A 22-year-old male patient with discoloration and gingival recession of the maxillary right central incisor received endodontic treatment due to injury nine years ago. He presented at the Department of Prosthodontics, Chonbuk National University Hospital. Maxillary right central incisor showed grade II mobility (according to the Miller classification). The 5 mm of periodontal pocket depth was measured at distal surface. Half of his palatal surface of teeth was destroyed (
Fig. 1). Cone-beam computed tomography (CBCT) was taken to evaluate bone height and width. Considering the age and sex of the patient, the tooth with poor prognosis was extracted and implant placement was determined.
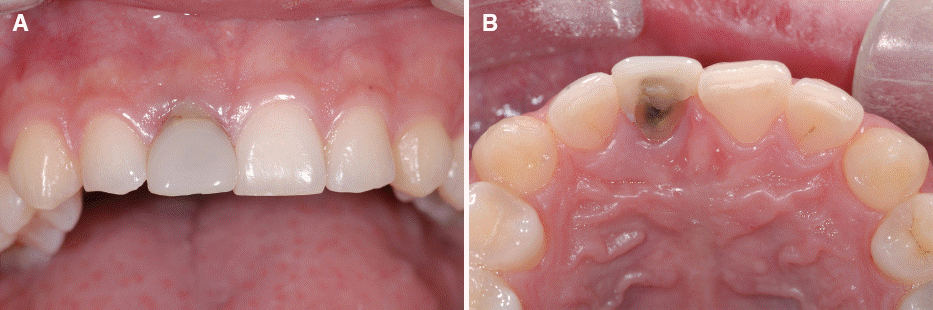 | Fig. 1Initial examination. (A) Right maxillary central incisor showing discoloration, (B) Destroyed palatal surface. 
|
After 3 months for tooth extraction, guided bone regeneration (GBR) was performed with xenograft material (Bio-Oss
®, Geistlich, Wilhusen, Switzerland), titanium mesh (T4 Neo tatinium mesh, Neobiotec, Seoul, Korea), and collagen membrane (Genoss Co., Ltd., Suwon, Korea) to obtain wide alveolar bone. At 7 months post GBR surgery, implant fixture (Superline 3.6 × 12 mm, Dentium Co., Seoul, Korea) was placed. Good initial stability was observed. After 6 months, the second surgery was carried out. Since good osseointegration was observed, provisional restoration was connected with 20 Ncm. Interdental papilla was stably maintained for 3 months (
Fig. 2). For duplicating the emergence profile of provisional restoration, custom impression coping was fabricated with pick-up type impression coping (DPU4011HL, Dentium Co., Seoul, Korea). Final impression was taken with polyvinyl siloxane (Aquasil XLV/Monophase, Dentsply Caulk, Milford, USA). Working cast was fabricated with type IV dental stone (Fuijirock EP, GC, Tokyo, Japan). Zirconia custom abutment with titanium insert (RaphaBio, Seoul, Korea) and veneered zirconia restoration was fabricated with CAD/CAM.
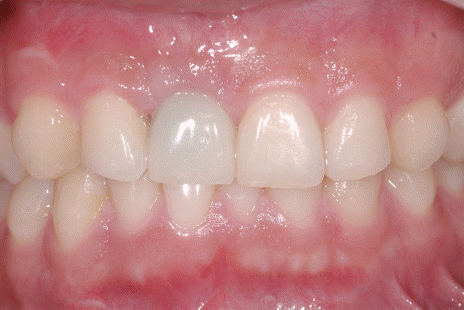 | Fig. 2Soft tissue around implant was well maintained for 3 months after connecting provision restoration. 
|
For fabricating the abutment replica with HMA, a thin layer of petroleum jelly (Vaseline, Unilever, London, UK) was applied to the inner surface of the zirconia crown using a microbrush (Microbrush International, Grafton, USA). The HMA (GS1085, Okong, Incheon, Korea) was filled inside of the restoration using an electronic glue gun (G250, Okong, Incheon, Korea). Dowel pin (Twin pin, World D&D Co., Seoul, Korea) was placed into the HMA and the replica was immersed into water to determine the space for cement after shrinkage (
Fig. 3A). If any defect was found on the surface of HMA abutment replica in this stage, a small amount of HMA could be used re-fill the restoration and re-seat the replica. After HMA was cooled, any excess HMA present in the margin of the abutment replica was trimmed with a knife (
Fig. 3B). After that, the custom abutment was connected to the implant for 30 Ncm with electric torque wrench (iSD 900, NSK Inc., Kanuma, Japan). The occlusal contact of the restoration was adjusted using a conventional procedure. After 10 minutes, screw was re-tighten
10 and screw hole was filled with cotton pellet and composite resin (Filtek z250, 3M EPSE AG, Seefeld, Germany). The inner surface of the restoration was cleaned with airborne particle abrasion. Resin cement (RelyX ultimate clicker, 3M EPSE AG) was applied along the margin with minimum amount.
