Introduction
Clinical trials (CTs) are a crucial part of new drug development. For a new drug to be approved and marketed, the safety and efficacy has to be confirmed by different phases of CTs, which usually involve a large number of patients. Therefore, interest, proper understanding and voluntary consent to participate in CTs are very important to ensure timely and unbiased, successful operation of CTs.
As the molecular understanding of diseases has expanded with improvements in engineering technology, the number of new drugs has also increased at an unprecedented rate, especially in cancer-related fields [
1]. Indeed, as of January 2016, the number of CTs registered at ClinicalTrials.gov was 207,521, representing a 17-fold increase since 2005 [
2]. However, not all drugs are successfully introduced to the market, and results of only 10% of the trials registered to ClinicalTrials.gov were posted. The low accrual rate is reportedly an important limitation of successful CTs, and several reports on factors influencing the accrual rate have been published [
3-
5].
In 2008, we collected questionnaires and analyzed cancer patient’s awareness of CTs and their willingness to participate [
6]. In that study, 82.6% of patients were familiar with CT, but only 64.7% were willing to participate. The patients’ awareness, perceptions regarding the benefits, and willingness to participate in CTs were influenced by multiple factors including their own health conditions, as well as social and cultural backgrounds. In the last eight years, there have been many changes in Korean society and the medical care environment. Since 2008, South Korea’s GDP has increased by roughly 25%, and Korean citizens’ spending on medical care has increased by over 50% [
7]. Additionally, people are becoming more interested in leading a healthier life, and as medical knowledge and awareness of CT increases, it is expected that patient views toward CTs will change. Moreover, the number of new drugs and CTs available to Korean patients has increased remarkably. Specifically, the number of CTs in Korea, registered to and approved by the Korean Food and Drug Administration increased by almost two-fold between 2007 and 2013, with investigator-initiated trials increasing almost 640% [
8].
In this context, we surveyed cancer patients to assess their current levels of awareness regarding CTs, as well as their perceived benefit and willingness to participate in CTs.
Go to :

Results
1. Patient characteristics of responders for the questionnaire
A total of 520 cancer patients receiving chemotherapy were asked to participate in this study. Among the 520 patients, 397 responded to the questionnaire (76.3%). The patient characteristics of the 397 patients are summarized in
Table 1. Among the evaluable patients, 62.5% were female, and the median age was 52 years (range, 20 to 81 years). Most patients were married (80.9%) and lived within 2 hours’ distance (69.3%) from the hospital. In terms of education, 48.1% of the included patients received equal to or higher than college education. Additionally, 55.4% answered that they were covered by additional private cancer insurance. Thirty-two patients (8.4%) answered the questions regarding awareness and willingness to participate in CTs but did not complete their demographic information.
Table 1.
|
Characteristic |
No. of patients (%) (n=397) |
|
Age, median (range, yr)
|
52 (20-81) |
|
Sex
|
|
|
Male |
117 (29.5) |
|
Female |
248 (62.5) |
|
Unknown |
32 (8.4) |
|
Disease status
|
|
|
Neoadjuvant |
52 (13.1) |
|
Adjuvant |
90 (22.7) |
|
Metastatic, first line |
80 (20.2) |
|
Metastatic, second line |
59 (14.9) |
|
Metastatic, third line |
36 (9.1) |
|
Metastatic, ≥ fourth line |
24 (6.1) |
|
Othera)/Unknown |
16 (4.2) |
|
Diagnosis
|
|
|
Breast |
173 (43.6) |
|
Stomach |
42 (10.6) |
|
Lung |
40 (10.1) |
|
Colorectal |
34 (8.6) |
|
Hepatobiliary/Pancreas |
21 (5.3) |
|
Head and neck/Esophagus |
13 (3.3) |
|
Lymphoma |
8 (2.0) |
|
Other |
26 (6.5) |
|
Multiple primary |
8 (2.0) |
|
Unknown |
32 (8.1) |
|
Previous history of clinical trial enrollment
