Abstract
Background
The objective of the study was to determine the impact of continuous care on health outcomes and cost of type 2 diabetes mellitus (T2DM) in Korea.
Methods
A nationwide retrospective, observational case-control study was conducted. Continuity of treatment was measured using Continuity of Care (COC) score. Information of all patients newly diagnosed with T2DM in 2004 was retrieved from the National Health Insurance database for the period of 2002 to 2013. The study examined 2,373 patients after applying exclusion criteria, such as for patients who died from conditions not related to T2DM. Statistical analyses were performed using frequency distribution, simple analysis (t-test and chi-squared test), and multi-method analysis (simple linear regression, logistic regression, and survival analysis).
Results
The overall COC score was 0.8±0.24. The average incidence of diabetic complications was 0.39 per patient with a higher COC score, whereas it was 0.49 per patient with a lower COC score. In both survival and logistic analyses, patients who had high COC score were significantly less likely to have diabetic complications (hazard ratio, 0.69; 95% confidence interval, 0.54 to 0.88). The average medical cost was approximately 3,496 United States dollar (USD) per patient for patients with a higher COC score, whereas it was 3,973 USD per patient for patients with a lower COC score during the 2006 to 2013 period, with a difference of around 477 USD, which is statistically significant after adjusting for other factors (β=−0.152).
Diabetes is one of the most rapidly growing diseases in the world. The International Diabetes Federation has predicted that every 10 seconds, three patients are diagnosed with diabetes [1], and its prevalence rate around the world was 6.6% in 2010 [2]. It is estimated that 415 million people, aged 20 to 79, would be diagnosed with diabetes in 2015, and approximately 5 million people died from it. Moreover, the number of people with diabetes would be expected to be 642 million by 2040 [3]. According to the American Diabetes Association, the direct expenditures on diabetes by the United States government amounted to 91.8 billion United States dollar (USD) in 2002, and 156 billion USD in 2010. It has been estimated that by 2020, 192 billion USD will be spent on diabetes. In 2002, the United States government's total expenditures on health and medication were 865 billion USD; among others, 160 billion USD, equivalent to 18.5% of its total health expenditures, were used for diabetes. Health expenditures per capita in the United States were 2,560 USD in 2002, and this number will increase by 5-fold to 13,243 USD if the individual is a diabetes patient. Moreover, if age, sex, and ethnicity are adjusted, the heath expenditures per capita will increase by 2.4 times [4].
In addition, a constant increase in medical expenditures due to complications of diabetes, proven in several studies [567], is also a public concern. Cost Of Diabetes in Europe-Type 2 (CODE-2) diabetes studies carried out in seven countries in Europe, including over 7,000 participants, have suggested that medical expenditures on complications of diabetes would increase 1.7 times for patients who develop microangiopathy, two times for patients with macroangiopathy, and 3.5 times for those who develop both types of complications [7].
Through continuous care, however, it is possible to prevent patients with diabetes from further development of the disease and reduce their medical expenses. Regardless of the type of care or treatment, continuous care of diabetes is important because absence of treatment will eventually lead to hospitalization or a number of medical complications [8]. According to the Centers for Disease Control and Prevention, patients with diabetes are 1.5 to 1.8 times more likely to be hospitalized from heart disease or stroke than patients who do not have diabetes. Cases of lower-extremity amputation due to diabetes have increased from 73,000 in 2010 to 108,000 in 2014 [910].
In the case of chronic diseases such as diabetes or hypertension, because the duration of the illness is so long, there are many cases in which the patient frequently changes medical institutions, which distorts usage behavior of medical services by casting about for a better medical practitioner [111213]. If a patient visits different medical institutions for the same disease, it reduces continuity of care because patients need to be re-examined, requiring new physical examinations and laboratory and radiological tests for the same symptoms.
The objective of this study, therefore, was to analyze the effect of Continuity of Care (COC) on health outcomes and health care costs for patients with type 2 diabetes mellitus (T2DM), using the Korean National Health Insurance database.
This study uses data from the Korean National Health Insurance database gathered between 2002 and 2013. Information about one million people (2% of the whole population) was extracted from the nation's health insurance claims data, including socioeconomic status, disability, death, and use of medical care institutions. Data about patients aged 20 years old or over who were newly diagnosed with T2DM in 2004 were collected for the study.
