I. Introduction
II. Methods
1. Outcome
Part 1
Part 2
Table 1
2. Data Collection
Part 1
Part 2
III. Results
Part 1
- Factors 1, 3, and 7 in combination attributed to the “treating doctor”: It was observed that the discharge TAT varied significantly with different treating doctors.
- Factor 2 attributed to “final day cross-consultation”: A pending investigation or cross-consultation on the last day of discharge leads to significant delay in the discharge TAT (Table 2).
Table 2
| Sl no. | Doc | Pending tests | TAT (min) | Difference | Squared difference | |
|---|---|---|---|---|---|---|
| Actual | Model | |||||
| 1 | Doc1 | Yes | 225 | 208.10743 | 16.89257 | 285.4 |
| 2 | Doc1 | Yes | 210 | 208.10743 | 1.89257 | 3.6 |
| 3 | Doc3 | No | 130 | 113.11635 | 16.88365 | 285.1 |
| 4 | Doc3 | No | 105 | 113.11635 | −8.11635 | 65.9 |
| 5 | Doc4 | No | 51 | 80.299866 | −29.29990 | 858.5 |
| 6 | Doc3 | Yes | 233 | 191.25022 | 41.74978 | 1743.0 |
| 7 | Doc1 | No | 122 | 129.97356 | −7.97356 | 63.6 |
| 8 | Doc4 | Yes | 240 | 158.43373 | 81.56627 | 6653.1 |
| 9 | Doc3 | Yes | 173 | 191.25022 | −18.25020 | 333.1 |
| 10 | Doc3 | Yes | 234 | 191.25022 | 42.74978 | 1827.5 |
| 11 | Doc1 | Yes | 179 | 208.10743 | −29.10740 | 847.2 |
| 12 | Doc2 | No | 120 | 86.433066 | 33.56693 | 1126.7 |
| 13 | Doc4 | Yes | 189 | 158.43373 | 30.56627 | 934.3 |
| 14 | Doc3 | No | 173 | 113.11635 | 59.88365 | 3586.1 |
| 15 | Doc4 | No | 51 | 80.299866 | −29.29990 | 858.5 |
