INTRODUCTION
MATERIALS AND METHODS
RESULTS
Pre-operative radiological parameter predicting clinical outcomes
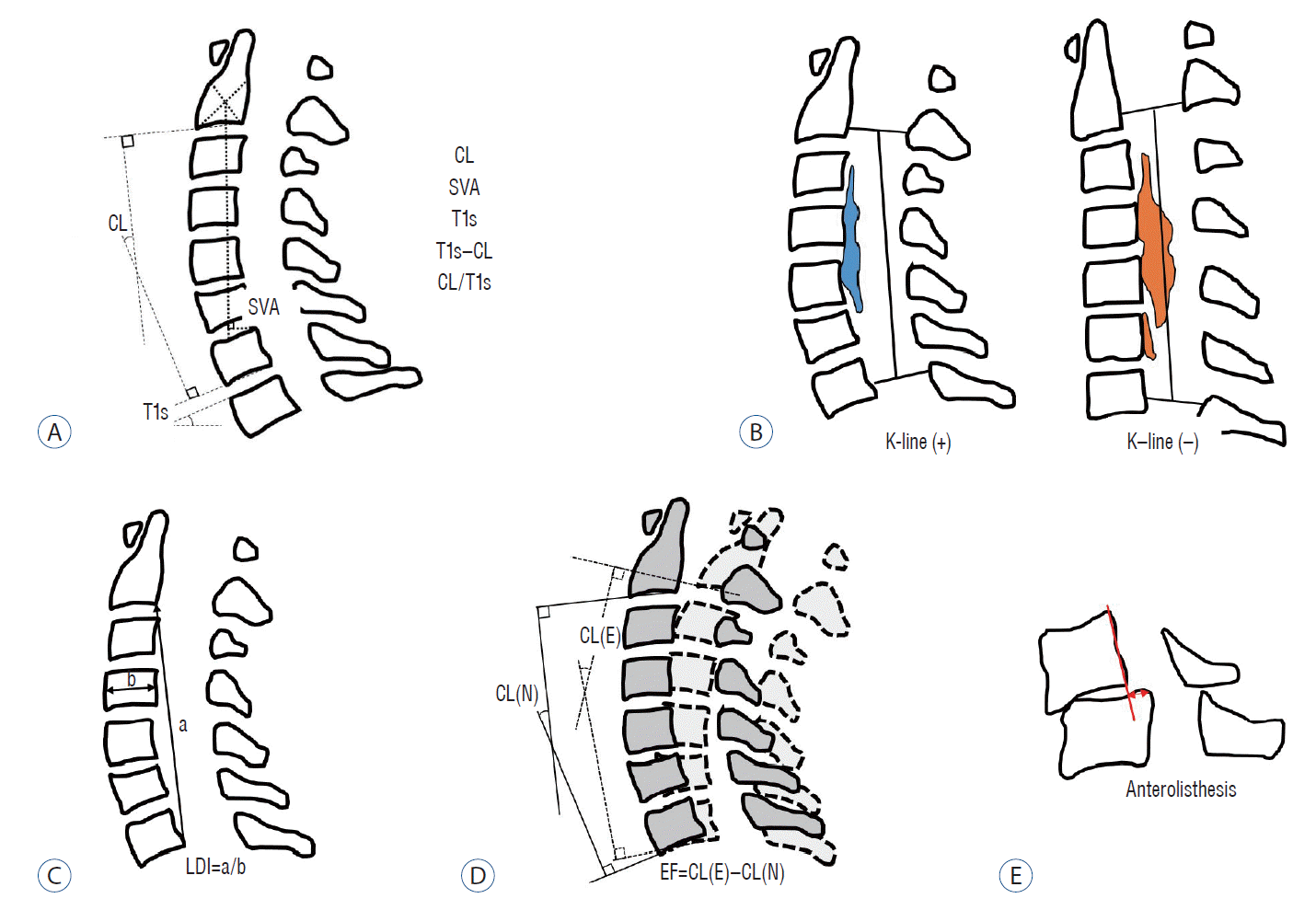 | Fig. 2.Schematic images of sagittal radiological parameters. A : Routine sagittal parameters. B : K-line. C : a means length of a vertical line drawn between the postero-inferior edges of C2 and C7, b means the antero-posterior diameter of C4, and LDI of the cervical spine. D : Extension function (EF). E : Anterolisthesis in flexion position. CL : cervical lordosis, SVA : sagittal vertical axis, T1s : T1 slope, LDI : longitudinal distance index, CL(N) : cervical lordosis in neutral position, CL(E) : cervical lordosis in extension position. |
Table 1.