|
|
|
Yes |
78 (19.6) |
|
No |
287 (72.3) |
|
Unknown |
32 (8.1) |
|
Marital status
|
|
|
Single |
22 (5.5) |
|
Married |
321 (80.9) |
|
Bereaved |
16 (4.0) |
|
Divorced |
21 (5.3) |
|
Unknown |
17 (4.3) |
|
Educational degree
|
|
|
College and higher |
191 (48.1) |
|
High school |
135 (34.0) |
|
Middle school |
35 (8.8) |
|
Elementary school |
20 (5.0) |
|
Unknown |
16 (4.0) |
|
Economic statusb)
|
|
|
> 8 |
32 (8.1) |
|
> 6 to ≤ 8 |
40 (10.1) |
|
> 4 to ≤ 6 |
77 (19.4) |
|
> 2 to ≤ 4 |
110 (27.7) |
|
≤ 2 |
103 (25.9) |
|
Unknown |
35 (8.8) |
|
Religion
|
|
|
Christian |
119 (30.0) |
|
Catholic |
65 (16.4) |
|
Buddhist |
78 (19.6) |
|
Atheist/Other |
116 (29.2) |
|
Unknown |
19 (4.8) |
|
Distance from clinic
|
|
|
≤ 2 hr |
275 (69.3) |
|
> 2 hr |
107 (27.0) |
|
Unknown |
15 (3.8) |
|
Possession of private cancer insurance
|
|
|
Yes |
220 (55.4) |
|
No |
152 (38.3) |
|
Unknown |
25 (6.3) |

Breast cancer was the most common cancer type (43.6%), followed by gastric cancer (10.6%) and lung cancer (10.1%). At the time of the survey, 199 patients (52.5%) were receiving chemotherapy for recurred or metastatic cancer, while 35.8% were receiving chemotherapy for neoadjuvant/adjuvant purposes. One hundred and fifty-seven (39.5%) answered that they have been recommended to participate in any CTs by their physicians during their treatment course. At the time of the survey, 78 patients (19.6%) had already experienced CT.
In terms of the basal knowledge and interest regarding general medical information, 55 responders (13.9%) answered that they were “extremely interested,” 34 (8.6%) answered “very interested.” One hundred seventy (42.8%) answered “fairly interested,” whereas 77 (19.4%) answered “not much interested,” 39 (9.8%) answe-red “minimum interest only,” and four (1.0%) answered “none at all.” The routes in which the patients received medical information were mass media (49.2%), the internet (33.3%), physicians or nurses (21.0%), or friends and family (12.3%).
2. Cancer patients’ awareness of CTs
When patients were asked about their awareness of CTs, 97.4% of the patients (387/397) answered that they had heard of CT before (scale ≥ 2). Of those, 20 patients (5.2%) answered that they could explain in full detail what CTs are (scale 6), 72 (18.6%) answered they could explain CTs in rough detail (scale 5), and 134 patients (34.6%) answered they understand what it is but cannot explain it to others (scale 4). Additionally, 70 (18.1%) answered that they have only a rough idea (scale 3), while 81 patients (20.9%) answered that they had heard of CT but do not know in detail (scale 2). Regarding the source of information of CTs, 37.5% of the patients (149/397) answered that they had gathered information from their physicians/nurses, and 34.3% (136/397) answered mass media including TV, newspapers and internet (multiple answers allowed).
Female gender (p=0.032), higher economic status (p=0.021), higher educational degree (p < 0.001), and prior history of CT enrollment (p=0.013) were positively associated with increasing level of awareness of CT. Moreover, the mean point scores of the awareness in patients whose answer to the source of information included physicians/nurses were significantly higher than the scores of those who did not receive the information from their physicians/nurses (6.3 [SD, 2.27] vs. 5.1 [SD, 2.12], p < 0.001). Patients who could answer the question regarding the stage of their disease, whether correctly or not, also answered more confidently about the awareness of CTs than those who did not or could not answer the question (p=0.002). The awareness of CTs was in modest positive correlation with interest in general health information (Spearman’s r=0.374, p < 0.001). Possession of private insurance, age, marital status, and travel distance to the hospital were not associated with the awareness of CTs. Moreover, whether the patient was receiving chemotherapy for curative or palliative aim, or the number of regimens the patient had received before survey were not associated with level of awareness.