11 The HMA abutment replica was seated to the restoration with a light pressure (
Fig. 4A). Any excess cement around the margin was wiped and the abutment replica was immediately pulled off. After confirming that the cement has been evenly applied to the inner surface of the restoration (
Fig. 4B), the restoration was seated on the abutment within the oral cavity. Any cement flowing outside was removed after the cement was hardened (
Fig. 5). Patient instruction for cleaning was conducted. At re-call check appointments after 1, 3, 6 months, no exudation or pus discharge was observed. The patient was satisfied with the esthetics and function of the prostheses.
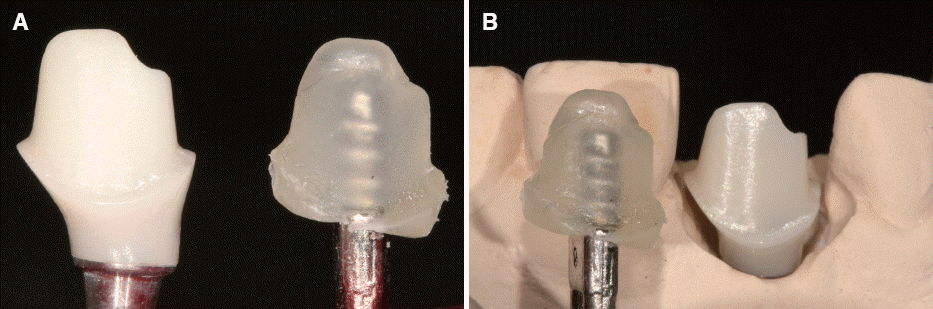 | Fig. 3(A) Fill the restoration with melted HMA and place the dowel pin, (B) Zirconia custom abutment (right) and hot melt adhesive material replica (left). 
|
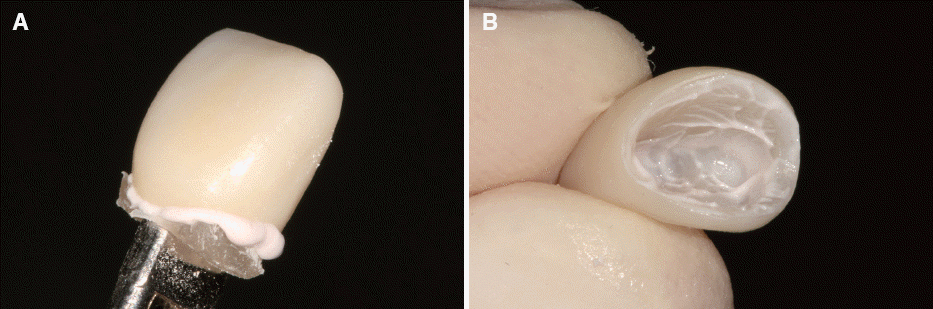 | Fig. 4(A) Apply cement, seat abutment replica, and wipe off excess cement, (B) Remove replica from seating and confirm that the cement has coated the inside. 
|
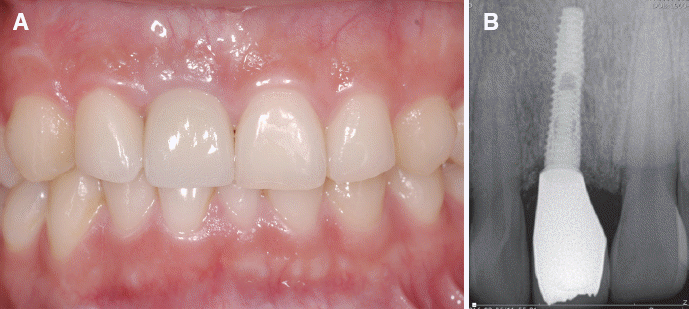 | Fig. 5(A) Zirconia crown was cemented with resin cement, (B) Periapcal radiograph. No cement remaining was observed. 
|

