Abstract
In most cases of ingested foreign bodies, endoscopy is the first treatment of choice. Moreover, emergency endoscopic removal is required for sharp and pointed foreign bodies such as animal or fish bones, food boluses, and button batteries due to the increased risks of perforation, obstruction, and bleeding. Here, we presented two cases that needed emergency endoscopic removal of foreign bodies without sufficient fasting time. Foreign bodies could not be visualized by endoscopy due to food residue; therefore, fluoroscopic imaging was utilized for endoscopic removal of foreign bodies in both cases.
Most foreign body ingestions occur in the pediatric population [1,2] and include coins, toys, magnets, and batteries [3]. Conversely, most foreign body ingestions in adults include food (meat) boluses, bones, toothbrushes, spoons, and razor blades [1,3]. Although most of the ingested foreign bodies pass spontaneously with conservative management [1], certain foreign bodies such as sharp and pointed objects, animal or fish bones, food boluses, and button batteries should be removed immediately because of the high risk of complications [1,3].
The European Society of Gastrointestinal Endoscopy recommends emergency endoscopic removal (preferably within 2 hours, but within a maximum of 6 hours) of batteries as well as of foreign bodies that cause complete esophageal obstruction or are sharp and pointed [4]. Endoscopy, using various instruments such as retrieval forceps, retrieval graspers, polypectomy snares, endoscopic baskets, and nets or bags, is used for the removal of foreign bodies [1,3,4].
However, few reports have described emergency endoscopic removal of foreign bodies using fluoroscopy in patients with insufficient nil per os (NPO) time. Here, we reported two patients who underwent emergency endoscopic removal of foreign bodies under fluoroscopic guidance, as the objects could not be observed by direct viewing due to abundant gastric food content.
A 60-year-old man was admitted to the emergency room (ER) after accidentally ingesting a 2-cm-long nail 1 hour earlier. On arrival, he did not present with any symptoms, and his vital signs were stable: blood pressure, 125/78 mm Hg; heart rate, 85 beats per minute; respiratory rate, 20 breaths per minute; body temperature, 36.5°C. He was alert and oriented. His bowel sounds were normal, with no abdominal tenderness. Laboratory examination showed thrombocytopenia (123,000/mm3); other values were unremarkable.
Chest radiography showed one 20-mm-long radio-opaque nail in the esophagus at the T9–10 level (Fig. 1). As there was no evidence of gastric perforation on physical examination and by radiological assessment, esophagogastroduodenoscopy using a single-channel endoscope (GIF-H260; Olympus Optical Co., Ltd., Tokyo, Japan) was performed 3 hours after arrival. On endoscopic view, the nail could not be visualized in the stomach because of the presence of abundant food residue in the greater curvature of the gastric body and fundus (Fig. 1B). Despite exploration using forceps, the nail within the residue could not be visualized or ensnared.
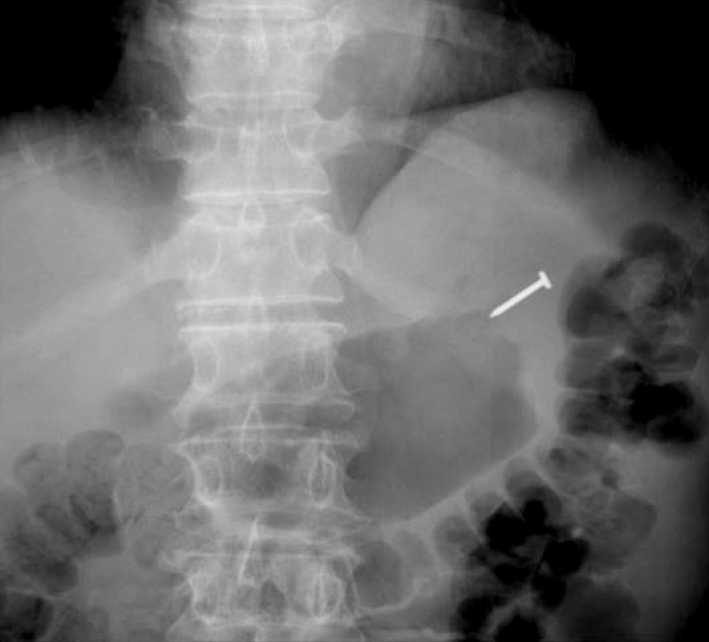
Owing to the high risk of gastrointestinal injury and perforation from nail ingestion, esophagogastroduodenoscopy under fluoroscopic guidance was planned to precisely locate and remove the nail. On fluoroscopic examination, the nail was located in the fundic area (Fig. 2) and could be reached by endoscopy. The object embedded in food residue was grasped using alligator forceps (Olympus Co., Tokyo, Japan) and retrieved from the stomach by using an endoscopic protector hood (MTW, Wesel, Germany) to prevent further mucosal injury (Fig. 3). After the removal of the nail (Fig. 3D), the absence of mucosal injury in the gastrointestinal junction and esophagus was confirmed by endoscopy. One hour later, the patient was discharged from the ER, without further medication, and remained symptom-free at the 1-week outpatient follow-up.
