I. Introduction
Facial fractures in the pediatric population are uncommon, accounting for 1.5% to 8.0% of injuries in children aged 12 years or younger, and less than 1% of injuries in children below the age of 5 years
1. The low incidence of maxillofacial injuries in children has been attributed to the elasticity of facial bones, greater cranium to face ratio, thicker layer of adipose tissue, and lack of pneumatization of paranasal sinuses in young children. In addition, preschool children receive more parental care and are less independent than older children. However, the incidence of facial trauma increases as children age and become more exposed to outdoor activities.
According to the literature, motor vehicle accidents (MVA), falls from height, sports-related injuries, and interpersonal violence are the leading causes of maxillofacial injuries
2-9. There is geographical variation in the incidence and pattern of maxillofacial trauma due to differences in socioeconomic, cultural, and environmental factors
4-6. Epidemiological data regarding maxillofacial injuries are essential for clinical auditing, improving patient management, and the development of preventive strategies
5,6. However, very few reports have investigated the epidemiology of facial trauma in the pediatric population, and none have focused on West Bengal, India. Therefore, the aim of the present study was to determine the etiological factors and patterns of maxillofacial injuries among children in this part of India.
IV. Discussion
Trauma is associated with significant morbidity and mortality in children. Although maxillofacial injuries are uncommon in children, when they occur they may lead to functional impairment and aesthetically unacceptable appearance. Several studies were carried out to understand the incidence and characteristics of pediatric maxillofacial injuries. In this study, we retrospectively evaluated maxillofacial injuries in a pediatric sample (<12 years).The mean age of the patients in this sample was 6.77±3.25 years, which is comparable with the sample used in a previous study that reported a mean age of 6.5±3.72 years among 0- to 12-year-old Pakistani children
7.
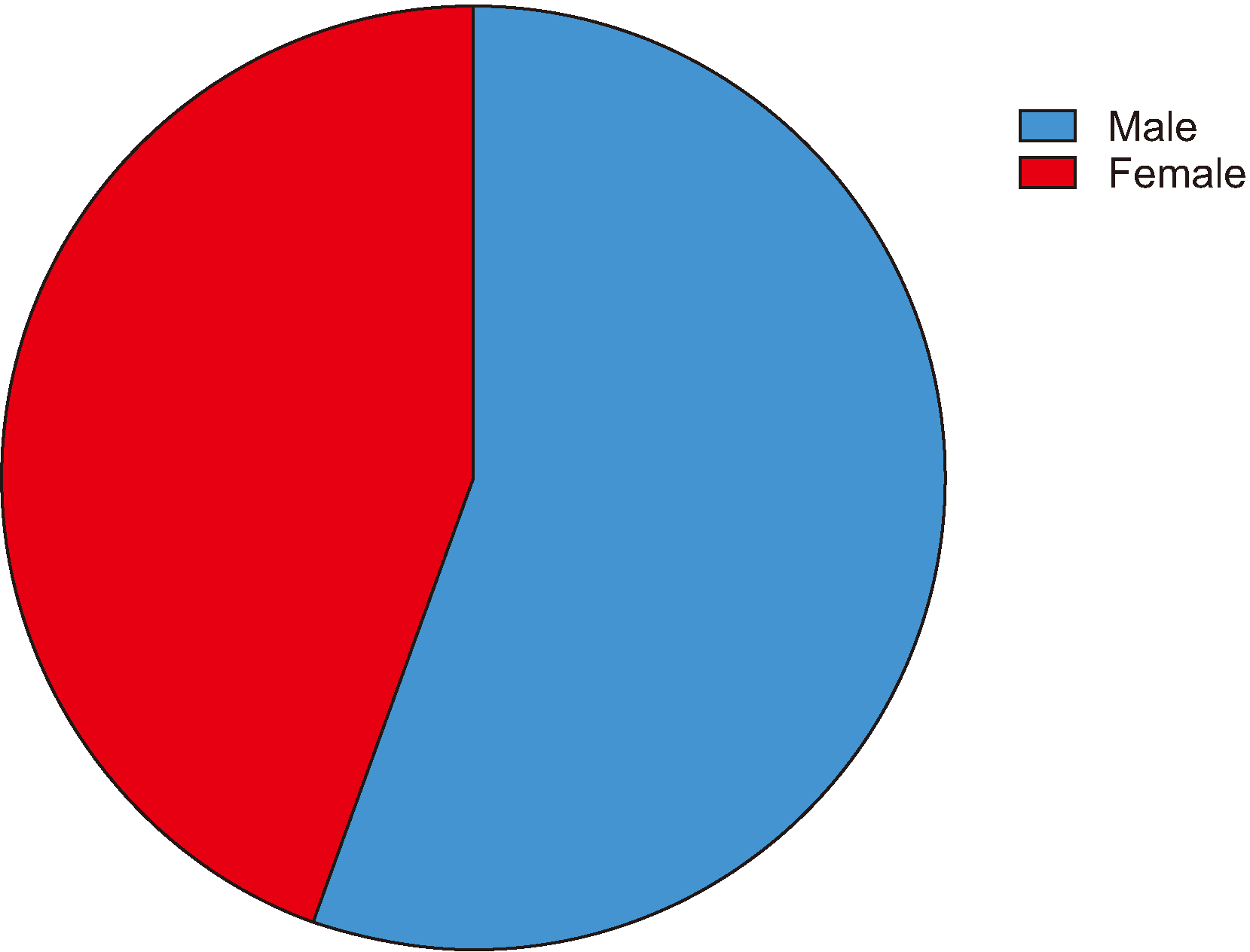
In this sample, boys suffered more facial injuries than girls, consistent with the findings of other reports. In fact, several previous investigations have suggested male predominance in the incidence of facial trauma, and the sex ratio in the literature varies between 1.6:1 and 3.3:1
