This article has been
cited by other articles in ScienceCentral.
Abstract
Although intracranial hemorrhage from arteriovenous malformation (AVM) during pregnancy is rare, it can have fatal consequences. Anesthetic techniques for these patients should ensure precise hemodynamic control, and the goals of anesthesia should include both fetal and maternal well-being. We report a case of anesthetic management for cesarean section in a 31-year-old woman who presented at 32 weeks gestation with an acute intracranial hemorrhage secondary to rupture of a previously diagnosed AVM. Our medical team decided to perform emergent cesarean section under regional anesthesia before transferring the patient to the neurosurgical intensive care unit for further monitoring and appropriate postoperative pain control. The patient was alert and cooperative during neuraxial anesthesia. The operation was successful, and the patient showed gradual improvement in neurosurgical status after several days. We concluded that in case of emergency, regional anesthesia can be a safe strategy for cesarean section in a pregnant woman with symptomatic AVM.
Keywords: Arteriovenous malformation, Cesarean section, Pregnancy, Regional anesthesia, IN
INTRODUCTION
Rupture of an intracranial arteriovenous malformation (AVM) during pregnancy is rare, with a reported incidence of 1 in every 10,000 pregnancies [
1], but it may have fatal consequences [
2]. Hemorrhagic stroke is a serious complication of AVM rupture during pregnancy and puerperium that has a substantial maternal mortality rate of 35% to 83% and contributes to at least 5% to 12% of all maternal deaths [
3]. There is a controversy among investigators as to whether the risk of AVM rupture is increased in pregnant women [
4-
6]. Nonetheless, when pregnant patients present with a ruptured AVM, aggressive management is warranted. The reported maternal mortality after AVM rupture during pregnancy is 28%, fetal mortality is 14%, and the risk of re-bleed during the same pregnancy (27% to 30%) is greater than the risk of re-bleed within one year (6%) in non-gravid women [
3,
7].
Anesthetic management of pregnant women with ruptured AVM poses multiple challenges to the anesthesiologist. Anesthetic techniques during cesarean section in these patients should ensure precise hemodynamic control [
8], but there are no definitive guidelines for these techniques because of the rarity of this condition. This is a report of successful administration of neuraxial anesthesia for emergency cesarean section in a case of ruptured maternal AVM.
CASE REPORT
A 31-year-old woman (gravida-2, para-1, height 162 cm, weight 62.0 kg, American Society of Anesthesiologists physical status classification 2) was admitted to our hospital at 32 weeks and 5 days gestation with a sudden headache accompanied by nausea and vomiting. Her past medical history was significant for embolization of an AVM 11 years ago and for four gamma knife radiosurgery procedures 10 years ago. She had undergone cesarean section under regional anesthesia 2 years ago. The patient was alert and oriented to person, place, but not time. The main neurologic finding was acute onset of a left homonymous hemianopsia. There were no abnormalities in laboratory findings and the electrocardiogram and chest radiograph were also normal. Computed tomography (CT) of the head showed a right parietooccipital intracranial hemorrhage extending to both lateral ventricles and the third and fourth ventricles with a mass effect causing left midline shift (7 mm) and suspected bilateral uncal herniation (
Fig. 1).
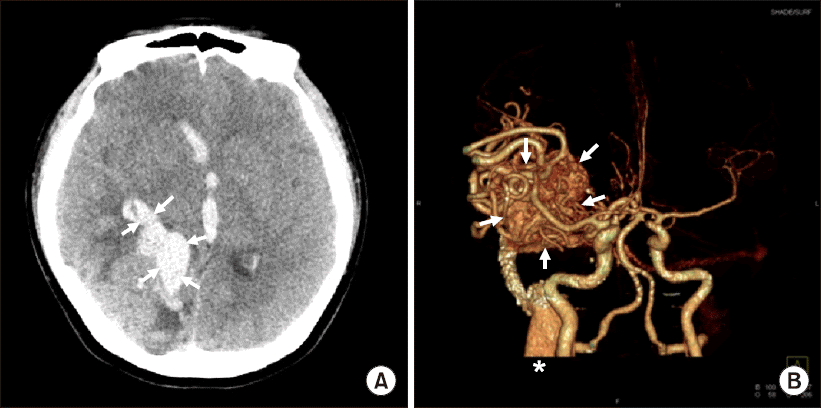
Fig. 1
Brain computed tomography (CT) and angiography findings of a 32-weekpregnant woman with ruptured cerebral arteriovenous malformation (AVM). CT at admission shows an intracranial hemorrhage (arrow) in the right parieto occipital lobe extending to the ventricles with a mass effect causing a midline shift to the left (7 mm) with possible bilateral uncal herniation (A). CT angiography shows a residual AVM nidus of approximately 5 × 4 × 3 cm (arrow) fed by branches of cerebral and drained by an engorged draining vein (*) (B).