CL : cervical lordosis, SVA : sagittal vertical axis, T1s : T1 slope, CL/T1s : ratio of cervical lordosis to T1 slope, ROM : range of motion, mK-line : modified Kline, MR : magnetic resonance image, VB : vertebral body, LDI : longitudinal distance index of cervical spine, AP : anterior-posterior, EF: extension function
Table 2.
| Study | Sample size, OP type, disease | Clinical outcomes | Pre-op kyphosis | Post-op kyphosis | LCL | SVA | T1s–CL | T1s | Other factor |
|---|---|---|---|---|---|---|---|---|---|
| Baba et al. [2] (1996) | 55, OD, CSM+OPLL | JOA RR (50%) | * | * | Posterior cord migration was related with RR | ||||
| Yamazaki et al. [72] (1999) | 38, FD, OPLL | Contact/non-contact | (10°)* | (5°)* | Maximal thickness of OPLL >7 mm | ||||
| Pre-op non-lordotic (CL <10°, n=12) | |||||||||
| Ishibashi [18] (2000) | 140, FD, CSM+OPLL | JOA RR | N.S. | N.S. | N.S. | Pre-op kyphosis (CL <0°, n=2) | |||
| Pre-op kyphosis was not related poor RR | |||||||||
| Chiba et al. [8] (2000) | 70, OD, CSM+OPLL | JOA RR | LDI had a negative correlation with RR (r=-0.308, p =0.014) | ||||||
| Iwasaki et al. [21] (2002) | 92, OD, OPLL | JOA RR | N.S. | N.S. | Follow up >10 years | ||||
| Pre-op kyphosis (n=1) | |||||||||
| Post-op alignment was not related with RR | |||||||||
| Kawakami et al. [24] (2002) | 103, FD, CSM+OPLL (?) | JOA RR | N. S | N.S. | Pre-op kyphosis (CL <0°, n=16) | ||||
| Pre-op kyphosis was not related poor RR | |||||||||
| Cord convex type, C2 decompression was related with poor RR | |||||||||
| Suda et al. [64] (2003) | 114, FD, CSM+OPLL (?) | JOA RR (50%) | (CL <0°)* | Pre-op kyphosis (CL <0°, n=12) | |||||
| Local kyphosis and cord signal change were independent risk factors of RR <50% | |||||||||
| Ogawa et al. [48] (2004) | 72, OD, OPLL | JOA RR | N.S. | N.S. | N.S. | Follow up >10 years | |||
| Pre-op kyphosis (n=10) | |||||||||
| Pre-op JOA, age, symptom duration affected clinical outcomes | |||||||||
| Chiba et al. [9] (2006) | 80, OD, CSM+OPLL | JOA RR | N.S. (CSM)* | N.S. | Follow up >10 years | ||||
| (OPLL) | |||||||||
| Masaki et al. [44] (2007) | 40, OD, OPLL | JOA RR (40%) | N.S. | * | Old age, long symptom duration, high LCL, low ROM were related to poor outcome | ||||
| Fujiyoshi et al. [13] (2008) | 27, OD, OPLL | JOA RR | N.S. | This study including patients with posterior laminectomy and fusion (n=8) | |||||
| Interop US | K-line (–) was closely related with poor RR | ||||||||
| Kim et al. [30] (2013) | 58, FD, CSM+OPLL | VAS, NDI | (10°) | Pre-op non-lordotic (CL <10°, n=18) | |||||
| N.S. | Pre-op kyphosis was not related poor RR | ||||||||
| Toyama classification was not related with RR | |||||||||
| Maruo et al. [43] (2014) | 45, FD, OPLL | JOA RR (50%) | N.S. | N.S. | N.S. | Pre-ROM was higher in the poor outcome group | |||
| Cho et al. [10] (2014) | 76, OD+FD, CSM+OPLL (?) | JOA, VAS, NDI, SF-36 | (27.3°) | ||||||
