Abstract
Background and Purpose
Methods
Results
Supplementary materials
Supplementary Table 1.
Supplementary Table 2.
Notes
Disclosure
Woo-Keun Seo received honoraria for lectures from Pfizer, Sanofi-Aventis, Otsuka Korea, Dong-A Pharmaceutical Co. Ltd., Bayer, Daewoong Pharmaceutical Co. Ltd., Daiichi Sankyo Korea Co. Ltd., and Boryung Pharmaceutical; study grants from Daiichi Sankyo Korea Co. Ltd.; a consulting fee from OBELAB Inc.; and stock option from JLK Inspection. The others have no financial conflicts of interest.
ACKNOWLEDGMENTS
References
Figure 1.
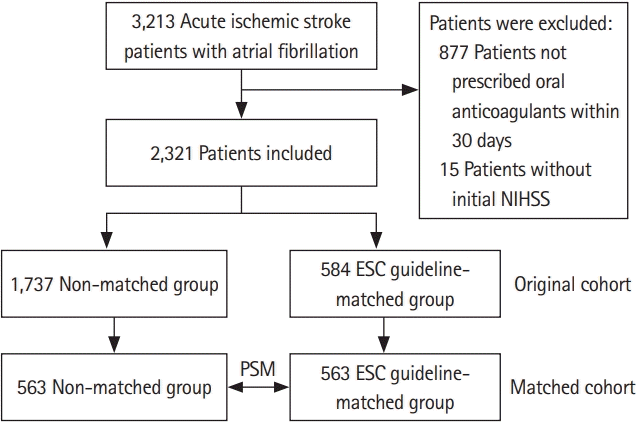
Figure 2.
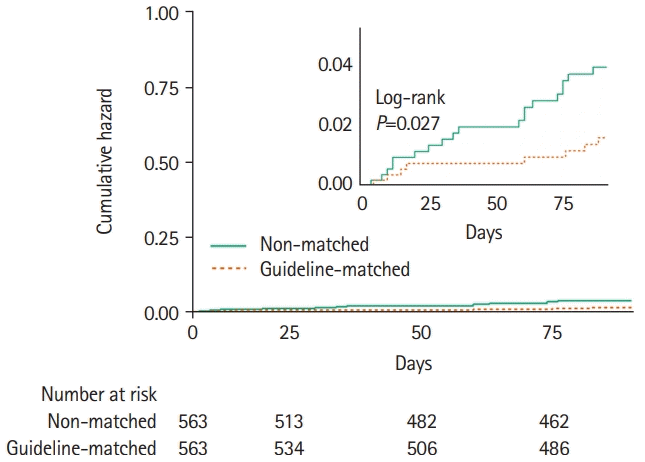
Figure 3.
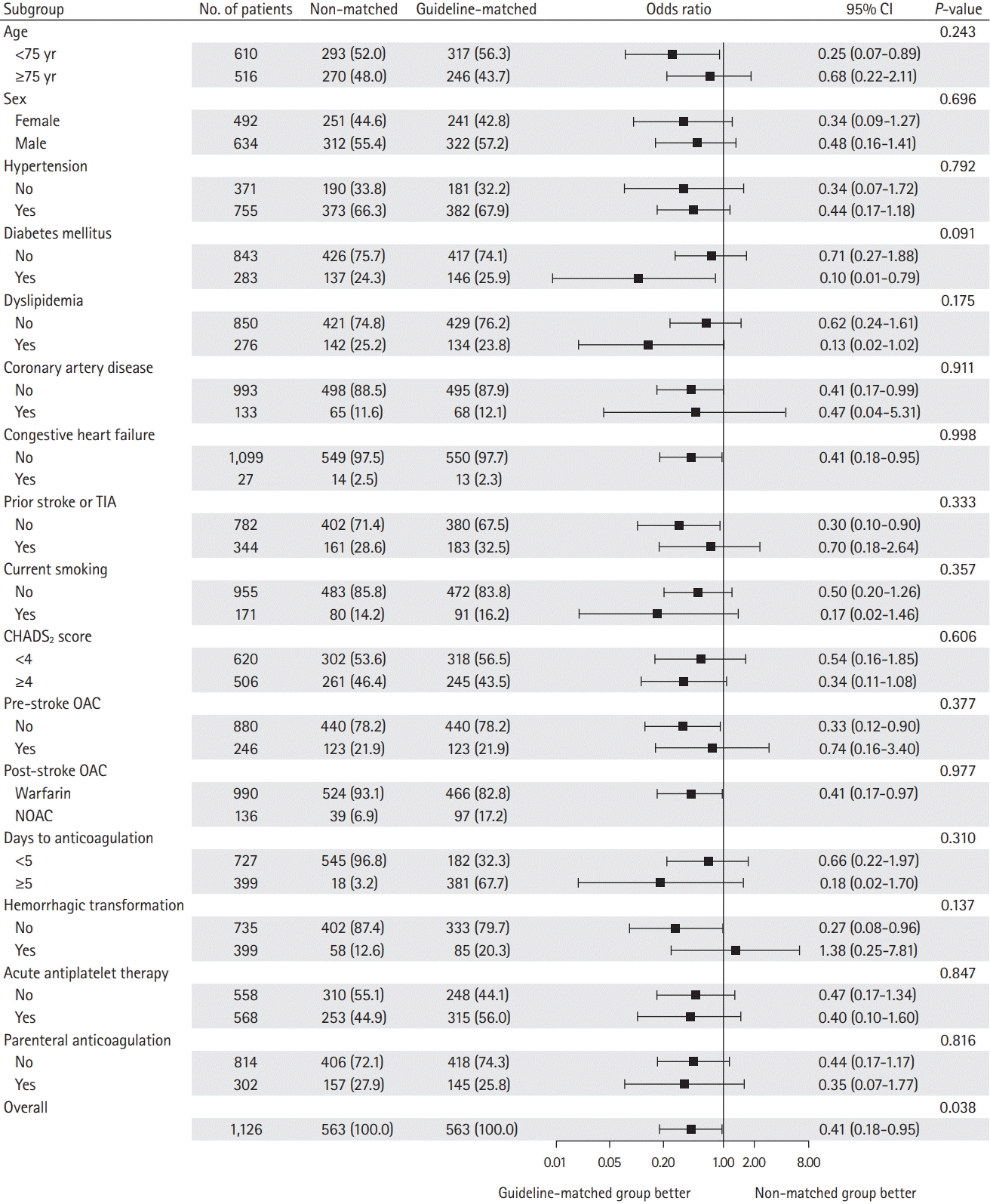
Table 1.
| Characteristic |
Original cohort |
Matched cohort† |
||||
|---|---|---|---|---|---|---|
| Non-matched (n=1,737) | Guideline-matched (n=584) | P * | Non-matched (n=563) | Guideline-matched (n=563) | P * | |
| Age (yr) | 73.1±9.9 | 71.9±10.0 | 0.003 | 72.8±10.2 | 71.9±10.0 | 0.040 |
| Male sex | 903 (52.0) | 331 (56.7) | 0.049 | 312 (55.4) | 322 (57.2) | 0.548 |
| History of risk factors | ||||||
| Hypertension | 1,195 (68.8) | 399 (68.3) | 0.831 | 373 (66.3) | 382 (67.9) | 0.568 |
| Diabetes mellitus | 475 (27.3) | 155 (26.5) | 0.705 | 137 (24.3) | 146 (25.9) | 0.536 |
| Dyslipidemia | 455 (26.2) | 142 (24.3) | 0.369 | 142 (25.2) | 134 (23.8) | 0.579 |
| Coronary artery disease | 228 (13.1) | 73 (12.5) | 0.697 | 65 (11.5) | 68 (12.1) | 0.782 |
| Congestive heart failure | 82 (4.7) | 17 (2.9) | 0.061 | 14 (2.5) | 13 (2.3) | 0.846 |