3. Perception of the benefits and risks of CTs
In the survey of the perception of CTs using VAS scale, patients gave a mean value of 6.43 (SD, 2.01) for the benefit and 4.42 (SD, 1.94) for the risk of CTs. The perceived benefits and risks of CTs in association with other patient characteristics are given in
Table 2. The patients who have already participated in any CTs before the survey had higher expectations of benefit (6.86 [SD, 2.03] vs. 6.38 [SD, 2.08], p=0.039), and safer perception of the CTs (3.99 [SD, 2.2] vs. 4.82 [SD, 1.86], p=0.001).
Table 2.
Perceptions regarding benefits/risks of clinical trials by patient characteristics
|
Benefit |
p-value |
Risk |
p-value |
|
Age group (yr)
|
|
|
|
|
|
≤ 30 |
6.60±2.01 |
0.239 |
5.30±0.82 |
0.222 |
|
> 30 to ≤ 40 |
6.87±1.78 |
|
4.92±1.83 |
|
|
> 40 to ≤ 50 |
6.42±1.72 |
|
4.71±1.84 |
|
|
> 50 to ≤ 60 |
6.77±2.16 |
|
4.22±2.05 |
|
|
> 60 to ≤ 70 |
6.07±2.46 |
|
4.77±2.02 |
|
|
> 70 |
6.10±1.94 |
|
4.90±2.20 |
|
|
Unknown |
5.71±1.80 |
|
5.00±1.74 |
|
|
Sex
|
|
|
|
|
|
Male |
6.41±1.98 |
0.196 |
4.78±1.71 |
0.253 |
|
Female |
6.53±2.12 |
|
4.54±2.06 |
|
|
Unknown |
5.79±1.82 |
|
5.10±1.80 |
|
|
Disease status
|
|
|
|
|
|
Neoadjuvant |
6.78±1.93 |
0.373 |
4.36±2.14 |
0.533 |
|
Adjuvant |
6.61±2.11 |
|
4.36±1.90 |
|
|
Metastatic, first line |
6.51±2.16 |
|
4.72±2.01 |
|
|
Metastatic, second line |
6.42±2.04 |
|
4.73±2.02 |
|
|
Metastatic, third line |
5.64±2.36 |
|
4.90±2.01 |
|
|
Metastatic, ≥ fourth line |
6.17±2.06 |
|
4.96±1.43 |
|
|
Othera)/Unknown |
6.36±1.81 |
|
4.96±1.83 |
|
|
Diagnosis
|
|
|
|
|
|
Breast |
6.70±2.01 |
0.012 |
4.38±2.09 |
0.251 |
|
Stomach |
6.65±2.00 |
|
4.49±1.85 |
|
|
Lung |
5.82±1.74 |
|
5.03±1.71 |
|
|
Colorectal |
6.10±2.51 |
|
4.47±1.91 |
|
|
Hepatobiliary/Pancreas |
5.47±2.65 |
|
5.05±2.01 |
|
|
Head and neck/Esophagus |
6.83±1.59 |
|
5.58±1.38 |
|
|
Lymphoma |
8.00±1.16 |
|
5.29±2.75 |
|
|
Other |
6.09±2.02 |
|
4.96±1.58 |
|
|
Multiple primary |
7.50±1.41 |
|
5.25±1.17 |
|
|
Unknown |
5.76±1.79 |
|
5.00±1.71 |
|
|
Previous history of clinical trial enrollment
|
|
|
|
|
|
Yes |
6.86±2.03 |
0.039 |
3.99±2.16 |
0.003 |
|
No |
6.38±2.08 |
|
4.82±1.86 |
|
|
Unknown |
5.76±1.79 |
|
5.00±1.71 |
|
|
Marital status
|
|
|
|
|
|
Single |
6.52±2.09 |
0.828 |
4.72±1.90 |
0.555 |
|
Married |
6.46±2.04 |
|
4.76±1.84 |
|
|
Bereaved |
5.79±2.55 |
|
4.43±2.34 |
|
|
Divorced |
6.50±1.79 |
|
4.13±2.22 |
|
|
Unknown |
6.33±2.54 |
|
4.00±2.28 |
|
|
Educational degree
|
|
|
|
|
|
College or higher |
6.61±1.78 |
0.079 |
4.78±1.85 |
0.477 |
|
High school |
6.50±2.12 |
|
4.51±2.05 |
|
|
Middle school |
5.64±2.63 |
|
4.37±1.84 |
|
|
Elementary |
5.93±2.76 |
|
5.19±2.07 |
|
|
Unknown |
5.55±2.51 |
|
4.30±2.16 |
|
|
Economic statusb)
|
|
|
|
|
|
> 8 |
7.19±1.74 |
0.079 |
5.13±2.40 |
0.681 |
|
> 6 to ≤ 8 |
6.25±1.66 |
|
4.81±1.66 |
|
|
> 4 to ≤ 6 |
6.72±1.90 |
|
4.54±1.85 |
|
|
> 2 to ≤ 4 |
6.43±1.92 |
|
4.71±1.86 |
|
|
≤ 2 |
5.99±2.33 |
|
4.57±2.04 |
|
|
Unknown |
6.70±2.58 |
|
4.35±1.90 |
|
|
Religion
|
|