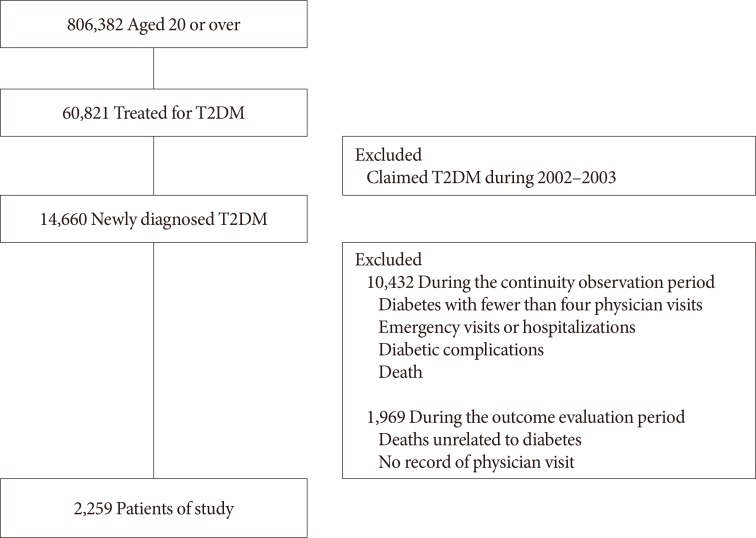
The observation period of the study is 10 years, consisting of two periods, the first one observing whether managing diabetes continuously for 2 years after initial diagnosis (continuity observation), and the following one observing the health outcome for 8 years thereafter (outcome evaluation). We excluded patients from the analysis who had fewer than four physician visits [14], had a record of emergency visits or hospital admission during the continuous observation period, had diabetic complications, or died within the first 2 years of initial diagnosis. In addition, patients who had no record of physician visits or who died for conditions not related to T2DM during the 8-year period were also excluded. In the end, the data from 2,259 patients in total were eligible for analysis (Fig. 1).
Most Frequent Provider Continuity (MFPC), Modified Continuity Index (MCI), and COC index have been used as measures for continuous care [1415161718192021]. We selected the COC index as the measure for continuity measure in this study. The COC index, developed by Bice and Boxerman [22], has all four characteristics for measurement of continuity defined by Shortell [23], which are (1) use of individuals as units of analysis, (2) the comparability of individuals using different numbers of providers, (3) the influence of total number of visits, and (4) referral patterns among providers. Therefore, it considers both the degree of concentration and dispersion of the medical providers visited by patients and is appropriate for measures that do not require an assigned provider as in Korea. It has been applied in a relatively large number of studies [24]. The values of the COC index range from 0 to 1, where 0 is when all physician visits are distributed to different providers, and 1 is when all physician visits are concentrated at one provider. The calculation formula is as follows.
To evaluate health outcome, the occurrence of diabetic complications was measured. Diabetic complications can be categorized by size of blood vessels involved in macro- and microvascular origins. Macrovascular complications affect the heart and large blood vessels and are probably the major cause of morbidity and mortality among diabetic patients. These are coronary artery disease, peripheral arterial disease, and stroke. Complications of microvascular origin include diabetic retinopathy, nephropathy, and neuropathy [725].
We referred to the study by Park et al. [26] for the medical diagnosis codes of these complications. When the patients with T2DM had either micro- or macrovascular complications or both, we defined them as having diabetic complications.
For health care costs, we calculated total medical costs incurred for T2DM during the outcome evaluation period. Direct, indirect, and intangible costs have been used to calculate medical costs [27], but we selected only direct costs as total medical costs. Direct costs are defined as all costs directly occurred for medical services such as diagnosis, treatment, care, rehabilitation, and terminal care without including non-medical costs such as transportation. We used health insurance claims data and added up all expenses related to T2DM claims. The computation of medical expenses started at the end of the continuity evaluation period, and ended at the end of the study (December 31, 2013), so the period differs with each patient.
As control variables, we examined patients' socioeconomic status, characteristics of disease and medical treatment, and features of medical institutions. Patients' socioeconomic status, such as age, insurance type, and income quintile, were variables that could be changed during the study period, so they were based on the time of the first diagnosis. The characteristics of the medical institutions, such as types, ownership, number of beds, and number of physicians, were based on the most visited medical institutions during the continuity observation period. According to previous studies [282930], the most visited medical institution was defined as the main medical institution during the continuity observation period. However, if there were medical institutions that had identical frequencies of visits in the same year, the most recently visited medical institution was defined as the main one.
Multivariate analysis was performed to examine the impact of continuous care on the occurrence of diabetic complications and medical costs. The Cox proportional hazards regression model was fitted to examine the hazard ratios (HRs) between continuous care and health complications of T2DM after adjusting other factors. In addition, the multivariate logistic analysis was performed to confirm the robustness of the obtained results.
The adjusted confounding factors included patients' characteristics, such as age, gender, health security type, income level, disease characteristics (hypoglycemic agents, Charlson comorbidity score), and institutional characteristics, such as types of health care providers, ownership, geographical location, number of physicians, and number of beds. Types of health security are categorized into two types: National Health Insurance and Medical Aid. Types of health care providers were categorized into three types: general hospital, hospital, and clinic. Institutional ownership was divided into three categories: national/public, corporate, and private.
