INTRODUCTION
MATERIALS AND METHODS
Subjects
Treatment protocol
Voice analysis
Swallowing function
Statistical analysis
RESULTS
Characteristics of subjects
Table 1
Baseline characteristics of patients
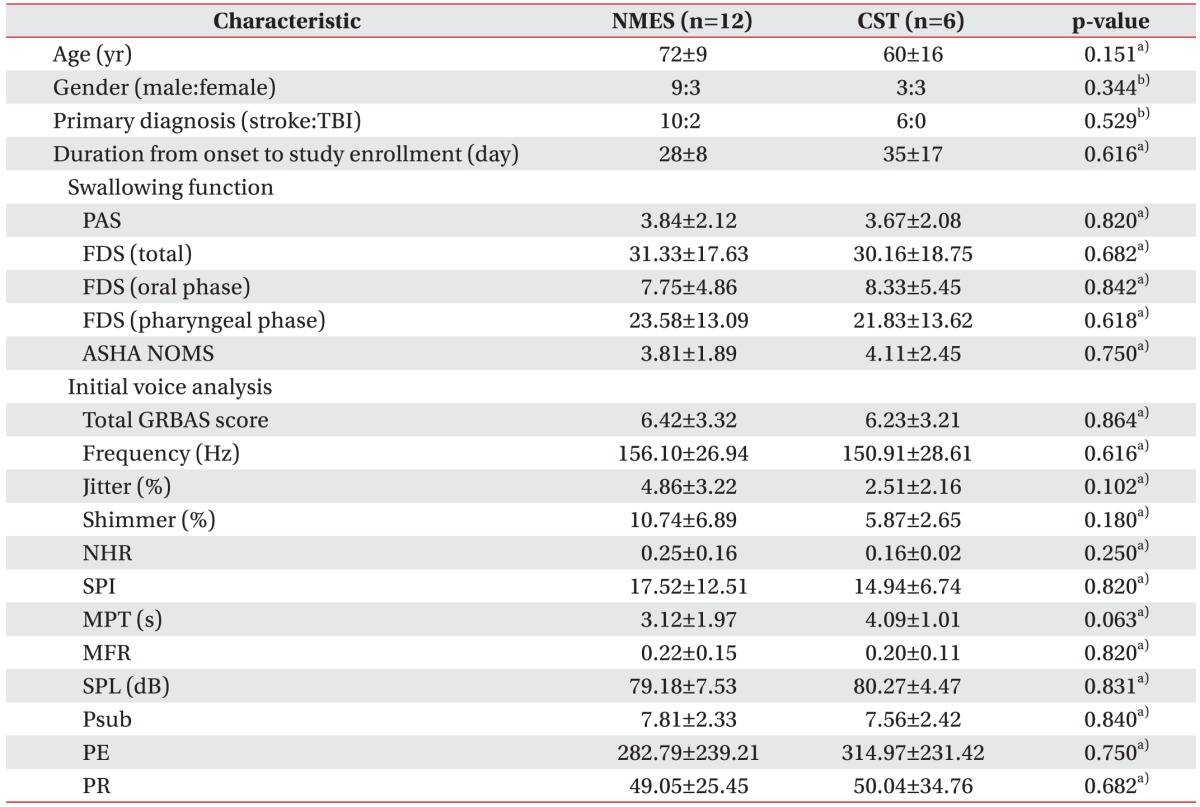
Values are presented as mean±standard deviation or numbers.
NEST, neuromuscular electrical stimulation; CST, conventional swallowing training; TBI, traumatic brain injury; PAS, penetration-aspiration scale; FDS, functional dysphagia scale; ASHA NOMS, American Speech-Language-Hearing Association National Outcome Measurement System swallowing scale; GRBAS, grade, roughness, breathiness, asthenia, and strain; NHR, noise-to-harmonic ratio; SPI, soft phonation index; MPT, maximal phonation time; MFR, mean flow rate; SPL, sound pressure level; Psub, subglottic pressure; PE, phonation efficiency; PR, phonation resistance
a)Mann-Whitney U test, b)Fisher's exact test.