A 1-year-old boy was admitted to the ER after ingesting a button battery about 3 hours earlier. On arrival, he did not present with any abnormal behavior, and his vital signs were stable: blood pressure, 99/61 mm Hg; heart rate, 109 beats per minute; respiratory rate, 22 breaths per minute; body temperature, 36.8°C. Bowel sounds were normal. There was no abdominal tenderness.
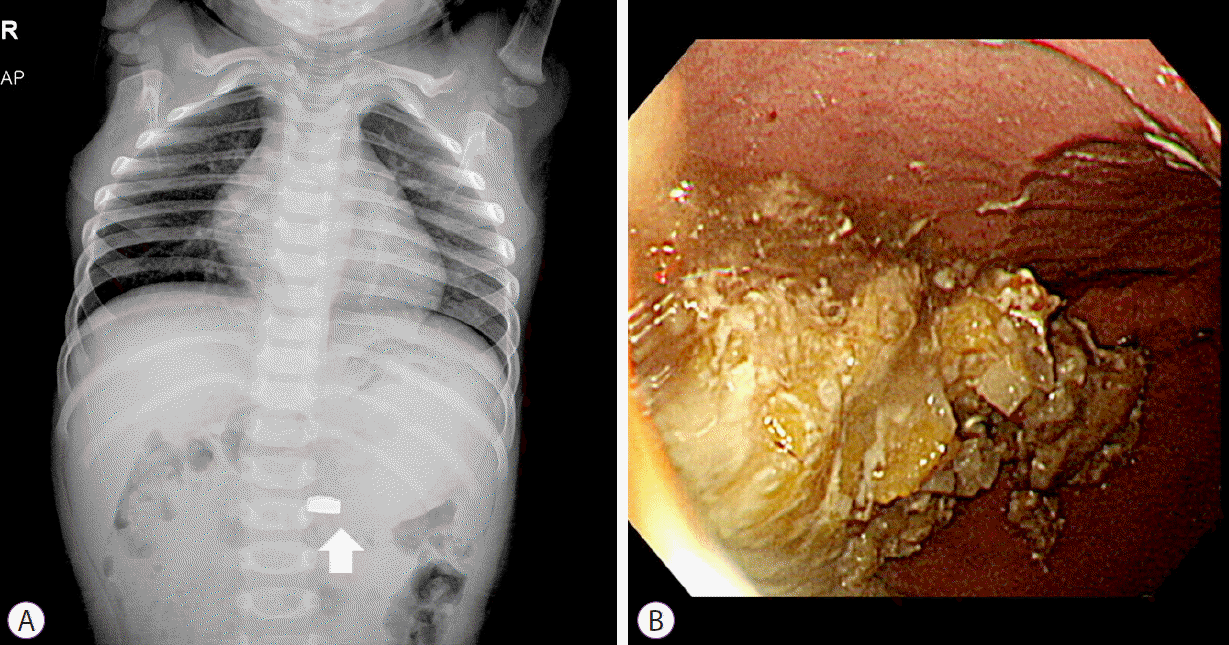
Chest radiography showed one 20-mm metallic foreign body in the stomach (Fig. 4), and emergency endoscopic removal of the foreign body was planned because of the risk of electrical discharge and/or chemical injury [3]. However, initial attempts at endoscopic retrieval of the button battery failed because of abundant food residue in the stomach resulting from insufficient NPO time.