| Prior stroke or TIA | 627 (36.1) | 168 (28.8) | 0.001 | 161 (28.6) | 183 (32.5) | 0.155 |
| Peripheral artery disease | 226 (13.0) | 93 (15.9) | 0.617 | 6 (1.1) | 9 (1.6) | 0.436 |
| Current smoking | 1,195 (68.8) | 399 (68.3) | 0.077 | 80 (14.2) | 91 (16.2) | 0.361 |
| Prestroke OAC | 536 (30.9) | 123 (21.1) | <0.001 | 123 (21.8) | 123 (21.8) | 1.000 |
| Prestroke mRS | 0 (0–1) | 0 (0–1) | 0.001 | 0 (0–1) | 0 (0–1) | 0.107 |
| Initial NIHSS | 8 (2–15) | 4 (1–9) | <0.001 | 4 (1–9) | 4 (1–9) | 1.000 |
| Intravenous thrombolysis | 360 (20.7) | 112 (19.2) | 0.422 | 105 (18.7) | 108 (19.2) | 0.819 |
| Mechanical thrombectomy | 207 (11.9) | 41 (7.0) | 0.001 | 33 (5.9) | 36 (6.4) | 0.709 |
| CHADS2 score | 3 (3–4) | 3 (3–4) | 0.046 | 3 (3–4) | 3 (3–4) | 0.711 |
| Parenteral anticoagulation | 448 (25.8) | 152 (26.0) | 0.913 | 157 (27.9) | 145 (25.8) | 0.459 |
| Acute antiplatelet therapy | 789 (45.4) | 336 (57.5) | <0.001 | 258 (45.8) | 324 (57.5) | <0.001 |
| Days to OAC therapy | 0 (0–2) | 6 (4–13) | <0.001 | 0 (0–1) | 6 (4–13) | <0.001 |
| Hemorrhagic transformation (original cohort, n=1,906; matched cohort, n=564) | 199 (11.5) | 89 (15.2) | <0.001 | 58 (10.3) | 85 (15.1) | 0.002 |
| Poststroke OAC | <0.001 | <0.001 | ||||
| Warfarin | 1,626 (93.6) | 486 (83.2) | 524 (93.1) | 466 (82.8) | ||
| NOAC | 111 (6.4) | 98 (16.8) | 39 (6.9) | 97 (17.2) | ||
Values are presented as mean±standard deviation, number (%), or median (interquartile range).
