INTRODUCTION
Coronavirus disease 2019 (COVID-19) cases in the world are 17,507,359 as of July 31, 2020.
1 Korea has about 52 million population, 18% of which is a pediatric population ≤ 19 years.
2 As of July 31, 2020, 14,305 individuals were confirmed with COVID-19 in Korea. The first pediatric patient was a 10-year Korean girl diagnosed on February 18, 2020.
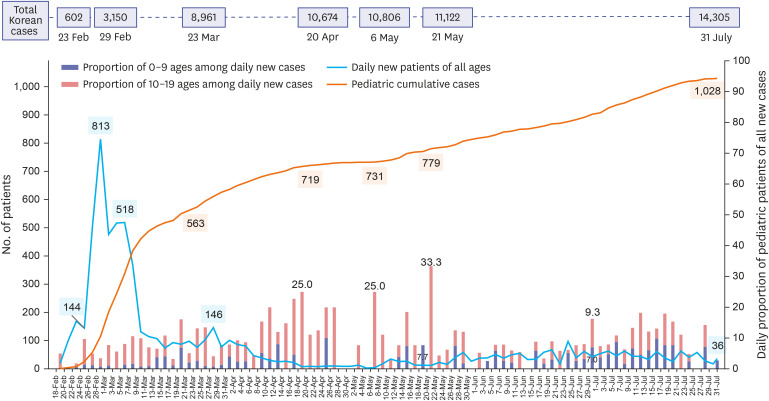
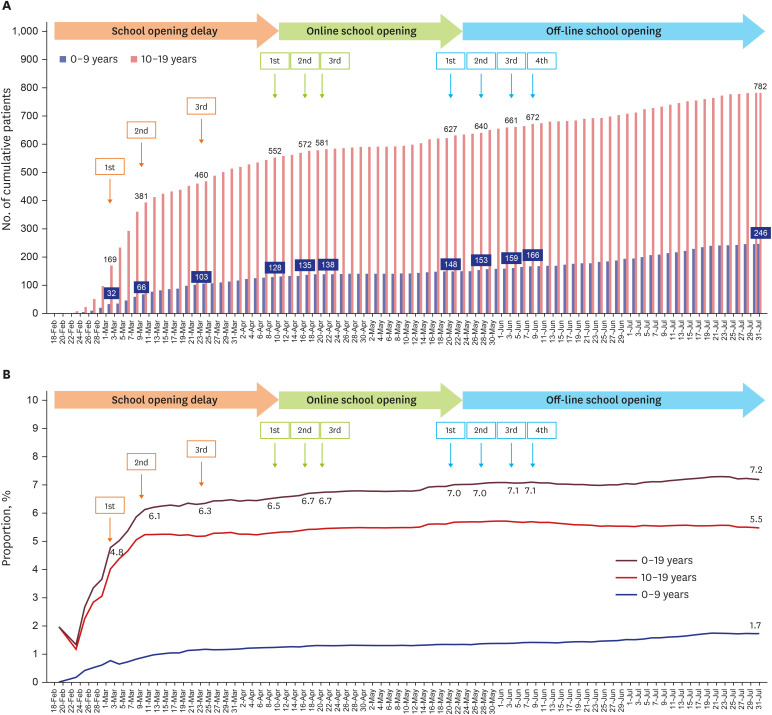
3 As of July 31, 2020, 1,028 Korean children ≤ 19 years have been diagnosed with COVID-19 (21.8 pediatric patients per 100,000 population ≤ 19 years). The proportions of pediatric cases ≤ 19 years and ≤ 9 years are 7.2% and 1.7% of all confirmed cases, respectively by data of the Korea Centers for Disease Control and Prevention (KCDC).
4
Respiratory virus infection among school-aged children is an important epidemiologic consideration. Data on severe acute respiratory syndrome coronaviru-2 (SARS-CoV-2) transmission from a pediatric index case to others at school settings are limited. However, it is unclear whether school closures are effective during coronavirus outbreaks due to SARS, Middle East respiratory syndrome (MERS), or especially SARS-CoV-2 of which transmission dynamics appear to be different.
It has been several months since schools are closed in more than 190 countries in the world, affecting 1.57 billion children, about 90% of the world student population. According to the United Nations Educational, Scientific and Cultural Organization (UNESCO), countrywide school closure peaked to 194 countries on April 13, 2020, and it decreased to 40 countries on July 31, 2020.
