INTRODUCTION
Secondary (AA) amyloidosis is a systemic disease caused by the deposition of amyloid in various tissues and organs leading to impaired function.
1 It occurs most frequently in patients with poorly controlled chronic inflammatory disease, mainly rheumatoid arthritis, and ankylosing spondylitis.
2 In systemic amyloidosis, the usual presentation is renal involvement, and the gastrointestinal tract is commonly involved.
3 Patients with gastric involvement present with various symptoms such as nausea, vomiting, hematemesis, and epigastric pain.
4 Most studies emphasize the presence of stomach motility disturbances in amyloidosis.
5 However, there have been few case reports of systemic amyloidosis with gastric outlet obstruction. Here, we report a case of systemic AA amyloidosis with gastric outlet obstruction mimicking linitis plastica secondary to ankylosing spondylitis.
Go to :

CASE REPORT
A 65-year-old woman was referred to us because of abdominal distention, nausea, and vomiting that had been occurring for a month. Her medical history includes a diagnosis of ankylosing spondylitis 1 year ago, and she had been taking celecoxib daily. Physical examination revealed decreased bowel sounds and direct tenderness in the lower abdomen. Complete blood cell count showed a leukocyte number of 7,470/µL, hemoglobin of 8.8 g/dL, and platelet count of 301,000/mm
3. Her blood chemistry values were as follows: total protein, 6.1 g/dL; albumin, 3.1 g/dL; total bilirubin, 0.4 mg/dL; aspartate aminotransferase, 26 U/L; alanine aminotransferase, 16 U/L; alkaline phosphatase, 368 U/L; blood urea nitrogen, 16.6 mg/dL; creatinine, 1.4 mg/dL; erythrocyte sedimentation rate, 79 mm/hr; and C-reactive protein, 2.8 mg/dL. Blood coagulation test revealed a prothrombin time/activated partial thromboplastin time of 11.8/29.5 seconds. Abdominal radiography showed a huge gastric shadow with a large amount of food materials in the gastric lumen. Abdominal computed tomography showed a large amount of retained food materials in the stomach and diffuse wall thickening of the gastric antrum (
Fig. 1A). Endoscopy revealed marked edema of the mucosa, multiple ulcerations, and luminal narrowing and limited distensibility of the gastric antrum (
Fig. 1B). Endoscopy also showed pyloric stenosis with ulceration (
Fig. 1C), but endoscopic mucosal change was not observed in the duodenum (
Fig. 1D). We performed endoscopic biopsies of the gastric antrum and the duodenum, which revealed the deposition of eosinophilic amorphous materials in the lamina propria and the submucosa in the stomach but not in the duodenum on hematoxylin and eosin staining (
Fig. 2), and the accumulation of apple-green materials in the lamina propria and the submucosa in the stomach on Congo red staining (
Fig. 3A, B). Electron microscopy showed amyloid fibrils in the subepithelial layers (
Fig. 3C, D). The histological findings were compatible with amyloidosis, and the amyloid was identified as the AA type on immunohistochemical testing with monoclonal antibodies specific to serum amyloid A protein. Colonoscopy with random biopsies showed no colonic involvement by the amyloidosis. Bence-Jones proteins were present in urine, but an M-peak was not found in serum. Moreover, there were no abnormalities on bone marrow biopsy. Her final diagnosis was amyloidosis secondary to ankylosing spondylitis presenting with gastric outlet obstruction. Subtotal gastrectomy was recommended because of the worsening obstruction symptoms; however, she refused surgery and wanted to be transferred to another hospital. Three months later, she died of aspiration pneumonia during medical treatment.