| N.S. | |||||||||
| Taniyama et al. [69] (2014) | 61, OD CSM | JOA | N.S. | mK-line was measured on midsagittal T1 MRI | |||||
| INTmin was correlated with RR with non-lordotic alignment. | |||||||||
| Lee et al. [34] (2016) | 50, OD, OPLL | JOA, VAS, NDI, SF-36 | N.S. | N.S. | N.S. | (30 mm) | (22°) | C7 involvement | |
| N.S. | N.S | Pre-op kyphosis (CL <0°, n=7) | |||||||
| Pre-op kyphosis was not related poor RR | |||||||||
| Oshima et al. [51] (2016) | 92, FD, CSM+OPLL | JOA, VAS, NDI, SF-36 | (50 mm)* | SVA >50 mm related to poor functional outcome, but improvement (RR) is not | |||||
| Oichi et al. [50] (2016) | 125, FD, OPLL | JOA RR (50%) | N.S. | Pre-op kyphosis (CL <0°, n=20) | |||||
| Pre-op kyphosis was not related poor RR | |||||||||
| Age and RR <50% (OR, 1.05; p =0.019), anterolisthesis and RR <50% (OR, 8.9; p =0.012) | |||||||||
| Sakai et al. [56] (2016) | 174, FD, CSM | JOA RR | (CL <-5°)* | Postop CL <-5° was related to poor clinical outcome | |||||
| Kato et al. [23] (2017) | 110, OD, CSM+OPLL | JOACMEQ, SF-36, JOA, VAS | N.S. | (35 mm) | N.S. | ||||
| CSF* | |||||||||
| PCS* | |||||||||
| Li et al. [40] (2017) | 40, OD, OPLL | JOA, NDI | K-line (–) NNP but K-line (+) NEP group also has a relatively effective and safe | ||||||
| Cao et al. [6] (2017) | 173, OD, CSM | JOA RR | (CL <-5°)* | Postop CL <-5° was related to poor clinical outcome | |||||
| Fujiwara et al. [12] (2018) | 57, OD, CSM+OPLL | VAS, JOACMEQ | N.S. (CSM) | N.S. | N.S. | N.S. | Pre-CL and UEF in OPLL : r=-0.42 | ||
| (OPLL)* | Pre-ROM and QOL in OPLL : r=0.53 | ||||||||
| Post-ROM and LEF in CSM : r=0.32 | |||||||||
| Miyazaki et al. [47] (2018) | 35, FD, OPLL | JOA RR | (30.1°) | Pre MRI grade independently associated with RR | |||||
| N.S. | |||||||||
| Lee et al. [38] (2018) | 33, OD, CSM+OPLL | JOA, NDI | (20°)* | ||||||
| Sakaura et al. [57] (2019) | 219, no data, CSM+OPLL | JOA RR | (0°) | (30 mm) | |||||
| (CSM)* | (CSM)* | ||||||||
| N.S. (OPLL) | N.S. (OPLL) | ||||||||
| Chen et al. [7] (2020) | 85, FD, CSM | JOA, VAS, Nurick | N.S. | (28.9 mm)* | (20°)* | Pre-op kyphosis (CL <0°, n=7) | |||
| Rao et al. [54] (2019) | 85, OD, CSM+OPLL (?) | JOA RR, NDI | (20°)* | ||||||
| Li et al. [41] (2019) | 78, OD, CSM+OPLL (?) | JOA RR | CL/T1s : fair ratio had a better outcome than the low or high ratio | ||||||
| Lee et al. [39] (2019) | 50, OD, CSM+OPLL | JOA RR (50%) | N.S. | N.S. | N.S. | Age has a correlation with RR (r=-0.330, p =0.019) | |||
| Sharma et al. [62] (2020) | 121, OD, CSM+OPLL | JOA, ODI | (20 mm)* | (30°)* | Cord signal change grade and mJOA were closely related. | ||||
| Classification system (A–D) | |||||||||
| Tamai et al. [67] (2020) | 60, OD, CSM | JOACMEQ, JOA, SF-36, VAS | (40 mm) | Propensity score-matching | |||||
| N.S. |
* Indicates statistically significant relationship, numbers in parentheses ( ) indicate cutoff values.
