INTRODUCTION
MATERIALS AND METHODS
Data collection
Laboratory tests and analytical methods
Comparison of test methods
Data analysis and reference interval determination
RESULTS
Hematology
Table 1
| Analyte (unit) | Total N | Age | Sex | N | Lower limit (90% CI) | Upper limit (90% CI) |
|---|---|---|---|---|---|---|
| WBC (× 109/L) | 385 | 0–3 mo | M | 17 | 6.48 (4.74–8.10) | 16.30 (14.52–17.68) |
| F | 17 | 5.78 (4.12–7.66) | 15.80 (14.05–17.00) | |||
| 4–11 mo | Both | 67 | 4.64 (3.78–5.42) | 13.85 (12.98–14.77) | ||
| 1–6 yr | Both | 138 | 4.85 (4,62–5,60) | 11.50 (11.09–11.90) | ||
| 7–18 yr | Both | 146 | 4,32 (2,72–4,62) | 10.22 (9.57–10.20) | ||
| ANC (× 109/L) | 383 | 0–11 mo | Both | 97 | 0.65* (N/A) | 3.35* (N/A) |
| 1–18 yr | Both | 286 | 1.40 (1.22–1.51) | 5.76 (5.42–5.96) | ||
| Segmented neutrophils (%) | 393 | 0–11 mo | Both | 101 | 3.3 (1.1–5.5) | 33.1 (30.1–35.6) |
| 1–6 yr | Both | 147 | 16.9 (12.8–19.0) | 62.2 (56.3–65.6) | ||
| 7–12 yr | Both | 46 | 28.4 (25.1–32.2) | 64.5 (60.5–68.3) | ||
| 13–18 yr | Both | 99 | 38.3 (36.4–40.3) | 67.7 (65.6–69.8) | ||
| Lymphocytes (%) | 391 | 0–11 mo | Both | 100 | 54.5 (52.0–57.6) | 87.6 (85.2–89.8) |
| 1–6 yr | Both | 147 | 26.9 (24.9–35.1) | 73.8 (72.6–77.5) | ||
| 7–12 yr | Both | 45 | 29.4 (26.2–32.8) | 59.3 (56.3–62.0) | ||
| 13–18 yr | Both | 99 | 21.5 (19.3–23.6) | 51.5 (49.5–53.6) | ||
| Monocytes (%) | 387 | All | Both | 387 | 3.5 (3.0–3.7) | 10.4 (10.0–10.7) |
| Eosinophils (%) | 375 | All | M | 181 | 0.3 (0.1–0.7) | 6.9 (6.4–7.3) |
| F | 194 | 0.4 (0.1–0.7) | 5.7 (4.9–5.9) | |||
| Basophils (%) | 380 | All | Both | 380 | 0.1 (0.1–0.1) | 0.8 (0.8–0.9) |
| RBC (× 106/µL) | 390 | 0–3 mo | Both | 32 | 3.22 (3.07–3.41) | 4.65 (4.44–4.82) |
| 4 mo–18 yr | M | 174 | 4.16 (4.09–4.29) | 5.49 (5.30–5.62) | ||
| F | 184 | 4.03 (3.86–4.10) | 5.16 (5.03–5.29) | |||
| MCV (fL) | 395 | 0–3 mo | Both | 35 | 73.9 (71.2–76.6) | 98.3 (95.2–100.9) |
| 4–11 mo | M | 34 | 68.6 (66.9–70.6) | 82.8 (81.0–84.5) | ||
| F | 35 | 70.8 (69.1–72.5) | 84.6 (82.8–86.2) | |||
| 1–6 yr | M | 73 | 72.3 (71.5–73.2) | 83.4 (82.5–84.3) | ||
| F | 72 | 73.9 (72.8–75.0) | 86.1 (85.2–87.0) | |||
| 7–12 yr | M | 22 | 74.7 (73.1–76.6) | 87.8 (85.7–89.8) | ||
| F | 26 | 78.3 (77.0–79.9) | 89.0 (87.6–90.3) | |||
| 13–15 yr | M | 27 | 76.4 (74.3–78.7) | 93.3 (91.1–95.3) | ||
| F | 35 | 80.5 (79.0–82.1) | 94.3 (92.6–96.0) | |||
| 16–18 yr | M | 18 | 80.3 (78.3–82.6) | 95.2 (92.4–97.8) | ||
| F | 18 | 83.4 (81.6–85.6) | 95.9 (93.9–97.5) | |||
| MCH (pg) | 390 | 0–3 mo | Both | 35 | 25.3 (24.4–26.4) | 33.7 (32.7–34.6) |
| 4–11 mo | M | 32 | 23.5 (22.8–24.2) | 28.6 (28.0–29.2) | ||
| F | 31 | 24.9 (24.5–25.4) | 28.2 (27.9–28.5) | |||
| 1–6 yr | Both | 146 | 24.6 (24.3–25.2) | 29.1 (28.8–29.3) | ||
| 7–12 yr | Both | 48 | 26.4 (26.0–26.7) | 30.4 (29.9–30.8) | ||
| 13–15 yr | Both | 62 | 26.4 (25.8–26.9) | 32.2 (31.7–32.7) | ||
| 16–18 yr | Both | 36 | 28.0 (27.5–28.6) | 32.3 (31.8–32.8) | ||
