Abstract
Acute adrenal insufficiency (AAI) in acute coronary syndrome (ACS) patients is rare and may be frequently underestimated as simple ACS, since symptoms of AAI are nonspecific. Physicians should be fully aware of the possibility of occult AAI combined with ACS, if clinical suspicion is high. Herein, we report a rare case of a 67-year-old female patient with concomitant AAI and drug eluting stent fracture-induced ACS. To our knowledge, there have been no case reports of AAI associated with ACS in Korea.
Acute adrenal insufficiency (AAI) is a rare but life hreatening complication in patients with chronic adrenal insufficiency. It presents nonspecific symptoms, such as fatigue, nausea, vomiting and hypotension, which can lead to underestimation. However, the ultimate prognosis of AAI critically depends on rapid administration of steroids by attending physician regardless of the underlying illness even before the diagnosis is made.[1,2]
AAI occurs in a substantial proportion of patients with chronic adrenal insufficiency mainly triggered by infectious disease, particularly gastrointestinal infections.[3] However, AAI has not yet been previously described in association with acute coronary syndrome (ACS), as a precipitating factor.
This case report shows a concomitant AAI and stent fracture induced ACS, in a 67-year-old female patient who had a past medical history of old myocardial infarction, rheumatoid arthritis, diabetes mellitus and hypertension. Since our case initially presented with classic symptoms and signs of ACS, it may have been overlooked. However, the history of steroid medication, sustained hypotension and unexplained abdominal pain led to high suspicion of AAI and ignorance of secondary adrenal insufficiency. After empirical and immediate steroid replacement with emergent percutaneous coronary intervention (PCI), she achieved clinical remission.
A 67-year-old female patient visited our emergency department with a 1-hour history of nausea, vomiting, abdominal pain and retrosternal chest pain. On arrival, her mentality was alert but gradually changed to drowsy status. She experienced new onset chest pain in that morning, which occurred at rest and was typically of squeezing type without radiating pain. The patient had complicated past medical history and comorbidities. Ten years prior to presentation, she had been diagnosed with diabetes mellitus and hypertension. At that time, she was treated with oral hypoglycemics and antihypertensive agents, and her blood glucose and pressure were well controlled. In addition, she had an AMI attack 4 years ago, and a zotarolimus-eluting stent was implanted in the postero-lateral branch of the right coronary artery along with anti-platelet agents. Also, she was diagnosed with rheumatoid arthritis 3 years ago and continually administered triamcinolone 2.5 mg daily prior to presentation. There was no other specific medical history.
Her vital signs were as follows: blood pressure 68/50 mmHg, pulse rate 94 beats/min, temperature 36.8°C and respiratory rate 22 breaths/min. Physical examination showed acutely ill appearance and her mentality gradually changed from conscious to drowsy status. There was no sign of skin hyper-pigmentation, conjunctiva pallor, sclera jaundice, or dilatation of the jugular vein. On chest auscultation breath sounds were clear without wheezing or crackles detected. Cardiac auscultation revealed heartbeats that were regular without murmurs. Bowel sounds were reduced and no mass was detected in the abdomen. No limb edema was seen.
The initial laboratory test results were as follows: white blood cells 7,930/mm3, hemoglobin 12.0 g/dl and platelets 336,000/mm3, total cholesterol 123 mg/dl, total protein 5.0 g/dl, albumin 3.3 g/dl, total bilirubin 1.4 mg/dl, alkaline phosphatase 289 U/L, aspartate aminotransferase 22 U/L, alanine aminotransferase of 28 U/L, blood urea nitrogen 38.7 mg/dL, creatinine 1.4 mg/dl, sodium 140 mmol/L, potassium 4.4 mmol/L, chloride 94 mmol/L and C-reactive protein 3.446 mg/L.
CK-MB, troponin-T and troponin-I were found to be 28.8 IU/L (normal value, 0–6.8 IU/L), 0.081 μg/L (normal value, 0.010–0.017 μg/L) and 0.10 μg/L (normal value, 0.010–0.023 μg/L), respectively all elevated.
Creatine phosphokinase 49 IU/L (normal value, 50–200 IU/L) and lactate dehydrogenase 212 IU/L (normal value, 106–211 IU/L)
N-terminal prohromone brain natriuretic peptide was 495 ng/L (normal value, 12–133 ng/L).
Chest X-ray and magnetic resonance imaging of the brain showed normal finding.
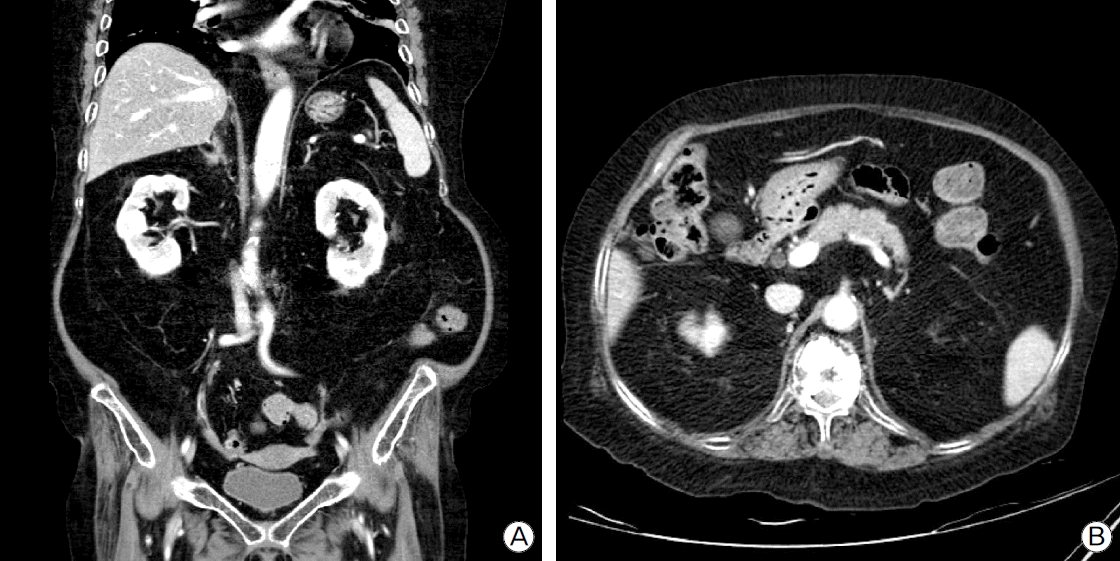
Abdominal computed tomography did not show the right adrenal gland and any abnormal findings (Fig. 1).
Electrocardiography (ECG) showed ST segment elevation in lead III as well as reciprocal changes in leads I and augmented vector left (aVL) (Fig. 2).
Echocardiography showed severe hypokinesia in mid to apical segment of the inferior wall, with preserved LV function (ejection fraction, 55%) (Fig. 3).
Since the above results were compatible with ACS, she was immediately transferred to the catheterization laboratory.
