Abstract
Cardiac rhabdomyoma is common cardiac mass found during the fetal period. Cardiac rhabdomyoma and tuberous sclerosis have significant associations. Tuberous sclerosis in newborns can cause disability in nearly all organs. Prenatal diagnosis of fetal tuberous sclerosis enables early evaluation and management of the affected infant. In Daegu Catholic University Hospital, a total of three cases of fetal intracranial tuberous sclerosis were diagnosed among five cases of fetal cardiac rhabdomyoma. The diagnosis in all three cases was confirmed by postnatal brain magnetic resonance imaging. Intracranial lesions appeared as multiple small, round and relatively hyperechoic masses on prenatal ultrasonography. Prenatal ultrasonography using transabdominal and transvaginal probes in various angles is helpful. As tuberous sclerosis is not observed in a single instance, regular follow-up examinations are necessary. Fetuses with cardiac rhabdomyoma require detailed prenatal evaluations for tuberous sclerosis, especially in the brain. For this, prenatal ultrasonography is a very useful technique.
Cardiac rhabdomyoma (CR) is the most common cardiac mass found in heart, with an incidence of about 60%. Notably, 90% of CR cases involve multiple tumors that are found in the ventricular septum or cardiac valves. Most CRs are benign; however, fetal cardiac function can be altered according to the size, number, and location of the tumor mass, which in turn affects the prognosis of the newborn.1
CR and tuberous sclerosis complex (TSC) have significant associations. Fetal CRs detected with prenatal fetal echocardiography are usually the earliest signs of TSC. TSC is a multi-organ involvement disorder and generally affects the proliferation of normal cells in the skin, brain, kidney, heart and lungs, resulting in the dysfunction of each organ. TSC in newborns can cause disability in most organs of the body, including skin, eyes and kidney as well as neurological systems. Therefore, prenatal diagnosis of fetal TSC is important because it enables early evaluation and management of the affected infants. There were many reports described fetal brain lesions associated with TSC. However, most of these brain lesions were detected by prenatal or postnatal brain magnetic resonance imaging (MRI), not prenatal brain ultrasonography (USG).2 Therefore, we report the fetal brain lesions associated with TSC detected by fetal USG in fetuses who have CRs.
From January 2015 to December 2018, there were five cases diagnosed with fetal CR at Daegu Catholic University Hospital. A retrospective review of medical records was conducted. Data on maternal characteristics, USG features of fetal CR and TSC, delivery, TSC gene mutations, and the clinical course; postnatal evaluation results, including neonatal transthoracic echocardiography (TTE) and brain MRI results were collected.
Table 1 shows the clinical features of the five fetuses. A total of four fetuses showed multiple CRs on prenatal USG and intracranial TSC findings were observed in three fetuses. Additionally, two patients were simultaneously diagnosed with CR and TSC, and one patient was diagnosed with TSC 6 weeks after the diagnosis of CR. Case no. 1 showed intracranial tuberous nodules appear as echogenic round masses. In case no. 4, several echogenic tubers with echogenic nodules and round tumor mass suspected with subependymal giant cell astrocytoma (SEGA) were revealed. In case no. 5, multiple echogenic nodules were present. The delivery method was determined regardless of the presence of CR or TSC. Four of the fetuses were delivered at our clinic, and one was delivered at another hospital.
Postnatal TTE and brain MRI were performed in all patients, and abdominal USG was performed in four cases born at Daegu Catholic University Hospital. The prenatal diagnosis in all cases of intracranial TSC was confirmed by postnatal brain MRI. Case no. 4 was diagnosed as having a SEGA on postnatal brain MRI and subsequent surgery. Two fetuses who had not been diagnosed with intracranial TSC on prenatal examination showed normal postnatal brain MRI findings. On postnatal abdominal USG, case no.1 showed a small renal cyst, and the findings were normal in case no. 2–4. Four newborns underwent genetic evaluation (case no. 2–5), and TSC2 gene mutation was found in two cases. Case no. 3 who had not revealed intracranial TSC lesion showed TSC2 gene mutation with variation of unknown significance (VUS). Parents of case no. 1 refused genetic evaluation.
Case no. 5 was diagnosed with multiple giant CRs in the right ventricle, obstructing the right ventricle outflow tract and compressing the left ventricle. The blood flow from the right ventricle toward the pulmonary artery was not seen and retrograde flow via ductus arteriosus was observed. Therefore, functional pulmonary atresia was suspected due to obstruction of the right ventricular outflow by large CR in case no. 5 (Fig. 1A). The fetus was delivered at another hospital for postnatal cardiac surgery. Postnatal brain MRI of the newborn revealed intracranial TSC findings, however, the baby died because of respiratory failure on the 19th day after birth.
