Abstract
Objective
Takayasu's arteritis (TAK) is a vasculitis that primarily involves the aorta and its branches. In Behçet's disease (BD), systemic vasculitis is one of major manifestations. We aimed to compare clinical and angiographic features and outcome between TAK and BD with arterial involvement.
Methods
We retrospectively reviewed medical records of 206 TAK patients and 50 BD patients between 1995 and 2015. Angiographic lesions were evaluated via computed tomography, magnetic resonance imaging, and/or conventional angiography.
Results
Fever (30% vs. 9.2%, p<0.001) and arthralgia (36% vs. 7.3%, p<0.001) were more common in BD. C-reactive protein was higher in BD compared with TAK (5.85 mg/dL vs. 2.08 mg/dL, p<0.001). Stenosis (89.8% vs. 60%, p<0.001) and occlusion (65.5% vs. 32%, p<0.001) were more observed in TAK. In contrast, aneurysm was common in BD (62% vs. 20.9%, p<0.001). The carotid artery (73.3% vs. 30%, p<0.001), subclavian artery (71.4% vs. 16%, p<0.001), descending aorta (35% vs. 12%, p=0.002), renal artery (23.8% vs. 10%, p=0.032), superior mesenteric artery (18.4% vs. 4%, p=0.012), and brachiocephalic trunk (13.6% vs. 2%, p=0.020) were more commonly involved in TAK, whereas the femoral artery (10% vs. 2.4%, p=0.027) was more frequently involved in BD. During follow-up, arterial dissection (10% vs. 1.9%, p=0.016), rupture (12% vs. 0.5%, p<0.001), and arterial replacement/resection (66% vs. 9.7%, p<0.001) were more observed in BD.
Go to : 
REFERENCES
1. Kerr GS, Hallahan CW, Giordano J, Leavitt RY, Fauci AS, Rottem M, et al. Takayasu arteritis. Ann Intern Med. 1994; 120:919–29.

2. Schmidt J, Kermani TA, Bacani AK, Crowson CS, Cooper LT, Matteson EL, et al. Diagnostic features, treatment, and outcomes of Takayasu arteritis in a US cohort of 126 patients. Mayo Clin Proc. 2013; 88:822–30.

3. Lee GY, Jang SY, Ko SM, Kim EK, Lee SH, Han H, et al. Cardiovascular manifestations of Takayasu arteritis and their relationship to the disease activity: analysis of 204 Korean patients at a single center. Int J Cardiol. 2012; 159:14–20.

5. Sarica-Kucukoglu R, Akdag-Kose A, KayabalI M, Yazganoglu KD, Disci R, Erzengin D, et al. Vascular involvement in Behçet's disease: a retrospective analysis of 2319 cases. Int J Dermatol. 2006; 45:919–21.
6. al-Dalaan AN, al Balaa SR, el Ramahi K, al-Kawi Z, Bohlega S, Bahabri S, et al. Behçet's disease in Saudi Arabia. J Rheumatol. 1994; 21:658–61.
7. Tüzün H, Beşirli K, Sayin A, Vural FS, Hamuryudan V, Hizli N, et al. Management of aneurysms in Behçet's syndrome: an analysis of 24 patients. Surgery. 1997; 121:150–6.

8. Ames PR, Steuer A, Pap A, Denman AM. Thrombosis in Behçet's disease: a retrospective survey from a single UK centre. Rheumatology (Oxford). 2001; 40:652–5.
9. Arend WP, Michel BA, Bloch DA, Hunder GG, Calabrese LH, Edworthy SM, et al. The American College of Rheumatology 1990 criteria for the classification of Takayasu arteritis. Arthritis Rheum. 1990; 33:1129–34.

10. International Team for the Revision of the International Criteria for Behçet's Disease (ITR-ICBD). The International Criteria for Behçet's Disease (ICBD): a collaborative study of 27 countries on the sensitivity and specificity of the new criteria. J Eur Acad Dermatol Venereol. 2014; 28:338–47.
11. Saliba E, Sia Y. The ascending aortic aneurysm: when to in-tervene? Int J Cardiol Heart Vasc. 2015; 6:91–100.

12. Gagné-Loranger M, Dumont É, Voisine P, Mohammadi S, Dagenais F. Natural history of 40-50 mm root/ascending aortic aneurysms in the current era of dedicated thoracic aortic clinics. Eur J Cardiothorac Surg. 2016; 50:562–6.