| MCHC (g/L) | 386 | 0–12 yr | Both | 298 | 327 (325–329) | 359 (357–364) |
| 13–18 yr | M | 44 | 325 (322–328) | 357 (354–360) | ||
| F | 44 | 323 (321–326) | 343 (341–345) | |||
| Hb (g/L) | 393 | 0–3 mo | Both | 33 | 97 (92–101) | 134 (128–140) |
| 4 mo–6 yr | Both | 214 | 108 (107–111) | 140 (138–143) | ||
| 7–12 yr | M | 23 | 117† (112–123) | 154† (148–159) | ||
| F | 25 | 115 (110–120) | 148 (143–152) | |||
| 13–15 yr | M | 27 | 124 (119–129) | 164 (158–169) | ||
| F | 34 | 118 (114–122) | 150 (146–152) | |||
| 16–18 yr | M | 18 | 138† (132–143) | 170† (164–176) | ||
| F | 19 | 119† (114–123) | 146† (141–151) | |||
| Hct (proportion of 1.0) | 380 | 0–3 mo | Both | 27 | 0.31 (0.30–0.31) | 0.36 (0.36–0.37) |
| 4 mo–6 yr | Both | 211 | 0.33 (0.32–0.33) | 0.40 (0.39–0.41) | ||
| 7–12 yr | Both | 48 | 0.34 (0.34–0.35) | 0.43 (0.42–0.44) | ||
| 13–15 yr | M | 27 | 0.36 (0.34–0.37) | 0.48 (0.46–0.50) | ||
| F | 34 | 0.36 (0.35–0.37) | 0.44 (0.43–0.45) | |||
| 16–18 yr | M | 18 | 0.40 (0.39–0.42) | 0.50 (0.49–0.52) | ||
| F | 15 | 0.36† (0.35–0.37) | 0.42† (0.41–0.43) | |||
| RDW (%) | 390 | 0–3 mo | Both | 35 | 11.7 (11.2–12.2) | 16.3 (15.7–16.8) |
| 4 mo–6 yr | M | 105 | 12.0 (11.8–12.1) | 14.4 (14.2–14.6) | ||
| F | 106 | 11.7 (11.5–11.9) | 14.1 (13.9–14.3) | |||
| 7–18 yr | Both | 144 | 11.7 (11.3–11.9) | 13.8 (13.6–13.8) | ||
| ESR (mm/hr) | 225 | All | Both | 225 | 2 (2–2) | 9 (8–9) |
| Platelets (× 109/L) | 390 | 0–3 mo | Both | 35 | 188 (143–243) | 610 (558–663) |
| 4–11 mo | Both | 65 | 199 (174–224) | 495 (467–520) | ||
| 1–12 yr | Both | 192 | 178 (171–192) | 414 (389–434) | ||
| 13–18 yr | Both | 98 | 165 (151–179) | 365 (351–379) | ||
| PCT (%) | 390 | 0–11 mo | Both | 102 | 0.17 (0.15–0.19) | 0.52 (0.49–0.54) |
| 1–18 yr | Both | 288 | 0.17 (0.15–0.18) | 0.38 (0.36–0.39) | ||
| MPV (fL) | 373 | 0–6 yr | Both | 236 | 7.6 (7.5–8.0) | 10.9 (10.5–11.1) |
| 7–18 yr | Both | 137 | 8.8 (8.6–9.1) | 11.4 (11.1–11.8) | ||
| PDW (%) | 358 | All | Both | 358 | 8.4 (8.1–8.6) | 13.3 (12.9–13.7) |
*Although the sample size was <120, the values presented were established using a nonparametric method because the 90% CI of the reference lower limit calculated using the robust method contained a negative value and the data did not pass a normality test; †The 90% CI was not determined using the robust method; however, the data passed a normality test and a parametric method based on the normal distribution was applied.
Abbreviations: CI, confidence interval; N/A, not applicable; yr, year; mo, month; M, male; F, female; ANC, absolute neutrophil count; MCH, mean corpuscular hemoglobin; MCHC, mean corpuscular hemoglobin concentration; RDW, red cell distribution width; PCT, plateletcrit; MPV, mean platelet volume; PDW, platelet distribution width; WBC, white blood cells; RBC, red blood cells; MCV, mean corpuscular volume; ESR, erythrocyte sedimentation rate; Hct, hematocrit.