Voice analysis
 | Fig. 1Schematization of perceptual evaluation changes: total GRBAS score at baseline and at 2 and 4 weeks after initiation of the study in each group. GRBAS, grade, roughness, breathiness, asthenia, and strain. a)p<0.017 by Mann-Whitney U test with Bonferroni correction. b)p<0.025 by Wilcoxon signed-rank test with Bonferroni correction. |
Table 2
Improved acoustic evaluation results

Values are presented as mean±standard deviation.
NEST, neuromuscular electrical stimulation; CST, conventional swallowing training; NHR, noise-to-harmonic ratio; SPI, soft phonation index; T0, baseline; T1, 2 weeks after initiation of study; T2, 4 weeks after initiation of study; NS, non-specific.
*p<0.05 by repeated-measures ANOVA.
**p<0.025 by Wilcoxon signed-rank test with Bonferroni correction.
Table 3
Improved aerodynamic evaluation results
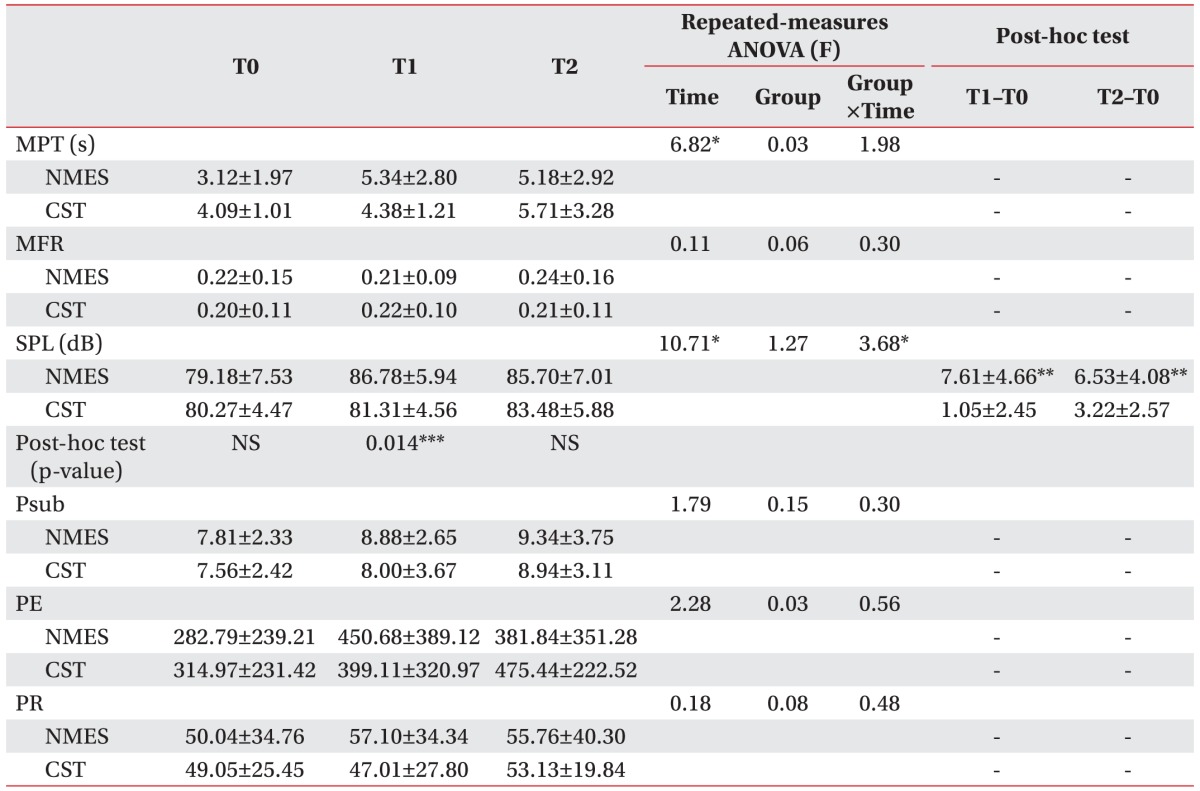
Values are presented as mean±standard deviation.
