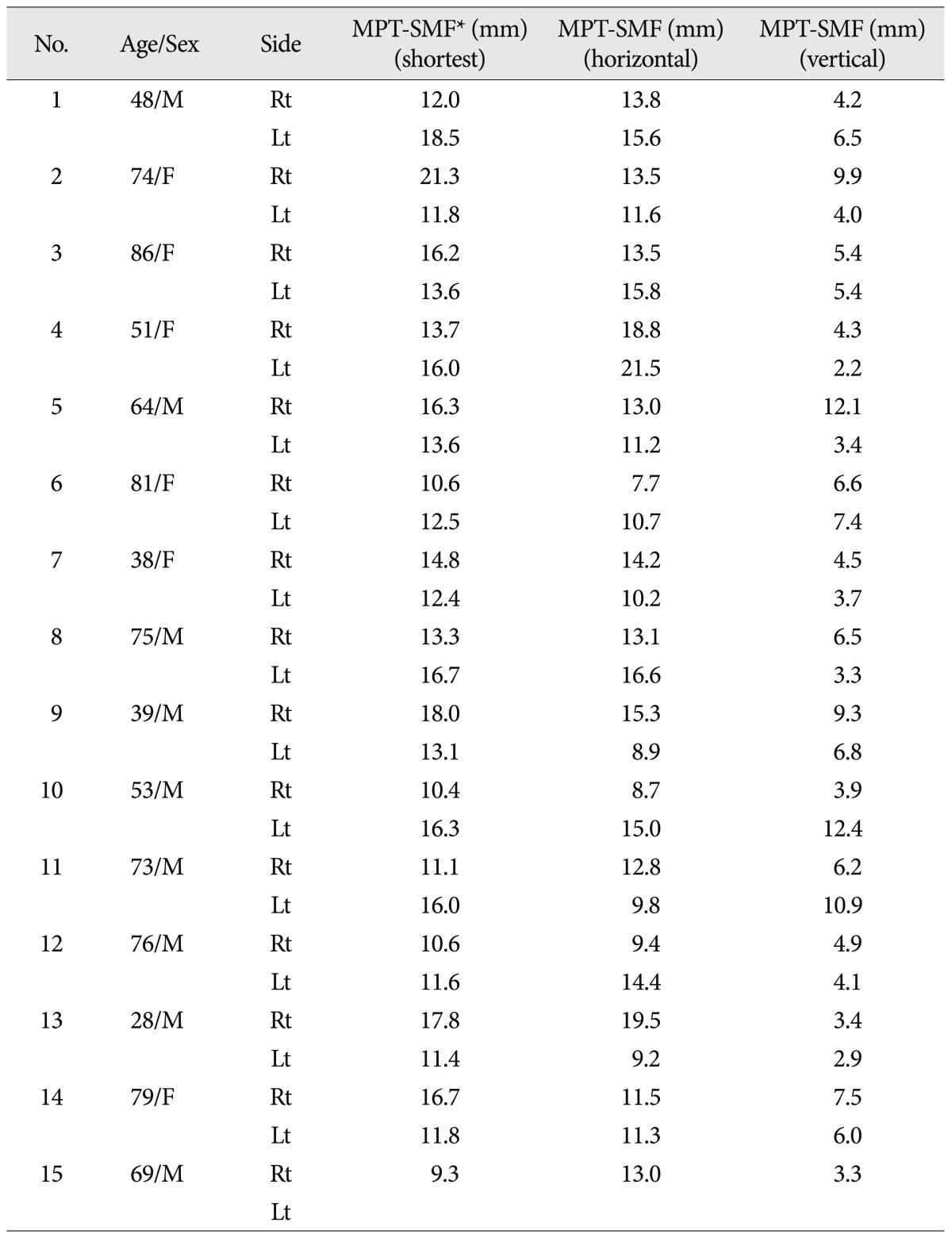
Based on the MPT, the following measurements were obtained : 1) the shortest distance to the SMF, which was the exit point of the FN; 2) the horizontal distance to the SMF; and 3) the vertical distance to the SMF (
Fig. 2).
