Abstract
Background
Rhinitis was the most frequently diagnosed disorder among users of humidifier disinfectants (HDs). The aim of our study was to investigate on the relationship between allergic rhinitis (AR) and HD uses.
Methods
Our study used the data from the eighth Panel Study on Korean Children; a total of 1,540 participants were enrolled. The χ2 test and multiple logistic regression analyses were conducted to debunk the association between AR and HD uses.
Results
In our analysis, odds ratios (ORs) of doctor-diagnosed AR increased significantly when simply the response of whether HDs were used in the past was considered. When the brands of HD were considered, ORs of doctor-diagnosed AR were found to be increased significantly for those who have used polyhexamethylene guanidine phosphate/oligo(2-[2-ethoxy]-ethoxyethyl)guanidinium-containing HDs (model 3: 1.41, 95% confidence interval [CI]: 1.02–1.95). However, once duration of usage was additionally considered, ORs of doctor-diagnosed AR increased significantly only for those who have used chloromethylisothiazolinone/methylisothiazolinone-containing HDs for more than or equal to 3 months (model 3: 2.08, 95% CI: 1.17–3.69). Further, past use of HD was associated with significantly increased ORs of AR diagnosed before 2013 (model 3: 1.35, 95% CI: 1.02–1.79).
Go to : 
References
1. Paek D, Koh Y, Park DU, Cheong HK, Do KH, Lim CM, et al. Nationwide study of humidifier disinfectant lung injury in South Korea, 1994–2011. Incidence and dose-response relationships. Ann Am Thorac Soc. 2015; 12(12):1813–21.

2. Kim HJ, Lee MS, Hong SB, Huh JW, Do KH, Jang SJ, et al. A cluster of lung injury cases associated with home humidifier use: an epidemiological investigation. Thorax. 2014; 69(8):703–8.

3. National Institute of Environmental Research. Establishing disease identification and standards criteria to expand the range of health hazards caused by the humidifier sterilizer. Incheon: National Institute of Environmental Research;2017.
4. Yoon J, Lee SY, Lee SH, Kim EM, Jung S, Cho HJ, et al. Exposure to humidifier disinfectants increases the risk of asthma in children. Am J Respir Crit Care Med. 2018; 198(12):1583–6.
5. Yoon J, Cho HJ, Lee E, Choi YJ, Kim YH, Lee JL, et al. Rate of humidifier and humidifier disinfectant usage in Korean children: a nationwide epidemiologic study. Environ Res. 2017; 155:60–3.

6. National Institute of Environmental Research. Study for improving recognition and judgment standard of health damage of humidifier disinfectant(I). Incheon: National Institute of Environmental Research;2018.
7. Bahk J, Yun SC, Kim YM, Khang YH. Impact of unintended pregnancy on maternal mental health: a causal analysis using follow up data of the Panel Study on Korean Children (PSKC). BMC Pregnancy Childbirth. 2015; 15(1):85.

8. Korea Institute of Child Care and Education. Panel Study on Korean Children (PSKC) data use manual for 1st–7th study. 2016. http://www.kicce.re.kr/eng/index.do. Accessed 23 May 2019.
9. Lee JH, Kim YH, Kwon JH. Fatal misuse of humidifier disinfectants in Korea: importance of screening risk assessment and implications for management of chemicals in consumer products. Environ Sci Technol. 2012; 46(5):2498–500.

10. Greiner AN, Hellings PW, Rotiroti G, Scadding GK. Allergic rhinitis. Lancet. 2011; 378(9809):2112–22.

11. Blaiss MS. Pediatric allergic rhinitis: physical and mental complications. Allergy Asthma Proc. 2008; 29(1):1–6.

12. Marshall PS, O'Hara C, Steinberg P. Effects of seasonal allergic rhinitis on fatigue levels and mood. Psychosom Med. 2002; 64(4):684–91.