Follow-up for 24 months revealed normal growth and development of case no. 2 and 3. Epileptic disorder was observed in case no. 1 and 4 and anticonvulsants were administered. Case no. 1 exhibited seizure symptoms from 3 months of age and is currently under medication, but the seizures are not well controlled. Case no. 4 exhibited seizure symptoms for about 7 months after birth, and a SEGA was surgically removed at 11 months after birth.
During the prenatal examination, TSC can be found in more than half of the fetuses with CR and can cause organ dysfunction.3 TSC is an autosomal-dominant inheritance and is expressed in at least one mutation of TSC1 on chromosome 9q34 and TSC2 on chromosome 16p13.3 gene.4 Mutation of the TCR gene causes over-activation of mTORC1 and leads to dysregulation of the signaling pathway, leading to neurodegeneration, epilepsy, diabetes mellitus and cancer.567 Currently, multiple CRs are thought to be related with TSC.3 Tworetzky et al.8 reported that three of nine patients (33.3%) with single CR had TSC and 30 of 33 patients (91%) with multiple CRs had TSC.
At the second International Tuberous Sclerosis Complex Consensus Conference held in 2012, experts updated the recommendations for the evaluation and management for patients with TSC.3 Brain lesions associated with TSC are cortical tuber (CT), subependymal nodule (SEN), and SEGA. Intracranial CT and SEN lesions usually appear as small, multiple, round, and relatively hyperechoic masses in prenatal USG. In case no. 1, intracranial tuberous nodules appear as echogenic round masses in the left frontal lobe and right temporal lobe (Fig. 1E). In case no. 4, several echogenic tubers with echogenic nodules suspected to be TSC were revealed in the cerebral cortex. We also discovered another major diagnostic finding associated with TSC in the above-mentioned case, namely SEGA. It appeared as a relatively hypoechoic, round mass compressing the cavum septum pellucidum, and the right frontal horn was located just adjacent to the inter-hemispheric fissure (Fig. 1B–D, F).
Case no. 2 and 3 didn't show intracranial TSC lesion in prenatal and postnatal evaluation. In genetic test, TSC2 gene mutation was not found in case no. 2 and case no. 3 just showed mutation with VUS. However, according to the Consensus Conference in 2012,3 possible diagnosis can be determined with either one major feature (CR) or more than two minor features. Therefore, patients with possible diagnosis need regular follow-up also.
Nowadays, several physicians prefer prenatal MRI for the evaluation of fetuses, especially in the case of fetal brain anomalies. Prenatal MRI may be helpful under many circumstances. However, it is expensive and causes more discomfort to the mothers than on USG. Furthermore, when the fetus moves during examination, interpretation of the image is difficult, or almost impossible, in some cases.9 In our study, we proved the accuracy and usefulness of prenatal brain USG and the antenatal diagnosis was accord to postnatal brain MRI findings.
Prenatal USG is cost-effective and reduces the discomfort experienced by the mother. Physicians can examine various angles using USG, the findings of which are free from fetal motion artifact. Occasionally, the examiner cannot get a precise image of the fetal head by transabdominal USG because of deep engagement of the fetal head into the pelvic cavity. In this situation transvaginal USG is appropriate, with adjustment of angles. Mild fundal pressure and changing the maternal position could also be helpful. In our cases of prenatal TSC, all three fetuses were diagnosed with transvaginal USG upon vertex presentation; sagittal view and coronal view brain images were also especially helpful.
In conclusion, fetuses with CR require detailed prenatal evaluation for TSC, especially in the brain. Newborn cardiac dysfunction from various aspects of CR needs to be prepared, also. In that respect, we emphasize importance and usefulness of prenatal USG. Furthermore, postnatal cardiac computer tomography, brain MRI, and TSC gene mutation tests may be helpful.
Figures and Tables
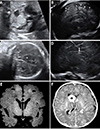 | Fig. 1(A) Fetal echocardiography showed multiple cardiac rhabdomyomas in the right ventricle, the left ventricle and the interventricular septum. (B) The para-sagittal view of the fetal brain showed multiple cortical tubers at the cerebral cortex as hyperechoic dots and round masses (arrowheads). (C) The coronal view of the fetal brain showed a single subependymal giant cell astrocytoma (SEGA) as a hypoechoic round mass adjacent to the foramen of Monro (asterisk). (D) The sagittal view of the fetal brain showed a subependymal nodule as an echogenic spot along the ependymal lining of the lateral ventricle (arrow). (E) Postnatal brain magnetic resonance imaging (MRI) of case no. 1. Hyperintensity of cortical and subcortical tubers in T1-weighted images (black arrows). (F) Postnatal brain MRI of case no. 4. SEGA within the lateral ventricle near the foramen of Monro (asterisk). |
Table 1
Clinical Features of the Five Patients with Cardiac Rhabdomyomas

