A 74-year-old female with a history of diabetes and multiple coronary stent insertion [right coronary artery (RCA) and left anterior descending coronary artery] presented to the emergency department (ED) with acute chest pain. Electrocardiogram (ECG) in the ED showed ST elevation in the II, III, and aVF leads as well as increase in the serum troponin T (0.312 ng/mL, normal range 0–0.1 ng/mL), indicating ST-segment elevation myocardial infarction. Occlusion of RCA at its origin was identified on immediate percutaneous coronary intervention (PCI). After balloon dilation of the occluded segment, a pseudoaneurysm was demonstrated at the proximal portion of the RCA, suggesting rupture (Figure 1). PCI was successfully performed although pseudo-aneurysm was developed during the procedure (Figure 1). On hospital day 8, the patient developed a fever (38.5°C). An epicardial coronary abscess with multiple air-pockets and rim-enhancement extending into the right atrioventricular (AV) groove and pericardium was identified on the chest computed tomography (CT) (Figure 2). Klebsiella pneumoniae was identified on blood cultures. Subsequent open heart surgery confirmed the CT findings, and removal of necrotic tissue and abscess with drainage catheter placement was done without extraction of RCA stent. After 6 weeks, the patient was improved and discharged.
Coronary stent infection has several risk factors (i.e., virulence of the pathogen, host response, device properties, and procedural difficulty). The most common cause of coronary stent infection is procedure-related infection from the skin or catheters, often due to Staphylococcus aureus (80%) followed by Pseudomonas aeruginosa (20%).1)2)3) In previous reports, the primary tool to identify coronary stent infection was the identification of pseudoaneurysm formation on coronary angiography.1)2)3) However, coronary angiography only visualizes a portion of the overall abscess pocket. In contrast, CT can evaluate the overall extent of coronary stent infection, facilitating proper therapeutic planning. In this regard, the case shows the value of CT in diagnosing complications of coronary stent infection and providing appropriate treatment planning.
Notes
Funding: The authors received no financial support for the research, authorship, and/or publication of this article.
Author Contributions:
Conceptualization: Lee D, Kim IJ, Yoo SM.
Formal analysis: Lee D, Kim IJ.
Investigation: Lee D, Kim IJ, Son MJ, Yoo SM, Lee HY, White CS.
Methodology: Lee HY, Son MJ, White CS.
Supervision: Yoo SM.
Writing - original draft: Lee D, Kim IJ, Son MJ, Yoo SM, Lee HY, White CS.
Writing - review & editing: Lee D, Kim IJ, Son MJ, Yoo SM, Lee HY, White CS.
References
1. Elieson M, Mixon T, Carpenter J. Coronary stent infections: a case report and literature review. Tex Heart Inst J. 2012; 39:884–889. PMID: 23304047.


2. Del Trigo M, Jimenez-Quevedo P, Fernandez-Golfin C, et al. Very late mycotic pseudoaneurysm associated with drug-eluting stent fracture. Circulation. 2012; 125:390–392. PMID: 22249529.

3. Reddy K V C, Sanzgiri P, Thanki F, Suratkal V. Coronary stent infection: interesting cases with varied presentation. J Cardiol Cases. 2018; 19:5–8. PMID: 30693049.


Figure 1
Percutaneous coronary angiography images. (A) Coronary angiographic image shows total occlusion at the origin of the right coronary artery (white arrowheads). Note multiple coronary stents in the RCA and left anterior descending coronary artery inserted in 16 months earlier. (B) Dissecting aneurysm or pseudoaneurysm (black arrows) is noted on a coronary angiographic image after balloon dilatation. (C) After completion of percutaneous coronary intervention by using Xience stent (3.5×33 mm), there is no evidence of residual pseudoaneurysm on coronary angiography.

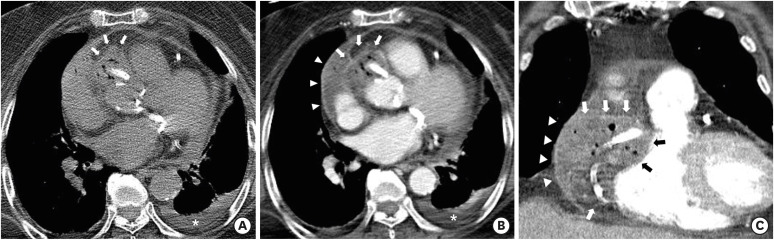
Figure 2
Chest CT images. (A) An air containing mass with high attenuation is noted on preconstrast CT around the proximal right coronary artery stent and along the right atrioventricular groove at the aortic sinus level (white arrows). Left pleural effusion is also seen (white asterisk). (B) On contrast enhanced axial CT image at the level of the left atrium, a low attenuation mass (arrows) with peripheral enhancement and multiple air-pockets is noted, consistent with air-forming epicardial coronary abscess (white and black arrows). Pericardial effusion (arrowheads) with linear pericardial thickening and enhancement is also demonstrated, indicating pericarditis (white arrowheads). (C) Coronal CT image at the level of the right ventricle shows similar findings.
CT = computed tomography.




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download