TIA, transient ischemic attack; OAC, oral anticoagulation; mRS, modified Rankin Scale; NIHSS, National Institutes of Health Stroke Scale; CHADS2, congestive heart failure, hypertension, age ≥75 years, diabetes mellitus, prior stroke or TIA, or thromboembolism (doubled); NOAC, non-vitamin K antagonist oral anticoagulant.
* Continuous variables were compared between groups using Student's t-tests or Mann-Whitney U tests. The chi-square test was used for noncontinuous variables;
† Propensity score matching was performed using a logistic regression model with covariates including age, sex, hypertension, diabetes mellitus, dyslipidemia, coronary artery disease, congestive heart failure, prior stroke or TIA, peripheral artery disease, current smoking, prestroke OAC, prestroke mRS, initial NIHSS score, intravenous thrombolysis, mechanical thrombectomy, CHADS2 score, and parenteral anticoagulation.
Table 2.
| Outcomes |
Original cohort |
Matched cohort |
||||
|---|---|---|---|---|---|---|
| Non-matched (n=1,737) | Guideline-matched (n=584) | P * | Non-matched (n=563) | Guideline-matched (n=563) | P * | |
| Any stroke | 47 (2.7) | 8 (1.4) | 0.066 | 19 (3.4) | 8 (1.4) | 0.032 |
| MACCE | 156 (9.0) | 38 (6.5) | 0.069 | 38 (6.7) | 37 (6.6) | 0.905 |
| Ischemic stroke | 36 (2.1) | 5 (0.9) | 0.054 | 15 (2.7) | 5 (0.9) | 0.024 |
| Intracranial hemorrhage | 14 (0.8) | 3 (0.5) | 0.474 | 5 (0.9) | 3 (0.5) | 0.478 |
| Acute coronary syndrome | 16 (0.9) | 5 (0.9) | 0.886 | 2 (0.4) | 5 (0.9) | 0.255 |
| All-cause mortality | 93 (5.4) | 18 (3.1) | 0.026 | 16 (2.8) | 17 (3.0) | 0.860 |
| Major hemorrhage | 15 (0.9) | 10 (1.7) | 0.086 | 5 (0.9) | 10 (1.8) | 0.194 |
Table 3.