Exploration through the food residue, using forceps, failed to locate the button battery; thus, esophagogastroduodenoscopy under fluoroscopic guidance was performed. Fluoroscopic imaging was successful in visualizing the battery in the greater curvature of the stomach, which was removed using alligator forceps and endoscopic basket (Olympus Co.) without complications (Fig. 5).
After successful conclusion of the procedure, the patient did not exhibit any abnormal behavior and was discharged from the hospital without further medication 4 hours later. At the 1-week outpatient follow-up visit, the patient remained asymptomatic.
We presented two cases of emergency endoscopic removal of foreign bodies by using fluoroscopic imaging owing to insufficient NPO time, with no complications. In both patients, the ingested foreign bodies—a nail and a button battery— were successfully removed by endoscopy using alligator forceps and a protector hood or a basket with fluoroscopic guidance. No complications occurred during or after the procedures in both cases.
While most ingested foreign bodies (80%–90%) pass spontaneously, the remaining 10%–20% require endoscopic removal and less than 1% of the cases need surgery [3-5]. Flexible esophagogastroduodenoscopy is the best diagnostic and therapeutic approach in the management of foreign bodies and food bolus impaction in the upper gastrointestinal tract, with success rates greater than 95% and complication rates of 0%–5% [1,2,4].
The management strategy for removal of ingested foreign bodies depends on patient age; clinical conditions such as size, shape, content, and anatomic location of the ingested foreign body; and time since ingestion [2]. Foreign body removal devices that are widely used in the gastrointestinal tract include the protector hood, rat-tooth forceps, shark-tooth forceps, alligator forceps, polypectomy snare, and endoscopic basket and net [1].
The removal of sharp/pointed objects is usually achieved with the protector hood, banding device cap, and endoscopic overtube to prevent mucosal injury during retrieval [1,4]. In the first patient who ingested the nail, an endoscopic protector hood with alligator forceps was used to prevent mucosal damage. Secure retrieval of blunt or round objects such as coins and disc batteries can be attempted with endoscopic baskets, nets, or bags [4]. An endoscopic basket was used in the second patient to avoid slippage during the removal of the button battery.
Sharp-pointed or long objects, food bolus impaction, and button batteries can increase the risk of perforation, obstruction, and bleeding. Therefore, in such cases, emergency intervention with endoscopic or surgical removal of the foreign body is necessary [1,3]. A recent study by Lee et al. [6] reported that the major complications of foreign bodies were laceration (9.5%), ulceration (6.8%), bleeding (3.4%), and perforation (2.1%). In that study, among those with foreign body-related perforation, ten patients received medical treatment, whereas the remaining four patients required surgical treatment [6]. In another study, Hong et al. [7] reported that foreign body–mediated complications included perforation (1.5%), laceration (16%), infection (0.5%), and ulceration (5.7%). In that study, all three cases with perforation needed surgical management [7]. In the present report, despite potential complications due to improper choice of endoscopic instruments and delayed removal of foreign bodies, the foreign bodies were successfully removed with the guidance of fluoroscopic imaging within a short time, without complications.
There are few reports of emergency and safe endoscopic removal of foreign bodies by using fluoroscopic guidance in the presence of food residue in the gastrointestinal tract. This is an unusual case report of two emergency cases with foreign bodies that were successfully removed with fluoroscopy-guided endoscopy without complications.
REFERENCES
1. Tang SJ. Endoscopic management of foreign bodies in the gastrointestinal tract. Video Journal and Encyclopedia of GI Endoscopy. 2013; 1:35–38.

2. ASGE Standards of Practice Committee, Ikenberry SO, Jue TL, et al. Management of ingested foreign bodies and food impactions. Gastrointest Endosc. 2011; 73:1085–1091.