|
|
|
|
Christian |
6.53±2.12 |
0.458 |
4.56±1.91 |
0.193 |
|
Catholic |
6.14±2.28 |
|
5.21±1.83 |
|
|
Buddhist |
6.75±1.87 |
|
4.59±2.18 |
|
|
Atheist/Others |
6.32±1.92 |
|
4.56±1.79 |
|
|
Unknown |
6.09±2.55 |
|
4.10±2.38 |
|
|
Distance from clinic
|
|
|
|
|
|
≤ 2 hr |
6.42±1.99 |
0.557 |
4.66±1.99 |
0.939 |
|
> 2 hr |
6.53±2.19 |
|
4.68±1.78 |
|
|
Unknown |
5.80±2.49 |
|
4.44±2.24 |
|
|
Private cancer insurance
|
|
|
|
|
|
Yes |
4.46±1.99 |
0.076 |
6.65±2.00 |
0.023 |
|
No |
5.01±1.82 |
|
6.18±2.07 |
|
|
Unknown |
4.24±1.89 |
|
5.94±2.39 |
|

The mean scores describing the benefits and risks of conventional therapy were 6.52 (SD, 1.92) and 4.42 (SD, 2.12), respectively, with no significant difference in perception of benefit or risk between CT and conventional therapy (p=0.315 and p=0.052, respectively).
When the perceived benefits and risks were analyzed in relation to the level of awareness of CTs, patients who were only familiar with the term without any knowledge of contents had the least expectation of benefit from CTs (p=0.015). While patients with higher confidence in their awareness of CTs showed higher expectation of benefits, the patients who were not aware of CTs at all answered the highest scores for the benefit. However, no significant difference between the groups in the level of perceived risk was observed (p=0.167). The average VAS scores of perception of benefits and risks according to awareness are given in
Table 3.
Table 3.
Perceived benefits and risks of clinical trials in association with levels of awareness of clinical trials
|
Benefit |
p-value |
Risk |
p-value |
|
Never heard of |
7.56±2.01 |
0.015 |
4.67±2.18 |
0.167 |
|
Heard of the term, but do not know content |
6.05±2.45 |
|
4.62±2.03 |
|
|
Rough idea only |
6.08±1.81 |
|
5.08±1.84 |
|
|
Understand, but cannot explain |
6.29±2.00 |
|
4.60±1.74 |
|
|
Can explain in rough detail |
7.03±1.94 |
|
4.61±2.02 |
|
|
Can explain in full detail |
7.00±2.00 |
|
3.68±2.65 |
|

4. Willingness to participate in CTs
Among the 397 patients, 225 (56.7%) answered that they would participate in the CTs. The most common reason for willingness to participate was “the opportunity to receive the most up-to-date treatment” (59.6%), followed by “physician recommendation” (25.8%), and “financial benefits of treatment” (11.1%). On the other hand, among patients who were unwilling to participate in CTs, the most common reason was “because the effects of CTs are not proven yet” (44.1%), followed by “fear of side-effects” (32.1%), and “I don’t want to be a guinea pig” (15.8%). Heavily treated patients showed more willingness to participate in CTs (p < 0.001). The patients who have experienced CTs before the survey also showed a higher willingness to participate (p < 0.001). Overall, patients who did not complete the questions showed lower willingness to participate. The percentages of patients’ willingness to participate in CTs in association with other patient characteristics are given in
Table 4.
Table 4.