8-11. In line with other reports, the male-to-female ratio in our sample increased progressively with age, from 1.1:1 in children aged 0-6 years to 1.6:1 in children aged 7-12 years
12,13. According to Collao-González et al.
13, the less marked difference in preschool children might be due to age-related childhood activities. The greater male predominance in older children and adolescents could be due to the fact that males are more often involved in outdoor activities, sports, and violence. Karim et al.
14 proposed that boys are more aggressive than girls, and therefore are more likely to get injured than girls.
Rowe
15 reported that about 1% of all facial bone fractures occur before 6 years of age, while a total of 5% occur under the age of 12 years. Posnick et al.
16 and Zimmermann et al.
9 observed that the incidence of maxillofacial injuries increases as children begin school. Other research
17-20 included major as well as minor orofacial injuries and observed a higher relative frequency of trauma in preschool children compared to school-age children. In our sample, trauma patients were almost equally divided among the preschool (0-6 years) and school-age (7-12 years) groups, probably due to the inclusion of minor soft tissue injuries and dentoalveolar fractures. We also observed that facial bone fractures were slightly more common (54.6%) in children aged 7-12 years compared to children between 0-6 years of age, so much so that no significant difference (
P>0.05) was observed between these two age groups. This finding was not only in agreement with several previous Indian studies
14,21, but also similar to some foreign studies
22,23. For example, the peak incidence of trauma occurred at the age of ten among 40 African children (<11 years) with maxillofacial injuries
22. Alcalá-Galiano et al.
24 and Rahman et al.
25 also observed a greater incidence of maxillofacial injuries in children aged 6-12 years and older.
The incidence and pattern of facial fractures depend not only on socioeconomic status, culture, and geographical location, but also on the age of the sample studied. For example, Cavalcanti and Melo
26 observed an incidence of facial fractures of 70% among 256 Brazilian patients with maxillofacial injuries aged 5-17 years. Osunde et al.
27 reported an incidence of 32% in children 15 years of age and younger in Nigeria. Kumaraswamy et al.