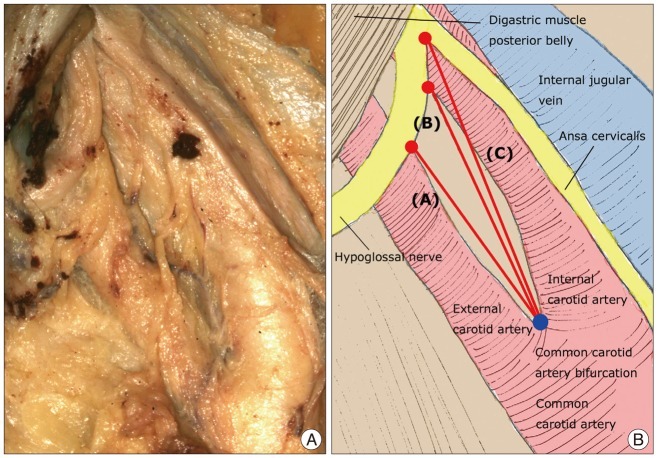
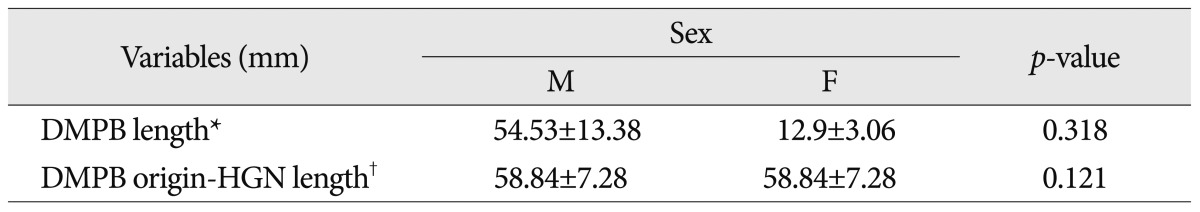
Based on the DMPB, the following measurements were obtained : 1) the whole length of the DMPB running from the digastric groove (DMPB origin) to the fibrous loop for the intermediate digastric tendon; and 2) the distance from the DMPB origin to the crossover point between the DMPB and the HGN (
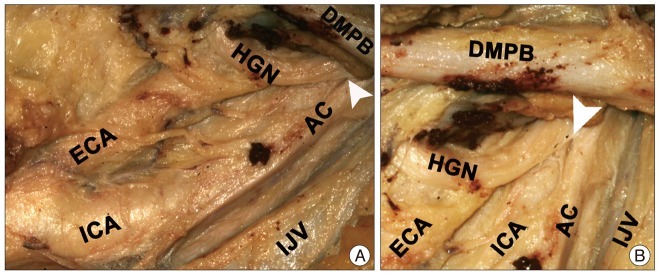
Fig. 3). The following measurements were also obtained based on the common carotid artery bifurcation (CCAB) : 1) the distance from the CCAB to the crossover point between the HGN and the ventral margin of the internal carotid artery (ICA); 2) the distance from the CCAB to the crossover point between the HGN and the dorsal margin of the external carotid artery (ECA); and 3) the distance from the CCAB to the HGN bifurcation (
Fig. 4).
A standard meter and goniometer were used to obtain measurements, and all measurements were made by one trained physician to minimize interobserver measurement errors. The data were used in a comparative analysis of sex and right/left differences. The data are presented as means±standard deviations for continuous variables and frequency (percentages) for categorical variables. Statistical analyses were performed using SPSS for Windows version 14.0 (SPSS, Inc., Chicago, IL, USA). Differences between groups were compared with Student's t-test for continuous variables. In all analyses, p<0.05 was taken to indicate statistical significance.
DISCUSSION
The FN appears from the SMF beside the styloid process. It lies medial, deep, and slightly anterior to the middle of the mastoid process at the lower end of the tympanomastoid fissure. After the FN ramifies the posterior auricular and branches to the posterior digastric and stylohyoid muscles, it runs obliquely inferiorly and laterally into the substance of the parotid gland. It divides into the temporofacial and cervicofacial divisions at a point vertically below the lowest part of the bony external auditory meatus (
Fig. 1)
7).
The HGN typically emerges between the ICA and the IJV to descend in the lateral groove between them to a point not far above the CCAB. It then gives rise to the superior root of the ansa cervicalis and curves forward across the lateral surfaces of both the internal and external carotid vessels. In this course, it usually passes downward until just lateral to the origin of the occipital artery and then turns forward, being held at the turn by the sternomastoid branch of the occipital artery so that it hooks around these vessels before it runs forward above the hyoid bone
4). After turning forward, the HGN crosses the ventral portion of the ICA, the dorsal portion of the ECA, and the DMPB (
Fig. 1,
2).
HFNA has been considered an effective means of reanimating the paralyzed facial nerve. However, classic HFNA involves sacrificing the normal HGN, causing hemitongue atrophy. Many modifications have been made to this technique to avoid hemitongue atrophy. May et al.
14) introduced a hypoglossal-facial nerve interpositional jump graft. However, direct HFNS was more effective for restoring facial function. Cusimano and Sekhar
5), Sekhar et al.
20), and Arai et al.
1) reported anastomosis of a split hypoglossal nerve to the facial nerve. These methods preserved hypoglossal function with mild or moderate hemiglossal atrophy. To minimize disruption of hypoglossal nerve function, hypoglossal-facial nerve side-to-end anastomosis was developed
17).