Willingness of patients to participate in cancer clinical trials
|
Willingness to participation (%) |
p-value |
|
Age group (yr)
|
|
|
|
≤ 30 |
3/10 (30.0) |
0.471 |
|
> 30 to ≤ 40 |
21/40 (52.5) |
|
|
> 40 to ≤ 50 |
55/96 (57.3) |
|
|
> 50 to ≤ 60 |
67/116 (57.8) |
|
|
> 60 to ≤ 70 |
46/80 (57.5) |
|
|
> 70 |
15/24 (62.5) |
|
|
Unknown |
18/31 (58.1) |
|
|
Sex
|
|
|
|
Male |
60/117 (51.3) |
0.638 |
|
Female |
146/248 (58.9) |
|
|
Unknown |
19/32 (59.4) |
|
|
Disease status
|
|
|
|
Neoadjuvant |
19/52 (36.5) |
< 0.001 |
|
Adjuvant |
36/88 (40.9) |
|
|
Metastatic, first line |
53/80 (66.2) |
|
|
Metastatic, second line |
37/59 (62.7) |
|
|
Metastatic, third line |
28/36 (77.8) |
|
|
Metastatic, ≥ fourth line |
25/28 (89.3) |
|
|
Othera)/Unknown |
26/51 (51.0) |
|
|
Diagnosis
|
|
|
|
Breast |
97/173 (56.1) |
0.368 |
|
Stomach |
29/42 (69.0) |
|
|
Lung |
23/40 (57.5) |
|
|
Colorectal |
19/34 (55.9) |
|
|
Hepatobiliary/Pancreas |
14/21 (66.7) |
|
|
Head and neck/Esophagus |
4/13 (30.8) |
|
|
Lymphoma |
4/8 (50.0) |
|
|
Other |
12/26 (46.2) |
|
|
Multiple primary |
5/8 (62.5) |
|
|
Unknown |
18/32 (56.2) |
|
|
Previous history of clinical trial enrollment
|
|
|
|
Yes |
69/78 (88.5) |
< 0.001 |
|
No |
138/287 (48.1) |
|
|
Unknown |
18/32 (56.2) |
|
|
Marital status
|
|
|
|
Single |
11/22 (50.0) |
< 0.001 |
|
Married |
184/321 (57.3) |
|
|
Bereaved |
13/16 (81.2) |
|
|
Divorced |
13/21 (61.9) |
|
|
Unknown |
4/17 (23.5) |
|
|
Educational degree
|
|
|
|
College or higher |
111/191 (58.1) |
< 0.001 |
|
High school |
83/135 (61.5) |
|
|
Middle school |
19/35 (54.3) |
|
|
Elementary school |
7/20 (35.0) |
|
|
Unknown |
5/16 (31.2) |
|
|
Economic statusb)
|
|
|
|
> 8 |
17/32 (53.1) |
< 0.001 |
|
> 6 to ≤ 8 |
20/40 (50.0) |
|
|
> 4 to ≤ 6 |
40/77 (51.9) |
|
|
> 2 to ≤ 4 |
65/110 (59.1) |
|
|
≤ 2 |
66/103 (64.1) |
|
|
Unknown |
17/35 (48.6) |
|
|
Religion
|
|
|
|
Christian |
74/119 (62.2) |
< 0.001 |
|
Catholic |
36/65 (55.4) |
|
|
Buddhist |
46/78 (59.0) |
|
|
Atheist/Other |
63/116 (54.3) |
|
|
Unknown |
6/19 (31.6) |
|
|
Distance from clinic
|
|
|
|
≤ 2 hr |
161/275 (58.5) |
< 0.001 |
|
> 2 hr |
60/107 (56.1) |
|
|
Unknown |
4/15 (26.7) |
|
|
Private cancer insurance
|
|
|
|
Yes |
122/220 (55.5) |
< 0.001 |
|
No |
95/152 (62.5) |
|
|
Unknown |
8/25 (32.0) |
|

Patients with higher levels of awareness of CTs were more willing to participate (p < 0.001). The average VAS points of perception of the benefits of CTs were higher in the group willing to participate in CTs (6.65 [SD, 2.05] vs. 6.14 [SD, 2.04], p=0.026). The percentage of patients showing willingness to participate and their perception of the benefits and risks of CTs, in association with the level of awareness of CTs, are shown in
Fig. 1. There were no significant differences between the willing and the unwilling group in perceived risks of CTs, or in perceived benefits or risks of conventional therapy.