11 observed facial fractures in 77 cases out of 95 patients (81%) in an Indian pediatric sample less than 12 years of age. A recent Pakistani study also found a high incidence (88%) of facial fractures in children aged 0-14 years
28. We observed an overall incidence of facial fractures of 43% in the present study.
Fall from height was the predominant cause of facial trauma in our sample, accounting for 56.5% of cases. This finding is comparable with the results obtained by Kumaraswamy et al.
11, Collao-González et al.
13, Karim et al.
14, and Cavalcanti and Melo
26, who also reported falls as the leading cause of facial trauma. In contrast, Holland et al.
23, Ul Haq and Khan
28, Posnick et al.
16, Osunde et al.
27, and Kim et al.
29 found that MVA was the most common cause of oral and maxillofacial trauma in their samples, possibly due to the inclusion of adolescents. In the present study, we observed that the incidence of falls decreased with age and varied significantly between children aged 0-6 years and 7-12 years (71.9% vs 41.5%,
P<0.001). On the other hand, MVA, bicycle accidents, sports related injuries, and trauma from tube well handles progressively increased with age. Young children tend to be prone to sustaining injuries through low velocity/energy traumas such as falls because their motor skills are not fully developed. However, when children begin school and are exposed to outdoor activities, the incidence of high energy/velocity trauma, such as MVA, bicycle accidents, sports-related injuries, and trauma from tube well handles increases. Additionally, the incidence of assault or interpersonal violence as a cause of injury was low in our sample (1.3%). This incidence agrees with the results of a Nigerian study
27 (3.8%) and an Austrian study
16 (3.9%), but is much lower than most reported in the literature
6,8,29. Similarly, we observed a low frequency of animal-related facial injuries (n=6, 2.6%) and all but one were among rural residents. This is consistent with the findings of previous studies and supports the observation that human animal conflicts are more common in rural areas
1,12.
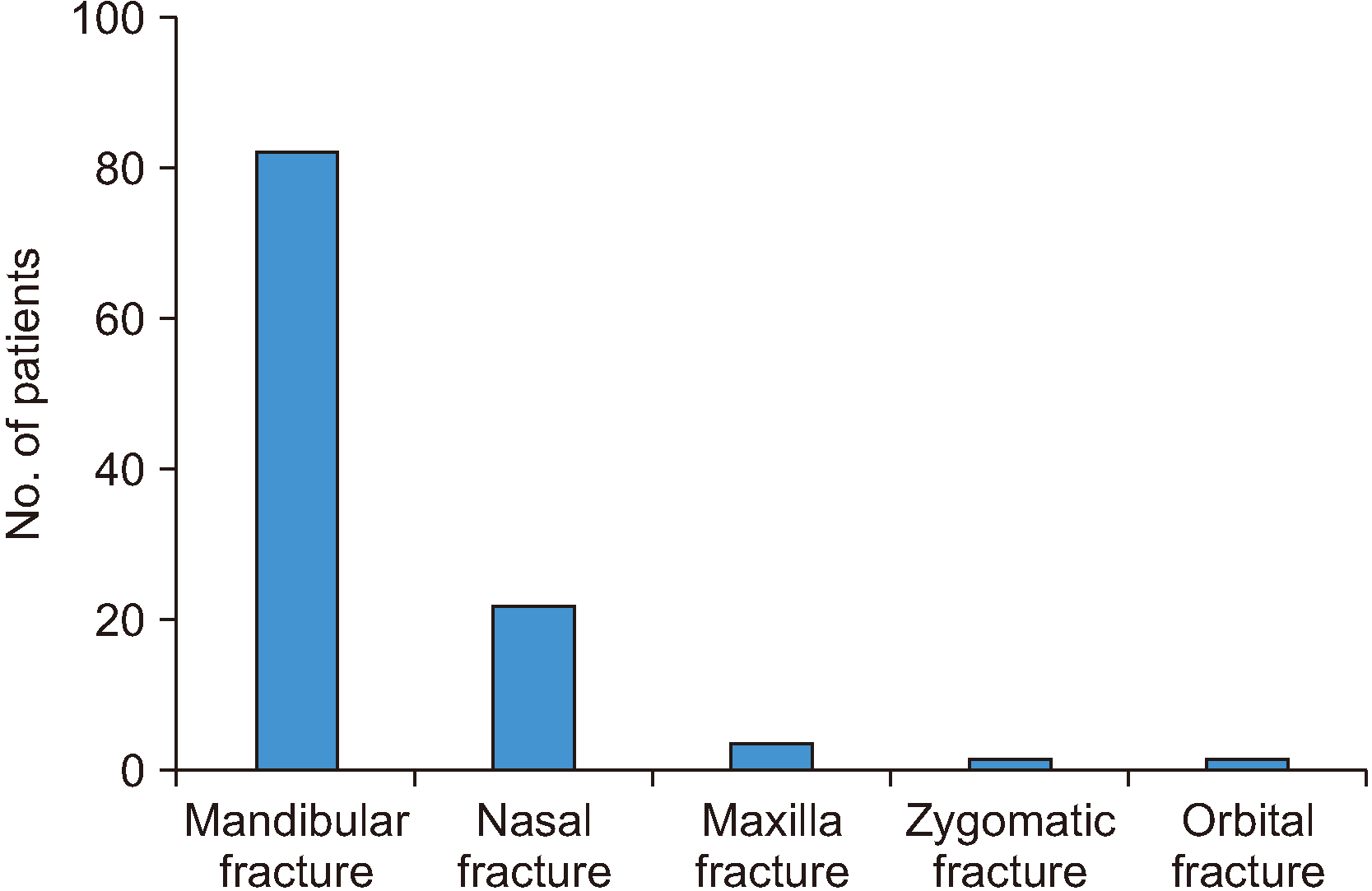
In the present study, mandibular fractures were the most common facial fractures (82.8%), and the frequency increased with age. This finding is in agreement with those of previous reports
1,4,11,14,16. Although some studies have shown that nasal bone fractures are the most frequent facial fractures, they were only the second most common type of fracture (22.2%) in our sample
