Introduction
The term congenital cholesteatoma is most commonly used to describe tumors that occur in the middle ear. Some authors have used a broader definition of congenital cholesteatoma to include all epidermoid cysts in the central nervous system [
1]. Although there is no histopathological difference between congenital cholesteatoma and epidermoid cysts [
2], they do differ radiologically and clinically [
3-
5]. Warren, et al. [
5] reported that the clinical presentation of congenital cholesteatoma originated from mastoid. We also encountered a rare case of isolated mastoid congenital cholesteatoma expanding to the occipital bone. Although there may be controversy about whether the mass is a congenital cholesteatoma or an epidermoid cyst, we performed a successful treatment via transmastoid approach without craniotomy. So, we report our experience and provide a review of the literature regarding congenital cholesteatoma isolated to the mastoid.
Go to :

Case
The Institutional Review Board of Chonnam National University Hospital approved this study protocol (CNUHEXP-2016-332). A 69-year-old woman presented with a recent (3 days) onset of headache and dizziness. Dizziness was non-whirling type and there was no specific neurological symptom. She had a 2-months history of left-sided otorrhea that was poorly responsive to empirical treatment at a primary hospital. She had no previous history of surgery. She was misdiagnosed as congenital middle ear cholesteatoma at a primary hospital, because otoscope revealed whitish mass be“hind an intact ear drum (
Fig. 1). She was referred to a tertiary hospital under a diagnosis of congenital middle ear cholesteatoma. Pure tone audiometry revealed a conductive hearing loss. The left mastoid air cell and middle ear cavity appeared soft tissue attenuation on axial views of temporal bone computed tomography (TBCT) (
Fig. 2A). Coronal views of TBCT demonstrated a 4.7×2.2 cm mass-like space-occupying lesion expanding to the posterior cranial fossa that destroyed part of mastoid, parietal, and occipital (
Fig. 2B). The mass occluded the adjacent transverse sinus. It was hyperintense and mottled on T1-weighted magnetic resonance imaging (T1WI), hypointense on T2-weighted imaging (T2WI) without contrast-enhancing (
Fig. 3). Conventional C-shape post-auricular skin incision was made for surgical intervention. Tympanomeatal flap was elevated. A defect of the mastoid cortex was observed. Pus-filled keratinous material was suctioned through the defect. However, there was only a small amount of effusion inside the middle ear and no keratinous material. In addition, the middle ear mucosa and ossicles maintained normal structure. Mastoidectomy was performed from the point of cortical destruction identified from preoperative TBCT. Mastoidectomy revealed relative healthy mastoid air cell anteriorly and intact sigmoid sinus wall. However, there was purulent discharge-filled pearly keratinous material at restrosigmoid area to posterior cranial fossa (
Fig. 4). The mass was removed via transmastoid retrosigmoid approach without craniotomy. It was possible to achieve near-total excision, leaving only the adherent cholesteatoma sac lining behind, because it was tightly adhered to the dura. The exposed dura was not covered and open cavity mastoidectomy was performed without obliteration to detect changes in remnant cholesteatoma. Immediately after surgery, ear dressing with use of otic drop was performed frequently. At this time, partial removal of the remnant cholesteatoma using the suction was also performed. Pathologic examination of the surgical specimen disclosed considerable keratinous material and stratified squamous epithelium which were consistent with the diagnosis of cholesteatoma. Headache and hearing loss improved after surgery and, a follow-up CT imaging at 1 year post operation showed well marsupialized cavity (
Fig. 5).
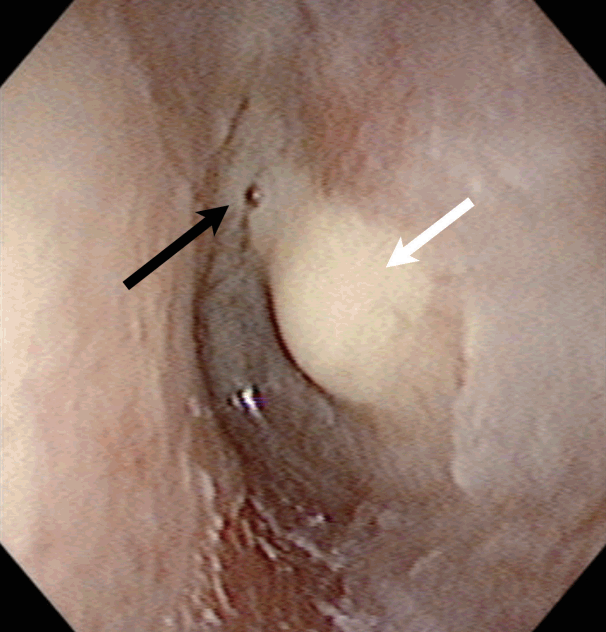 | Fig. 1.Images of left ear drum. Scanty prulent discharge (black arrow) is noted and there was whitish mass-like lesion (white arrow) behind an intact ear drum. 