In addition, we also suspected occult AAI associated with ACS. Because, although fluid resuscitation, inotropics and vasopressor, hypotension (initial blood pressure 68/50 mm Hg) sustained in the patient who has received steroid medication.
Thus, we administered intravenous dexamethasone 5 mg immediately before PCI, which does not interfere with rapid adrenocorticotropic hormone (ACTH) test.
Emergent coronary angiography was performed, which showed a midportion fracture and distal portion 99% in-stent restenosis of the zotarolimus-eluting stent (2.75 × 24-mm Endeavor-Resolute; Medtronic Vascular, Santa Rosa, CA, USA), that had been implanted in the posterolateral branch of the right coronary artery 4 years prior, with Thrombolysis in Myocardial Infarction (TIMI) flow grade 2. (Fig. 4) An everolimus-eluting stent (2.5 × 23-mm Xience V; Abbott Vascular, Santa Clara, CA, USA) was deployed at the restenosis and fracture sites. After that, final coronary angiography showed complete reperfusion and TIMI flow grade 3 (Fig. 5).
And to verify the suspected diagnosis of AAI, the rapid ACTH stimulation test was performed after successful PCI. Then, intravenous hydrocortisone sodium succinate (solucortef) 50 mg was replaced every 6 hours.
The standard high dose ACTH (cosynthropin 250 μg/dl) stimulation test results showed in table 1, which suggested adrenal insufficiency. Basal plasma ACTH, rennin and aldosterone were 17.1 pg/ml (normal value, 20–52 pg/ml) 1.53 ng/ml/h (normal value, 1–4 ng/ml/h) and 98.54 pg/ml (normal value, 50–300 pg/ml) that were coupled with simultaneous measurement of basal serum cortisol.
After several hours of steroid injection and successful PCI, hypotension was dramatically reversed. The next morning, her mental status became completely alert, with improvement in nausea, vomiting, and abdominal pain. Her general condition gradually improved and she was discharged from the hospital and followed up with current glucocorticoid replacement therapy.
AAI is a rare but severe condition caused by sudden defective production of adrenal steroids. It is an emergency situation and thus rapid awareness and prompt therapy are critical for survival even before the diagnosis is made.[1,2] The recent study of Hahner et al.[3] reported that AAI occurs in a substantial proportion of patients with chronic adrenal insufficiency (primary and secondary adrenal insufficiency) due to various causes. The most common precipitating factor for AAI is infectious disease, particularly gastrointestinal infections. To date, limited data are available regarding the incidence and precipitating factors for AAI, mainly from single-case reports.
Several previous studies have reported that adrenal insufficiency is associated with ACS. Norasyikin et al.[4] reported that 21.6 % of patients admitted with ACS were diagnosed with adrenal insufficiency by using a low-dose ACTH stimulation test and that no patient was diagnosed with adrenal insufficieny by using the post-standard dose (increments of less than 250 nmol/L) ACTH stimulation test.
Chang et al.[5] demonstrated, in a study on the prevalence of functional adrenal insufficiency in patients with acute myocardial infarction, that there is the relationship between herbal medication use and low cortisol in patients with acute myocardial infarction. They also stated that there were only 2 of the 13 patients (9 with severe sepsis and 4 with acute myocardial infarction and a serum cortisol level of < 15 μg/dl) with true acrenal insufficiency by using the rapid ACTH test.
The pathogenesis of AAI is poorly understood. Numerous studies have suggested that various factors can impair normal corticosteroid responses following AAI occurrence during severe illness.[1,3,6,7]
In our case, the pre-existing condition of AAI was an overlooked secondary adrenal insufficiency due to long-term steroid medication, which made the differential diagnosis of AAI more difficult. In addition, the main precipitating factor for AAI was ACS induced by stent fracture.
Coronary stent fracture is a relatively uncommon complication of stent implantation. The reported incidence of stent fracture in patients with drug-eluting stents, including a zotarolimus-eluting stent, as shown in this case, is reported to be between 1% and 8%.[8,9] This can cause in-stent restenosis, stent thrombosis, recurrent angina, myocardial infarction, and even sudden death.[10] In our case, stent fracture resulted in ACS, thereby precipitating AAI.
AAI may present with various clinical symptoms and can be life-threatening if not successfully treated. In particular, AAI associated with acute illness is more difficult to establish a clinical diagnosis as shown in this case. Early diagnosis and successful treatment of such cases can increase cure rate. Herein, we reported the rare case of a 67-year-old female patient with AAI accompanied by ACS due to stent fracture. Further studies are needed to elucidate the pathogenesis of concurrent AAI and ACS.
References
1). Grossman A, Johannsson G, Quinkler M, Zelissen P. Therapy of endocrine disease: Perspectives on the management of adrenal insufficiency: clinical insights from across Europe. Eur J Endocrinol. 2013; 169:R165–75.

