INTRODUCTION
CASE REPORT
1. Clinical findings
2. Image and pathologic findings
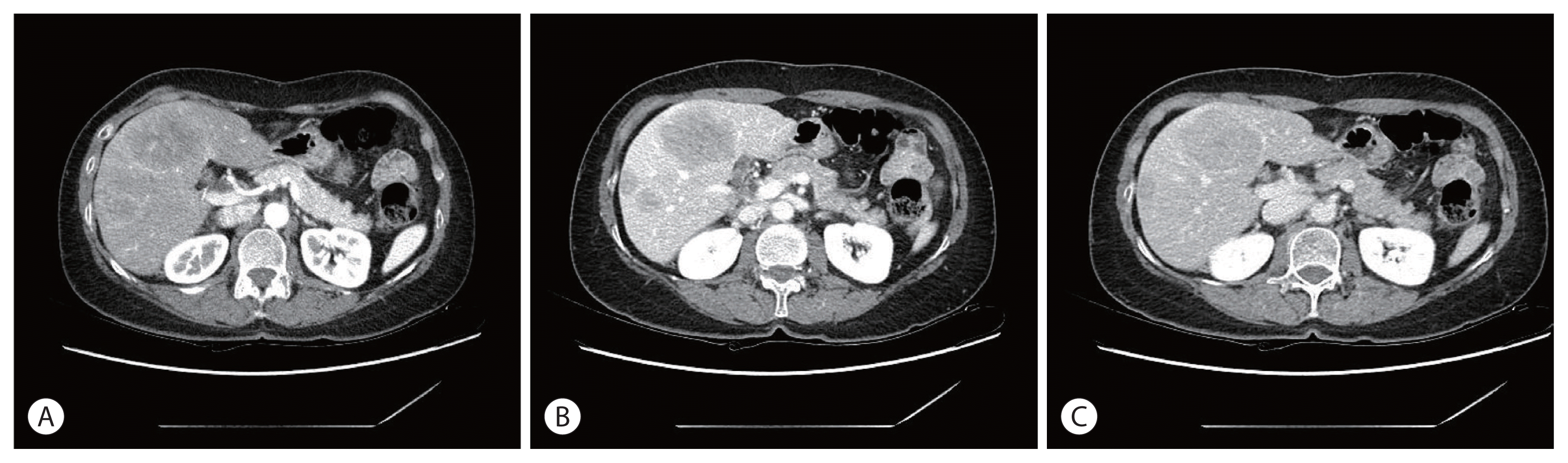 | Figure 1Liver dynamic computed tomography image findings. Multinodular liver masses measuring 6 cm in the greatest diameter in both hepatic lobes show heterogeneous enhancement during the arterial phase (A) and washout during the portal venous and delayed phases (B, C). |
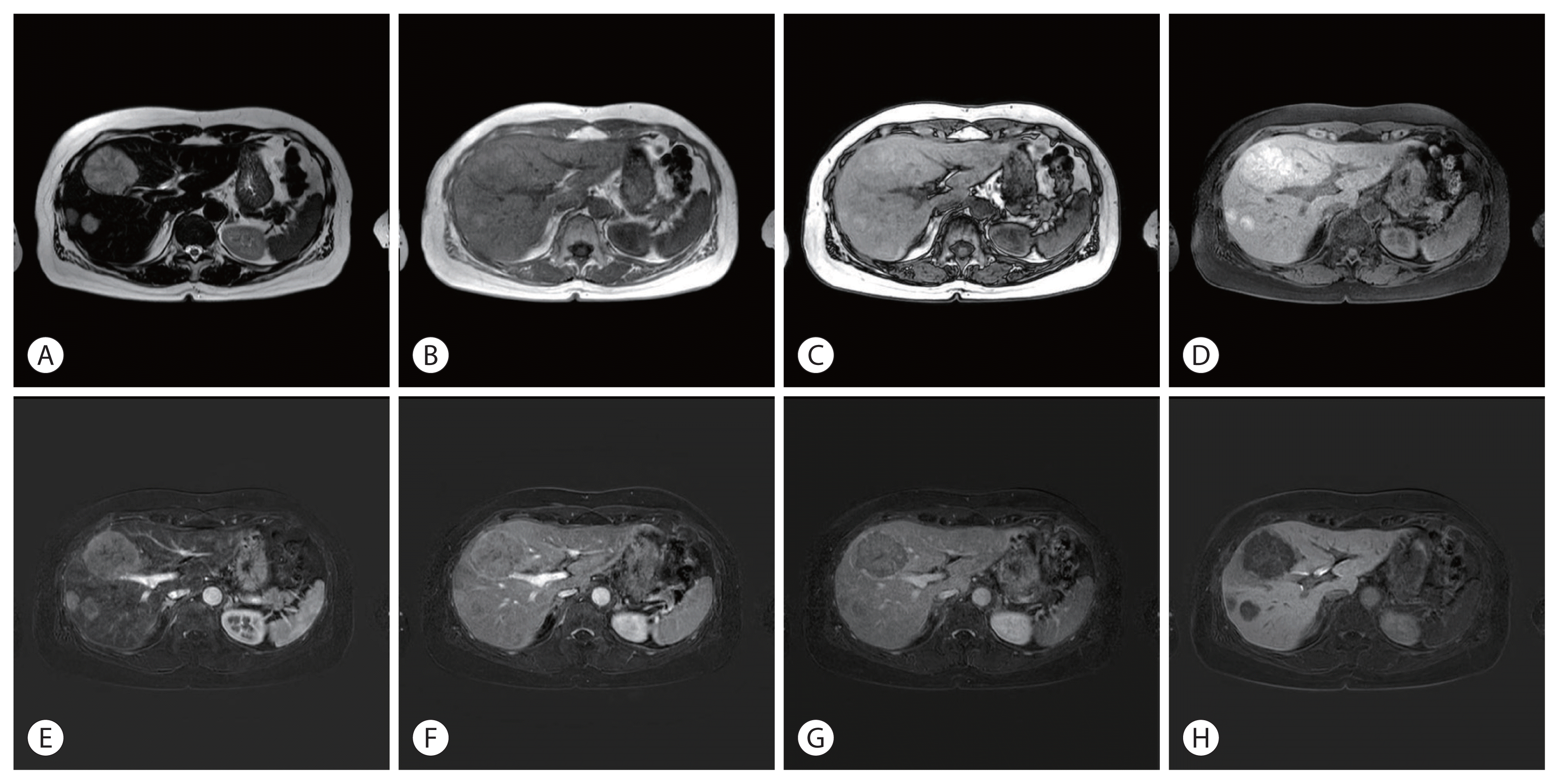 | Figure 2Liver dynamic magnetic resonance imaging image findings. Multiple liver masses show hyperintensity on T2-weighted images (A), isointensity on T1-weighted in-phase and out-of-phase images (B, C). Fat suppression increases the conspicuity of the lesion. A fat-suppressed T1-weighted image shows high signal intensity (D), a finding that suggests hemorrhage or melanin. Dynamic images after the administration of contrast agents show hyperintensity during the arterial phase (E), isointensity during the portal venous phase (F), and hypointensity during the delayed phase (G) and hepatobiliary phase (H). |




 PDF
PDF Citation
Citation Print
Print


 XML Download
XML Download