|
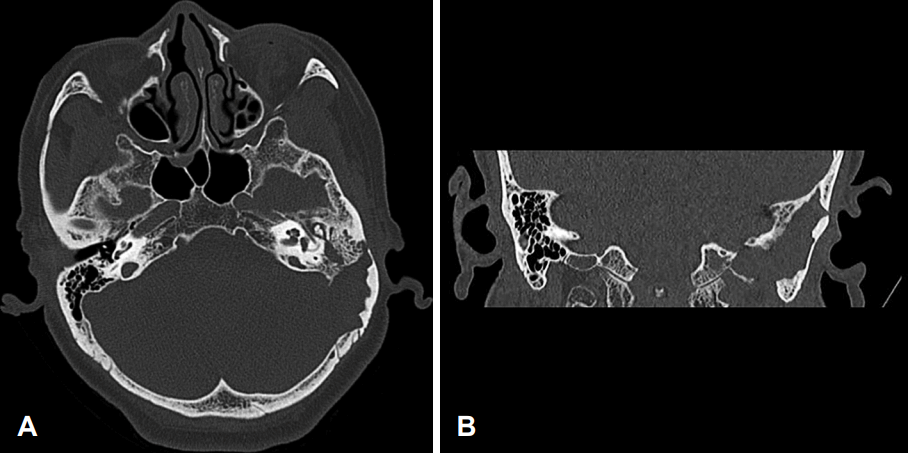 | Fig. 2.Computed tomographic images of left temporal bone showing soft tissue density on mastoid antrum and middle ear cavity, and eroded mastoid and posterior cranium; axial image (A), coronal image (B). 
|
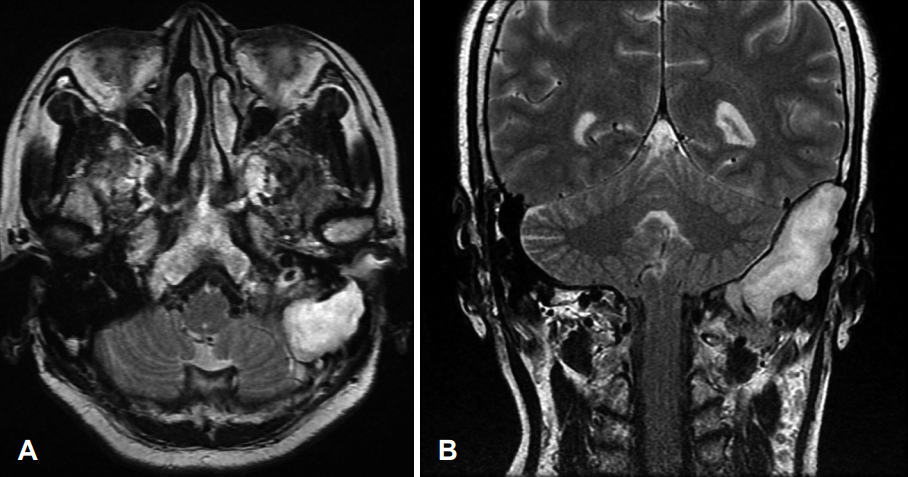 | Fig. 3.MRI scan demonstrating lesion of the left posterior fossa and temporal bone; high signal intensity on T2-weighted axial MRI scan (A), T2-weighted coronal MRI scan (B). 
|
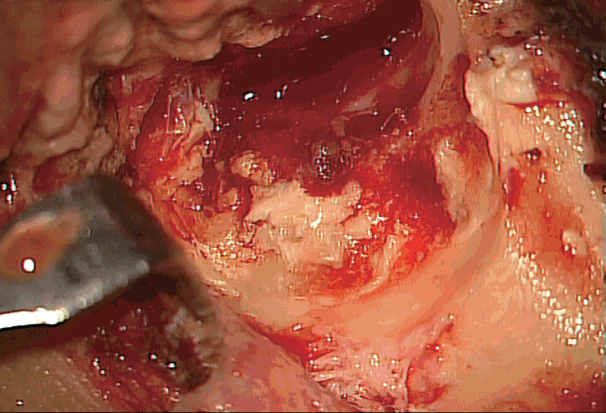 | Fig. 4.There was a purulent discharge-filled pearly keratinous material at poasterior mastoid. 