OP type : operation type, Pre-op : preoperative, Post-op : postoperative, LCL : loss of cervical lordosis, SVA : sagittal vertical axis, T1s : T1 slope, CL : cervical lordosis, OD : open-door laminoplasty, CSM : cervical spondylotic myelopathy, OPLL : ossified posterior longitudinal ligament, JOA : Japanese orthopedic association scale, RR : recovery rate, FD : French-door laminoplasty, N.S. : no statistical relationship, LDI : longitudinal distance index of cervical spine, OPLL (?) : OPLL was not clearly excluded from enroll data, ROM : range of motion, US : ultrasonography, NDI : neck disability index, VAS : Visual analog scale for neck pain, ODI : Oswestry disability index, SF-36 : short form-36, mK-line : modified K-line, MRI : magnetic resonance image, INTmin : minimum interval between the mK-line and the anterior compression factor on the midsagittal T1 MR image, OR : odds ratio, JOACMEQ : JOA cervical myelopathy evaluation questionnaire, CSF : cervical spine function, PCS : physical component summary of SF-36, NNP : neck neutral position, NEP : neck extension position, UEF: upper extremity function, QOL : quality of life, LEF : lower extremity function, CL/T1s : ratio of Cervical lordosis to T1 slope
Pre-operative kyphotic alignment (CSM and OPLL)
K-line (OPLL), modified K-line (CSM) and variants
Sagittal balance-related parameters (CSM and OPLL)
T1s (CSM and OPLL)
Range of motion (ROM) (OPLL)
Radiological change (LCL, post-operative kyphosis) (CSM and OPLL)
Miscellaneous
Preoperative radiological parameters predicting radiological outcomes
LCL
Table 3.
| Study | Sample size, OP type, disease | Radiological outcomes | Pre-op CL | SVA | T1s | T1s–CL | ROM | Other factor |
|---|---|---|---|---|---|---|---|---|
| Suk et al. [65] (2007) | 85, OD, CSM+OPLL | Post kyphosis (<0°) | CL <10°* | Flex CL > Ext CL was related with post kyphosis | ||||
| Kim et al. [31] (2013) | 51, FD, CSM+OPLL | LCL | (26.4°)* | |||||
| Post kyphosis (<0°) | N.S. | |||||||
| Cho et al. [10] (2014) | 76, OD+FD, CSM+OPLL (?) | LCL | (27.3°) | |||||
| N.S. (r=0.148) | ||||||||
| Sakai et al. [56] (2016) | 174, FD | LCL | N.S. | CGH-C7* | C7s | N.S. | Age | |
| CSM | Post kyphosis (<-5°) | N.S. | (42 mm)* | (r=0.362)* | N.S. | Age (75 years) | ||
| N.S. | ||||||||
| Kato et al. [23] (2017) | 110, OD, CSM+OPLL | LCL | (35 mm)* | SVA <35 mm group had a more LCL | ||||
| Lee et al. [36] (2017) | 49, OD, CSM+OPLL | LCL | N.S. | N.S. | (r=0.302)* | |||
| Zhang et al. [74] (2017) | 41, OD, CSM | LCL | N.S. | (r=0.393)* | (r=0.351)* | CVLL (C3) | ||
| Cao et al. [6] (2017) | 194, OD, CSM | Post kyphosis (<-5°) | N.S. | * | N.S. | N.S. | CVLL (C3), facet injury | |
| Lee et al. [38] (2018) | 33, OD, CSM+OPLL | LCL | N.S. | N.S. | (r= -0.419)* | N.S. | N.S. | |
| Miyazaki et al. [47] (2018) | 35, FD, OPLL | LCL | (30.1°) | |||||
| Post kyphosis | (r=0.326)* | |||||||
| N.S. | ||||||||
| Matsuoka et al. [45] (2018) | 27, OD, OPLL | Post kyphosis (<0°) | * | * | N.S. | Age | ||
| Matsuoka et al. [45] (2018) | 42, OD, CSM | Post kyphosis (<0°) | * | N.S. | N.S. | C7 SVA | ||
| Lee et al. [33] (2018) | 144, OD+FD | LCL | N.S. | N.S. | (r=0.337)* | SCSA of SC at C6 | ||
| CSM | ||||||||
| Lin et al. [42] (2018) | 40, OD, CSM | LCL | (2 2mm) | (20°) | ||||
| N.S. | N.S. | |||||||
| Chen et al. [7] (2020) | 85, FD | LCL | (28.9 mm) | (r=0.291)* | (20°) | |||
| CSM | (r=0.457)* | (r=0.245)* | ||||||
| Rao et al. [54] (2019) | 85, OD, CSM+OPLL (?) | LCL | (20°)* | |||||
| Lee et al. [39] (2019) | 50, OD | LCL | N.S. | (r=0.443)* | (C7s) | (C2s) | N.S. | EF (r=0.504) |
| CSM+OPLL | N.S. (r=0.148) | (r=0.371)* | ||||||
| Li et al. [41] (2019) | 78, OD, CSM+OPLL (?) | LCL | High ratio CL/T1s | |||||
| Post kyphosis (<0°) | Low ratio CL/T1s | |||||||
| Sharma et al. [62] (2020) | 121, OD, CSM+OPLL | LCL | (10°)* | N.S. | (30°)* | EF (12°), Sharma classification (score 0–4) |
* Indicates statistically significant relationship, numbers in parentheses ( ) indicate cutoff values.