13. Forsdahl SH, Solberg S, Singh K, Jacobsen BK. Abdominal aortic aneurysms, or a relatively large diameter of nonaneurysmal aortas, increase total and cardiovascular mortality: the Tromsø study. Int J Epidemiol. 2010; 39:225–32.
14. Bicakcigil M, Aksu K, Kamali S, Ozbalkan Z, Ates A, Karadag O, et al. Takayasu's arteritis in Turkey – clinical and angiographic features of 248 patients. Clin Exp Rheumatol. 2009; 27(1 Suppl 52):S59–64.
15. Seyahi E, Karaaslan H, Ugurlu S, Yazici H. Fever in Behçet's syndrome. Clin Exp Rheumatol. 2013; 31(3 Suppl 77):64–7.
16. Müftüoğlu AU, Yazici H, Yurdakul S, Tüzün Y, Pazarli H, Güngen G, et al. Behçet's disease. Relation of serum C-reactive protein and erythrocyte sedimentation rates to disease activity. Int J Dermatol. 1986; 25:235–9.
17. Saadoun D, Asli B, Wechsler B, Houman H, Geri G, Desseaux K, et al. Long-term outcome of arterial lesions in Behçet disease: a series of 101 patients. Medicine (Baltimore). 2012; 91:18–24.
18. Ostertag-Hill CA, Abdo AK, Alexander JQ, Skeik N. Unique case of Takayasu arteritis with severe distal aortic stenosis and iliac thrombosis. Ann Vasc Surg. 2016; 32:128.e7-13.

19. Purkayastha S, Jayadevan ER, Kapilamoorthy TR, Gupta AK. Suction thrombectomy of thrombotic occlusion of the subclavian artery in a case of Takayasu's arteritis. Cardiovasc Intervent Radiol. 2006; 29:289–93.

20. Wu X, Li G, Huang X, Wang L, Liu W, Zhao Y, et al. Behçet's disease complicated with thrombosis: a report of 93 Chinese cases. Medicine (Baltimore). 2014; 93:e263.
21. Yang SS, Park KM, Park YJ, Kim YW, Do YS, Park HS, et al. Peripheral arterial involvement in Behcet's disease: an analysis of the results from a Korean referral center. Rheumatol Int. 2013; 33:2101–8.

22. Park YB, Hong SK, Choi KJ, Sohn DW, Oh BH, Lee MM, et al. Takayasu arteritis in Korea: clinical and angiographic features. Heart Vessels Suppl. 1992; 7:55–9.

23. Vaideeswar P, Deshpande JR. Pathology of Takayasu arteritis: a brief review. Ann Pediatr Cardiol. 2013; 6:52–8.

24. Kobayashi M, Ito M, Nakagawa A, Matsushita M, Nishikimi N, Sakurai T, et al. Neutrophil and endothelial cell activation in the vasa vasorum in vasculo-Behçet disease. Histopathology. 2000; 36:362–71.

25. Matsumoto T, Uekusa T, Fukuda Y. Vasculo-Behçet's disease: a pathologic study of eight cases. Hum Pathol. 1991; 22:45–51.

26. Suwanwela NC, Suwanwela N. Takayasu arteritis: ultrasonographic evaluation of the cervico-cerebral arteries. Int J Cardiol. 1998; 66(Suppl 1):S163–73.

27. Koo HJ, Yang DH, Kang JW, Lee JY, Kim DH, Song JM, et al. Demonstration of infective endocarditis by cardiac CT and transoesophageal echocardiography: comparison with intraoperative findings. Eur Heart J Cardiovasc Imaging. 2018; 19:199–207.

28. Koo HJ, Lee JY, Kim GH, Kang JW, Kim YH, Kim DH, et al. Paravalvular leakage in patients with prosthetic heart valves: cardiac computed tomography findings and clinical features. Eur Heart J Cardiovasc Imaging. 2018; 19:1419–27.

29. Yang KQ, Meng X, Zhang Y, Fan P, Wang LP, Zhang HM, et al. Aortic aneurysm in Takayasu arteritis. Am J Med Sci. 2017; 354:539–47.

30. Tsui KL, Lee KW, Chan WK, Chan HK, Hon SF, Leung TC, et al. Behçet's aortitis and aortic regurgitation: a report of two cases. J Am Soc Echocardiogr. 2004; 17:83–6.

