This article has been
cited by other articles in ScienceCentral.
Abstract
Soft tissue and bone defect due to the machinery penetrating injury of elbow joint are a rare and challenging problem for reconstructive surgeons. After reconstructing soft tissue with anterolateral thigh (ALT) flap and external fixator, the authors planned restoration of elbow function using total elbow replacement (TER). Finally, the patient regained the soft tissue reconstruction and the motion of the elbow using TER, and satisfied with the clinical results. Therefore, the authors present the successful case of ALT flap and TER to treat the machinery penetrating the injury of the elbow.
Go to :

Keywords: Open fractures, Surgical flap, Elbow replacement arthroplasty
INTRODUCTION
Machinery penetrating injury of the elbow is a rare and challenging problem for reconstructive surgeons. In such cases, surgeons should consider functional recovery for the treatment of open fracture and bone loss as well as soft tissue reconstruction. The anterolateral thigh (ALT) flap is commonly used perforator free flap due to its versatility, ease of use, large size, and minimal donor site morbidity [
1]. Fractures of the distal humerus are best treated surgically by anatomical reduction and rigid internal fixation, and this is not impossible in severely comminuted fractures associated with soft tissue and bone defects [
2]. Total elbow replacement (TER) has presented as a reliable treatment option with satisfactory functional recovery for acute distal humeral comminuted fractures, distal humeral nonunion, and posttraumatic arthritis [
2,
3].
In this case, we treated the elbow joint that showed a comminuted fracture of the distal humerus with bone loss and soft tissue defects after the machinery penetrating injury with ALT flap and TER and report the result with a review of the literature.
This report was approved by the Institutional Review Board of Duson Hopital. Written informed consent for publication of the clinical images was obtained from the patient.
Go to :

CASE REPORT
A 58-year-old male patient showed a distal humeral bone-losing comminuted fracture with large penetrating soft tissue injury resulting from a high pressure injecting machinery accident. Soft tissue defect of both medial and lateral sides had a diameter of about 10 cm (
Fig. 1). He underwent emergency debridement of the wound, external fixation of the elbow joint was established and antibiotic cement block was inserted due to infection control of severely contaminated wound and prevent elbow contracture. Fortunately, radial, median, ulnar nerve, and the brachial artery was intact. Also, the triceps and biceps attachment was partially ruptured. However, there was a whole joint defect of distal humerus except for medial condyle and medial condyle was protecting ulnar nerve. Because of the above surgical findings, subsequent TER was therefore planned. Medial condyle was fixated with Steinmann pin and anterior transposition of the ulnar nerve was performed for subsequent TER (