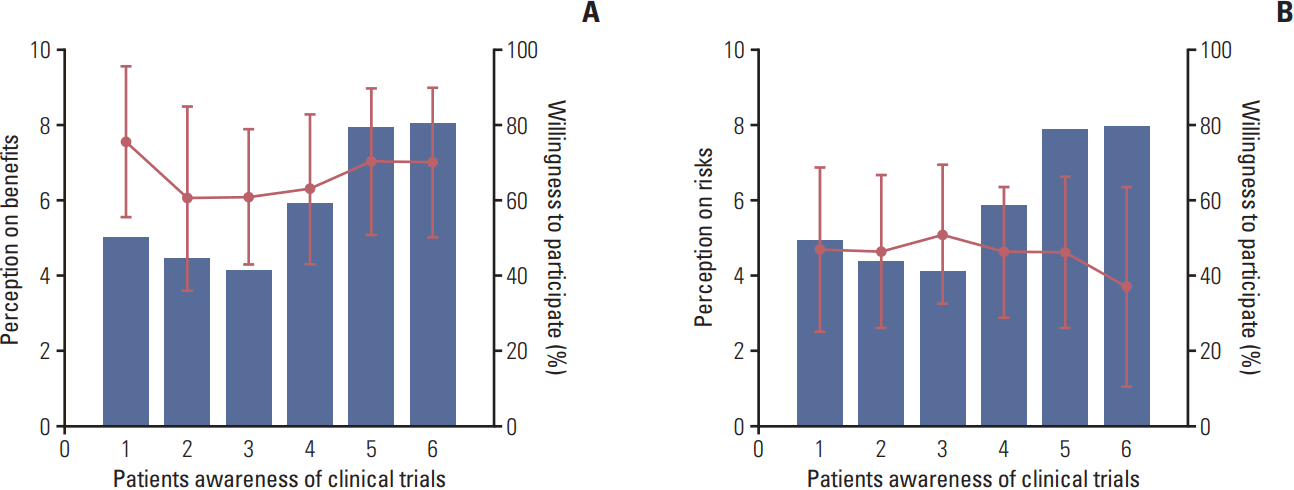 | Fig. 1.Cancer patients’ willingness to participate in clinical trials relative to level of awareness and perceived benefits/risks of clinical trials. (A) Cancer patients’ awareness of clinical trials and willingness to participate relative to perceived benefits (red line: perceived benefit; blue blocks: willingness to participate). (B) Cancer patients’ awareness of clinical trials and willingness to participate relative to perceived risks (red line: perceived risk; blue blocks: willingness to participate). (A, B) Patients’ awareness of clinical trials: 1, never heard of; 2, heard of clinical trial but do not know in detail; 3, rough idea of only; 4, understand, but cannot explain; 5, can roughly explain; 6, know in full detail. 
|
5. Actual participation of the patients in CTs
During the period, an average of 109 studies were available for enrollment at Seoul National University Hospital. We followed up the 222 of the patients who participated in this survey earlier during the collection period, and had more than one year of follow-up time after completion of the survey. Out of the 222 patients, 30 (13.5%) were actually enrolled in trials after the survey. Additionally, 23 of the 30 patients (76.7%) were those who showed willingness to participate in CTs, while the other seven either answered no or gave no answer.
Go to :

Discussion
In our study, we surveyed cancer patients receiving chemotherapy to assess the current levels of awareness of CTs and perceptions regarding the benefits/risks of CTs and finally to assess the willingness of the patients to participate in cancer CTs. While 97.4% of the surveyed patients answered that they were at least not unfamiliar with CTs, only 5.2% answered that they were confident with their knowledge. Interestingly, the patients with vague knowledge of CTs had the most doubt about the benefit of the CTs. Overall, 59.4% of the patients answered positively to the question asking if they were willing to participate in CTs when offered. Additionally, patients with higher confidence of awareness of CTs showed higher willingness to participate.