OP type : operation type, Pre-op : preoperative, CL : cervical lordosis, SVA : sagittal vertical axis, T1s : T1 slope, ROM : range of motion, OD : open-door laminoplasty, CSM : cervical spondylotic myelopathy, OPLL : ossified posterior longitudinal ligament, Post kyphosis : postoperative kyphosis, Flex CL : cervical lordosis in flexion position, Ext CL : cervical lordosis in extension position, FD : French-door laminoplasty, LCL : loss of cervical lordosis, N.S. : no statistical relationship, OPLL (?) : OPLL was not clearly excluded from enroll data, CGH : center of gravity of head, VLL : cephalad vertebral level undergoing laminoplasty, SCSA of SC : summation of cross sectional area of the semispinalis cervicis, C7s : C7 slope, C2s : C2 slope, EF : extension function, CL/T1s : ratio of Cervical lordosis to T1 slope
Postoperative kyphosis
Case presentation
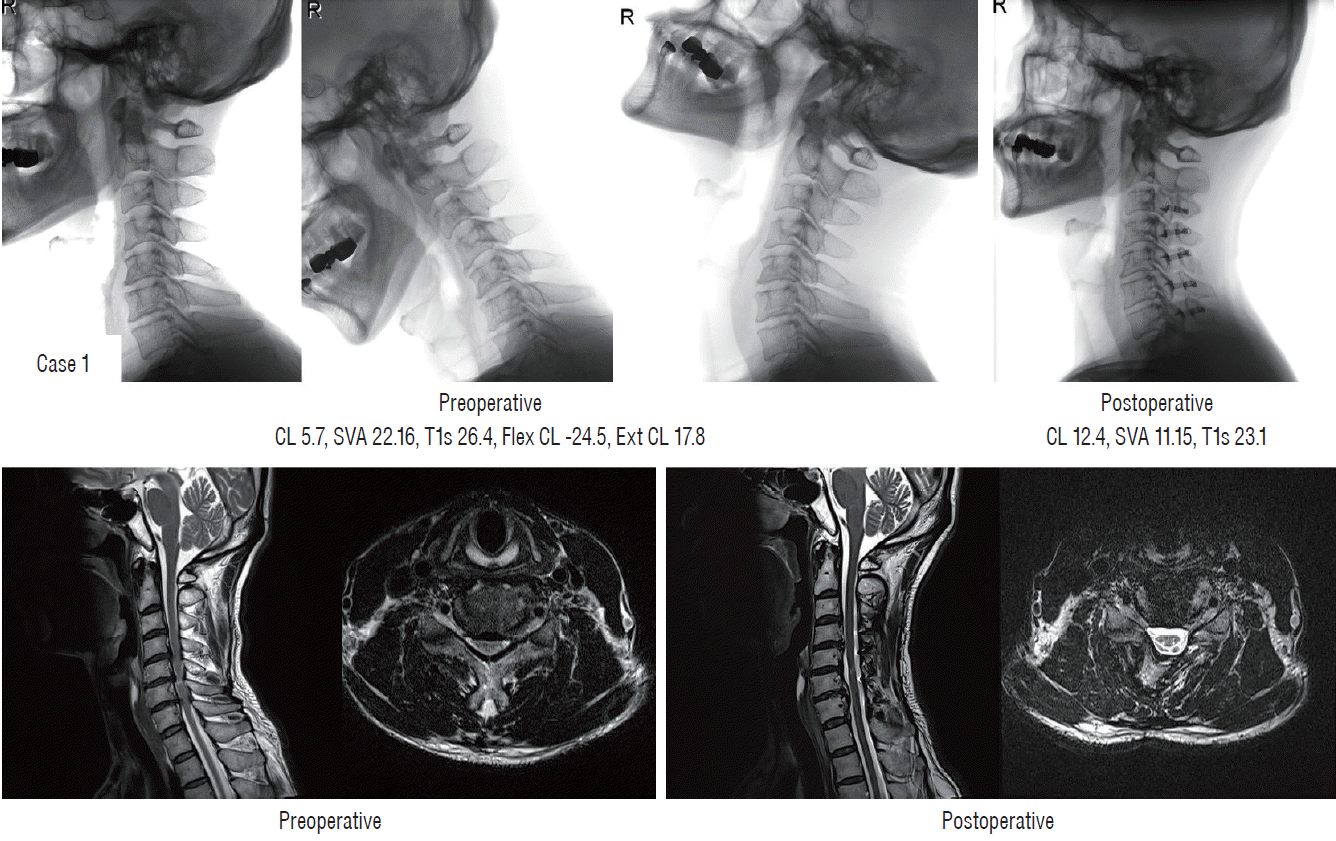
Case 1 (Fig. 4)