13,24,26. The lower incidence of mandibular fractures in preschool children compared to older children may be attributed to the retruded position of the face in relation to the skull in younger children. However, as age increases, the mandible grows inferiorly and anteriorly and the increased prominence of the middle and lower third of the face correspond to the greater incidence of mandibular and nasal fractures in older children and adolescents. Maxillary fractures constituted 4% all facial fractures in our sample, while zygomatic and orbital fractures were the least common (2.0%), and most of those were due to MVA. This is consistent with the findings of other reports finding that midface fractures are uncommon in children and usually result from high-energy injuries such as MVA
9,13,22.
The incidence of soft tissue injuries (57.3%) in the present study was greater than the incidence of facial fractures (42.7%), which agrees with the findings of other studies
20,27. Furthermore, among the soft tissue injuries, perioral or lip injuries were the most prevalent in our sample. Yang et al.
30 observed that soft tissue injuries are the most common in the lip region due to the prominence of the mandible. The incidence of dentoalveolar fractures was 61.6% in our sample, which agrees with the results found by Gassner et al.
17 (76.3%), but is greater than those found by Kumaraswamy et al.
11 (42.1%), Cavalcanti and Melo
26 (25.8%), and Osunde et al.
27 (12.5%). Zimmermann et al.
9 reported that dentoalveolar fractures are very common in children and are often treated in the outpatient setting. Previous has also shown that type of trauma is generally related to the age of the population
31.
Various studies have shown that 10% to 88% of patients with facial trauma present with associated injuries in other parts of the body
4,9,23,24. Concomitant bodily injuries were registered in 6% of the patient population in our study. The wide variation in the frequency of associated injuries is largely attributed to variation in the mechanism of trauma.
The present study has limitations, which include small sample size and its retrospective nature. Furthermore, we did not study the outcomes of treatment, as treatment is carried out in the Department of Oral and Maxillofacial Surgery at our institution. In addition, our data were obtained from an injury report register maintained in the Department of Pediatric Dentistry, which included referred patients as well as patients coming directly to the outpatient department. Therefore, data from exclusive maxillofacial trauma centers may show different patterns.