13. Kremer B, den Hartog HM, Jolles J. Relationship between allergic rhinitis, disturbed cognitive functions and psychological well-being. Clin Exp Allergy. 2002; 32(9):1310–5.

14. Hong S, Kwon HJ, Choi WJ, Lim WR, Kim J, Kim K. Association between exposure to antimicrobial household products and allergic symptoms. Environ Health Toxicol. 2014; 29:e2014017.

15. Choi H, Schmidbauer N, Sundell J, Hasselgren M, Spengler J, Bornehag CG. Common household chemicals and the allergy risks in pre-school age children. PLoS One. 2010; 5(10):e13423.

16. Slager RE, Poole JA, LeVan TD, Sandler DP, Alavanja MC, Hoppin JA. Rhinitis associated with pesticide exposure among commercial pesticide applicators in the Agricultural Health Study. Occup Environ Med. 2009; 66(11):718–24.

17. Bertelsen RJ, Longnecker MP, Løvik M, Calafat AM, Carlsen KH, London SJ, et al. Triclosan exposure and allergic sensitization in Norwegian children. Allergy. 2013; 68(1):84–91.

19. Meng JF, Rosenwasser LJ. Unraveling the genetic basis of asthma and allergic diseases. Allergy Asthma Immunol Res. 2010; 2(4):215–27.

20. Von Mutius E, Martinez FD. Natural history, development, and prevention of allergic disease in childhood. In: Adkinson NF Jr, Yunginger JW, Busse WW, Bochner B, Holgate ST, Simons FER, editors. Middleton's Allergy: Principles and Practice. 4th ed.St. Louis, MO: Mosby;2003. p. 1169–74.
21. Song JA, Park HJ, Yang MJ, Jung KJ, Yang HS, Song CW, et al. Polyhexamethyleneguanidine phosphate induces severe lung inflammation, fibrosis, and thymic atrophy. Food Chem Toxicol. 2014; 69:267–75.

22. National Institute of Environmental Research. Study on hazardous chemical substances in household chemical products and their health impact. 2014. http://webbook.me.go.kr/DLi-File/NIER/06/021/5591231.pdf. Accessed 10 Jan 2020.
23. Scientific Committee on Consumer Safety. Opinion on: the mixture of 5-chloro-2-methylisothiazolin-3 (2h)-one and 2-methylisothiazolin-3 (2h)-one. 2009. http://ec.europa.eu/health//sites/health/files/scientific_committees/consumer_safety/docs/sccs_o_009.pdf. Accessed 10 Jan 2020.
24. EAACI Task Force on Occupational Rhinitis. Moscato G, Vandenplas O, Gerth Van Wijk R, Malo JL, Quirce S, et al. Occupational rhinitis. Allergy. 2008; 63(8):969–80.

25. Jacobs KD, Brand PL. Can sensitization to aeroallergens disappear over time in children with allergic disease? Acta Paediatr. 2010; 99(9):1361–4.
26. Lim DH. Epidemiology of allergic rhinitis in Korean children. World Allergy Organ J. 2015; 8(Suppl 1):A41.