5
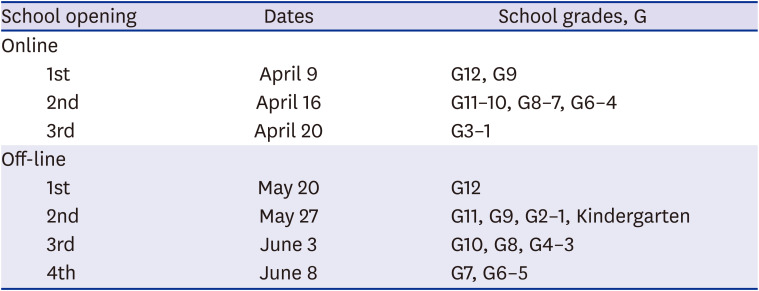
Korea also delayed the school opening after winter vacation and closed the schools because of COVID-19 outbreak. However, online and off-line (in-person) school opening proceeded. We reviewed the pediatric epidemiology of COVID-19 according to the timeline of school opening delay and school re-opening using the data of the KCDC, and Korean Ministry of Education (KMOE) website.
6
We examined whether school opening led the increase of pediatric COVID-19 cases in Korea, a country that had never been lockdown, only performed varying degrees of social distancing and rigorous contact tracing with rapid testing for early detection.
Discussion
This report describes the impact of school opening on pediatric COVID-19 epidemiology in Korea. There was no significant increase in the number of pediatric patients or the proportion of pediatric patients among all confirmed cases in the nation after the off-line (in-person) school opening. School opening did not cause significant school-related outbreak with good adherence to safety measures for symptom monitoring, personal hygiene, wearing masks, and distancing among students.
Closing and re-opening of schools and preschools is a major educational, political, and a public health issue worldwide. There are concerns about the transmission of the virus among children and teenagers in the closed space of the school. However, the negative impact of limiting social and physical activities for an extended period in children is worrisome. In addition, significant inequalities among children with a high- and low-socioeconomic environment may exist in online learning accessibility and the level of care provided at home with prolonged school closure.
It is well-known that children are susceptible to many respiratory viral infections with frequent epidemics in the communities. Therefore, there were questions about the role of the pediatric population for the spread of the SARS-CoV-2. However, early transmission clusters were identified mainly from adults, making children less likely to be index cases in households or the communities. As data accumulated, a significant proportion of pediatric patients are known to be asymptomatic or mildly symptomatic, with an exception for unusual cases with multisystem inflammatory syndrome in children (MIS-C).
1516 In addition, pediatric patients with COVID-19 also appeared to have similarly high viral loads at the early stage of illness as in adult patients.
171819 Therefore, the possibility for virus transmission from pre-symptomatic or mildly symptomatic pediatric index case(s) to others can also be questioned.
1920
However, there are limited data that reported the transmission among children that led to a large outbreak, especially in school exposure. A systematic review also suggested that children seem unlikely to be the main drivers of the COVID-19 pandemic.
21 It is not clear whether the viral transmission dynamic in the pediatric population is different from that of adults, or this may be simply because most schools are closed for extended periods. There may be certain different features in the pediatric population that need to be further explored.
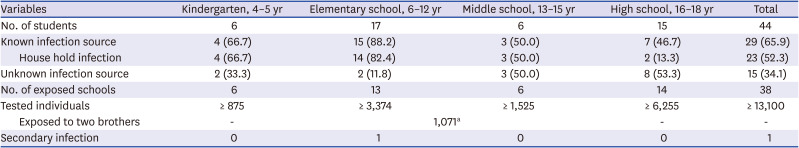
It is of interest that of more than 13,000 students and staffs tested from 38 schools and preschools, only one additional student was infected in the same classroom at the elementary school. Based on our data, we consider that spread of COVID-19 within Korean schools has been very limited even after off-line classes started while following the rules for symptom monitoring and distancing among students. Since rigorous contact tracing and tests have been performed in Korea from the early phase of pandemic, there is little possibility that there are hidden pediatric cases. In addition, a recent seroepidemiological survey reported that only 0.03% of tested positive for SARS-CoV-2 antibody among 3,055 Koreans.
22 Therefore, we consider that transmission among children at school appears to be very low and what we observed in this study would represent the real situation of the Korean pediatric population.
Transmission from a pediatric index patient to others (children or adults) and susceptibility of children, when exposed to infected index case (children or adults), may be different from that of adults. The secondary attack rate from the index pediatric patient of the household has been reported as low as 0.5% (0 to 2.6%) in Korean data.
