Abstract
CT enterography and magnetic resonance (MR) enterography are widely used imaging modalities used to examine the small bowel. These radiologic tests are distinguished from routine abdominopelvic CT and MRI by the oral ingestion of a large amount of neutral contrast to distend the small bowel before scanning. For achievement of high quality, diagnostic images and proper technique are required. Conducted protocols still vary in patient preparation, enteric contrast, and CT and MRI acquisition sequences, resulting in heterogeneous diagnostic accuracy. The purpose of this article is to review the processes and techniques that optimize CT/MR enterography for patients with suspected Crohn's disease or other small bowel diseases.
Go to : 
References
1. Sturm A, Maaser C, Calabrese E, et al. ECCO-ESGAR guideline for diagnostic assessment in IBD part 2: IBD scores and general principles and technical aspects. J Crohns Colitis. 2019; 13:273–284.

2. Boone D, Taylor SA. Magnetic resonance of the small bowel: how to do it. Magn Reson Imaging Clin N Am. 2020; 28:17–30.
3. Park SH, Ye BD, Lee TY, Fletcher JG. Computed tomography and magnetic resonance small bowel enterography: current status and future trends focusing on Crohn's disease. Gastroenterol Clin North Am. 2018; 47:475–499.
5. Choi IY, Park SH, Park SH, et al. CT enterography for surveillance of anastomotic recurrence within 12 months of bowel resection in patients with Crohn's disease: an observational study using an 8-year registry. Korean J Radiol. 2017; 18:906–914.

6. Baker ME, Hara AK, Platt JF, Maglinte DD, Fletcher JG. CT enterography for Crohn's disease: optimal technique and imaging issues. Abdom Imaging. 2015; 40:938–952.

7. Fidler JL, Goenka AH, Fleming CJ, Andrews JC. Small bowel imaging: computed tomography enterography, magnetic resonance enterography, angiography, and nuclear medicine. Gastrointest Endosc Clin N Am. 2017; 27:133–152.
8. Pola S, Santillan C, Levesque BG, Feagan BG, Sandborn WJ. An overview of magnetic resonance enterography for Crohn's disease. Dig Dis Sci. 2014; 59:2040–2049.

9. Naganuma M, Hisamatsu T, Kanai T, Ogata H. Magnetic resonance enterography of Crohn's disease. Expert Rev Gastroenterol Hepatol. 2015; 9:37–45.

10. Greenup AJ, Bressler B, Rosenfeld G. Medical imaging in small bowel Crohn's disease-computer tomography enterography, magnetic resonance enterography, and ultrasound: "which one is the best for what?". Inflamm Bowel Dis. 2016; 22:1246–1261.
11. Tolan DJ, Greenhalgh R, Zealley IA, Halligan S, Taylor SA. MR en-terographic manifestations of small bowel Crohn disease. Radiographics. 2010; 30:367–384.

12. Masselli G, Guida M, Laghi F, Polettini E, Gualdi G. Magnetic resonance of small bowel tumors. Magn Reson Imaging Clin N Am. 2020; 28:75–88.

13. Mantarro A, Scalise P, Guidi E, Neri E. Magnetic resonance enterography in Crohn's disease: how we do it and common imaging findings. World J Radiol. 2017; 9:46–54.

14. Liu W, Liu J, Xiao W, Luo G. A diagnostic accuracy metaanalysis of CT and MRI for the evaluation of small bowel Crohn disease. Acad Radiol. 2017; 24:1216–1225.

15. Anupindi SA, Grossman AB, Nimkin K, Mamula P, Gee MS. Imaging in the evaluation of the young patient with inflammatory bowel disease: what the gastroenterologist needs to know. J Pediatr Gastroenterol Nutr. 2014; 59:429–439.
16. Takenaka K, Ohtsuka K, Kitazume Y, et al. Utility of magnetic resonance enterography for small bowel endoscopic healing in patients with Crohn's disease. Am J Gastroenterol. 2018; 113:283–294.