| Outcome | Univariate analysis | P * | Multivariate analysis | P * |
|---|---|---|---|---|
| Original cohort | ||||
| Any stroke | 0.50 (0.24–1.06) | 0.072 | 0.50 (0.24–1.06) | 0.072 |
| MACCE | 0.71 (0.49–1.02) | 0.063 | 0.84 (0.57–1.22) | 0.347 |
| Ischemic stroke | 0.41 (0.16–1.05) | 0.062 | 0.36 (0.14–0.92) | 0.032 |
| Intracranial hemorrhage | 0.64 (0.18–2.22) | 0.477 | 0.67 (0.19–2.36) | 0.537 |
| Acute coronary syndrome | 0.93 (0.34–2.55) | 0.886 | 0.87 (0.32–2.39) | 0.785 |
| All-cause mortality | 0.56 (0.34–0.94) | 0.028 | 0.79 (0.47–1.35) | 0.388 |
| Major hemorrhage | 2.00 (0.89–4.48) | 0.092 | 1.56 (0.68–3.60) | 0.294 |
| Matched cohort | ||||
| Any stroke | 0.41 (0.18–0.95) | 0.038 | 0.41 (0.18–0.95) | 0.038 |
| MACCE | 0.97 (0.61–1.55) | 0.941 | 0.97 (0.61–1.56) | 0.904 |
| Ischemic stroke | 0.33 (0.12–0.91) | 0.032 | 0.32 (0.11–0.88) | 0.028 |
| Intracranial hemorrhage | 0.60 (0.14–2.51) | 0.483 | 0.60 (0.14–2.51) | 0.483 |
| Acute coronary syndrome | 2.51 (0.49–13.01) | 0.272 | 2.38 (0.44–13.00) | 0.316 |
| All-cause mortality | 1.06 (0.53–2.13) | 0.860 | 1.09 (0.53–2.23) | 0.814 |
| Major hemorrhage | 2.02 (0.69–5.94) | 0.203 | 1.47 (0.48–4.48) | 0.499 |
Values are presented as odds ratios and 95% confidence interval. In the original cohort, MACCE was adjusted by age, congestive heart failure, prestroke modified Rankin Scale (mRS), CHADS2 (congestive heart failure, hypertension, age ≥75 years, diabetes mellitus, prior stroke or transient ischemic attack [TIA], or thromboembolism [doubled]) score, and initial National Institutes of Health Stroke Scale (NIHSS). Ischemic stroke was adjusted by diabetes mellitus and initial NIHSS. Intracranial hemorrhage was adjusted by prior stroke or TIA. Acute coronary syndrome was adjusted by age. All-cause mortality was adjusted by age, congestive heart failure, prestroke mRS, CHADS2 score, and initial NIHSS. Major hemorrhage was adjusted by the type of oral anticoagulants. Major hemorrhage was adjusted by the type of poststroke oral anticoagulants. In the matched cohort, MACCE was adjusted by initial NIHSS. Ischemic stroke was adjusted by diabetes mellitus. Acute coronary syndrome was adjusted by age, current smoking, and CHADS2 score. All-cause mortality was adjusted by age, dyslipidemia, congestive heart failure, CHADS2 score, and initial NIHSS. Major hemorrhage was adjusted by the type of poststroke oral anticoagulants.
ESC, European Society of Cardiology; MACCE, major adverse cerebrovascular, and cardiovascular events.




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download