Introduction
Materials and methods
1. Subjects
2. Methods
1) Demographic characteristics
2) Cephalometric analysis
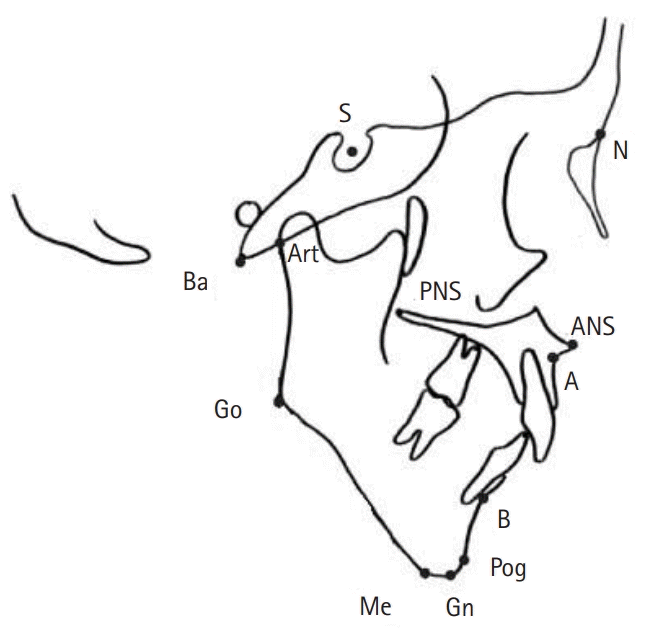 | Fig. 1.Cephalometric landmarks. S, sella; N, nasion; Ba, basion; Art, articulare; PNS, posterior nasal spine; ANS, anterior nasal spine; Go, gonion; A, subspinale; B, supraentale; Pog, pogonion; Me, menton; Gn, gnathion. |
Table 1.
Table 2.
| Measurement | Abbreviation | Cephalometric landmark |
|---|---|---|
| Linear | ||
| Anterior cranial base lengtha) | ACB | N-S |
| Posterior cranial base lengtha) | PCB | S-Ba |
| Total cranial base length | TCB | N-Ba |
| Upper anterior facial heighta) | UAFH | N-ANS |
| Upper posterior facial height | UPFH | S-PNS |
| Lower anterior facial heighta) | LAFH | ANS-Me |
| Anterior total facial heighta) | ATFH | N-Me |
| Posterior total facial height | PTFH | S-Go |
| Maxillar lengtha) | MaxL | ANS-PNS |
| Mandibular ramus lengtha) | MandRL | Art-Go |
| Mandibular corpus lengtha) | MandCL | Go-Pog |
| Overall mandibular length | OMandL | Art-Pog |
| Angular | ||
| Saddle anglea) | SA | N-S-Art |
| Gonial angle | GA | Art-Go-Me |
| Mandibular plane anglea) | MPA | S-N-Go-Gn |
| Position of maxillaa) | SNA | S-N-A |
| Position of mandiblea) | SNB | S-N-B |
| Maxilla/mandiblea) | ANB | A-N-B |
| Posterior position of mandible | PPMand | S-N-Art-Go |
a) For these variables, norms are given in Broadbent et al. [15],1975.
3) Statistical analysis
Results
1. Demographic characteristics of the study subjects
2. Cephalometric analysis
Table 4.
Values are presented as mean±standard error.
SS-HD, short-statured children with growth hormone deficiency; SS-I, idiopathic short-statured children; NC, normal children; ACB, anterior cranial base length; PCB, posterior cranial base length; TCB, total cranial base length; UAFH, upper anterior facial height; UPFH, upper posterior facial height; LAFH, lower anterior facial height; ATFH, anterior total facial height; PTFH, posterior total facial height; MaxL, maxillar lenghth; MandRL, mandibular ramus length; MandCL, mandibular corpus length; OMandL, overall mandibular length.
p-value of MANOVA, Bonferroni correction (a<b<c).
Table 5.
Values are presented as mean±standard error.
SS-HD, short-statured children with growth hormone deficiency; SS-I, idiopathic short-statured children; NC, normal children; SA, saddle angle; GA, gonial angle; MPA, mandibular plane angle; SNA, position of maxilla; SNB, position of mandible; ANB, maxilla versus mandible; PPMand, posterior position of mandible.
p-value of MANOVA, Bonferroni correction (a<b<c).




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download