17. Manetta R, Capretti I, Belleggia N, et al. Magnetic resonance enterography (MRE) and ultrasonography (US) in the study of the small bowel in Crohn's disease: state of the art and review of the literature. Acta Biomed. 2019; 90(5-S):38–50.
18. Deepak P, Park SH, Ehman EC, et al. Crohn's disease diagnosis, treatment approach, and management paradigm: what the radiologist needs to know. Abdom Radiol (NY). 2017; 42:1068–1086.

19. Guglielmo FF, Anupindi SA, Fletcher JG, et al. Small bowel Crohn disease at CT and MR enterography: imaging atlas and glossary of terms. Radiographics. 2020 Jan 17. [Epub ahead of print].
20. Grand DJ, Harris A, Loftus EV Jr. Imaging for luminal disease and complications: CT enterography, MR enterography, small-bowel follow-through, and ultrasound. Gastroenterol Clin North Am. 2012; 41:497–512.

21. Gale HI, Sharatz SM, Taphey M, Bradley WF, Nimkin K, Gee MS. Comparison of CT enterography and MR enterography imaging features of active Crohn disease in children and adolescents. Pediatr Radiol. 2017; 47:1321–1328.

22. Kim JS, Jang HY, Park SH, et al. MR enterography assessment of bowel inflammation severity in Crohn disease using the MR index of activity score: modifying roles of DWI and effects of contrast phases. AJR Am J Roentgenol. 2017; 208:1022–1029.

23. Fidler JL, Guimaraes L, Einstein DM. MR imaging of the small bowel. Radiographics. 2009; 29:1811–1825.

24. Anupindi SA, Terreblanche O, Courtier J. Magnetic resonance enterography: inflammatory bowel disease and beyond. Magn Reson Imaging Clin N Am. 2013; 21:731–750.
25. Ahmed O, Rodrigues DM, Nguyen GC. Magnetic resonance imaging of the small bowel in Crohn's disease: a systematic review and metaanalysis. Can J Gastroenterol Hepatol. 2016; 2016:7857352.

26. Kahn J, Posch H, Steffen IG, et al. Is there long-term signal intensity increase in the central nervous system on T1-weighted images after MR imaging with the hepatospecific contrast agent gadoxetic acid? A cross-sectional study in 91 patients. Radiology. 2017; 282:708–716.

27. Fiorino G, Bonifacio C, Peyrin-Biroulet L, et al. Prospective comparison of computed tomography enterography and magnetic resonance enterography for assessment of disease activity and complications in ileocolonic Crohn's disease. Inflamm Bowel Dis. 2011; 17:1073–1080.