Fig. 2). The medial side was approximated using bipedicle advancement flap to protect the ulnar nerve and the lateral side remained for ALT flap. Postoperative computed tomography angiogram was performed to evaluate the vasculature of the injured site and showed an intact brachial artery (
Fig. 3). Two weeks after the emergency surgery, the area of the lateral wound was demarcated and ALT flap was performed. With the identified two perforating arteries from the descending branch of the lateral cutaneous femoral artery (LCFA), a 15.0 × 10.0 cm-sized flap was designed to cover the defect of the lateral side. The pedicle was prepared for about 10 cm. To minimize the graft size, the donor site was approximated and a delayed split-thickness skin graft was planned. The profunda brachii artery was injured and used as a recipient artery. Vessel anastomoses were done by the end-to-end anastomosis between LCFA to recipient artery and end-to-end anastomosis between two vena comitantes to cephalic vein. The flap was placed according to the soft tissue defect and sutured (
Fig. 4). Three weeks after emergency surgery, the proximal pin of external fixator showed breakage; therefore, removal of the external fixator was performed and a hinged elbow brace was applied for a range of motion exercise. Two weeks later, infection markers such as erythrocyte sedimentation rate and C-reactive protein showed normal values and there was no indication of infection of the external wound. We performed TER with a semiconstrained type prosthesis (Coonrad Morrey System; Zimmer Biomet, Warsaw, IN, USA) (
Fig. 5). Lateral biased posterior approach was performed while protecting vascular pedicle by incision into the inferior boundary of the flap. One month after TER, the flap maintained stably without any complications, and the arc of flexion–extension was 0° to 110° and the arc of pronation–supination was 90° to 70°. At the latest follow-up, 1 year after the TER, he showed the same arc of motion. There was no radiological loosening, and there was a union of bone block in plain radiographs (
Fig. 6)
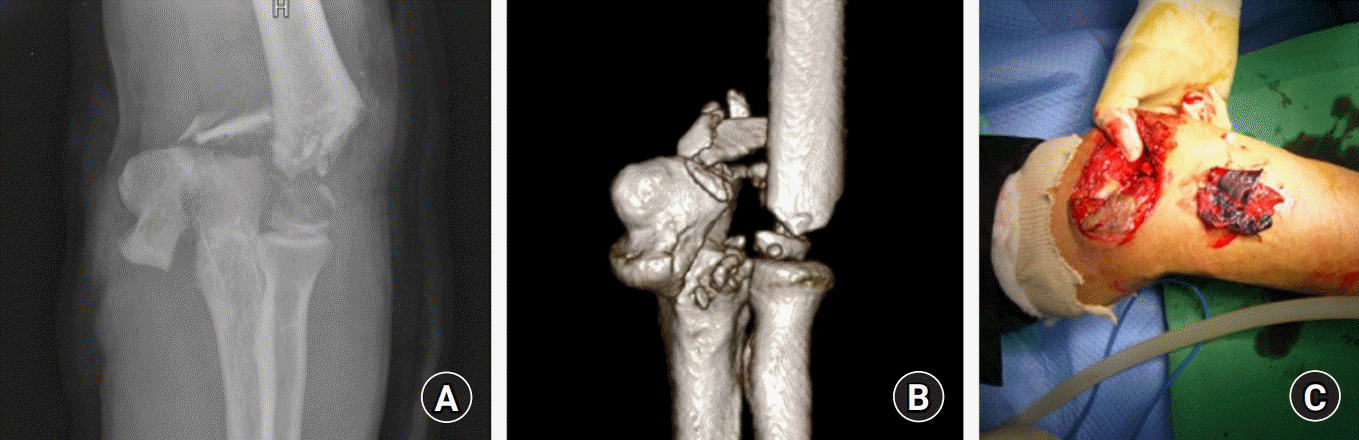 | Fig. 1.Plain radiograph (A) and computed tomography (B) showed a severely comminuted fracture of the distal humerus. (C) Penetrating injury showed both medial and lateral soft-tissue defect with severely contaminated status. Written informed consent for publication of the clinical images was obtained from the patient. 
|
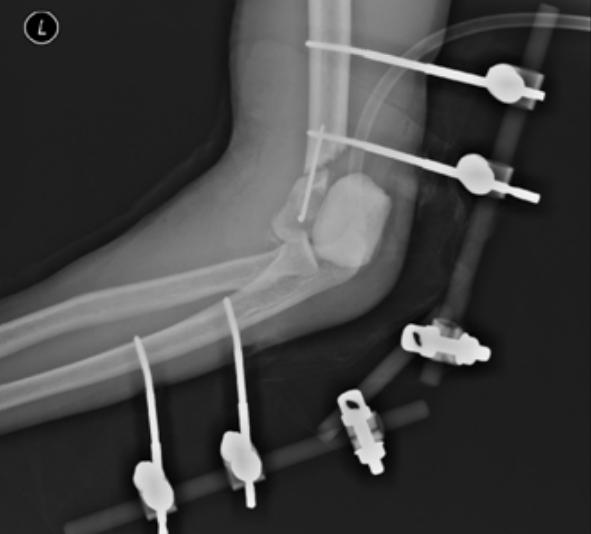 | Fig. 2.Postoperative radiograph showed external fixator with antibiotic cement block. Written informed consent for publication of the clinical images was obtained from the patient. 
|
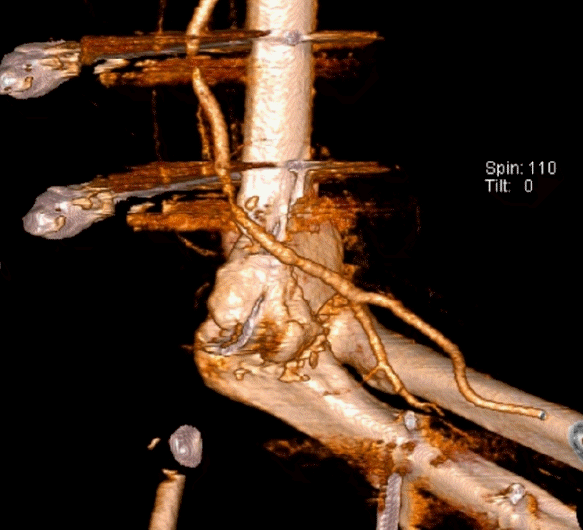 | Fig. 3.Postoperative computed tomography angiogram showed an intact brachial artery. Written informed consent for publication of the clinical images was obtained from the patient. 
