This article has been
cited by other articles in ScienceCentral.
Abstract
Obstructive fibrinous tracheal pseudomembrane (OFTP) is a rare condition usually associated with endotracheal intubation. Airway obstruction caused by OFTP may occur after endotracheal tube extubation and can lead to severe respiratory distress. It is a rare but potentially fatal complication. In this report, we present a case of OFTP presented with atelectasis that caused dyspnea after extubation and was successfully treated by mechanical removal using a rigid bronchoscope.
Go to :

Keywords: airway obstruction, bronchoscopy, intubation, pulmonary atelectasis
Obstructive fibrinous tracheal pseudomembrane (OFTP) is a poorly known complication associated with endotracheal intubation. Little is known about the exact mechanism, but superficial damage of the trachea at the site of the endotracheal cuff is thought to trigger OFTP.[
1,
2] OFPT usually presents as a thick tubular, rubber-like, whitish pseudomembrane molding the tracheal wall under bronchoscopy. Immediate mechanical removal is regarded as the definitive therapy. Herein, we report a case of OFTP presented with atelectasis that developed after short-duration endotracheal intubation.
CASE REPORT
A 21-year-old woman was referred to our Emergency Department for the removal of a tracheal lesion by rigid bronchoscopy. According to the medical records from another hospital, she had been diagnosed with end-stage renal disease (ESRD) caused by vesico-ureteral reflux and had been treated with maintenance hemodialysis (HD). Two days earlier, she was admitted to the hospital owing to acute pulmonary edema caused by excessive water intake. In the Emergency Department, she developed respiratory failure requiring endotracheal intubation and emergency HD. She was transferred to the intensive care unit. The physicians there reported use of a low-pressure and high-volume endotracheal tube for intubation with no complications. The physicians reported that endotracheal cuff pressure was checked routinely and adjusted to 20–25 cmH
2O. After 38 hours of lung protective pressure support mechanical ventilation, the patient’s pulmonary edema had resolved, and she was successfully weaned from mechanical ventilation. She completed an 1 hour spontaneous breathing trial without incident. After extubation, she complained of mild dyspnea without stridor or whezzing. Chest radiography showed newly developed atelectasis in the right lower lobe (
Fig. 1). Flexible bronchoscopy was performed for tracheobronchial hygiene and revealed a whitish rubbery membrane encircling the upper trachea (
Fig. 2). There was no definite endobronchial lesion in the right lower lobal bronchus except some mucoid impaction. The tracheal lesion was so firmly attached to the trachea that it could not be removed using flexible forceps. There was no evidence of aggravation of respiratory symptom after the bronchoscopic procedure. After transfer to our hospital, emergency rigid bronchoscopy was performed under general anesthesia, and the pseudomembrane was removed using the distal tip of a rigid bronchoscope and mechanical forceps (
Fig. 3). After the procedure, no findings suggestive of tracheomalacia or granulation tissue formation in the tracheal wall were detected (
Fig. 4). The biopsy specimen showed fibrinoid material with acute inflammatory cells (
Fig. 5). After 5 days, follow-up flexible bronchoscopy showed no residual lesion.
 | Fig. 1.Chest radiograph showing newly developed atelectasis in the right lower lobe. 
|
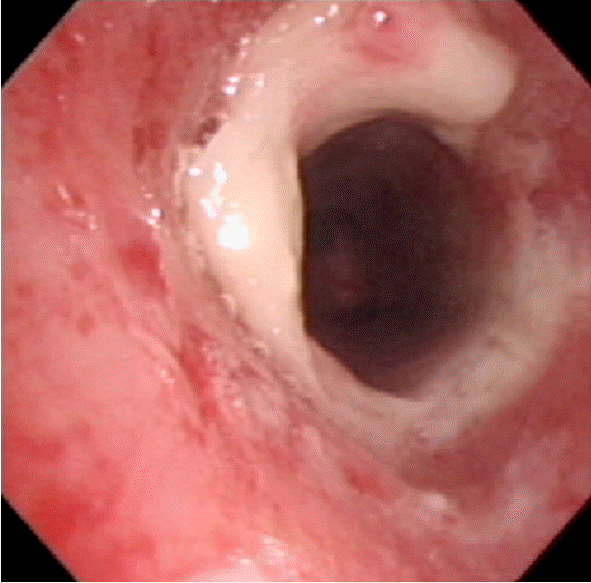 | Fig. 2.Bronchoscopic image showing a thick tubular rubber-like whitish pseudomembrane molding the trachea. 
|
 | Fig. 3.Gross findings for the pseudomembrane removed by bronchoscopy. 