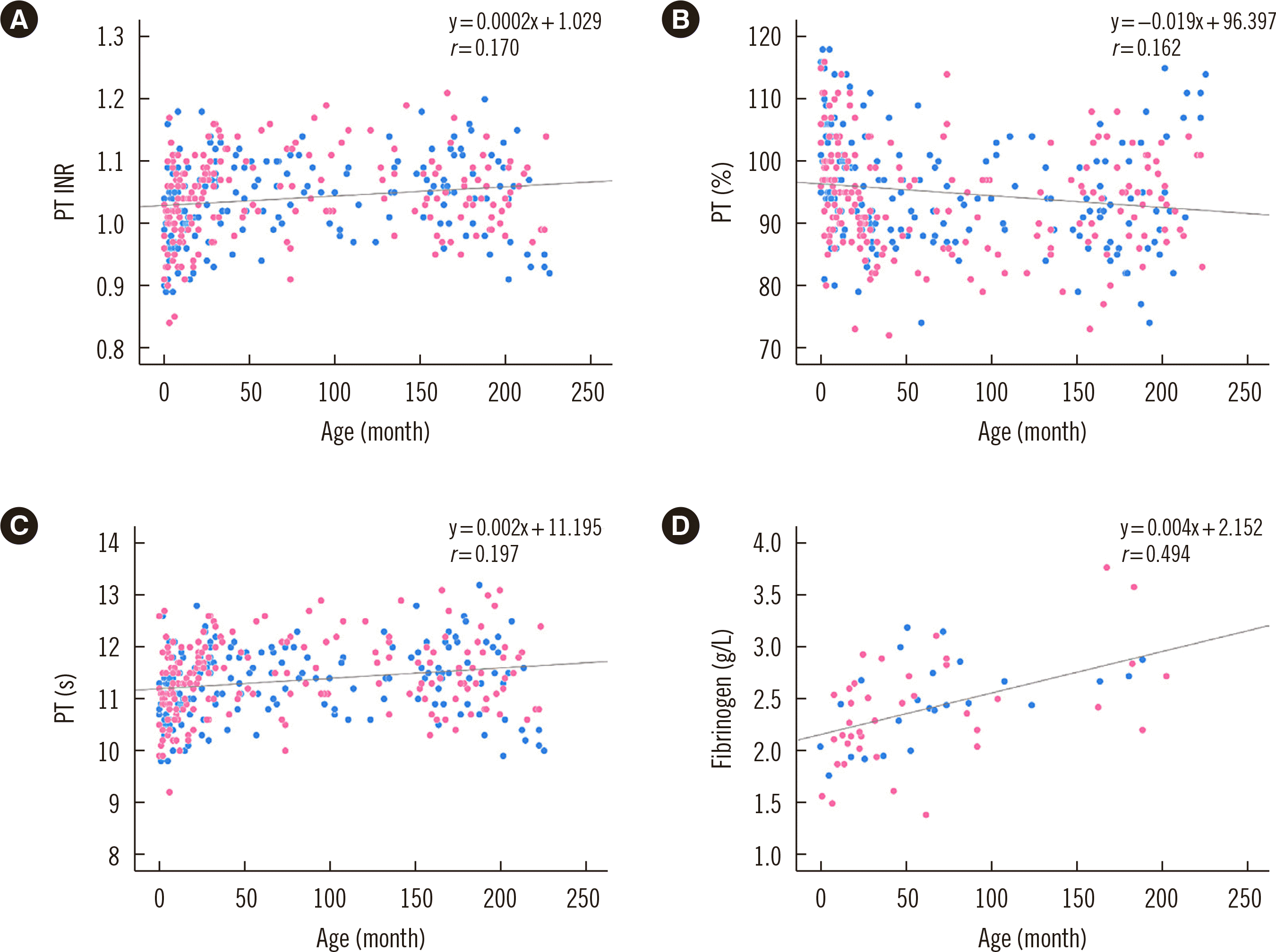
Coagulation
Table 2
| Analyte (unit) | Total N | Age | Sex | N | Lower limit (90% CI) | Upper limit (90% CI) |
|---|---|---|---|---|---|---|
| PT INR | 389 | 0–11 mo | Both | 102 | 0.87 (0.85–0.89) | 1.14 (1.12–1.16) |
| 1–18 yr | Both | 287 | 0.93 (0.91–0.94) | 1.17 (1.15–1.19) | ||
| PT (%) | 392 | 0–11 mo | Both | 100 | 82 (79–84) | 117 (114–120) |
| 1–18 yr | Both | 292 | 78 (73–81) | 111 (109–114) | ||
| PT (s) | 387 | 0–11 mo | Both | 100 | 9.6 (9.4–9.8) | 12.3 (12.1–12.5) |
| 1–18 yr | Both | 287 | 10.1 (10.0–10.3) | 12.8 (12.6–13.1) | ||
| aPTT (s) | 383 | All | Both | 383 | 28.3 (27.5–29.0) | 41.3 (40.8–41.7) |
| Fibrinogen (g/dL) | 67 | 0–12 yr | Both | 56 | 1.46 (1.31–1.63) | 3.21 (3.04–3.35) |
| 13–18 yr | Both | 11 | 1.96* (1.54–2.37) | 3.79* (3.38–4.21) |
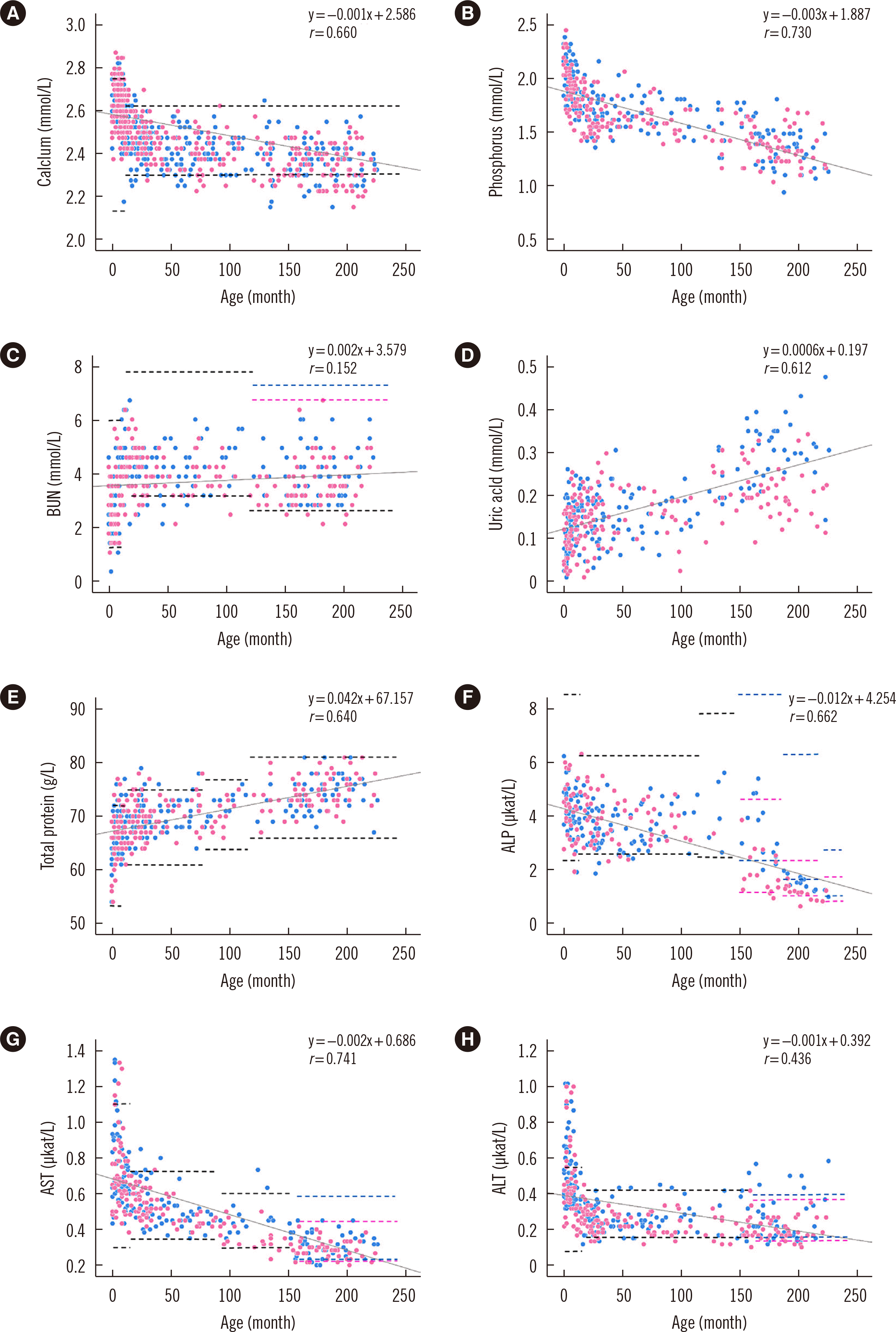
Chemistry
Table 3
| Analyte (unit) | Total N | Age | Sex | This study | Severance Hospital [15] | CALIPER [8] | ||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
|
|
|
||||||||||
| N | Lower limit (90% CI) | Upper limit (90% CI) | Age | Lower limit | Upper limit | Age‡ | Lower limit | Upper limit | ||||
| Calcium (mmol/L) | 387 | 0–11 mo | Both | 101 | 2.44 (2.41–2.47) | 2.85 (2.82–2.87) | 0–1 yr | 2.13 | 2.75 | |||
| 1–6 yr | Both | 143 | 2.28 (2.23–2.33) | 2.61 (2.60–2.70) | 1–19 yr | 2.30 | 2.63 | |||||
| 7–18 yr | Both | 143 | 2.23 (2.20–2.25) | 2.53 (2.48–2.53) | ||||||||
| Multicenter combined (T+C+H) | 780 | 0–11 mo | Both | 270 | 2.43 (2.40–2.48) | 2.81 (2.80–2.85) | ||||||
| 1–6 yr | Both | 280 | 2.28 (2.25–2.30) | 2.67 (2.63–2.70) | ||||||||
| 7–18 yr | Both | 230 | 2.20 (2.15–2.23) | 2.58 (2.55–2.63) | ||||||||
| Phosphorus (mmol/L) | 390 | 0–3 mo | Both | 32 | 1.74 (1.63–1.85) | 2.54 (2.45–2.61) | M: 2–16 yr | 1.23 | 1.91 | |||
| 4–11 mo | Both | 68 | 1.57 (1.51–1.63) | 2.29 (2.23–2.35) | F: 2–14 yr | 1.26 | 1.87 | |||||