|
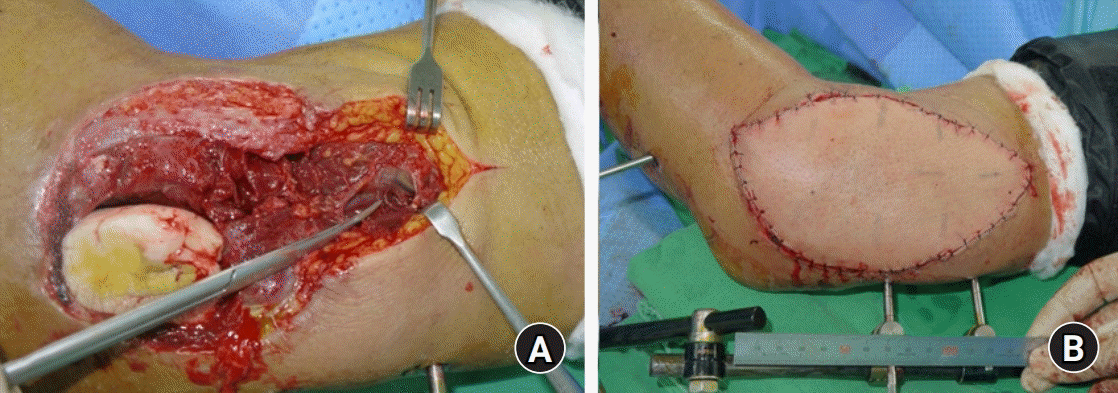 | Fig. 4.(A) Previously injured profunda brachii artery was used as a recipient artery. (B) Postoperative status of anterolateral thigh flap. Written informed consent for publication of their clinical images was obtained from the patient. 
|
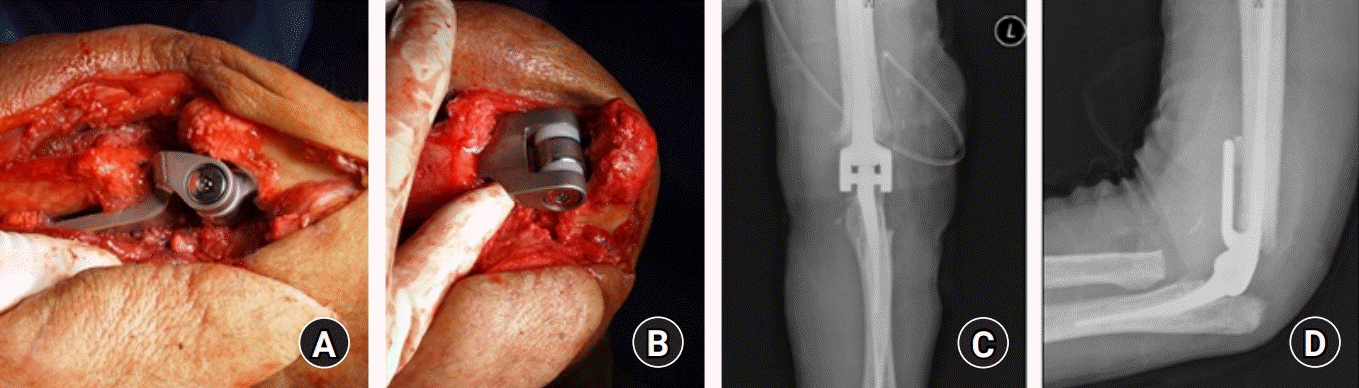 | Fig. 5.(A, B) Intraoperatively, posterolateral approach was utilized under the base of the ALT flap for total elbow replacement (TER). (C, D) Postoperative radiograph of TER. Written informed consent for publication of the clinical images was obtained from the patient. 