3. Sugawa C, Ono H, Taleb M, Lucas CE. Endoscopic management of foreign bodies in the upper gastrointestinal tract: a review. World J Gastrointest Endosc. 2014; 6:475–481.

4. Birk M, Bauerfeind P, Deprez PH, et al. Removal of foreign bodies in the upper gastrointestinal tract in adults: European society of gastrointestinal endoscopy (ESGE) clinical guideline. Endoscopy. 2016; 48:489–496.

5. Anderson KL, Dean AJ. Foreign bodies in the gastrointestinal tract and anorectal emergencies. Emerg Med Clin North Am. 2011; 29:369–400. ix.

Fig. 1.
(A) Chest radiography showing a radio-opaque, 20-mm-long nail in the esophagus, at the T9-T10 vertebral level (black arrow). (B) Endoscopy showing abundant food residue in the stomach.
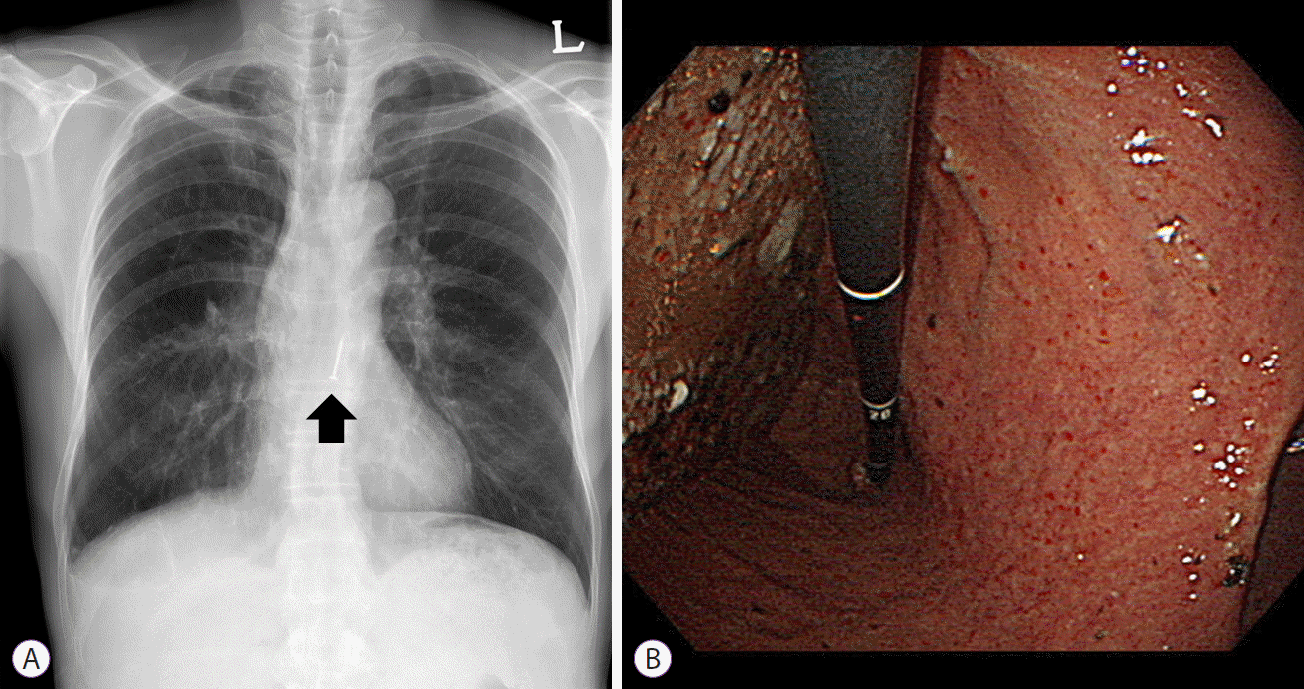
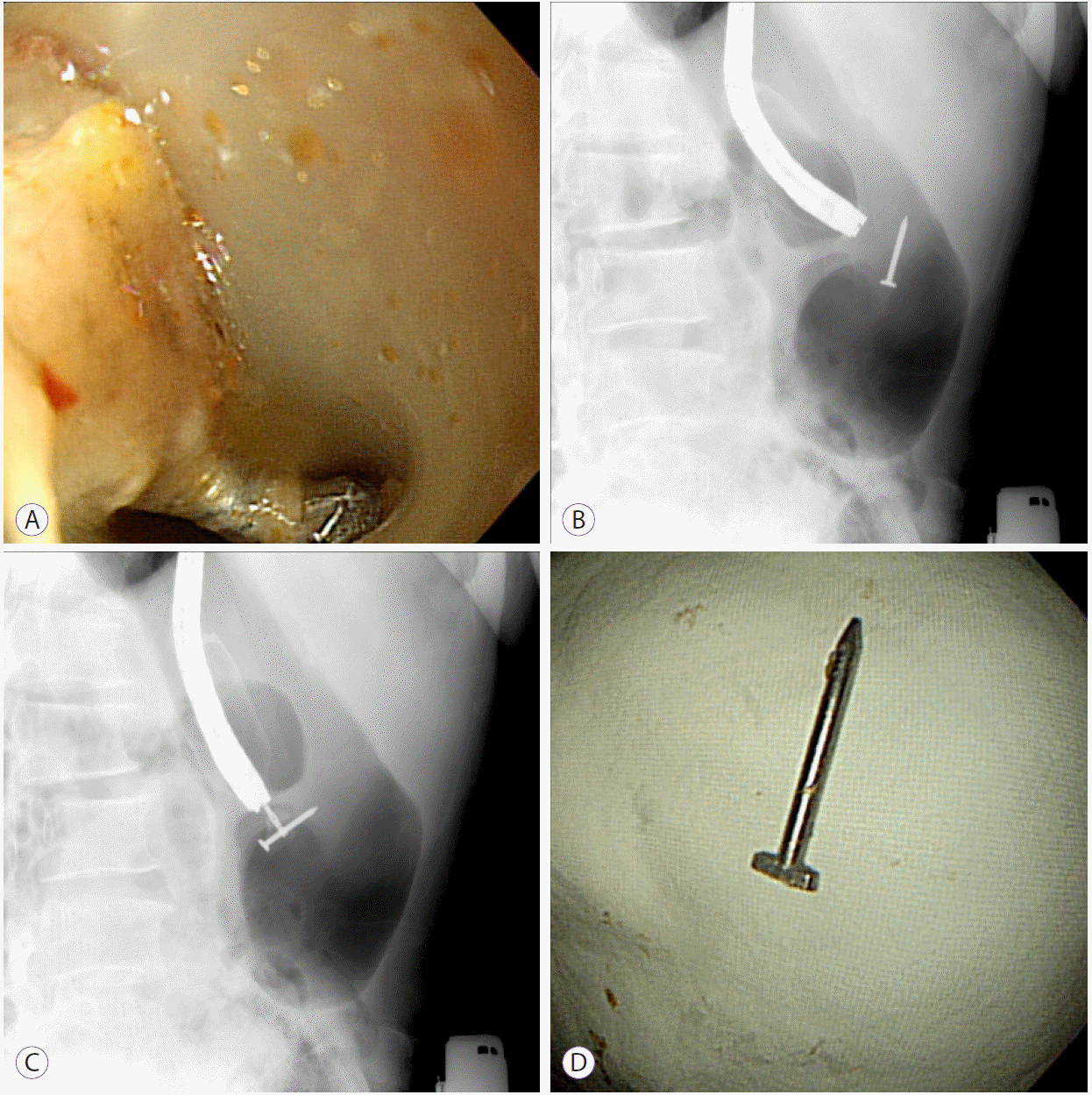