| 1–6 yr | Both | 147 | 1.42 (1.26–1.45) | 2.07 (2.00–2.16) | ||||||||
| 7–12 yr | M | 23 | 1.26 (1.16–1.41) | 2.02 (1.92–2.15) | ||||||||
| F | 23 | 1.15*(1.05–1.25) | 1.80* (1.70–1.91) | |||||||||
| 13–18 yr | Both | 97 | 1.01 (0.96–1.06) | 1.73 (1.67–1.78) | ||||||||
| Glucose (mmol/L) | 377 | All | Both | 377 | 4.38 (4.11–4.44) | 6.44 (6.33–6.49) | M: 2–16 yr | 4.16 | 6.49 | |||
| Multicenter combined (T+C) | 655 | All | Both | 655 | 4.38 (4.16–4.50) | 6.42 (6.33–6.49) | F: 2–14 yr | 4.11 | 6.72 | |||
| BUN (mg/dL) | 396 | 0–11 mo | Both | 101 | 0.40 (0.11–0.70) | 5.17 (4.85–5.61) | 0–14 d | 1.00 | 8.21 | |||
| 1–18 yr | Both | 295 | 2.28 (2.14–2.50) | 6.07 (6.07–6.43) | 15 d–1 yr | 1.21 | 6.00 | |||||
| 1–10 yr | 3.21 | 7.89 | ||||||||||
| 10–19 yr | M: 2.61, F: 2.61 M: | 7.50, F: 6.78 | ||||||||||
| Uric acid (mmol/L) | 357 | 0–3 mo | Both | 33 | 0.08 (0.06–0.10) | 0.25 (0.23–0.27) | M: 2–10 yr | 0.15 | 0.35 | |||
| 4 mo–6 yr | Both | 204 | 0.12 (0.11–0.14) | 0.30 (0.29–0.34) | M: 11–16 yr | 0.18 | 0.45 | |||||
| 7–12 yr | M | 21 | 0.16 (0.14–0.19) | 0.37 (0.33–0.40) | F: 2–14 yr | 0.15 | 0.35 | |||||
| F | 25 | 0.12 (0.09–0.15) | 0.37 (0.33–0.40) | |||||||||
| 13–18 yr | M | 34 | 0.23 (0.21–0.27) | 0.46 (0.43–0.49) | ||||||||
| F | 40 | 0.16 (0.14–0.18) | 0.36 (0.34–0.39) | |||||||||
| Cholesterol (mmol/L) | 388 | All | Both | 388 | 2.95 (2.82–3.06) | 5.64 (5.46–5.83) | M: 2–16 yr | 3.16 | 5.41 | 0–14 d | M: 1.09, F: 1.19 M: | 2.82, F: 3.24 |
| Multicenter combined (T+H) | 489 | All | Both | 489 | 2.90 (2.82–3.03) | 5.72 (5.52–5.85) | F: 2–14 yr | 3.32 | 5.46 | 15 d–1 yr | 1.66 | 6.14 |
| 1–19 yr | 2.90 | 5.39 | ||||||||||
| Total Protein (g/L) | 389 | 0–3 mo | Both | 32 | 53.6 (51.1–56.4) | 75.0 (72.4–77.2) | M: 2–5 yr | 61 | 74 | 0–14 d | 53 | 83 |
| 4–11 mo | Both | 70 | 58.5 (57.0–59.7) | 74.7 (73.0–76.2) | M: 6–16 yr | 63 | 77 | 15 d–1 yr | 44 | 71 | ||