Go to : 
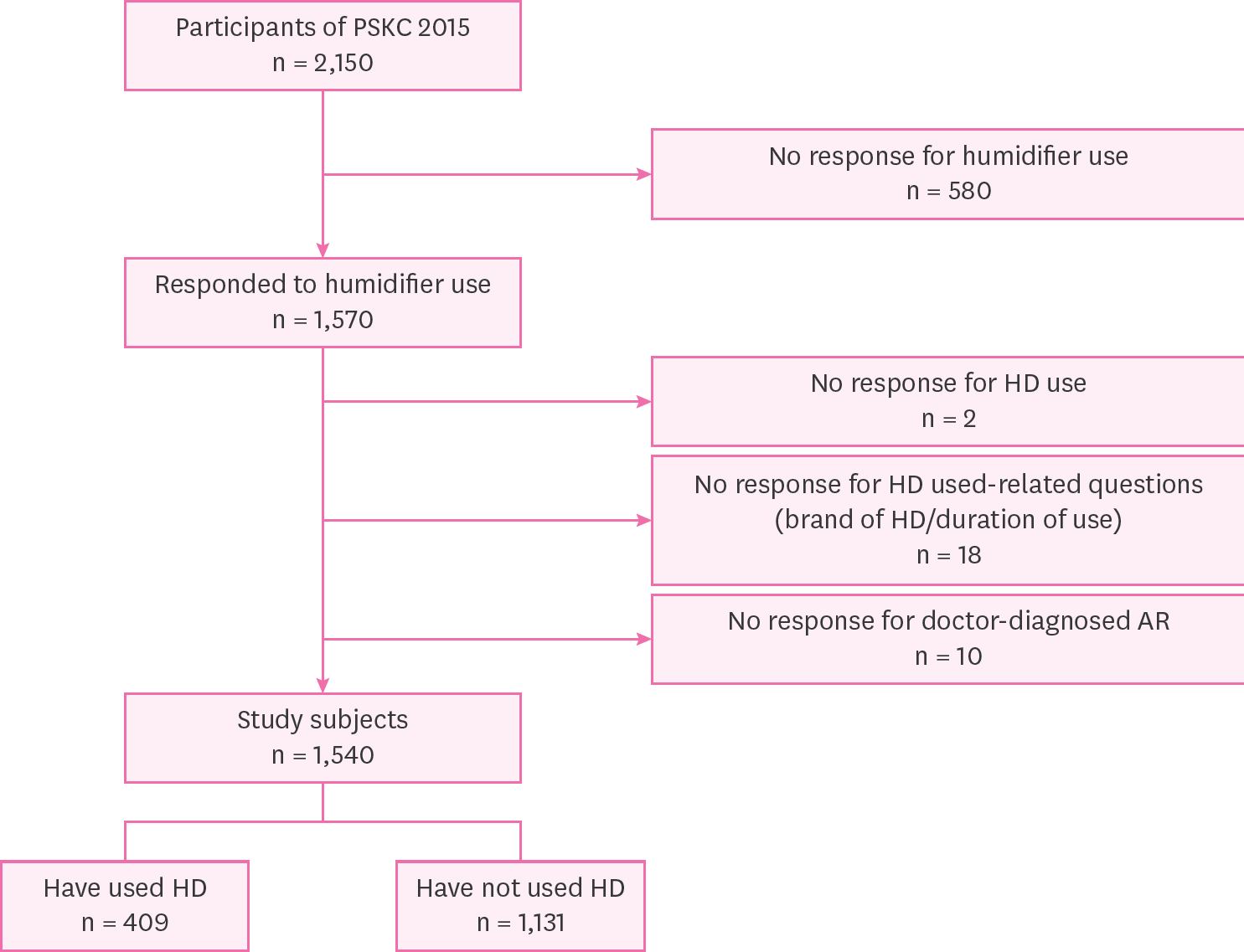 | Fig. 1.Flow chart of the selection of study subjects. PSKC: Panel Study on Korean Children; AR: allergic rhinitis; HD: humidifier disinfectant. |
Table 1.
Socioeconomic characteristics of the subjects
Table 2.
Characteristics regarding allergic disorders and relevant environmental exposures of the subjects
Table 3.
Association between doctor-diagnosed AR and types and duration of HDs used
Table 4.
Crude and adjusted OR for doctor-diagnosed AR based on HD use in the past
| Characteristics | Category | Model 1 a | Model 2 b | Model 3 c | |||
|---|---|---|---|---|---|---|---|
| OR | 95% CI | OR | 95% CI | OR | 95% CI | ||
| Have ever used HD | No | 1.00 | – | 1.00 | – | 1.00 | – |
| Yes | 1.43 | 1.14–1.79 | 1.42 | 1.12–1.82 | 1.33 | 1.02–1.75 | |
| Have used PHMG/PGH-containing HD | Have never used HD | 1.00 | – | 1.00 | – | 1.00 | – |
| No, but have used other types of HDs | 1.12 | 0.80–1.57 | 1.20 | 0.83–1.73 | 1.22 | 0.81–1.82 | |
| Yes | 1.66 | 1.26–2.19 | 1.57 | 1.17–2.11 | 1.41 | 1.02–1.95 | |
| Have used CMIT/MIT-containing HD | Have never used HD | 1.00 | – | 1.00 | – | 1.00 | – |
| No, but have used other types of HDs | 1.56 | 1.18–2.05 | 1.47 | 1.09–1.97 | 1.28 | 0.93–1.77 | |
| Yes | 1.24 | 0.89–1.73 | 1.36 | 0.95–1.95 | 1.43 | 0.96–2.13 | |
Table 5.
Crude and adjusted OR for doctor-diagnosed AR based on HD use in the past further stratified by duration
| Characteristics | Category | Model 1a | Model 2b | Model 3c | |||
|---|---|---|---|---|---|---|---|
| OR 1.00 | 95% CI | OR 1.00 | 95% CI | OR 1.00 | 95% CI | ||
| Have ever used HD | No | 1.00 | – | 1.00 | – | 1.00 | – |
