INTRODUCTION
MATERIALS AND METHODS
Embolization technique
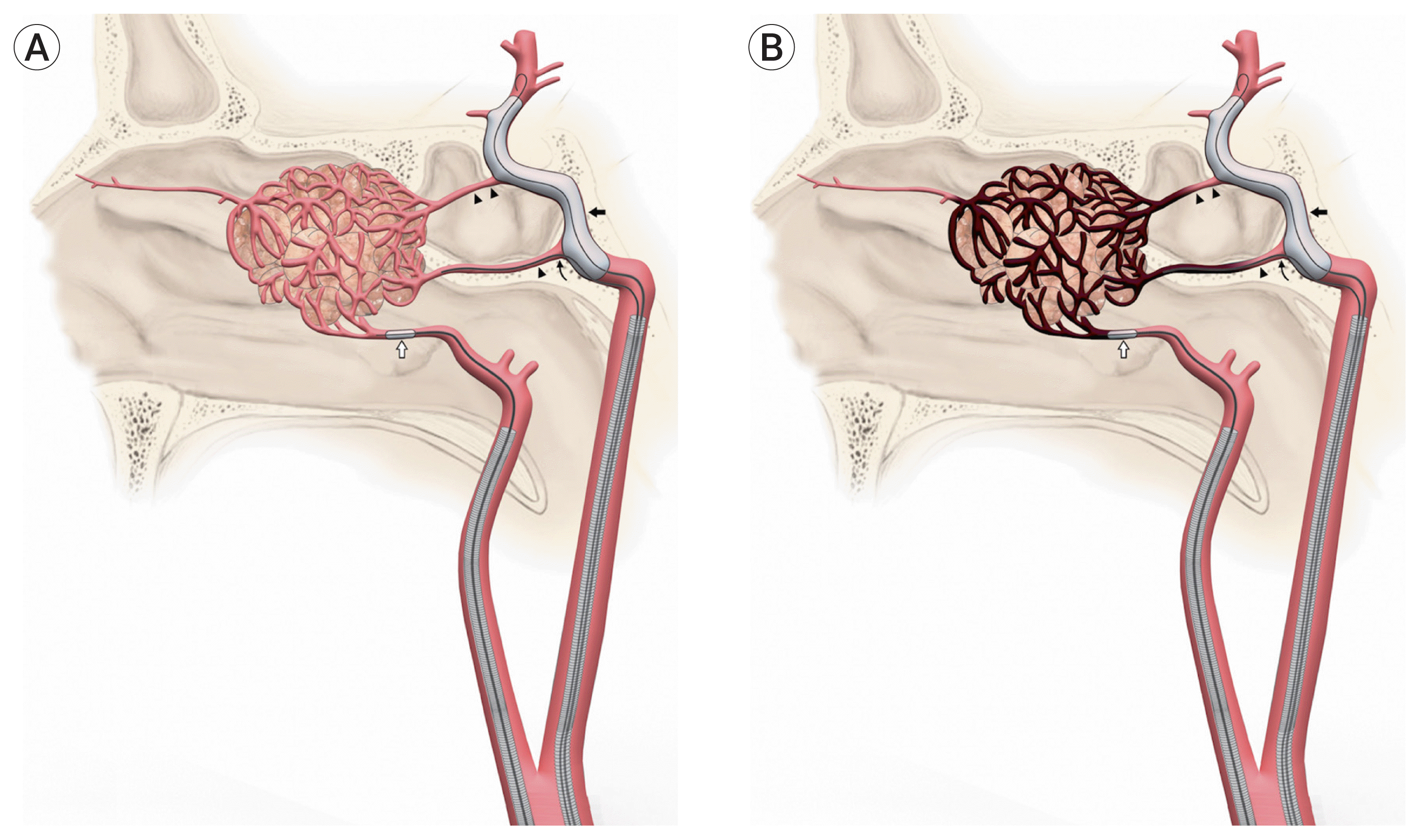 | Fig. 1Illustration demonstrating example of catheter and balloon placement prior to (A) and after (B) infusion of Onyx in tumor feeders resulting in complete embolization of tumor vasculature. Black arrow: The 5×30 mm Hyperglide™ balloon in the ICA is inflated, thus protecting the C2-C4 segments of the ICA and their branches (single, double arrow heads). White arrow: Scepter™ balloon is inflated in ECA for selective Onyx-34 injection. Curved arrow: Duo™ microcatheter loaded with an 0.10 microwire to be inserted into arterial feeder of interest using the proximal end of balloon to assist in guiding wire into arterial trunk. ICA, internal carotid artery; ECA, external carotid artery. |
RESULTS