| 1–6 yr | Both | 147 | 64.0 (61.0–64.0) | 78.0 (76.0–79.0) | F: 2–14 yr | 63 | 77 | 1–6 yr | 61 | 75 | ||
| 7–12 yr | M | 20 | 68.5* (67.2–69.8) | 76.2* (74.9–77.5) | 6–9 yr | 64 | 77 | |||||
| F | 25 | 65.0* (63.0–67.0) | 78.8* (76.7–80.8) | 9–19 yr | 65 | 81 | ||||||
| 13–18 yr | Both | 95 | 68.7 (67.8–69.6) | 80.9 (80.1–81.8) | ||||||||
| Albumin§ (g/L) | 394 | All | Both | 394 | 40 (39–41) | 50 (50–51) | M: 2–16 yr | 40 | 49 | 0–14 d | 33 | 45 |
| F: 2–14 yr | 40 | 49 | 15 d–1 yr | 28 | 47 | |||||||
| 1–8 yr | 38 | 47 | ||||||||||
| 8–15 yr | 41 | 48 | ||||||||||
| 15–19 yr | M: 41, F: 40 | M: 51, F: 49 | ||||||||||
| Total bilirubin (µmol/L) | 367 | All | Both | 367 | 3.4 (3.4–3.4) | 13.7 (13.7–13.7) | M: 2–8 yr | 3.4 | 13.7 | 0–14 d | 3.2 | 283.9 |
| M: 9–16 yr | 3.4 | 17.1 | 15 d –1 yr | 0.9 | 11.6 | |||||||
| F: 2– 9 yr | 3.4 | 13.7 | 1–9 yr | 0.9 | 6.8 | |||||||
| F: 10–14 yr | 3.4 | 17.1 | 9–12 yr | 0.9 | 9.4 | |||||||
| 12–15 yr | 1.7 | 12.0 | ||||||||||
| 15–19 yr | 1.7 | 14.4 | ||||||||||
| ALP (µkat/L) | 268 | 0–12 yr | Both | 212 | 2.01 (1.64–2.47) | 5.75 (5.46–6.20) | M: 2–5 yr | 1.77 | 4.35 | 0–14 d | 1.50 | 4.55 |
| 13–15 yr | M | 13 | 1.04* (0.08–2.00) | 5.66* (4.71–6.62) | M: 6–14 yr | 1.97 | 5.68 | 15 d–1 yr | 2.23 | 8.63 | ||
| F | 17 | 0.92† (N/A) | 2.76† (N/A) | M: 15–16 yr | 1.03 | 4.17 | 1–10 yr | 2.60 | 6.15 | |||
| 16–18 yr | M | 13 | 0.96* (0.76–1.15) | 1.89* (1.69–2.08) | F: 2–5 yr | 1.95 | 4.35 | 10–13 yr | 2.35 | 7.67 | ||
| F | 13 | 0.57* (0.35–0.78) | 1.61* (1.39–1.82) | F: 6–12 yr | 2.05 | 5.50 | 13–15 yr | M: 2.12, F: 1.03 | M: 8.62, F: 4.67 | |||
| F: 13–14 yr | 1.02 | 6.65 | 15–17 yr | M: 1.48, F: 0.90 | M: 6.08, F: 2.13 | |||||||
| 17–19 yr | M: 0.98, F: 0.80 | M: 2.73, F: 1.58 | ||||||||||
| AST (GOT) (µkat/L) | 376 | 0–11 mo | Both | 97 | 0.25 (0.19–0.33) | 1.15 (1.07–1.24) | M: 2–16 yr | 0.25 | 0.65 | 0–14 d | 0.53 | 2.70 |