The patient initially presented with vomiting and headache. As time passed, the neurological symptoms receded and the patient developed severe labor pain. Considering both maternal and fetal risks and benefits, the anesthesiologists, neurologists, and obstetricians discussed the case and decided to perform emergent cesarean section following AVM embolization. Because the patient was relatively alert and cooperative, we decided to use regional anesthesia for the cesarean section.
The patient’s preoperative vital signs were well controlled. The blood pressure (BP; systolic/diastolic) was 112/64 mmHg and the heart rate was 83 beats/min. The preoperative hemoglobin level was 11.8 g/dl, and the other laboratory findings were normal. We began standard monitoring (electrocardiogram, pulse oximetry, noninvasive blood pressure) when the patient arrived at the operating room, and the initial BP, heart rate, and peripheral oxygen saturation (SpO2) on room air were 120/64 mmHg, 90 beats/min, and 100%. Fetal heart rate was 130–140 beats/min with good variability. Oxygen was administered via nasal cannula at a rate of 2 L/min and there was one 18-gauge intravenous line in the patient’s left arm, 1,000 ml of crystalloid was administered over 10 min. We performed a combined spinal-epidural block at the 4th–5th lumbar interlaminar space under aseptic conditions with the patient in left lateral decubitus position by a needle-through-needle technique with an 18-gauge Tuohy and 25-gauge pencil point spinal needle via the median approach. Loss of resistance was noted at 5.5 cm. After dura puncture, we confirmed cerebrospinal fluid return before intrathecal administration of 7 ml 5% heavy bupivacaine and 15 μg fentanyl. An epidural catheter was inserted and the tip was advanced 5 cm into the epidural space, after which 3 ml 1% lidocaine was slowly administered into the epidural space. No changes were observed in vital signs. We subsequently assessed the extent of bilateral sensory blockade by observing the loss of cold sense to alcohol sponges and the loss of pain sense to pinpricks. A sensory block to the level of T4 was obtained. During aseptic drape for surgery, prophylactic phenylephrine was administered 50 μg only once.
The obstetricians proceeded with the surgery at 20 min from the time of induction, and at 26 min the patient delivered a male infant weighing 2,380 g. The Apgar scores were 9 and 10 at 1 and 5 minutes, respectively. The infant was transferred to the neonatal intensive care unit. The mother’s intraoperative vital signs were stable and well maintained within normal range (BP 118/60 mmHg, heart rate 76 beats/min, and SpO
2 100%). She received 1 g intravenous cefazolin immediately after the baby was delivered as well as 3 mg midazolam and 35 μg fentanyl intravenously after placental expulsion, and she remained comfortable until the end of surgery. The total operative time was 40 min, and the anesthesia time was 70 min. The patient received a total of 1,400 ml of crystalloid (lactated Ringer’s solution 300 ml and plasma solution 1,100 ml). Estimated blood loss and urine output were 1,000 ml and 90 ml, respectively. The intraoperative BP range was 110–130/50–60 mmHg and the heart rate was 70–93 beats/min (
Fig. 2).
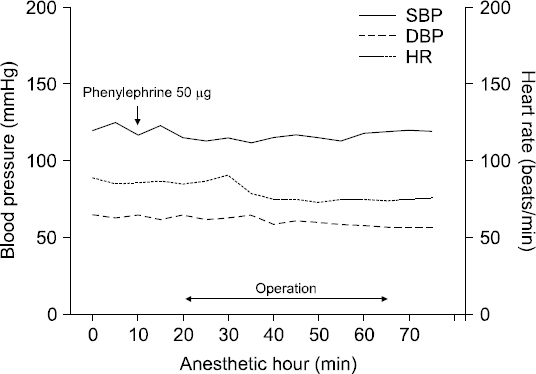
Fig. 2
Hemodynamic status during regional anesthesia for cesarean delivery in a pregnant woman with ruptured cerebral rteriovenous malformation. SBP: systolic blood pressure, DBP: diastolic blood pressure, HR: heart rate.
The patient was transferred to the neurosurgical intensive care unit for monitoring and her postoperative pain was managed with an epidural patient-controlled analgesia device (0.12% ropivacaine 200 ml with fentanyl 1,000 μg, basal rate 2 ml, bolus 2 ml, lockout time 15 min, volume limit 10 ml/h) for 3 days. She stayed in the neurosurgical intensive care unit for 17 days, during which her neurological status gradually improved with conservative management. A follow-up non- contrast CT scan confirmed decreased volume of the intracranial hemorrhage in the right parietooccipital region and in the ventricles, and the patient was cleared for discharge on postoperative day 17. After 23 days she was re-admitted for embolization, remained asymptomatic, and was discharged on the seventh day post-embolization.