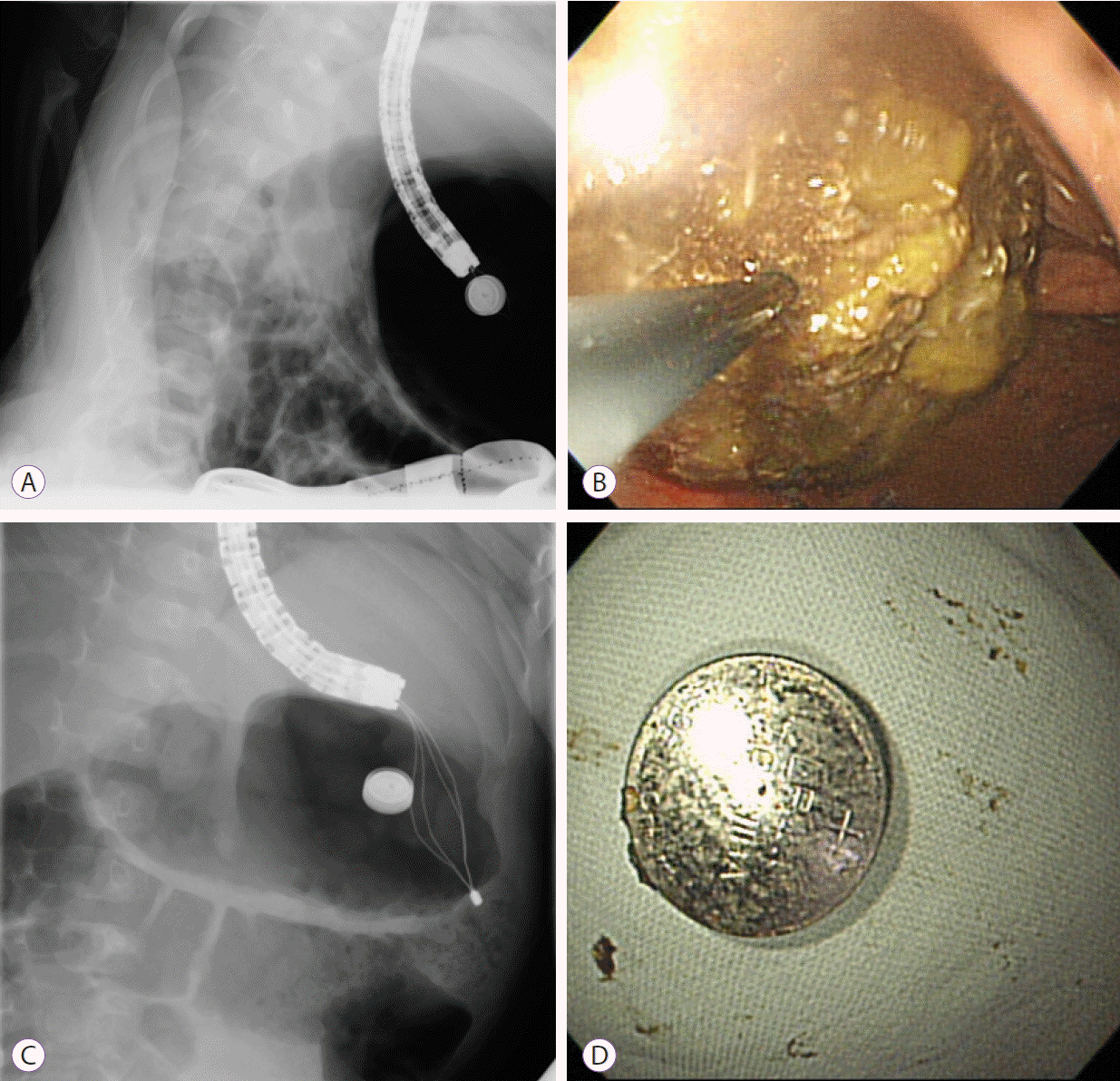
Fig. 3.
Endoscopic removal of the nail under fluoroscopic guidance. (A, B) The nail in the fundic area. (C) Alligator forceps were used to grasp the nail, which was retrieved using the protector hood. (D) The nail was removed successfully and without any complications.




 PDF
PDF Citation
Citation Print
Print


 XML Download
XML Download