|
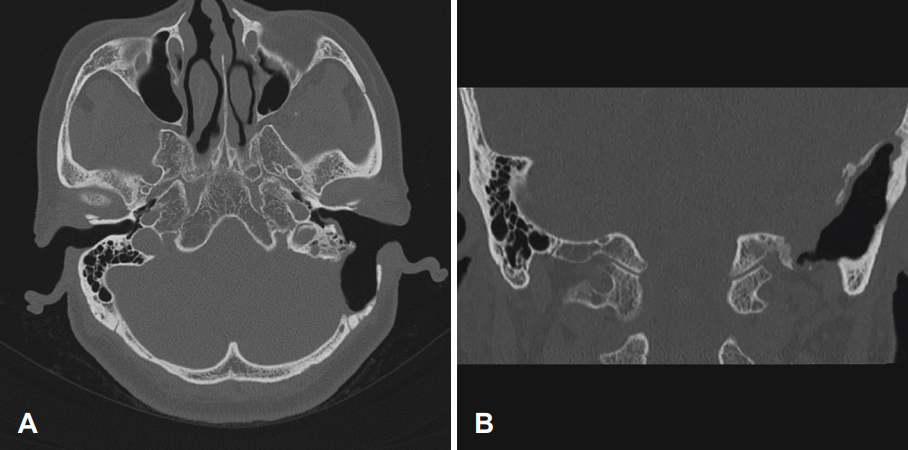 | Fig. 5.Postoperative axial image (A) and coronal image (B) of computed tomography shows well marsupialized cavity. 
|
Go to :

Discussion
It is difficult to differentiate congenital cholesteatoma from epidermoid cyst because they have similar radiologic, histopathologic and clinical features. Both of them have mass of soft tissue density, pressure erosion on adjacent bone, no contrast enhancement on CT, low signal intensity in T1WI, high signal intensity in T2WI, and no enhancement on MRI image. Pathologically, both have keratinized squamous epithelia, including keratin [
4,
6]. They typically present with painless mass of the scalp due to their slow growing nature. However, rarely complications including malignant change, abscess formation, hemorrhage, and intracranial mass effect do occur [
7]. Some authors suggest that epidermoid cyst and cholesteatoma are the same disease entity [
4].
However, congenital cholesteatoma tends to be more invasive into surrounding bones and air cells than epidermoid cyst. Congenital cholesteatoma destroys bone through osteoclastic bone resorption rather than through pressure necrosis secreting interleukin-α, fibroblast production, collagenase, and granulocyte-macrophage colony-stimulating factor [
5]. Lee [
3] suggested radiologic differences between cholesteatoma and epidermoid cyst. Epidermoid cyst has a rounder, well-demarcated contour with boundary between adjacent bones clearer and smoother. Cholesteatoma mostly shows sharply marginated and expansile mass with irregular and scalloped margin and accompanied by various degrees of bony erosion [
3].
Unlike usual clinical feature of epidermoid cyst, our case patient presented with intractable otorrhea. The most common symptom of an epidermoid cyst is painless swelling of scalp due to the slow growth of the tumor. When they become sizable, they may produce headache, increased intracranial pressure, seizure, on-going hemiparesis, and other local neurological signs [
4,
6-
8]. However, bone resorption by cholesteatoma may cause other problems such as hearing impairment and vertigo [
9], which is another difference between cholesteatoma and epidermoid cyst.
The reported patient had two months history of otorrhea. Her ear drum was intact. However, there was whitish masslike lesion behind the ear drum on otoscopic examination (
Fig. 1). CT and MRI showed that the mass expanded to the posterior cranial fossa and destroyed the temporal, parietal, and occipital bone. The mass compressed the lateral sinus (
Figs. 2 and
3). Although the mass did not involve middle ear cavity, the middle ear was filled with thick yellowish discharge. Considering both radiologic and clinical feature, we concluded that this was a case of isolated mastoid congenital cholesteatoma which involving temporal, parietal, occipital bone, and posterior cranial fossa. Moreover, this mass compressed and occluded the lateral sinus and it was well demonstrated by radiologic image. To our knowledge, only one case of large intradiploic epidermoid of temporal bone which compressed lateral sinus has been reported in the literature. However the mastoid of this case was preserved from a mass [
10].
Standard treatment of an intradiploic epidermoid cyst is surgical removal with complete resection [
8]. However, it needs craniotomy. Lesions localized in the area of the major dural sinuses are of special concern because potential major bleeding problems may occur during surgical exploration [
10]. To reduce complications from operation, keratinous materials were marsupialized and desquamated from the bone and dura mater carefully. During 30 months postoperative follow up period, there was an event of cavity problem. She developed otomycosis at postoperative 28 month. However, otomycosis was well controlled by vinegar irrigation.
This case showed the patient who presented with intractable otorrhea had a large congenital cholesteatoma that expanded to posterior cranial fossa and compressed major vessel causing epidural abscess to middle ear cavity. Even if patients only with otorrhea did not respond to medication with newly developed neurologic symptoms, imaging study should be performed. In addition, transmastoid marsupialization can be a choice for otolaryngologist in treating giant cholesteatoma that extends to post cranial fossa.
Go to :







 PDF
PDF Citation
Citation Print
Print





 XML Download
XML Download