Case 2 (Fig. 5)
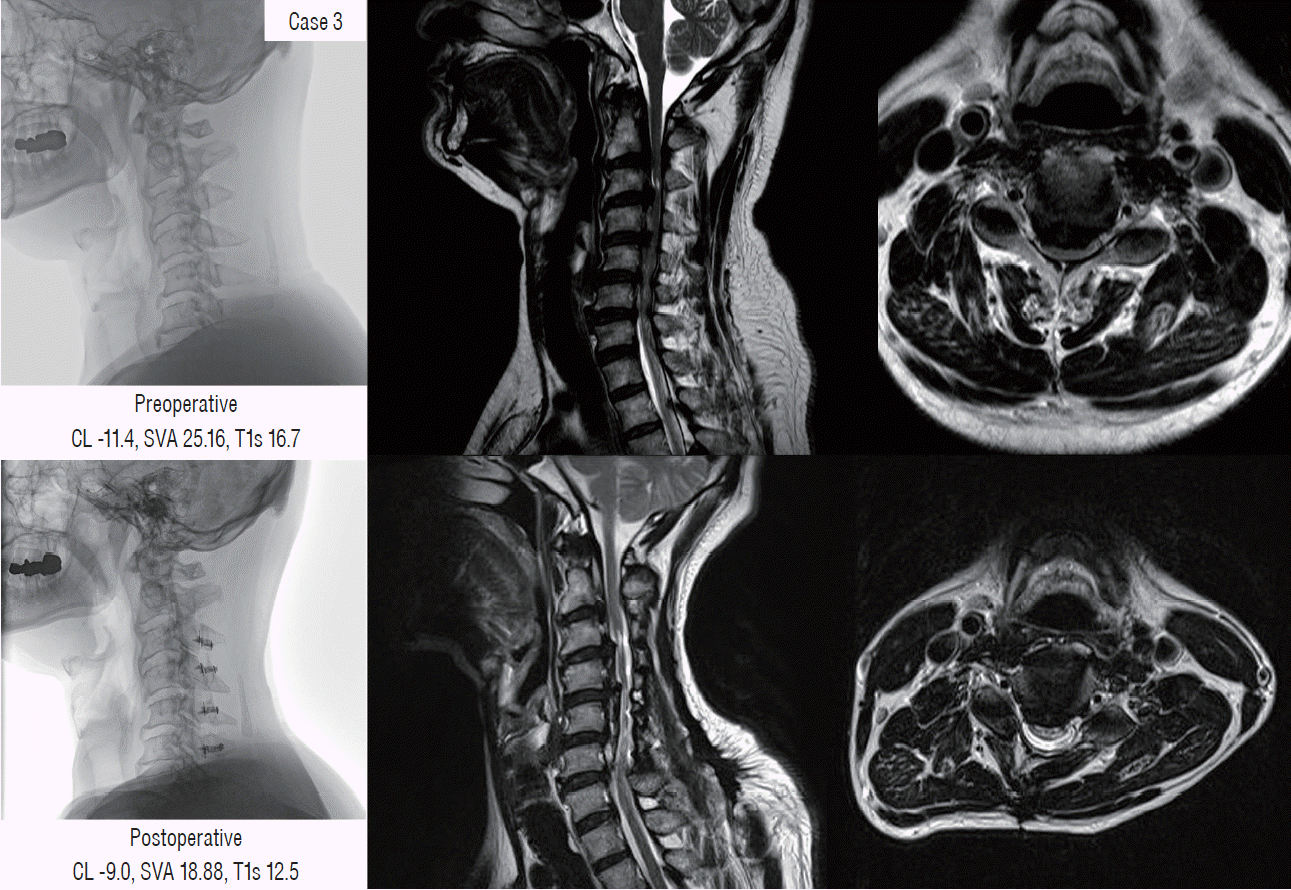
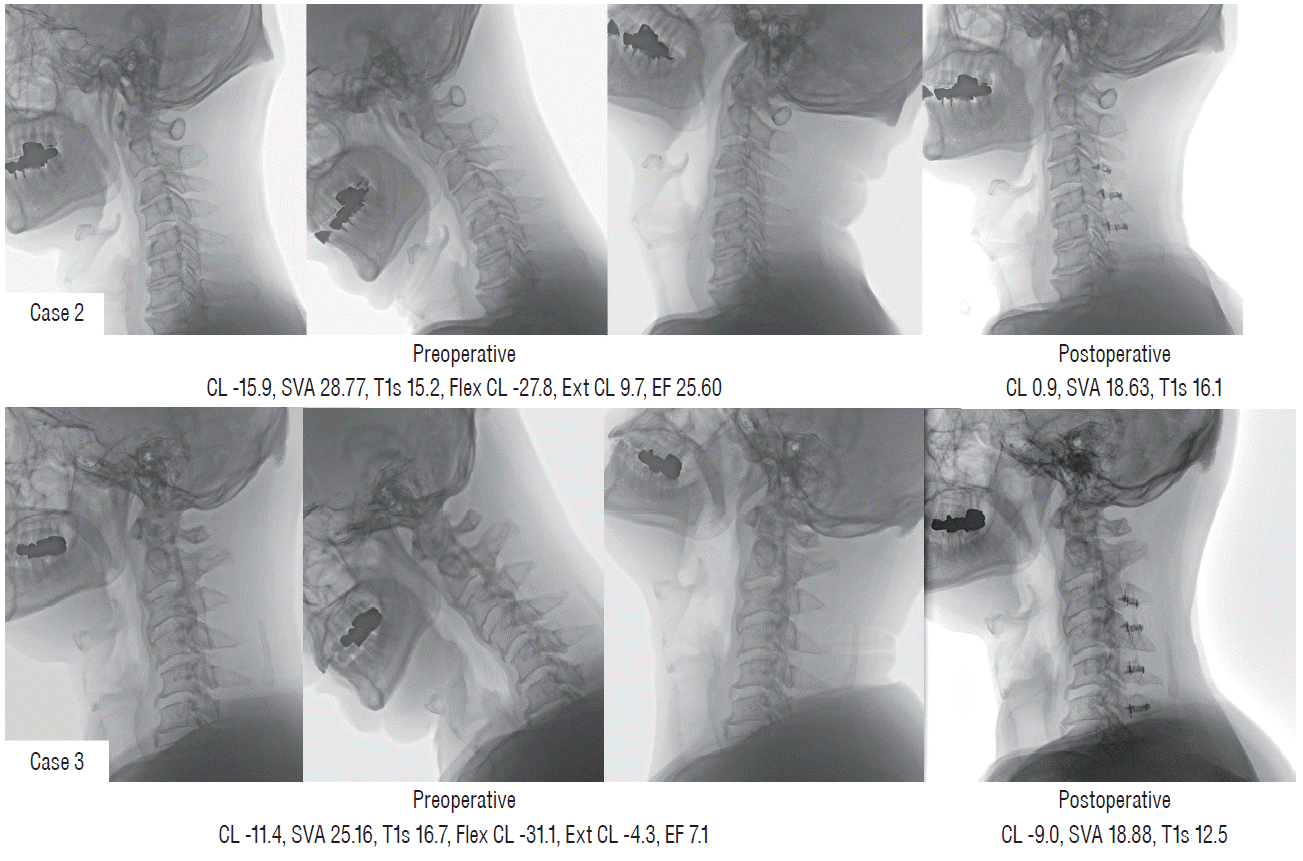 | Fig. 5.Different postoperative alignment and clinical outcomes in two patients with preoperative kyphotic alignment (case 2 [upper] and case 3 [lower]). CL : cervical lordosis, SVA : sagittal vertical axis, T1s : T1 slope, Flex CL : cervical lordosis in flexion position, Ext CL : cervical lordosis in extension position, EF : extension function. |
Case 3 (Figs. 5 and 6)