| 16 | Doc3 | Yes | 219 | 191.25022 | 27.74978 | 770.1 |
| 17 | Doc1 | No | 120 | 129.97356 | −9.97356 | 99.5 |
| 18 | Doc1 | Yes | 225 | 208.10743 | 16.89257 | 285.4 |
| 19 | Doc1 | Yes | 205 | 208.10743 | −3.10743 | 9.7 |
| 20 | Doc3 | Yes | 192 | 191.25022 | 0.749777 | 0.6 |
| 21 | Doc6 | Yes | 142 | 189.06024 | −47.06020 | 2214.7 |
| 22 | Doc1 | No | 132 | 129.97356 | 2.026439 | 4.1 |
| MAE (min) | 25.24 | |||||
| MSEa (min2) | 1038.88 | |||||
| RMSE (min) | 32.23 | |||||
| R2 (%) | 69.2 | |||||
| SE (min) | 32.4 | |||||
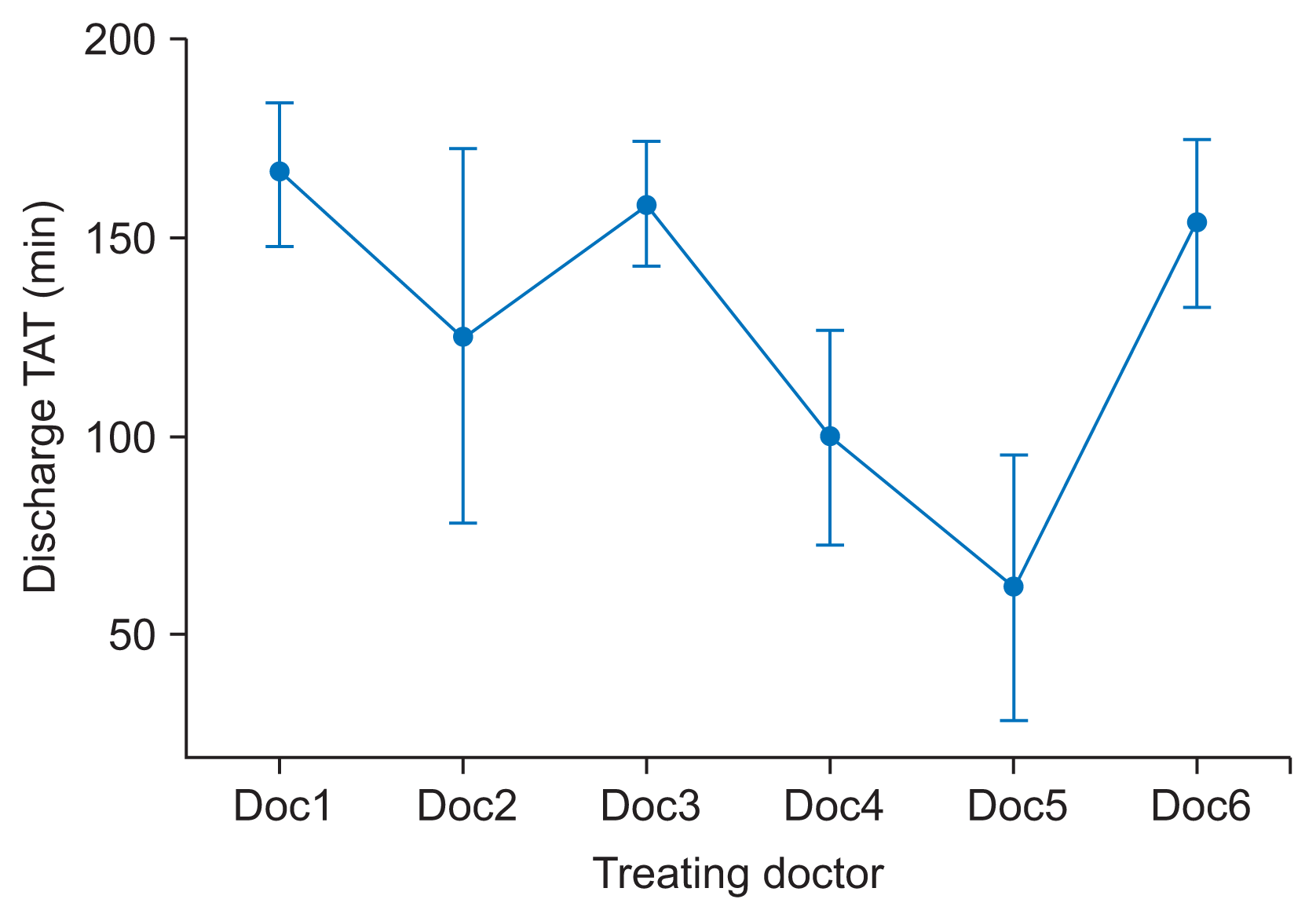 | Figure 3Interval plot discharge TAT vs. doctors. Bar represents as 95% confidence interval for the mean. The pooled standard deviation was used to calculate the intervals. TAT: turnaround time. |