|
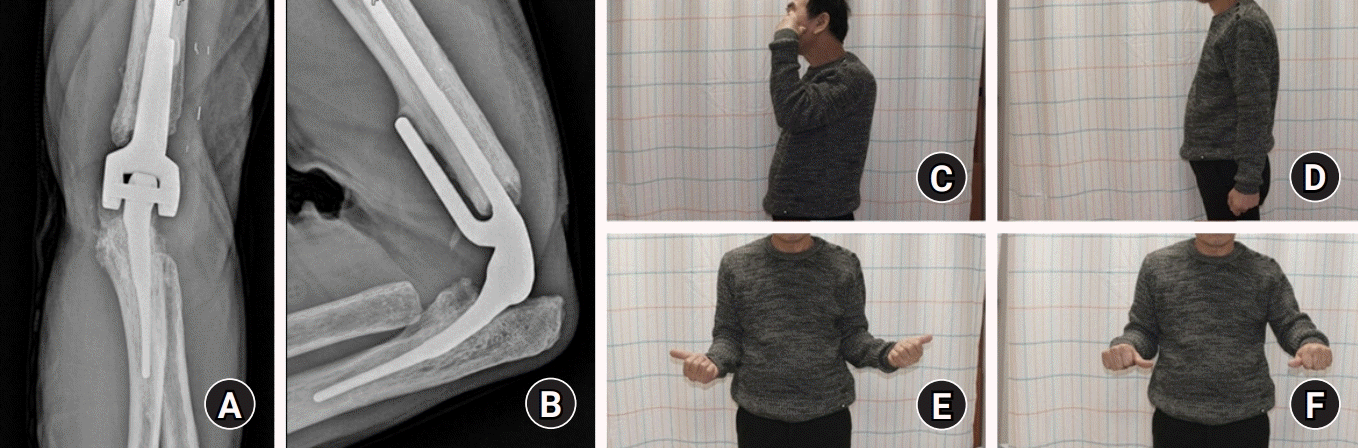 | Fig. 6.Radiological and clinical outcome at 1-year follow-up. (A, B) Plain radiographs showed no radiological loosening. (C, D) The arc of flexion–extension was 0° to 110°. (E, F) The arc of pronation–supination was 90° to 70°. Written informed consent for publication of the clinical images was obtained from the patient. 
|
Go to :

DISCUSSION
The perforator flap has recently been used mainly for the reconstruction of soft tissue defect of the upper extremity, allowing the use of free flap without significant arterial sacrifice, increasing the frequency of free flap [
4]. The advantages of ALT flap are known to be relatively low in anatomical variation, making it easier to elevate and relatively low in the morbidity of donor site [
5]. Also, the ALT flap can be designed in various shapes and can be used as a composite flap for the reconstruction of composite soft tissue defects [
4,
5]. So, the authors decided to use ALT flap and could consider one lateral flap or two separated medial and lateral flap for this penetrating injury. Finally, one lateral flap used and the medial defect was covered by bipedicle advancement flap for the protection of the ulnar nerve, and posterolateral approach was utilized under the base of the ALT flap for TER.
It is very difficult to determine the treatment policy in cases where the internal fixation is difficult due to severely comminuted fracture or in elderly patients with poor bone quality. In particular, the presence of comminuted fractures associated with severely contaminated wounds is more difficult to treat, and the complication rate is higher even if internal fixation is performed. Cobb and Morrey [
6] reported satisfactory results of twenty cases of primary TER for distal humeral fractures in elderly patients. In most studies, primary TER is considered in elderly patients; however, it is sometimes inevitable to primary TER because of an extensive bone loss associated with open comminuted fracture. Kim and Jung [
7] reported internal fixation was difficult with the treatment of severe comminuted distal humeral fractures, and they thought TER was one of the good alternatives even in younger patients. The semiconstrained linked TER provides long-lasting, satisfactory results; however, the longevity of TER is not proved yet and revision surgery is still a challenging problem [
8]. Therefore, surgeons should also consider methods to reduce complications and secondary surgical procedures for younger patients treated with TER, and it may require further study in the future.
In this presented case, ALT flap with TER was a challenging surgical procedure for the reconstruction of machinery penetrating injury of the elbow joint. There were some important technical points and originalities with satisfactory results. First, the authors considered subsequent TER in emergency surgery because of large bone loss except for medial condyle. Therefore, ALT flap was performed for soft tissue coverage, then TER was performed. The approach of TER was lateral sided over the original approach to perfume TER without the risk of damage to the vascular pedicle. Second, treatment of complex injury of the elbow joint using free flap coverage with TER is the rarely documented reconstruction of the elbow joint and the surgery resulted in early recovery of range of motion at 1-year follow-up.
This presented case has inherent considerations. The external fixator was used for the temporary process, but it was broken 3 weeks later. Therefore, In case of complex elbow fracture, it is thought that the use of a hinged brace from the initials for the early range of motion exercise can be considered in a favorable method [
9]. Hinge brace and hinged external fixator can be considered for complex fracture and dislocation of the elbow and it has the advantage of being able to prevent stiffness until subsequent surgery while maintaining a certain degree of stability [
9,
10]. Additionally, there will still be limitations in the long-term follow-up of TER; therefore, this treatment option may require further investigation in the future.
As described above, successful reconstruction of the elbow joint and soft tissue defect was possible using ALT flap and TER. Although there are limitations that require long-term follow-up of TER, it is certain that the result within 1 year obtained in our patient was encouraging and we believe that this technique offers early recovery.
Go to :











 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download