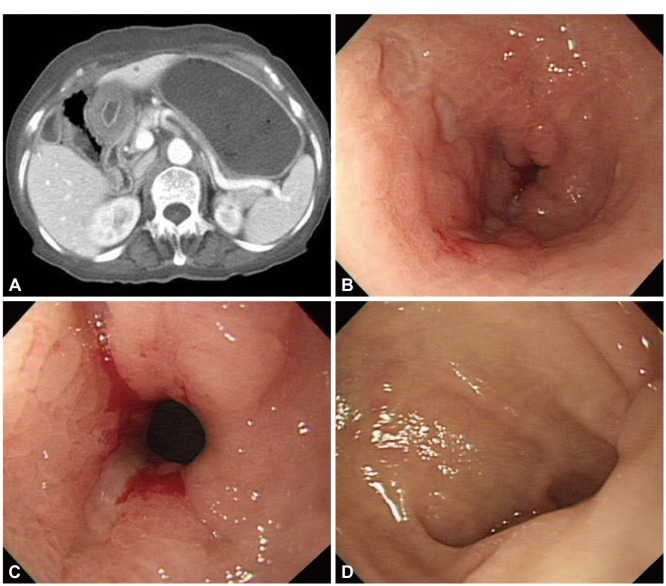 | Fig. 1(A) Computed tomography of the stomach showing a large amount of food stasis with focal submucosal thickening in the gastric antrum. (B) Endoscopic finding of the gastric antrum showing marked edema of the mucosa, multiple ulcerations, and luminal narrowing of the gastric antrum. (C) Endoscopic finding of the pylorus showing pyloric stenosis with ulceration. (D) Endoscopic finding of the duodenal bulb showing a normal appearance. 
|
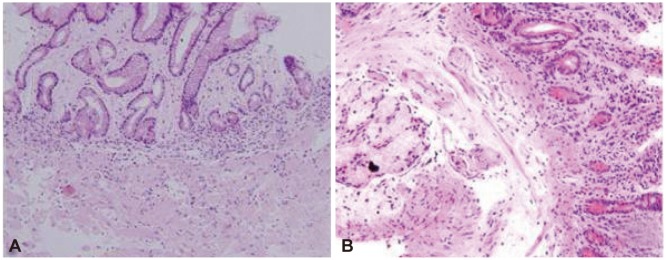 | Fig. 2(A) Photomicrograph of the gastric biopsy specimen showing deposition of eosinophilic amorphous materials in the lamina propria and the submucosa of the gastric antrum, consistent with amyloidosis (H&E stain, ×200). (B) Photomicrograph of the duodenal biopsy specimen showing deposition of amyloid fibrils in the lamina propria and the submucosa of the duodenum (H&E stain, ×200). 
|
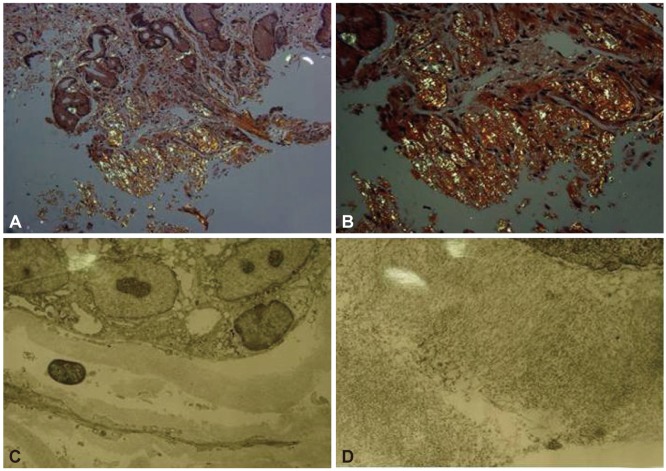 | Fig. 3(A, B) Polarization microscopic findings of the stomach showing apple-green birefringence (A, Congo red stain, ×200; B, ×400). (C, D) Electron microscopic findings of the stomach showing amyloid fibrils attached to the subepithelial layers (C, ×2,500; D, ×4,000). 
|
Go to :

DISCUSSION
Amyloidosis is a group of disorders characterized by the accumulation of amyloid in various organs and tissues of the body. It is categorized according to the tissue distribution of the amyloid as systemic or localized amyloidosis, and according to the presence or absence of the predisposing factors as AA or primary (AL) amyloidosis.
6 Serum amyloid A protein is an acute phase reactant that is produced because of chronic infection or inflammation. The most common causes of AA amyloidosis are inflammatory arthritides and spondyloarthropathies. The prevalence of AA amyloidosis in patients with ankylosing spondylitis was estimated to be from 4.4% to 8.6%.
7
The frequency of clinically apparent gastrointestinal involvement varies with the type of amyloidosis. Gastrointestinal disease is present in as many as 60% of patients with AA amyloidosis.
8 In cases of gastrointestinal tract involvement, gastrointestinal symptoms include gastrointestinal bleeding, chronic intestinal dysmotility, malabsorption, and protein-losing enteropathy. AA amyloidosis presents with diarrhea and malabsorption, whereas AL amyloidosis usually presents with constipation, mechanical obstruction, or chronic intestinal pseudo-obstruction.