| 1–6 yr | Both | 144 | 0.38 (0.35–0.40) | 0.80 (0.75–0.85) | F: 2–7 yr | 0.33 | 0.68 | 15 d–1 yr | 0.30 | 1.12 | ||
| 7–12 yr | M | 19 | 0.27* (0.21–0.33) | 0.63* (0.57–0.69) | F: 8–14 yr | 0.23 | 0.57 | 1–7 yr | 0.35 | 0.73 | ||
| F | 25 | 0.22* (0.17–0.26) | 0.51* (0.47–0.56) | 7–12 yr | 0.30 | 0.60 | ||||||
| 13–18 yr | Both | 91 | 0.17 (0.16–0.19) | 0.42 (0.39–0.43) | 12–19 yr | M: 0.23, F: 0.22 | M: 0.58, F: 0.43 | |||||
| ALT (GPT) (µkat/L) | 380 | 0–11 mo | Both | 98 | 0.23† (N/A) | 1.01† (N/A) | M: 2–16 yr | 0.13 | 0.65 | 0–1 yr | 0.08 | 0.55 |
| 1–18 yr | Both | 282 | 0.12 (0.12–0.13) | 0.45 (0.43–0.52) | F: 2–14 yr | 0.12 | 0.52 | 1–13 yr | 0.15 | 0.42 | ||
| 13–19 yr | M: 0.15, F: 0.13 | M: 0.40, F: 0.37 | ||||||||||
| Creatinine| (µmol/L) | 391 | 0–3 mo | Both | 33 | 13.4 (11.3–15.8) | 31.7 (29.7–34.2) | M: 2–5 yr | 19.4 | 49.5 | 0–14 d | 37.1 | 92.8 |
| 4–11 mo | Both | 69 | 18.5 (17.1–20.0) | 33.4 (32.3–34.8) | M: 6–9 yr | 28.3 | 61.9 | 15 d–1 yr | 28.3 | 46.9 | ||
| 1–6 yr | Both | 147 | 23.0 (18.6–23.9) | 46.5 (43.3–47.1) | M: 10–12 yr | 34.5 | 70.7 | 1–4 yr | 33.6 | 47.7 | ||
| 7–12 yr | Both | 48 | 30.2 (27.4–33.5) | 66.2 (62.0–70.0) | M: 13–16 yr | 39.8 | 86.6 | 4–7 yr | 38.9 | 56.6 | ||
| 13–15 yr | M | 27 | 38.7 (31.8–47.4) | 97.1 (89.4–104.3) | F: 2–5 yr | 18.6 | 46.9 | 7–12 yr | 46.0 | 61.0 | ||
| F | 30 | 44.4 (41.2–48.3) | 71.7 (68.1–75.7) | F: 6–8 yr | 28.3 | 56.6 | 12–15 yr | 50.4 | 70.7 | |||
| 16–18 yr | M | 18 | 61.7* (54.5–68.9) | 102.8* (95.6–110.0) | F: 9–14 yr | 32.7 | 63.6 | 15–17 yr | M: 58.3, F: 52.2 | M: 91.9, F: 76.0 | ||
| F | 19 | 48.9* (44.0–53.8) | 77.8* (72.9–82.7) | 17–19 yr | M: 61.0, F: 53.0 | M: 97.2, F: 77.8 | ||||||
| Na (mmol/L) | 392 | 0–6 yr | Both | 248 | 134 (133–134) | 141 (140–141) | ||||||
| 7–18 yr | Both | 144 | 136 (135–136) | 142 (142–143) | ||||||||
| Multicenter combined (T+C+A) | 909 | 0–3 mo | Both | 42 | 132 (131–133) | 142 (141–143) | ||||||