3). Hahner S, Loeffler M, Bleicken B, Drechsler C, Milovanovic D, Fassnacht M, et al. Epidemiology of adrenal crisis in chronic adrenal insufficiency: the need for new prevention strategies. Eur J Endocrinol. 2010; 162:597–602.

4). Norasyikin AW, Norlela S, Rozita M, Masliza M, Shamsul AS, Nor Azmi K. Adrenal insufficiency in acute coronary syndrome. Singapore Med J. 2009; 50:962–6.
5). Chang SS, Liaw SJ, Bullard MJ, Chiu TF, Chen JC, Liao HC. Adrenal insufficiency in critically ill emergency department patients: a Taiwan preliminary study. Acad Emergency Med. 2001; 8:761–4.

6). Cooper MS, Stewart PM. Corticosteroid insufficiency in acutely ill patients. N Engl J Med. 2003; 348:727–34.

7). Quinkler M, Beuschlein F, Hahner S, Meyer G, Schöfl C, Stalla GK. Adrenal cortical insufficiency--a life threatening illness with multiple etiologies. Dtsch Arztebl Int. 2013; 110(51–52):882–8.
8). Canan T, Lee MS. Drug-eluting stent fracture: incidence, contributing factors and clinical implications. Catheter Cardiovasc Interv. 2010; 75:237–45.

9). Wu MC, Cheng CC, Huang TY. Fracture of zotarolimuseluting stent after implantation. Texas Heart Inst J. 2009; 36:618–20.
10). Alexopoulos D, Xanthopoulou I. Coronary stent fracture: how frequent it is? Does it matter? Hellenic J Cardiol. 2011; 52:1–5.
Fig. 2.
Electrocardiography showed ST segment elevation in lead III as well as reciprocal changes in leads I and augmented vector left (aVL).
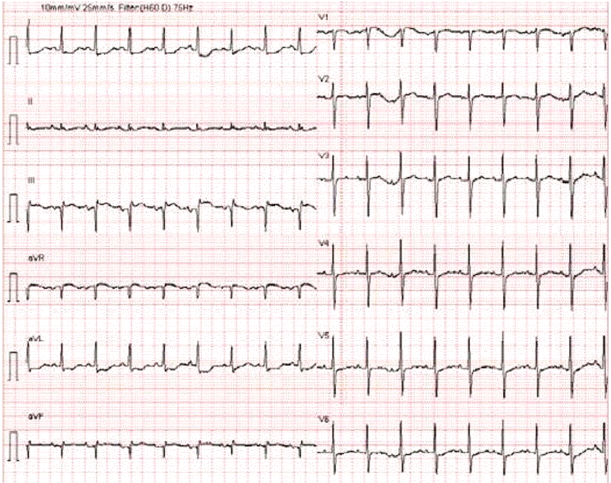
Fig. 3.
Echocardiography short axis views of systole and diastole status at mid and apical level. That showed severe hypokinesia in mid to apical segment of the inferior wall, with preserved Left ventricle function (ejection fraction, 55%).

Fig. 4.
Initial coronary angiography showing mid portion fracture and distal portion 99% in-stent restenosis of a drug-eluting stent (2.75 × 24-mm Endeavor-esolute) in the postero-lateral branch of the right coronary artery with Thrombolysis in Myocardial Infarction flow grade 2.





 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download