Go to : 
 | Fig. 1.Computed tomography enterography of active Crohn's disease. Axial image (A) showed bowel wall thickening, mucosal enhancement and edema (arrows). (B) Coronal image demonstrated mesenteric vessel engorgement (comb sign, arrow) with lymph node enlargement (arrowhead). (C, D) Coronal image (C) and axial image (D) noted star-shaped entero-enteric fistula (arrows). |
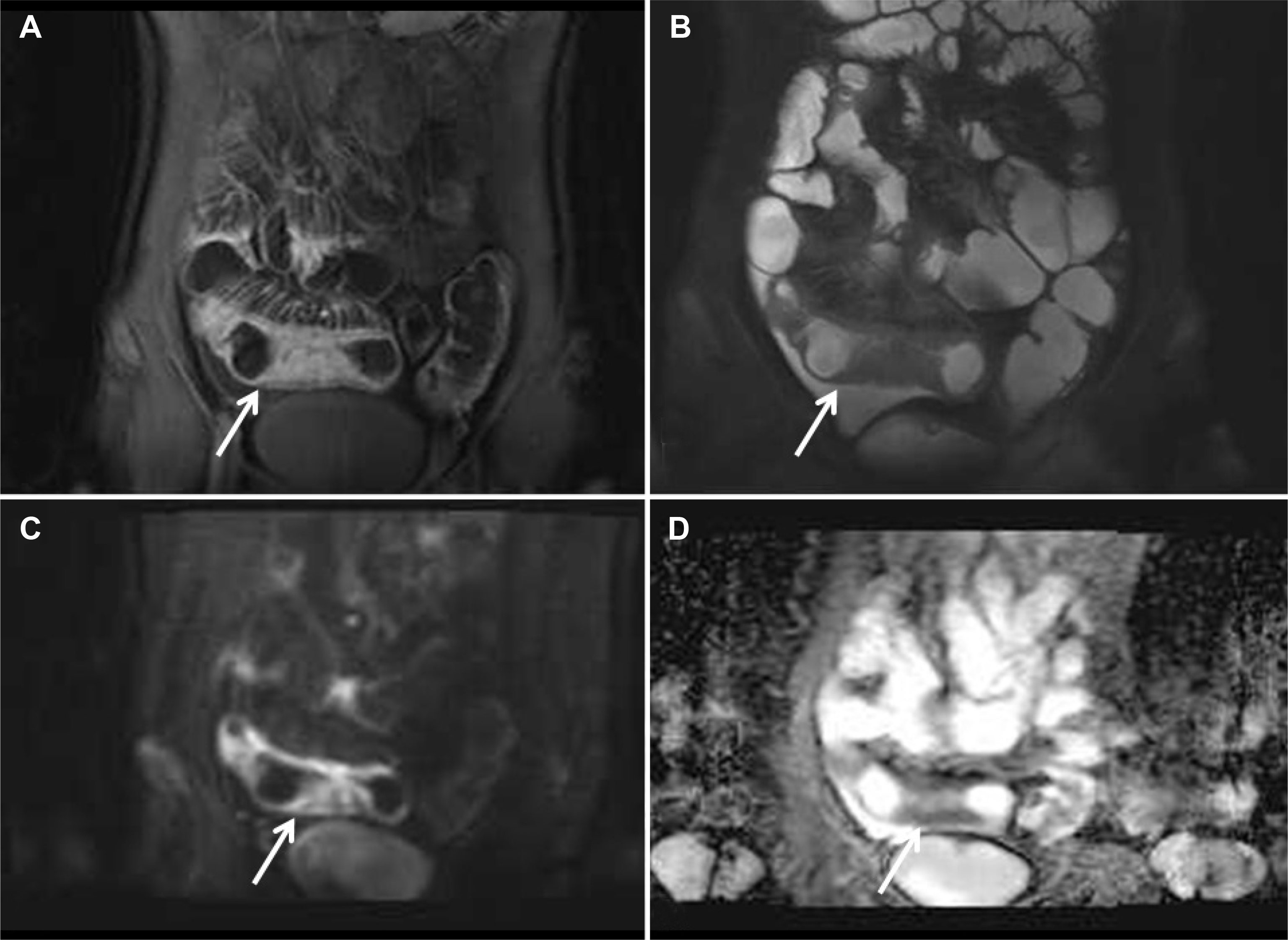 | Fig. 2.Magnetic resonance enterography of active Crohn's disease. (A) Coronal scan of postcontrast T1-weighted image showed mucosal enhancement, wall thickening (arrow), and mesenteric vessel engorgement. (B) Coronal scan of true fast imaging with steady-state precession (FISP) noted intermediate signal intensity of involved ileal segment (arrow). (C, D) Diffusion-weighted image (C, high b-value=1,000) and apparent diffusion coefficient (ADC) (D) images demonstrated diffusion restriction presenting active inflammation (arrows). |
Table 1.
Summary of International Consensus Guidance1,2,8,17
PEG, polyethylene glycol; MR, magnetic resonance; IV, intravenous; FSE, fast-spin echo; FS, fat saturation; SSFPGE, steady-state free precession gradient-echo; 3D, three-dimensional; GRE, gradient-echo; IBD, inflammatory bowel disease; s, seconds; GI, gastrointestinal; DWI, diffusion-weighted image; T2W, T2-weighted image; 2D, two-dimensional; T1W, T1-weighted image.
Table 2.
CT and MR Techniques in Common Clinical Settings that Require Examination of Small Bowel3,29




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download