| 4 mo–6 yr | Both | 603 | 135 (135–136) | 143 (142–143) | ||||||||
| 7–18 yr | Both | 264 | 136 (135–136) | 144 (143–144) | ||||||||
| K (mmol/L) | 389 | 0–3 mo | Both | 33 | 4.5 (4.2–4.7) | 6.3 (6.1–6.5) | ||||||
| 4–11 mo | Both | 67 | 4.1 (4.0–4.2) | 5.3 (5.2–5.4) | ||||||||
| 1–18 yr | Both | 289 | 3.7 (3.6–3.7) | 4.8 (4.7–4.9) | ||||||||
| Multicenter combined (T+C+A) | 911 | 0–3 mo | M | 20 | 4.7* (4.4–4.9) | 6.2* (5.9–6.4) | ||||||
| F | 21 | 4.3* (4.0–4.6) | 6.2* (5.9–6.5) | |||||||||
| 4–11 mo | Both | 248 | 4.2 (4.0–4.3) | 5.4 (5.3–5.5) | ||||||||
| 1–18 yr | Both | 622 | 3.7 (3.7–3.8) | 5.0 (4.9–5.1) | ||||||||
| Cl (mmol/L) | 398 | All | Both | 398 | 100 (99–100) | 108 (108–109) | ||||||
| Multicenter combined (T+C+A) | 890 | All | Both | 890 | 101 (100–101) | 107 (107–108) | ||||||
| TCO2 (mmol/L) | 393 | 0–6 yr | Both | 248 | 17 (17–18) | 26 (26–28) | 0–14 d | 5 | 20 | |||
| 7–12 yr | Both | 47 | 21† (N/A) | 29† (N/A) | 15 d–1 yr | 10 | 24 | |||||
| 13–18 yr | Both | 98 | 21 (20–22) | 31 (30–32) | 1–5 yr | 14 | 24 | |||||
| 5–15 yr | 17 | 26 | ||||||||||
| 15–19 yr | M: 18, F: 17 | M: 28, F: 26 | ||||||||||
| CRP (mg/L) | 241 | All | Both | 241 | 0.10 (0.10–0.10) | 1.80 (1.70–2.30) | 0–14 d | 0.3 | 6.1 | |||
| 15 d–15 yr | 0.1 | 1.0 | ||||||||||
| 15–19 yr | 0.1 | 1.7 | ||||||||||
*The 90% CI was not determined using the robust method; however, the data passed a normality test and a parametric method based on the normal distribution was applied; †Although the sample size was <120, the values presented were established using a nonparametric method because the 90% CI calculated using the robust method contained a negative value; ‡Age-specific group for the CALIPER study described as “A-B” means equal to or older than A, and younger than B; §Albumin concentration was measured using a bromocresol green dye-binding assay (AlbBCG). |Creatinine was measured using the Jaffe reaction.