31. Wu XP, Zhu P. Clinical features of aortic dissection associated with Takayasu's arteritis. J Geriatr Cardiol. 2017; 14:485–7.
Go to : 
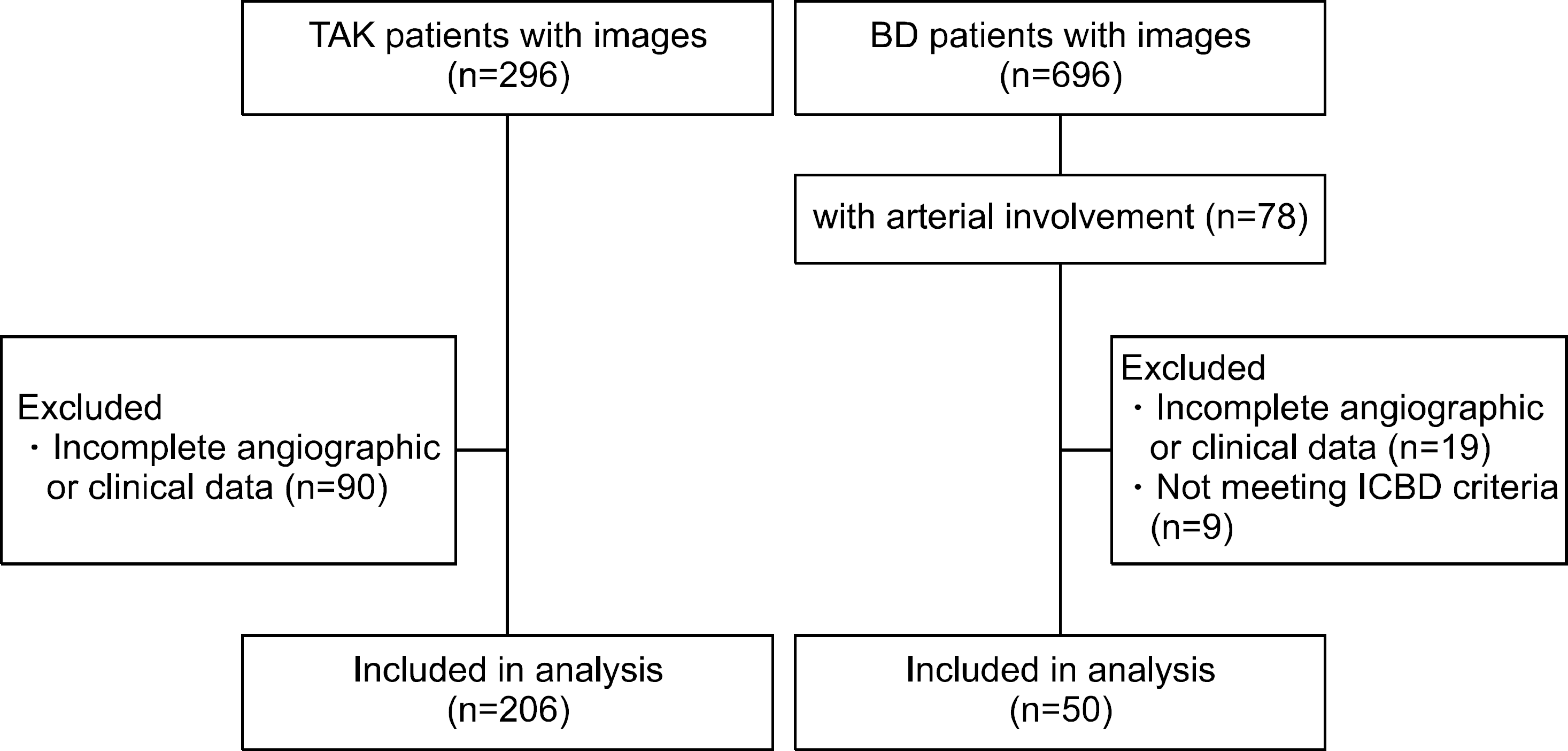 | Figure 1.Study participants in Takayasu's arteritis (TAK) and Behçet's disease (BD). ICBD: International Criteria for Behçet's disease. |
 | Figure 2.Pattern of angiographic features in Takayasu's arteritis (TAK) and Behçet's disease (BD) according to distribution region. Results presented as number (%). *p<0.05, **p<0.01, and ***p<0.001. |
