Congenital pericardial anomalies are rare, manifested as pericardial cyst, diverticulum and absence of pericardium.1) Acquired and localized pericarditis manifested as a constrictive pericardial band causing strangulation and hourglass shaping of ventricles has been reported in adolescents and adults, but this type of congenital pericardial anomaly has not been reported in neonates.2)3)
A fetal echocardiography done at 22 weeks of gestation showed an unusual white ring-like structure which constricts both mid-ventricular cavities (Figure 1 and Supplementary Video 1). Both ventricular systolic and diastolic functions were within normal limits. After an uneventful pregnancy, the baby was born at 38+3 weeks of gestation with a birth weight of 3.3 kg. Echocardiography showed a pericardial fibrous band causing strangulation of both ventricles, extending from mid left ventricular lateral wall, diaphragmatic surface of both ventricles, lateral wall of right ventricle and into the right ventricular outflow track (Figures 2, 3, and Supplementary Video 2). A 3-dimensional cardiac computed tomography also showed the same findings (Figure 4). The baby was asymptomatic and discharged home 4 days after birth. At 20 months of age, the baby was still asymptomatic. Chest X-ray and electrocardiogram were unremarkable. Both ventricular global systolic functions looked normal on echocardiography. Mitral valve inflow Doppler early diastolic E velocity and late diastolic A velocity were 0.9 m/sec and 0.7 m/sec, respectively. Tricuspid annular plain systolic excursion was 15 mm. Tissue Doppler imaging showed decreased early diastolic E′ velocities of mitral and tricuspid annuli (Figure 5) along with mild dilatation of both atria, suggesting an early stage of ventricular diastolic dysfunction. This type of pericardial anomaly has not been reported, and the etiology and natural course are unknown. Close follow up is needed to assess ventricular functions and to decide necessity of any surgical intervention timely.4)
Figures and Tables
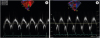
Figure 1
Fetal echocardiography findings. (A) A short-axis view showing an unusual white ring-like structure encircling both mid-ventricular cavities. (B) A 4-chamber view showing a band-like structure crossing diaphragmatic surface of both ventricles (arrows). The star (★) indicates the crux cordis.
LA = left atrium; LV = left ventricle; RA = right atrium; RV = right ventricle.
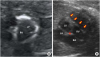
Figure 2
Parasternal long-axis views showing invaginations of pericardium (arrows) into diaphragmatic surfaces of LV (A) and RV (B).
LA = left atrium; LV = left ventricle; RA = right atrium; RV = right ventricle.
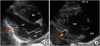
Figure 3
A modified apical 4-chamber view showing a band-like structure crossing diaphragmatic surface of both ventricles (arrows). The star (★) indicates the crux cordis and dotted lines indicate atrioventricular junctions.
LA = left atrium; LVA = apical part of left ventricle; LVI = inlet part of left ventricle; RA = right atrium; RVA = apical part of right ventricle; RVI = inlet part of right ventricle.
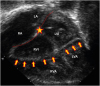
Figure 4
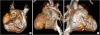
Three-dimensional cardiac computed tomography showing indentations (arrows) of diaphragmatic surface of both ventricles (A), lateral wall of LV (B) and lateral wall of RV (C). The star (★) indicates the crux cordis and dotted lines indicate atrioventricular groove or junctions.
LA = left atrium; LV = left ventricle; RA = right atrium; RV = right ventricle.
References
1. Parmar YJ, Shah AB, Poon M, Kronzon I. Congenital abnormalities of the pericardium. Cardiol Clin. 2017; 35:601–614.

2. Gautam MP, Gautam S, Sogunuru G, Subramanyam G. Constrictive pericarditis with a calcified pericardial band at the level of left ventricle causing mid-ventricular obstruction. BMJ Case Rep. 2012; 2012:bcr0920114743.

3. Karakus A, Ari H, Camci S, Ari S, Tutuncu A, Melek M. Hourglass-shaped right ventricle and localized constrictive pericarditis. Echocardiography. 2017; 34:320–321.

4. Adler Y, Charron P. The 2015 ESC guidelines on the diagnosis and management of pericardial diseases. Eur Heart J. 2015; 36:2873–2874.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download