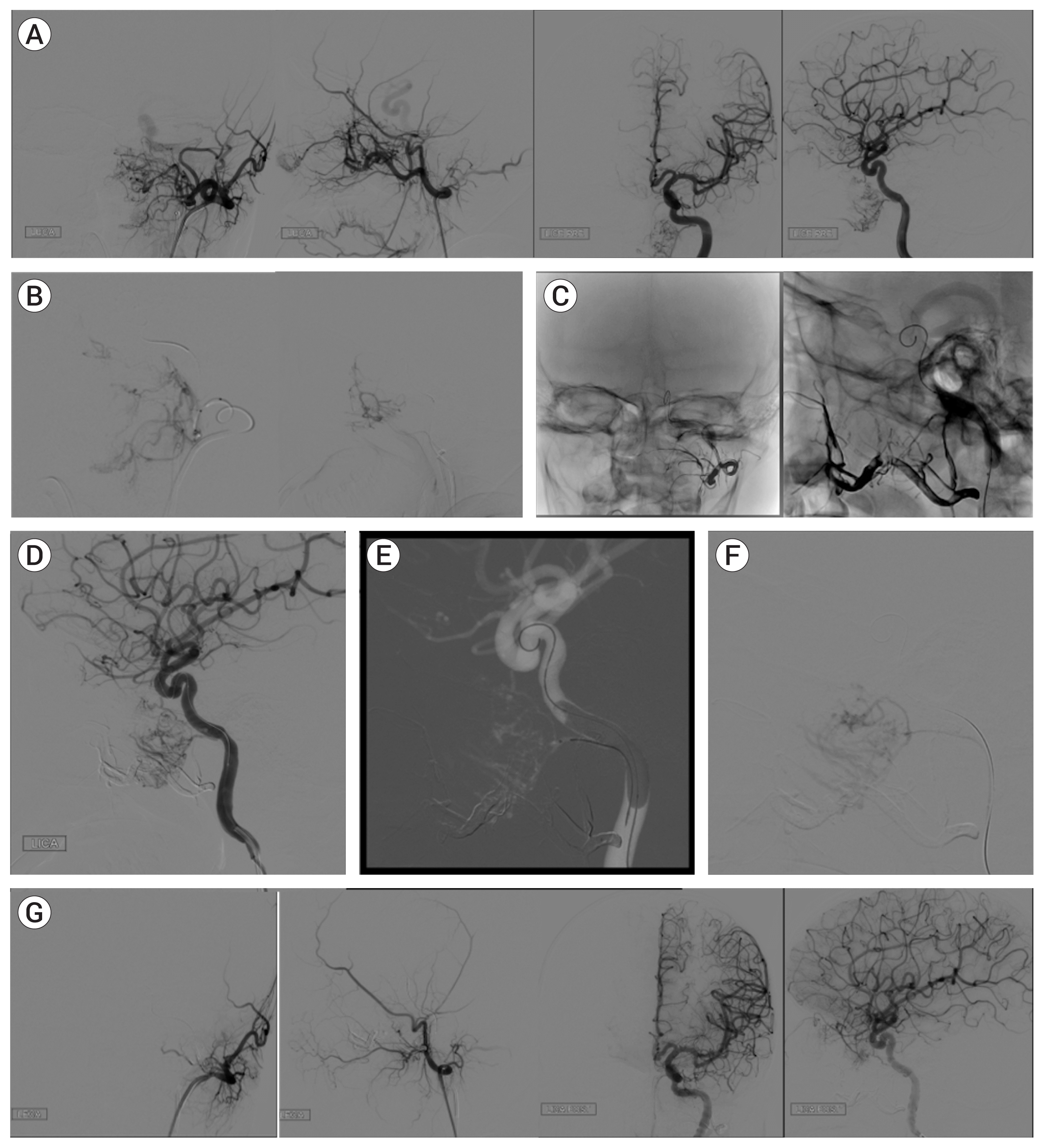 | Fig. 2Demonstrative case, Part 1: (A) Pre-embolization subtracted angiogram of left ICA and left ECA circulations (coronal and sagittal views) shows a large left posterior nasal cavity tumor measuring 43.5 mm×44.1 mm×55.7 mm with a blood supply from distal branches of the left sphenopalatine artery, left accessory meningeal artery, left middle meningeal artery, left inferior lateral trunk, and left vidian artery. (B) Embolization of ECA feeders (balloon inflated but not visualized). (C) Unsubtracted angiogram showing Onyx cast with evidence of deep penetration to peripheral feeders. (D) Subtracted angiogram of ICA after ECA embolization shows persistent vascularization supplied by vidian artery. (E) Roadmap showing microcatheter in distal vidian