23 In addition, low angiotensin-converting enzyme 2 (ACE2) gene expression was observed in nasal epithelium of children relative to adults.
24 These findings may help explain why COVID-19 is less prevalent in children.
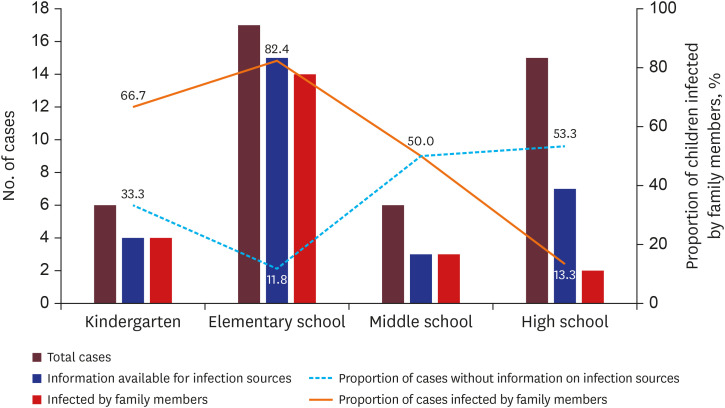
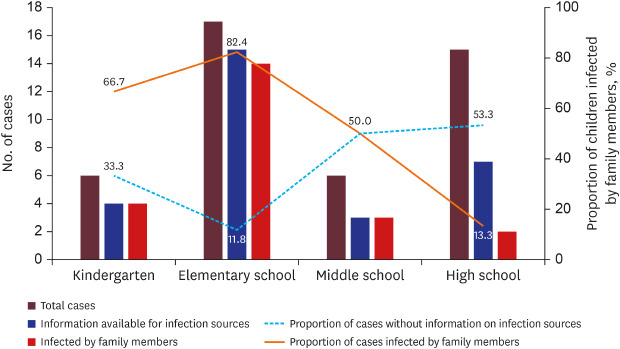
It is of note that the infection sources were more likely available in the younger age group (kindergarten and elementary school) than the older age group. When the information on infection source was available, the majority of the younger children were infected by family members. In a study from China, they also reported that 90.1% of 171 pediatric cases were related to family clusters.
25 In a study from Switzerland on 40 pediatric cases, they investigated the dynamics of infection in their families; one or more adult family member was suspected or confirmed for COVID-19 before symptom onset of the study child in 79% of households.
26 Therefore, the most common infection sources for pediatric cases appear to be their adult family members; children are not the primary source of infection or did not cause large outbreaks at school.
2728 Careful attention should be paid to older adolescents who may have more sources of infection outside of the household.
28
There are some limitations to this study. First, our epidemiologic data are not complete since our data were collected from publicly available press releases without detailed epidemiologic information. Second, we only analyzed the situation when the index patient was a student and did not examine the situation when the index patient was an adult staff. However, overall, there were no large school outbreaks after in-person school opening in both situations when exposures occurred after a student or an adult staff was identified as the index at school. Third, we could not analyze the data in detail by the region, which could be added in the future study. Finally, the data mainly contained numbers of the confirmed cases and exposed individuals who were tested, but detailed epidemiologic investigation data was insufficient. However, we tried to fill up the data as much as possible by follow-up data search when the additional information was released on any additional student cases (either yes or no) in the same school of the index student.
Although there are several reports from the school exposure investigation in various countries,
2930 there has been limited report that systematically described national progress on school closure, online opening, and off-line opening with an epidemiological analysis based on all the reported numbers of the total national pediatric population.
Of note, Korea had the second wave of a large outbreak in mid-August and mid-September, which caused the school opening delay at the end of summer vacation and transient school closure. However, this time, G12 students continued to go to school, and the school opened again for off-line (in-person) classes within one month. This was quite different from March to May situation when the school reopened again after 72 days for all students. The pediatric proportion of all confirmed cases remained stable, and most of all, there were no school-related outbreaks that led the nation-wide school closure again.
In conclusion, Korea had a successful transition from school closure to re-opening for online and off-line (in-person) classes with various efforts to keep our pediatric population safe while they attend the school during COVID-19 pandemic. More information will be needed on whether, compared to adults, children are less susceptible to SARS-CoV-2 when exposed, or less capable of transmitting the virus to others when they are the primary cases. Impact of school opening in various epidemiological situation in the community (low level vs. high-level transmission) needs to be carefully examined with the degree of adherence to the school guideline related to COVID-19.




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download