9 Especially, amyloidosis with gastric involvement presents with gastroparesis, epigastric pain, gastric outlet obstruction, gastric amyloid tumors, peptic ulceration, hematemesis, and melena.
10 Gastric amyloidosis with obstructive symptoms is usually due to submucosal tumors, polyps, or antral narrowing but rarely due to lesions similar to linitis plastic.
11,
12 Endoscopically, AL amyloidosis typically forms a polypoid mass lesion and AA amyloidosis shows a fine granular appearance.
13
In our case, the patient presented with gastric outlet obstruction, which is unusual in AA amyloidosis. Moreover, endoscopically, she showed multiple ulcerations on the edematous mucosa of the antrum in the stomach, which showed a poorly demarcated margin suggestive of gastric lymphoma or linitis plastica. Gastric amyloidosis could be misdiagnosed as gastric cancer because of the likeness in endoscopic and radiologic findings. Bedioui et al.
14 reported a case of gastric amyloidosis mimicking linitis plastica. Although they performed various examinations, including gastroscopy with biopsy, barium meal, and endoscopic ultrasonography, they did not find any evidence of amyloidosis. However, they finally diagnosed amyloidosis after a subtotal gastrectomy.
Although most of the gastric amyloidosis cases are not related to gastric cancer, some might be associated with gastric malignancies.
15 In such cases, the confirmative diagnostic method is biopsy.
16 The amyloid displays amorphous, homogenous, translucent, and acidophilic materials under a light microscope on hematoxylin and eosin staining. With Congo red staining, the amyloid could be observed as an apple-green birefringence under polarized light. Under an electron microscope, the amyloid is seen as thin linear fibrils. In our case, we found apple-green birefringence under the light microscope and thread-like fibrils under the electron microscope on Congo red staining. It involved the stomach and the duodenum but there was no colonic involvement. Analysis of monoclonal immunoglobulin in serum and urine has little role in the diagnosis of AA amyloidosis but could help exclude AL amyloidosis.
The treatment of AA amyloidosis is focused on the treatment of the underlying inflammatory disease, whereas the mainstay treatment for AL amyloidosis has been chemotherapy. Recently, several reports have described the benefits of tumor necrosis factor-α (TNF-α) inhibitors in patients with amyloidosis secondary to chronic inflammatory disease.
17 These agents have a remarkable ability to suppress inflammatory reactions.
17 Two reports about AA amyloidosis and TNF-α inhibitor therapies showed improvement of protein-uria and renal function in patients with renal amyloidosis secondary to ankylosing spondylitis.
18,
19 However, studies on the treatment of gastrointestinal amyloidosis especially for patients with ankylosing spondylitis are limited. McMahan et al.
17 emphasized the importance of early treatment with a TNF-α inhibitor for gastrointestinal amyloidosis secondary to ankylosing spondylitis because delayed treatment might prevent patients from obtaining the full benefits of the drug.
The prognosis of amyloidosis differs according to type. AL amyloidosis has a poor prognosis with a median survival of <2 years despite treatment with mephalan and steroids.
13 The prognosis of AA amyloidosis differs according to the underlying disease and is correlated with serum amyloid A concentration.
20 A cohort study of patients with systemic AA amyloidosis showed a median survival of 133 months.
20 In that cohort study, mortality, amyloid burden, and renal prognosis were all significantly correlated with the serum amyloid A concentration during follow-up.
20 The risk of death was 17.7 times higher in patients with serum amyloid A concentrations of ≥155 mg/L compared to that in those with concentrations of 4 mg/L.
20 Whole-body
123I-labeled serum amyloid P component scintigraphy for measuring the concentration of serum amyloid A is not commercially used in Korea yet, so we were not able to measure the amyloid burden in our patient.
In this case, the patient presented with nonspecific symptoms such as nausea, vomiting, and abdominal distention, and endoscopy showed segmental luminal narrowing similar to linitis plastica, which is rare in patients with AA amyloidosis. However, with suspicion, we performed Congo red staining and finally concluded a diagnosis of amyloidosis secondary to ankylosing spondylitis. Therefore, in a patient with long-standing ankylosing spondylitis, gastric amyloidosis should be differentiated when the patient presents with gastric outlet obstruction.
Go to :







 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download