NEST, neuromuscular electrical stimulation; CST, conventional swallowing training; MPT, maximal phonation time; MFR, mean flow rate; SPL, sound pressure level; Psub, subglottic pressure; PE, phonation efficiency; PR, phonation resistance; T0, baseline; T1, 2 weeks after initiation of study; T2, 4 weeks after initiation of study; NS, non-specific.
*p<0.05 by repeated-measures ANOVA.
**p<0.025 by Wilcoxon signed-rank test with Bonferroni correction.
***p<0.017 by Mann-Whitney U test with Bonferroni correction.
Swallowing function
Table 4
Improved swallowing function results
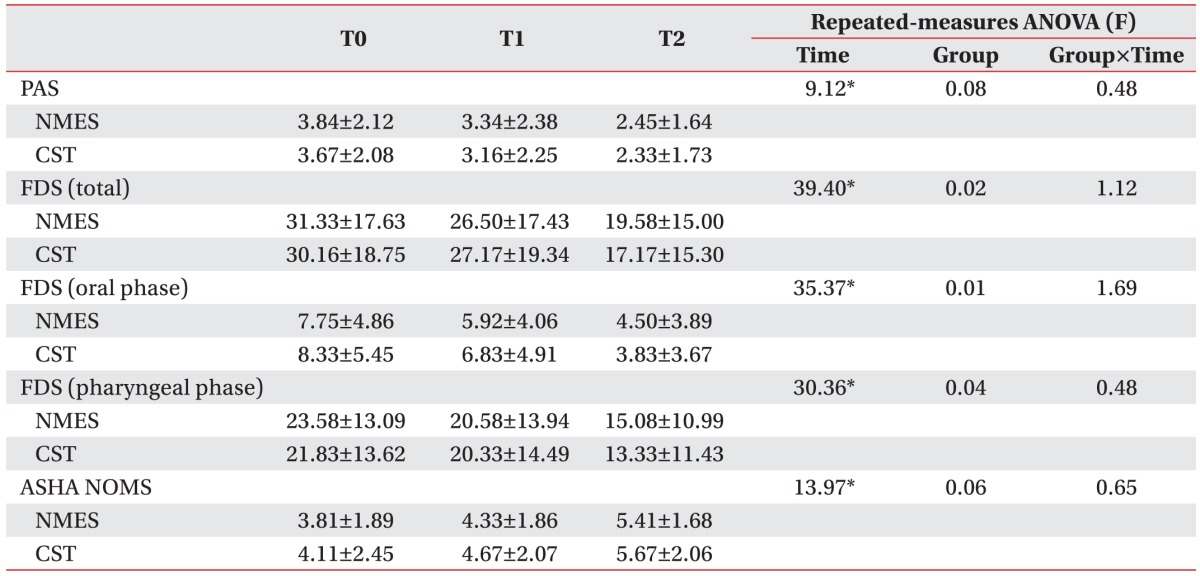
Values are presented as mean±standard deviation.
NEST, neuromuscular electrical stimulation; CST, conventional swallowing training; PAS, penetration-aspiration scale; FDS, functional dysphagia scale; ASHA NOMS, American Speech-Language-Hearing Association National Outcome Measurement System swallowing scale; T0, baseline; T1, 2 weeks after initiation of study; T2, 4 weeks after initiation of study.
*p<0.05 by repeated-measures ANOVA.




 PDF
PDF ePub
ePub Citation
Citation Print
Print






 XML Download
XML Download