A low accrual rate has often been identified as an important barrier against successful conduction of CTs [
9-
12]. It has been reported that only approximately 3%-5% of adult cancer patients enroll in CTs [
13]. Understanding and overcoming the patient factor is important to overcoming this barrier. The patients’ awareness and understanding of CTs, which are the important factors with potential improvability, have been a subject of interest, and a few studies have been conducted among different populations [
14-
17]. A number of previous studies have reported positive correlation of patient awareness with the willingness to participate, although some inconsistency still remains. Lara et al. [
18] conducted a survey of the residents of California and reported that there was a positive correlation between the respondent awareness of cancer CTs and the willingness to participate. On the other hand, there was a Korean study in 2012 that reported discrepancies between the awareness and the willingness to participate [
19]. A summary and recommendations from the National Cancer Institute-American Society of Clinical Oncology Cancer Trial Accrual Symposium suggested that, with existing literature evidence, raising general awareness about CTs alone may not be sufficient to improve accrual; however, the report went on to recommend education of patients and the community about CTs using culturally appropriate materials that considered the patients’ point of view [
20].
We reported a considerably high percentage of patients having at least heard of CTs (97.4%). The high proportion being at least familiar with CTs may be related to the fact that the respondents in our patients were all cancer patients receiving chemotherapy. Lara et al. [
18] reported that 69% of the respondents answered that they had heard the term “clinical trial” before; however, their survey had included not only cancer patients, but also their friends and family, and even a small proportion of general public. However, the percentage of patients having at least heard of CTs in this study is still higher than the result reported in our study in 2008, which was 82.6% [
6]. The general increase in awareness may be at least in part explained by the actual increase in the number of CTs available to cancer patients [
8]. With improvements in cancer research and new drug development, the number of CTs available has recently expanded rapidly. Indeed, the average number of cancer CTs available for enrollment on any given day at our institution, which is one of the largest university hospitals with a cancer center in Korea, has increased from 47 in 2008 to 110 in 2015.
The results of this study revealed a positive correlation between the patient’s awareness and their willingness to participate. These results are in accordance with several previously reported western studies [
18]. However, the willingness to participate observed in our report was not much higher than that observed in other reports considering the high percentage of awareness of CTs in our cohort, although consent rates reported in previous studies varied widely [
3]. Furthermore, no definite improvement in willingness was observed from our previous study in 2008.
Interestingly, we found that the expectation of benefit from CTs of patients with only a rough idea of CTs was even lower than that of patients without any knowledge of CTs at all. Additionally, although the percentage of patients showing willingness to participate in CTs gradually increased in line with the level of awareness, reaching more than 80% among patients with a relatively higher understanding of CTs, the percentage of patients with a lower level of understanding that were willing to participate was still not very different from that of patients with no knowledge of CTs at all. A possible explanation for this may be that an accurate or confident level of understanding, rather than any level of awareness of CTs, is important to improving the positive perception and willingness to participate. In our study, patients who answered that they have gathered most of the information from their doctors/nurses answered the question regarding the level of awareness of CTs with higher confidence. These results suggest that active patient education, especially by their physicians and nurses, to provide patients with unbiased accurate information and help them properly understand CTs is important. Proper education may eventually lead to improvement in the accrual rate in future CTs.
This study has limitations in that it was conducted at a single center, and focusing only on cancer patients receiving chemotherapy. Moreover, we were not able to include all of the target patients during the study period, which may have led to bias in the study population. Moreover, it is possible that patients with negative attitudes towards any research, including CTs, may have not agreed to participate in this survey. Even among those who agreed to participate in the survey, patients who skipped any of the questions showed less willingness to participate in CTs. This implies a possibility that the results may be skewed from the actual reality towards positive attitudes. As these caveats are one of limitations of collecting questionnaires from large populations, we chose to include and reveal the patients who skipped any of the questions; however, this necessitates that caution be taken when interpreting the results. Despite the limitations, our center is one of the largest cancer centers in Korea, and one of the centers conducting the highest number of cancer CTs. Therefore, the results of this study were based on an important group of cancer patients treated in Korea.
Overall, this research shows the significance and importance of supplying patients with accurate and detailed information regarding the CTs to increase their willingness to participate. As the numbers of novel drugs increase, it will be important to understand the mindset of patients in order to perform CTs. The results presented herein will help predict patients’ future attitudes toward CTs in Eastern countries.
Go to :






 PDF
PDF Citation
Citation Print
Print


 XML Download
XML Download