 PDF
PDF Citation
Citation Print
Print



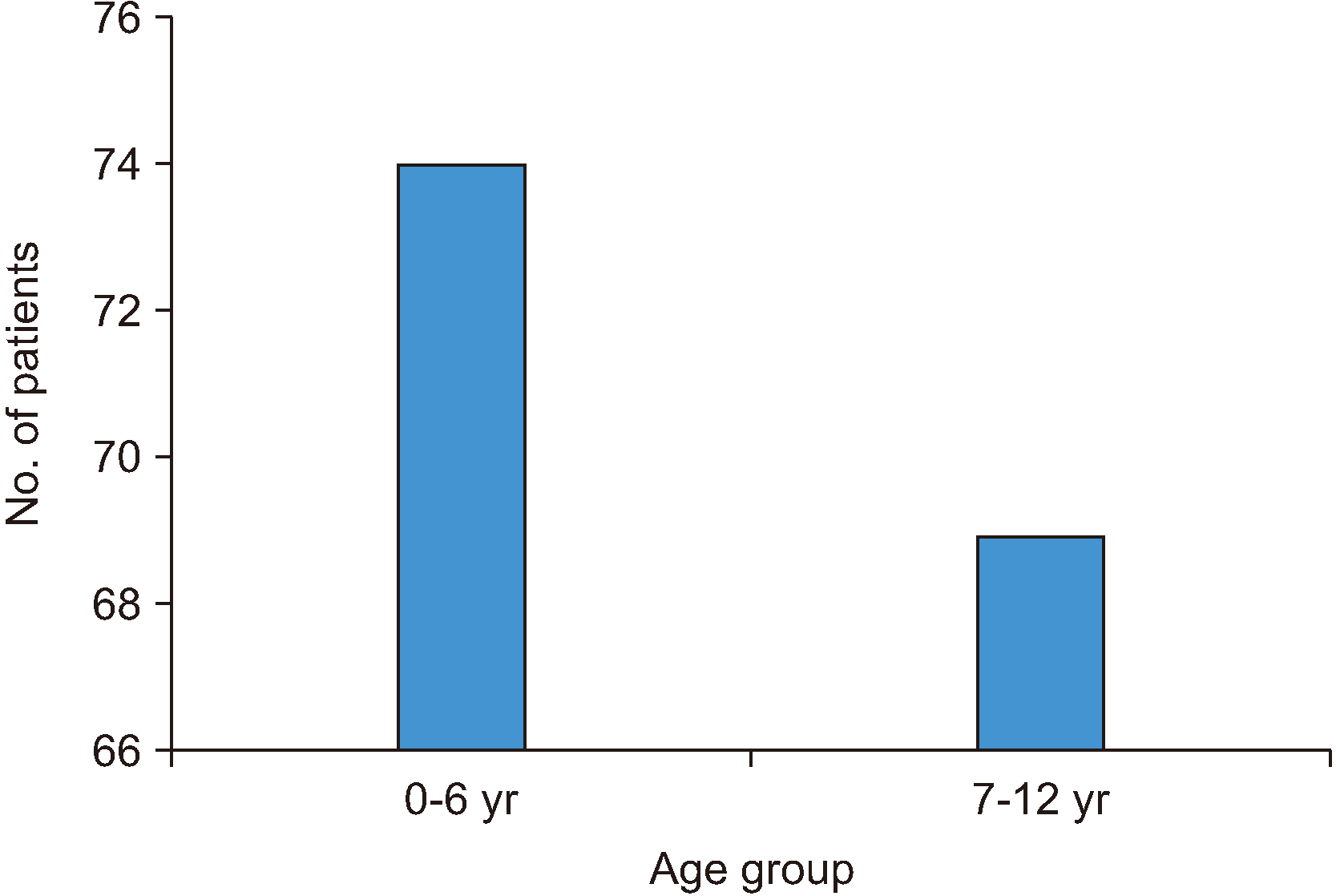
 XML Download
XML Download