Case 4 (Fig. 7)
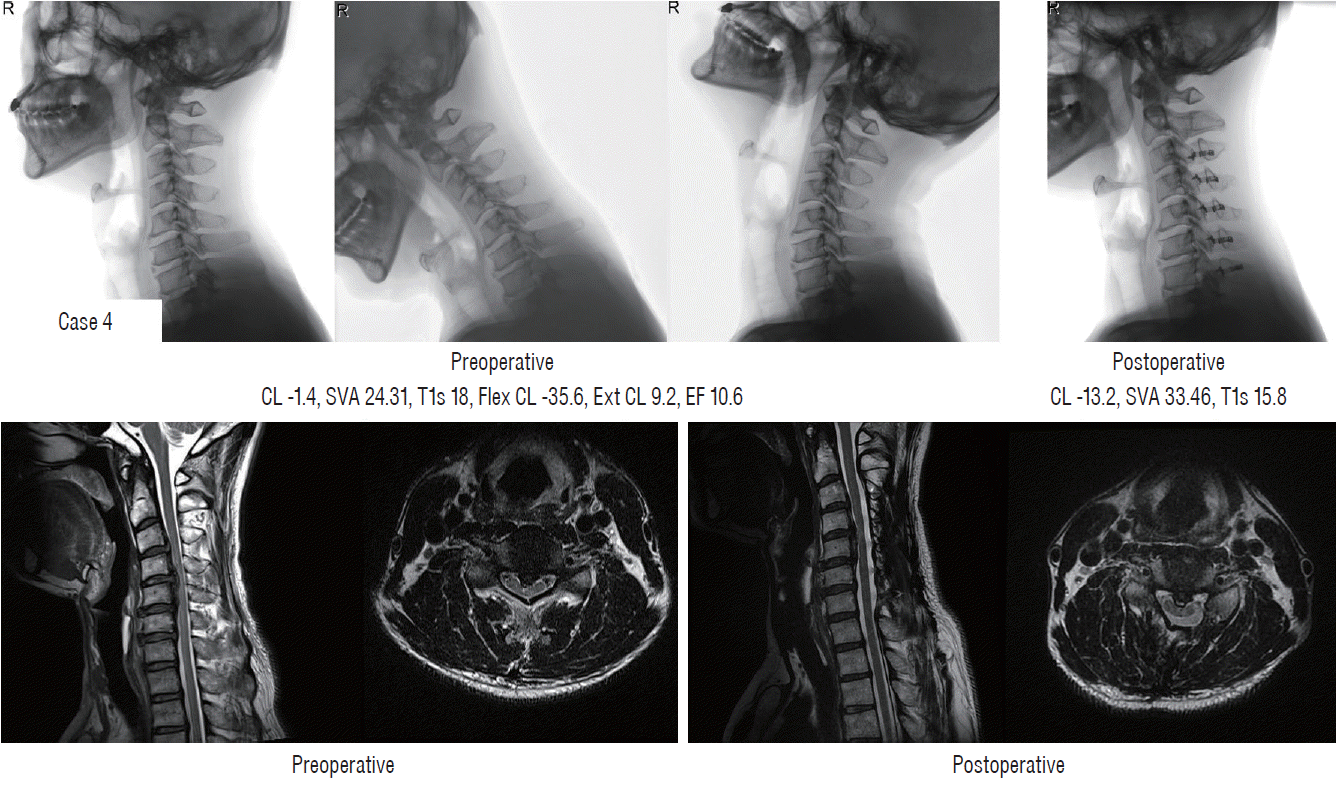 | Fig. 7.Failure of indirect decompression following loss of cervical lordosis in preoperative straight alignment patients (case 4). CL : cervical lordosis, SVA : sagittal vertical axis, T1s : T1 slope, Flex CL : cervical lordosis in flexion position, Ext CL : cervical lordosis in extension position, EF : extension function. |




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download