DISCUSSION
AVM is an abnormal tangle of blood vessels, usually in the brain or spine, in which arteries shunt directly into veins with no intervening capillary bed. The cause of cerebral AVM is unknown, but AVM is usually congenital and forms during the third week of fetal development. Although the prevalence of cerebral AVM in humans cannot be precisely determined, AVM is uncommon and estimates vary from about 0.001% to 0.5% of the population [
1,
9-
11]. AVM is frequently asymptomatic and therefore remains undiagnosed [
4], but AVMs can cause severe and devastating effects when they bleed.
The natural history of AVM in pregnant patients is poorly understood because AVM is rare and the mother’s body undergoes complex changes during pregnancy. Whether the risk of rupture is increased during pregnancy remains controversial. Several case reports and at least one single-center analysis have suggested that pregnancy increases the risk for hemorrhagic stroke, which can be partly explained by an increased tendency for cerebral AVMs to rupture during pregnancy [
9]. It has been reported that pregnant women may have a four times greater risk of AVM rupture than non-pregnant women [
7]. This risk was associated with other risks of pregnancy (hypertension, increased age, coagulopathy, disseminated intravascular coagulation, and recent use of vasoactive substances), and the authors hypothesized that the increase in cardiac output associated with pregnancy, and especially labor, can stress fragile AVMs and render them more susceptible to rupture [
7]. However, Horton et al. [
4] reported that pregnancy is not a risk factor for hemorrhage in women without a previous hemorrhage.
To date, there is no definitive guideline for the treatment of AVM during pregnancy, and the optimal management of cerebrovascular disease in pregnancy is under discussion [
4-
6]. In most cases, management decisions for pregnant patients with ruptured AVMs should be based primarily on neurosurgical indications rather than on obstetrical indications [
12]. When maternal AVM rupture causes neurological deterioration, emergency surgery is necessary. However, if the fetus is sufficiently mature, simultaneous cesarean section is possible.
In the present case, the patient had a known AVM and had undergone embolization 11 years before the AVM re-ruptured during her second pregnancy. The patient initially presented with vomiting and headache, but as time passed, the neurological symptoms receded and the patient developed severe labor pain, which prompted the neurosurgeons, obstetricians, and anesthesiologists to recommend cesarean section before emergent neurosurgery or embolization after determining that the risk of fetal death had become greater than the risk to the mother. Although dural puncture in patients with evidence of increased intracranial pressure can produce cerebellar herniation, we decided to perform the cesarean section under regional anesthesia rather than under general anesthesia, because neuraxial anesthesia has indisputable advantages and because the mother was alert and mostly able to cooperate. Neuraxial anesthesia eliminates the risk of hemodynamic instability caused by endotracheal intubation and avoids increased intracranial pressure associated with positive pressure ventilation, which can also lead to AVM re-rupture. On follow-up head CT, the patient’s intracranial hemorrhage appeared to be receding, and there were no complications related to the regional anesthesia or the dural puncture.
The primary anesthetic goal in this case was to maintain maternal hemodynamic stability [
13] to avoid hypotension or hypertension and subsequent utero-placental ischemia or increased risk of bleeding. Because failed epidural anesthesia converts to general anesthesia and results in a great hemodynamic change, the combined spinal-epidural technique is a common technique for obstetric anesthesia that can be used safely and effectively in community practices and academic institutions [
14]. It is well known that regional anesthesia has several advantages over general anesthesia. In addition to those mentioned above, regional anesthesia can also reduce the risk of hemodynamic instability caused by anesthetic drugs and opioids, as well as that associated with intubation and extubation. Moreover, regional anesthesia can prevent increased intracranial pressure associated with post-operative nausea and vomiting, and the indwelling epidural catheter provides a ready means of post-operative pain control [
15].
As noted, emergency cesarean section was the choice of the multidisciplinary team. When cesarean section is performed in a parturient with AVM rupture, the time of delivery and decision for any combined neurosurgical procedure should be made according to the clinical presentation, gestational age, and hemodynamic status of the mother, and the hemodynamic status, maturity, and viability of the fetus. Using the comprehensive neurological and obstetric knowledge, careful anesthetic management should be guided by comprehensive neurological and obstetrical data and should be tailored to maintain favorable hemodynamic status of the mother and viability of the fetus.
In conclusion, the cooperative management of the present case allowed for safe and successful emergency cesarean section under regional anesthesia before neurosurgical intervention in a patient with intracranial hemorrhage secondary to ruptured AVM