|
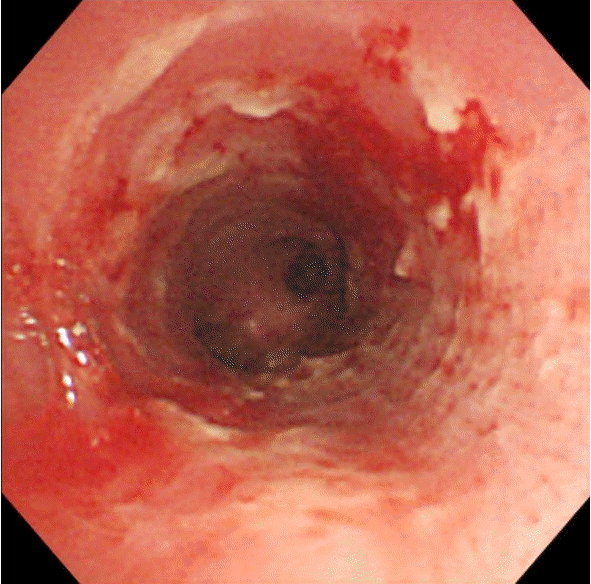 | Fig. 4.Rigid bronchoscopic image showing no findings suggestive of tracheomalacia or granulation tissue formation in the tracheal wall. 
|
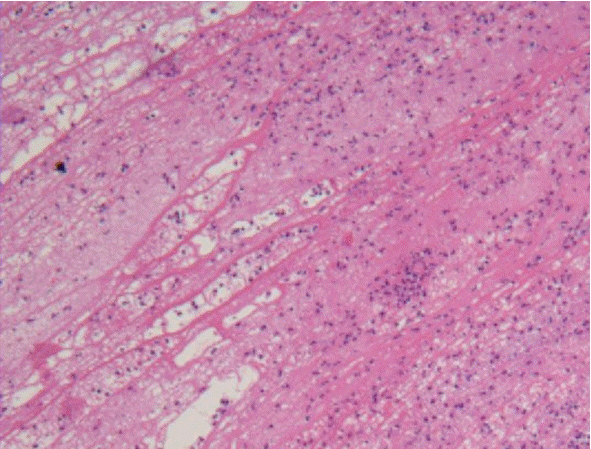 | Fig. 5.Microscopic examination showing that the pseudomembrane consists of fibrinous material with polymorphonuclear cell infiltration (H&E stain ×100). 
|
Go to :

DISCUSSION
OFTP is a rare and poorly known tracheal complication that can be associated with tracheal intubation. It develops after endotracheal intubation of short duration. Shortly after extubation, partial detachment of the pseudomembrane can induce stridor or acute respiratory failure due to valve-manner tracheal obstruction.[
1] Emergent removal by rigid bronchoscopy or reintubation is regarded as the standard first-line treatment.[
1–
3]
The condition has not been characterized, and the risk factors for this complication remain largely unknown, resulting in few reports of OFTP. The term OFTP was proposed by Deslee et al. [
1] in 2000. Since then, only about 30 cases have been reported worldwide.[
2–
9] The condition presents clinically as stridor or respiratory insufficiency after extubation. It is certainly difficult to differentiate OFTP from other conditions because laryngeal spasm, edema, and the retention of secretions also present with stridor or respiratory insufficiency.[
2] Only two of these cases were asymptomatic, and the diagnosis was a fortuitous finding of flexible bronchoscopy performed for atelectasis.[
1] In our case, although the patient complained of mild dyspnea, atelectasis was the reason for bronchoscopy. OFTP was a fortuitous finding in our case. It is generally accepted that OFTP is caused by superficial injury. Pathological analysis has shown that the pseudomembrane consists of fibrinous material admixed with neutrophilic granulocytes and necrotic epithelial cells with no evidence of subepithelial involvement.[
1,
2] It is difficult to reveal risk factors that increase the risk of developing OFTP owing to the rarity of reported cases. Although increased cuff pressure, cardiopulmonary resuscitation, and the aspiration of gastric contents are common in OFTP cases, all these findings also occur in many intubated patients. In this case, the patient presented comorbid ESRD. To our knowledge, this is the first case of OFTP in a patient with ESRD maintained on HD. However, the direct relationship between OFTP and ESRD is unclear. The prognosis of OFTP is quite good after mechanical ablation by rigid bronchoscopy. It is known that OFTP never recurs, in contrast with post-intubation tracheal stenosis, suggesting that the condition is a superficial injury.[
1]
Rigid bronchoscopy is accepted as a standard therapy. Although 4 cases were treated with flexible bronchoscopy, the use of a rigid bronchoscope allows for rapid detachment of the pseudomembrane from the trachea while safely maintaining a patent airway.[
1,
2,
9] Partial detachment of the proximal pseudomembrane during this procedure can induce life-threatening acute respiratory failure due to valve-manner tracheal obstruction.[
1]
In summary, we described a rare case of OFPT presented with atelectasis in a patient with ESRD maintained on HD. OFTP is a rare tracheal complication associated with intubation but should be considered in every dyspneic patient shortly after extubation. The risk factors of OFTP remain unclear, but endotracheal injury prevention during intubation period may be an effort to prevent or reduce the risk of developing OFTP. Physicians must be aware of this potentially fatal complication related to intubation, and flexible bronchoscopy should be performed for an accurate diagnosis. The first-line therapy should be mechanical ablation using a rigid bronchoscope.
Go to :