| Yes (less than 3 months) | 1.00 1.34 | −1.01–1.77 | 1.00 1.34 | −1.00–1.81 | 1.00 1.26 | −0.91–1.75 | |
| Yes (greater than or equal to 3 months) | 1.57 | 1.14–2.17 | 1.55 | 1.09–2.21 | 1.46 | 0.99–2.16 | |
| Have used PHMG/PGH-containing HD | Have never used HD | 1.00 | – | 1.00 | – | 1.00 | – |
| No, but have used other types | 1.12 | 1.01–1.77 | 1.20 | 0.83–1.73 | 1.22 | 0.81–1.82 | |
| Yes (less than 3 months) | 1.60 | 1.14–2.17 | 1.52 | 1.05–2.20 | 1.39 | 0.92–2.32 | |
| Yes (greater than or equal to 3 months) | 1.74 | 1.18–2.58 | 1.66 | 1.08–2.54 | 1.45 | 0.90–2.33 | |
| Have used CMIT/MIT-containing HD | Have never used HD | 1.00 | – | 1.00 | – | 1.00 | – |
| No, but have used other types | 1.00 1.56 | – 1.19–2.05 | 1.00 1.47 | – 1.09–1.97 | 1.00 1.28 | – 0.93–1.77 | |
| Yes (less than 3 months) | 1.56 1.00 | 1.19–2.05 0.64–1.56 | 1.47 1.04 | 1.09–1.97 0.64–1.69 | 1.28 1.04 | 0.93–1.77 0.61–1.76 | |
| Yes (greater than or equal to 3 months) | 1.59 | 0.99–2.56 | 1.83 | 1.09–3.06 | 2.08 | 1.17–3.69 | |
Table 6.
Crude and adjusted OR for doctor-diagnosed AR before 2011 and 2013 based on HD use in the past
| Characteristics | Category | Model 1a | Model 2b | Model 3c | |||
|---|---|---|---|---|---|---|---|
| OR | 95% CI | OR | 95% CI | OR | 95% CI | ||
| Diagnosed with AR before 2011 (the year when HDs were banned) | No | 1.00 | – | 1.00 | – | 1.00 | – |
| Yes | 1.27 | 0.92–1.83 | 1.36 | 0.94–1.95 | 1.21 | 0.83–1.76 | |
| Diagnosed with AR before 2013 (risk period) | Yes | 1.00 | – | 1.00 | – | 1.00 | – |
| No | 1.48 | 1.15–1.89 | 1.46 | 1.12–1.91 | 1.35 | 1.02–1.79 | |




 PDF
PDF Citation
Citation Print
Print


 XML Download
XML Download