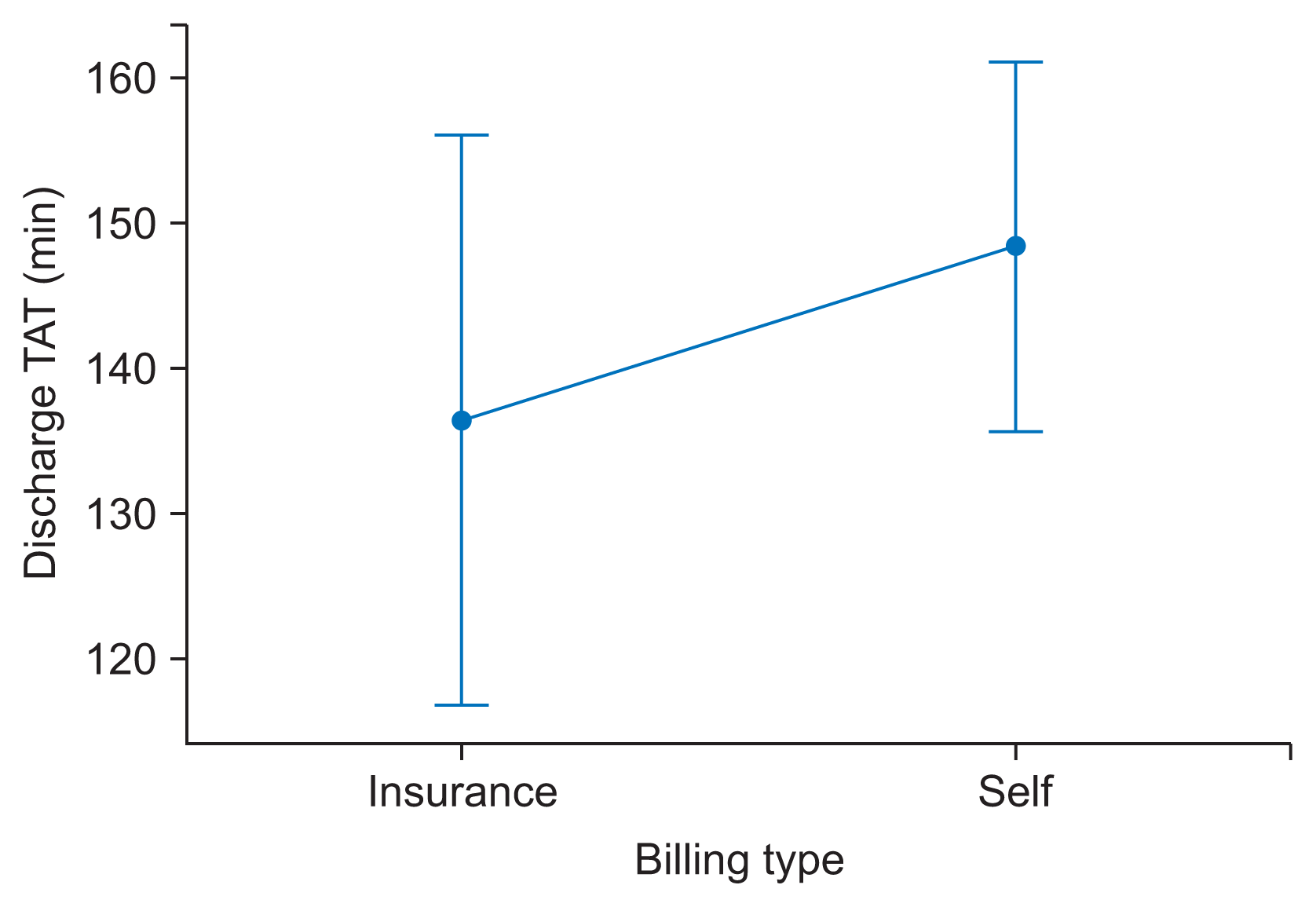 | Figure 4Interval plot discharge TAT vs. billing type. Bar represents as 95% confidence interval for the mean. The pooled standard deviation was used to calculate the intervals. TAT: turnaround time. |
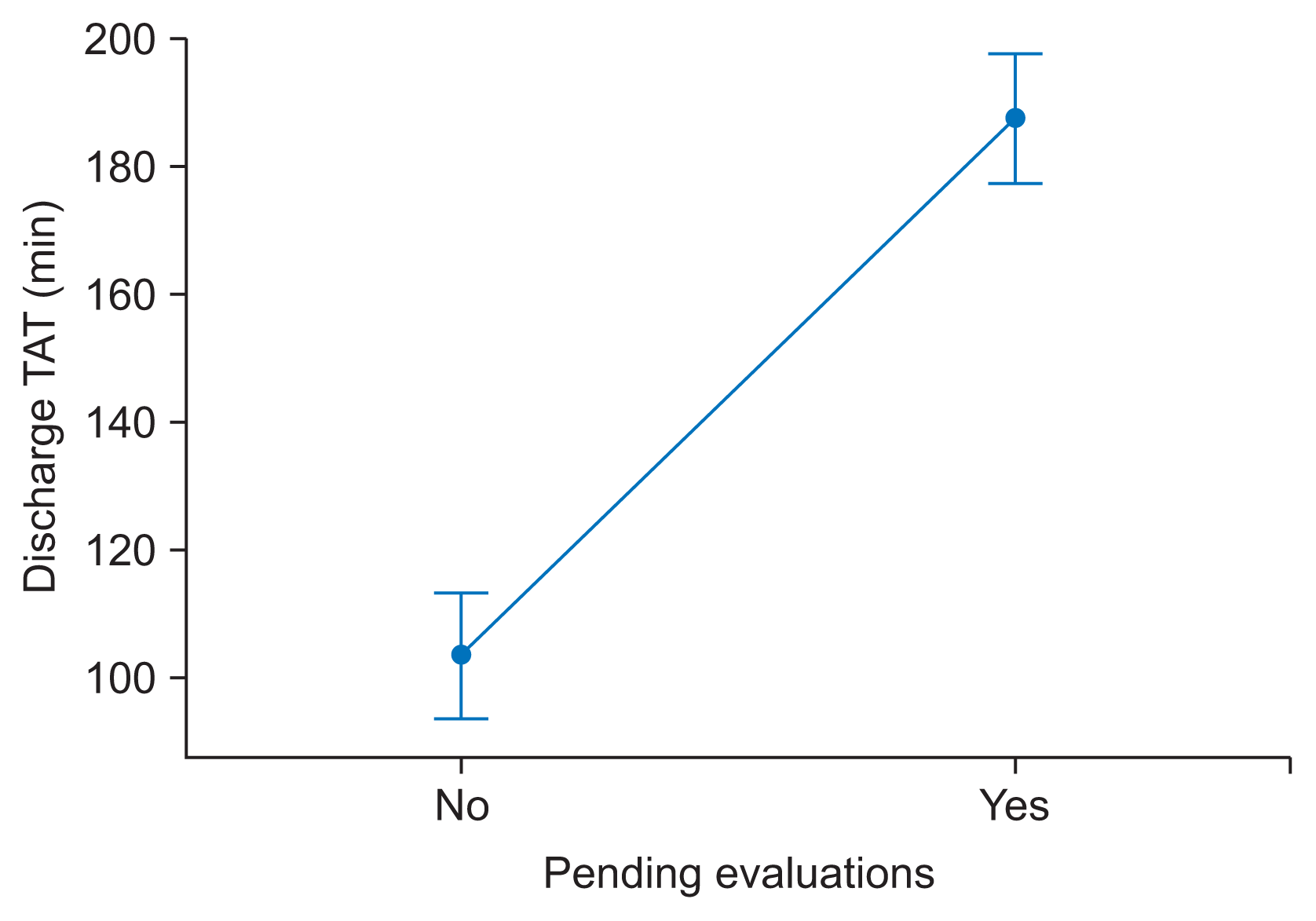 | Figure 5Interval plot discharge TAT vs. pending evaluations. Bar represents as 95% confidence interval for the mean. The pooled standard deviation was used to calculate the intervals. TAT: turnaround time. |
Table 3
Part 2
Table 4
| Evaluation | Value |
|---|---|
| MAE (min) | 20.86 |
| MSEa (min2) | 702.26 |
| RMSE (min) | 26.5 |
| R2 (%) | 77.3 |
| SE (min) | 26.7 |




 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download