Abbreviations: CALIPER, Canadian laboratory initiative on pediatric reference interval database; T, TBA-c16000; C, Cobas 800; H, Hitachi 7600; d, day; mo, month; yr, year; A, AU 5800; BUN, blood urea nitrogen; ALP, alkaline phosphatase; AST, aspartate aminotransferase; GOT, glutamate oxaloacetate transaminase; ALT, alanine aminotransferase; GPT, glutamate pyruvate transaminase; TCO2, total CO2; CRP, C-reactive protein.
Fig. 1
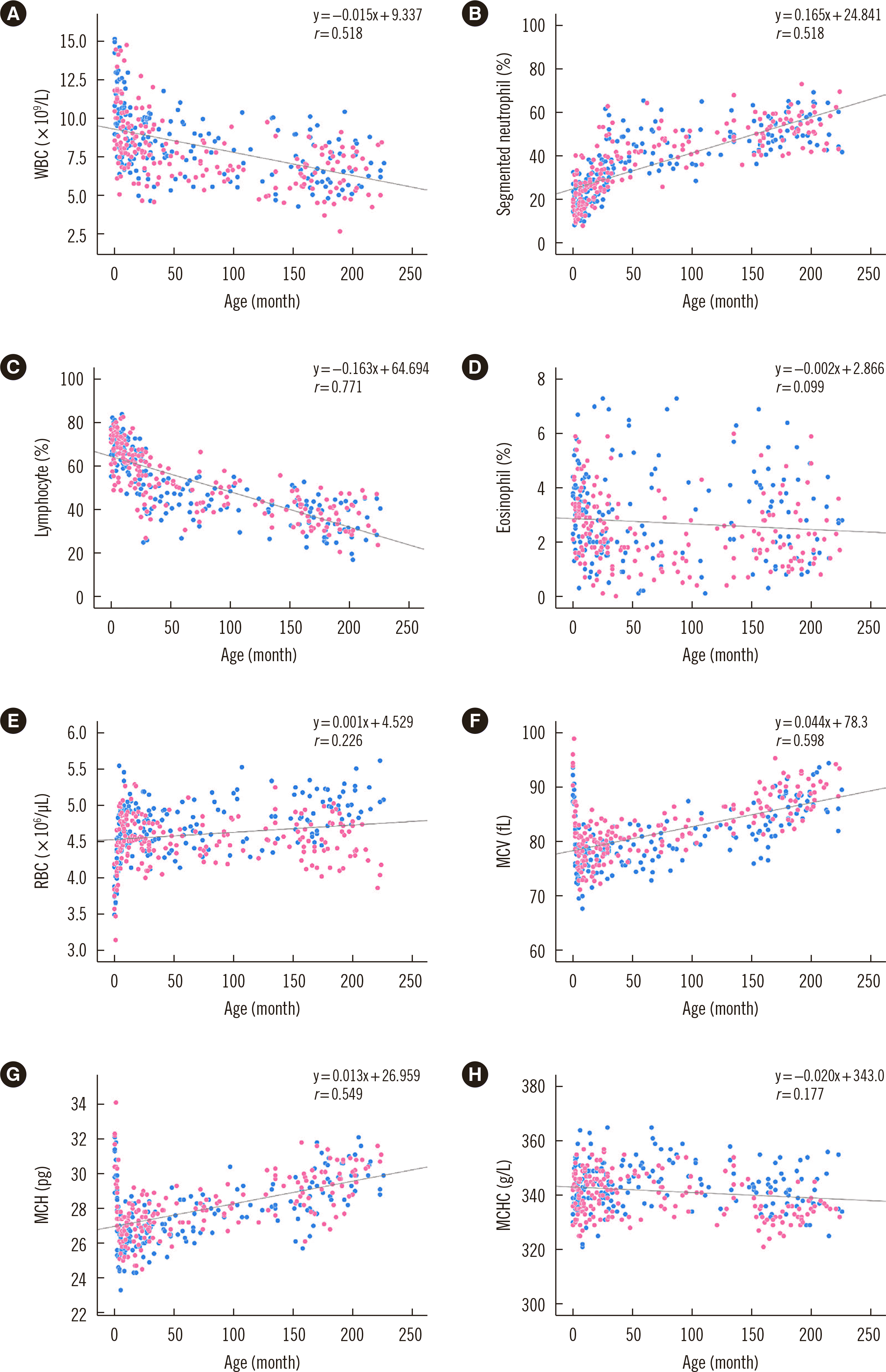
Fig. 3
DISCUSSION
Fig. 2




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download