Abbreviations: BMI, body mass index; GA, gestational age; CR, cardiac rhabdomyoma; LV, left ventricle; LA, Left atrium; RV, right ventricle; TSC, tuberous sclerosis; USG, ultrasonography; CS, cesarean section; NSD, normal spontaneous delivery; TTE, transthoracic echocardiography; MRI, magnetic resonance imaging; CTs, cortical tubers; SEN, subependymal nodule; r/o, rule out; SEGA, subependymal giant cell astrocytoma; NA, not appear; VUS, variation of unknown significance.
References
1. Yuan SM. Fetal primary cardiac tumors during perinatal period. Pediatr Neonatol. 2017; 58:205–210.

2. Dragoumi P, O'Callaghan F, Zafeiriou DI. Diagnosis of tuberous sclerosis complex in the fetus. Eur J Paediatr Neurol. 2018; 22:1027–1034.

3. Northrup H, Krueger DA. International Tuberous Sclerosis Complex Consensus Group. Tuberous sclerosis complex diagnostic criteria update: recommendations of the 2012 international tuberous sclerosis complex consensus conference. Pediatr Neurol. 2013; 49:243–254.
4. Saxena A, Sampson JR. Epilepsy in tuberous sclerosis: phenotypes, mechanisms, and treatments. Semin Neurol. 2015; 35:269–276.

5. Kapoor A, Girard L, Lattouf JB, Pei Y, Rendon R, Card P, et al. Evolving strategies in the treatment of tuberous sclerosis complex-associated angiomyolipomas (TSC-AML). Urology. 2016; 89:19–26.

6. Wang CC, Wang CY, Lai YJ, Chang TY, Su HY. Prenatal diagnosis of tuberous sclerosis complex using fetal ultrasonography and magnetic resonance imaging and genetic testing. Taiwan J Obstet Gynecol. 2018; 57:163–165.

7. Ekmekci E, Ozkan BO, Yildiz MS, Kocakaya B. Prenatal diagnosis of fetal cardiac rhabdomyoma associated with tuberous sclerosis: a case report. Case Rep Womens Health. 2018; 19:e00070.





 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download