artery protected by balloon. (F) Embolization of Vidian artery feeders under balloon protection. (G) Post-embolization subtracted angiogram shows reduction of tumor blush by >90%. ICA, internal carotid artery; ECA, external carotid artery. |
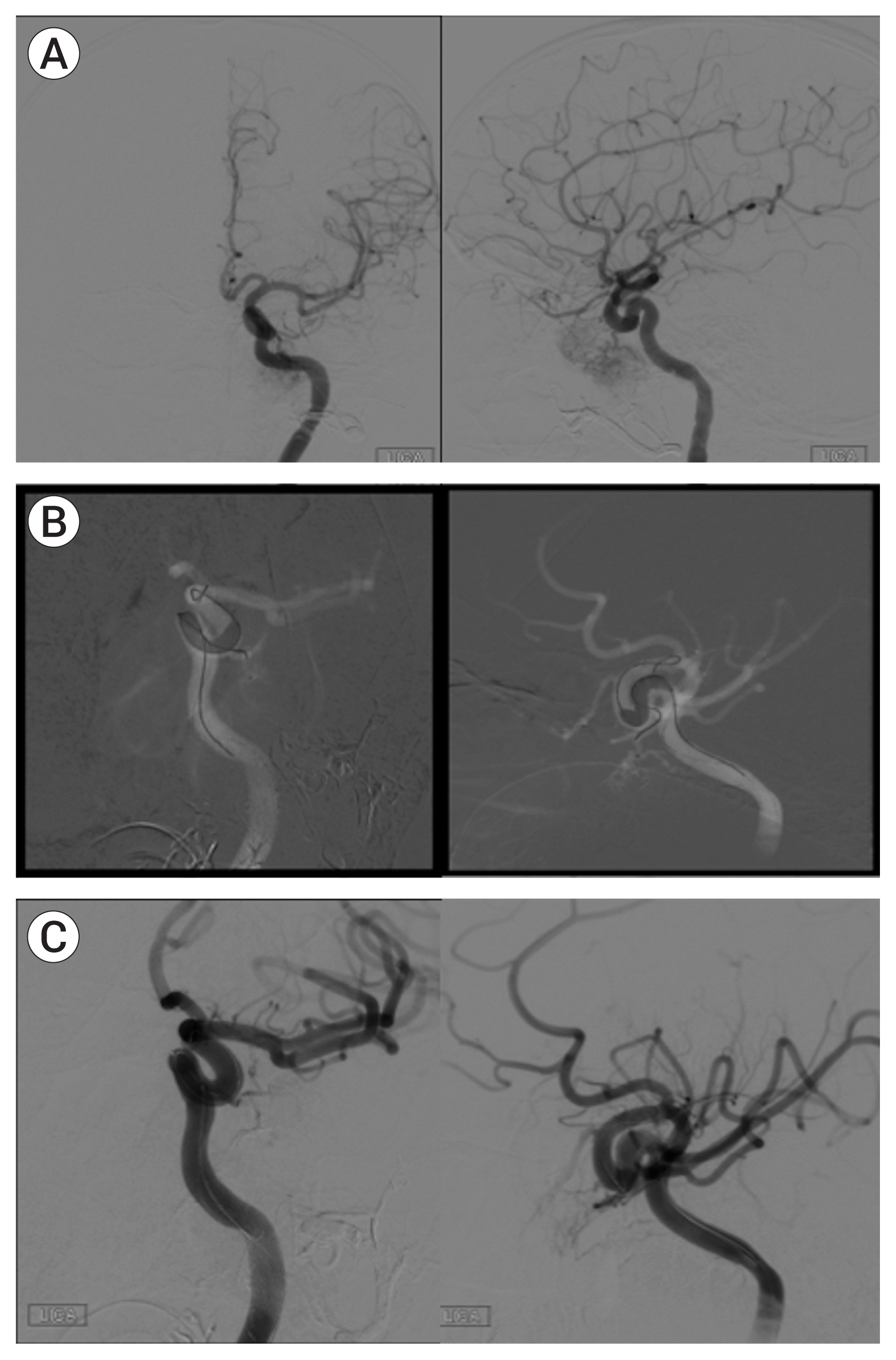 | Fig. 3Demonstrative case, Part 2: (A) Pre-embolization subtracted angiogram after ICA injection demonstrates recurrent tumor supplied by inferior lateral trunk. (B) Roadmap showing placement of microcatheter in distal inferior lateral trunk with ICA balloon inflated for protection. (C) Post-embolization subtracted ICA injection shows blush reduction of 90% and abrupt cut-off of inferior lateral trunk flow to tumor. ICA, internal carotid artery. |




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download