HFNA remains the most commonly used technique, and many modifications have been made to achieve nerve dissection without injury. However, it is difficult to dissect the submandibular region without damaging the FN and the HGN. Several studies have shown that it is difficult to identify and expose the FN during dissection as the FN is surrounded by dense connective tissue
10,
21). As the FN and the HGN are located in complex areas, surgeons must be well acquainted with the anatomy to prevent procedural damage. Many authors have suggested that detailed anatomical knowledge is necessary to achieve successful anastomosis
1,
2,
13,
16). Gardner et al.
9) suggested that the DMPB should first be found to identify the FN. Malone and Maisel
12) cautioned that using a nerve stimulator to identify the FN may be misleading because of false negative responses. Sawamura and Abe
17) used a method involving initial exposure of the MPT to search for the FN. Salame et al.
16) recommended following the styloid process until the SMF emerged to identify the FN. Asaoka et al.
3) reported that the FN usually appeared on the ventral portion of the MPT. Some reports suggested that landmarks may be used for safe FN dissection. Three of the above-mentioned studies used bony landmarks for FN dissection
3,
16,
17). Two studies used the MPT, and the other used the styloid process. The MPT is a relatively large structure and is located superficially. Moreover, the MPT is not surrounded by any dangerous structures and allows the surgeon to gain a solid general understanding of the local anatomy. For these reasons, the MPT was used as a landmark in this study. Kempe
11) noted previously that it is a common error to go deep to look for the nerve. Salame et al.
16) introduced several parameters associated with the FN and surrounding structures. They used 23 formaldehyde-fixed adult cadavers (13 female and 10 male) aged 51 to 74 years at the time of death and dissected bilaterally (46 dissections). The distance was 17.22±3.18 mm between the SMF and the MPT. Jones
19) estimated the depth from the MPT to the SMF as 2 cm. In the present study, the distance was 14.1±2.9 mm between the SMF and the MPT. Morphometric measurements in the present study were slightly shorter than those reported by Salame et al.
16) because of differences in the proportion of males to females and the numbers of specimens between the two studies. However, the age spectrum was similar between the present study and that of Salame et al.
16) The numerical discrepancies between these two studies may have been due to differences in proportion of males to females as well as to racial differences. It can be inferred that other parameters, such as horizontal and vertical distances between the MPT and SMF, would show numerical differences. Further investigations are required to determine the relationship between the SMF and the MPT. This FN dissection-related database will be helpful for predicting the FN exit or route prior to surgery.
HGN dissection is more complicated, as the location of the HGN is much deeper than that of the FN, and there are many variations in the HGN branching patterns. Moreover, there are no bony landmarks around the HGN. Therefore, the digastric muscle, the ICA, and the IJV were used as landmarks for HGN dissection. Martins et al.
13) suggested that the HGN should be dissected at the lowest portion of the cervical incision, inferior and medial to the DMPB. Vacher and Dauge
23) suggested that access to the sternocleidomastoid muscle region should be achieved initially. Rebol et al.
15) reported that the HGN was located in the neck under the digastric muscle. Arai et al.
1) proposed that the HGN should be exposed deeply to the plane of the digastric muscle and superficially to the carotid vessels. Asaoka et al.
2,
3) suggested that the HGN could be found by retracting the IJV posteriorly. In the extreme-high cervical area, the HGN runs parallel to the vagus and accessory nerves on the dorsal portion of the ICA. Roberto et al.
13) dissected the HGN inferior and medial to the DMPB and reported that it was located near and superior to the CCAB, identified by its pulsation. Although the CCA appeared in variable locations in this study, CCAB was a continuous valid landmark in HGN dissection. The digastric muscle was a good enough landmark to find the HGN, as mentioned in many previous reports
1,
3,
9,
13,
16,
19,
23). However, most of these studies did not use only the DMPB as a landmark. As mentioned above, the carotid vessels, jugular vein, and DMPB are used together as landmarks
3,
13,
23) as the high cervical and submandibular anatomy is very complicated and variable. According to this study, although the location of the CCAB was not the same due to interindividual variations, the HGN was mostly detected in the area between the DMPB and the CCAB. The HGN appeared under the DMPB, and the crossing point corresponded to about 65.5% of the whole length of the DMPD from the digastric groove. The HGN was located within the area between the CCAB and the DMPB. Considering the complicated anatomy of the cervical and submandibular region, the use of only one surgical landmark is not recommended. The DMPB and the CCAB represent good landmarks during submandibular dissection to identify the HGN.
Although a great deal of effort was made to acquire accurate measurements, this study still has several limitations. Formalin-fixed cadavers were used in this study, and therefore, the muscles and tissues were firmly fixed. Therefore, there could be differences in tissue extension or muscle length depending on the neck rotation angle, and there is no way to correct this variation. Thus, there will always be differences in these measurements depending on surgical position when applied under clinical conditions.
These measurements will help not only in finding the FN and HGN but also in defining the appropriate site for anastomosis during surgery. Additionally, nerve injury and operation time will be reduced, thereby benefiting patients.











 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download