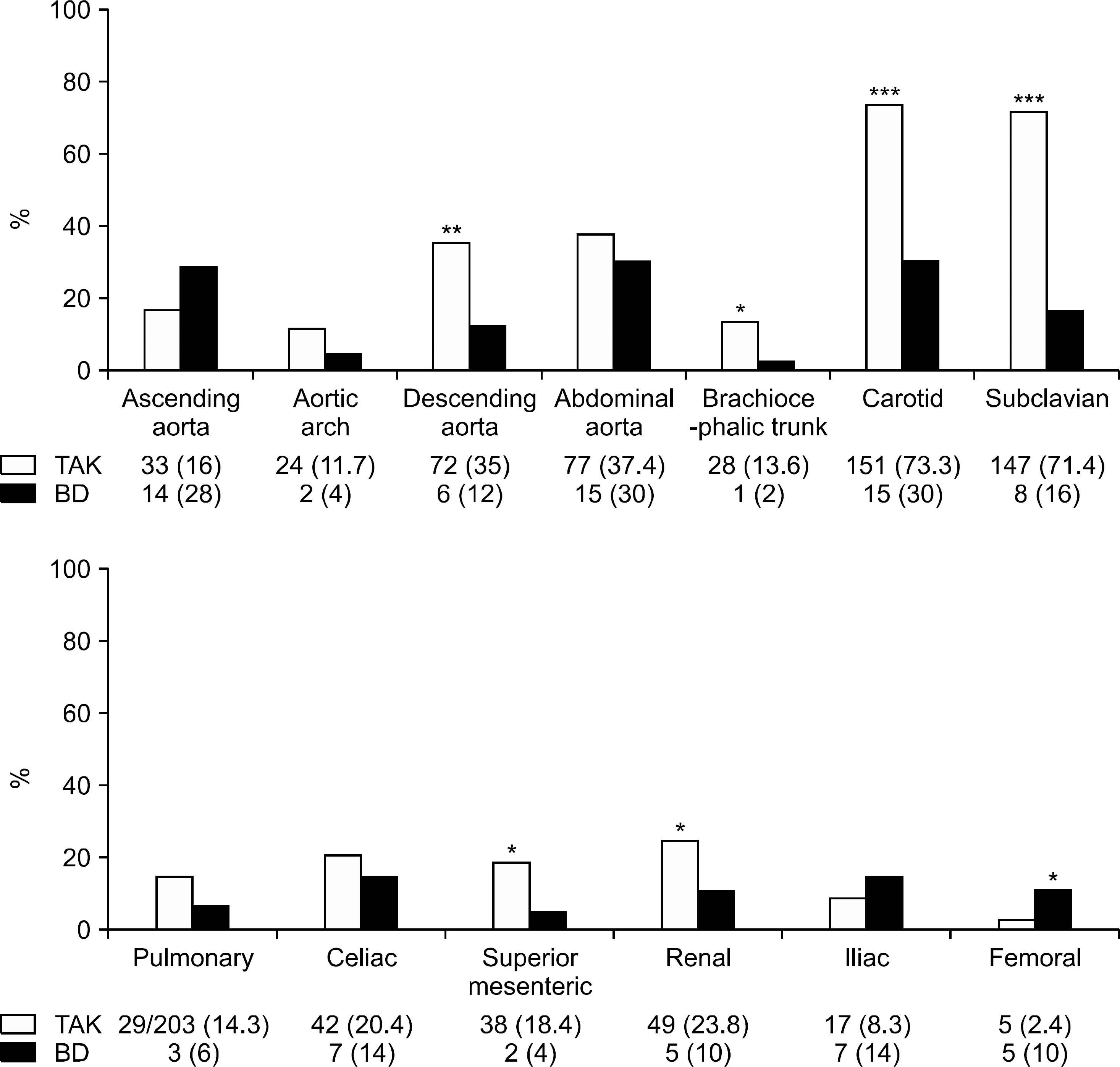 | Figure 3.Arterial involvement in Takayasu's arteritis (TAK) and Behçet's disease (BD) according to distribution. Results presented as number (%). *p<0.05, **p<0.01, and ***p<0.001. |
Table 1.
Demographic data and clinical features at diagnosis in Takayasu's arteritis and Behçet's disease
Table 2.
Angiographic features of arterial involvement in Takayasu's arteritis and Behçet's disease
Table 3.
Complications and interventions in Takayasu's arteritis and Behçet's disease




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download