Statistical analyses were performed using STATA software version 14.0 (StataCorp LP., College Station, TX, USA). Ethical approval for this study was obtained from the Catholic Medical Center Institutional Review Board (MC15RNSI0043). Informed consent was waived by the board.
Characteristics of the study subjects at the time of their first diagnosis are shown in Table 1. The portion of males was about 11% higher than of females. The age distribution was skewed toward subjects over 50 years of age. A significant number of respondents were in income level 1 to 2 or 9 to 10, both equally 28.0%. Most patients used clinics (75.9%), medical institutions in the private sector (79.6%), institutions with 0 to 50 beds (75.7%), and with one physician (59.4%). The overall COC score was 0.83±0.24.
Because COC values were skewed (−1.073), we divided continuity scores into two groups, higher and lower, based on the median. Table 1 shows the baseline characteristics of included patients in the high-COC and low-COC groups. Among the patients' characteristics, sex, age, insurance status, and comorbidity score were statistically significant variables. In the higher continuity group, the proportion of males aged 60 or younger, with Medical Aid and a comorbidity score of 1 or above, were high. As for the characteristics of medical institutions, types of medical institution, and number of physicians were the significant variables. The proportion of general hospital and medical institutions with more than 21 physicians were high in the higher continuity group.
A little less than half (n=982, 43.5%) of the whole study population had diabetic complications. The incidence of microvascular and macrovascular complications among the study population were 875 (38.7%) and 310 (13.7%), respectively. When the COC score was high, 39.2% (513 out of 1,310 participants) of these patients developed health complications. However, when the COC score was low, 49.4% of these patients had complications. Definitely, these are statistically significant (Table 2).
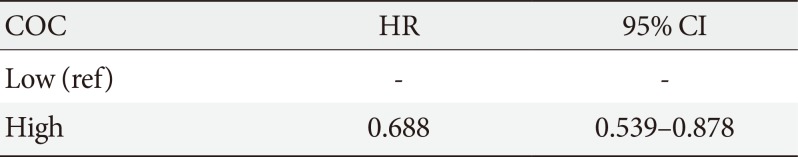
In the multivariate Cox analysis, the COC was found to be significantly associated with T2DM complications after adjusting for other factors, including patient characteristics (sex, age, insurance type, income), disease characteristics (hypoglycemic agent, comorbidity score), and medical institution characteristics (type, ownership, region, number of physicians, and number of beds). The risk of having T2DM complications among patients who had higher COC scores was 0.69 times (95% confidence interval [CI], 0.539 to 0.878), significantly lower than those who had lower COC scores (Table 3). Patients' gender, age, income level, and type of hospital at diagnosis were also significantly associated with T2DM complications. The results of the multiple logistic regression of higher-COC patients on diabetic complications showed an odds ratio of 0.55 (95% CI, 0.40 to 076) so that supports the robustness of COC scores as the survival analysis of having no diabetes complications.
The risk of having microvascular and macrovascular complications among patients with higher COC scores were 0.66 times (95% CI, 0.509 to 0.856) and 0.92 times (95% CI, 0.582 to 1.467) higher, respectively, than those with lower COC scores.
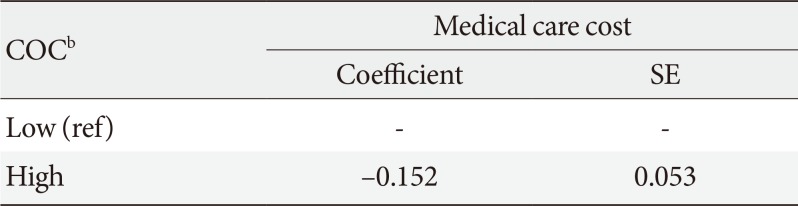
The average health care cost for patients with T2DM during the outcome evaluation period was about 3,696 USD. After analyzing the relationship between COC score and diabetes treatment costs from 2006 to 2013, the average medical costs for treating T2DM was around 3,496 USD for patients with a high COC score, whereas it was around 3,973 USD for patients with a low COC score, an increase of 477 USD, which was not statistically significant (Table 2). However, after adjusting for the other factors, medical costs incurred for patients with T2DM were significantly lower for patients with a high COC score compared to those for patients with a low COC score (Table 4).
The effects of continuity of treatment for T2DM on diabetic complications and health care costs were assessed using the National Health Insurance cohort database (2002 to 2013). Continuity of care was evaluated based on managing diabetes continuously for 2 years after initial diagnosis during the continuity observation period and the diabetes-related complications for the 8 years of follow-up thereafter during the outcome evaluation period. The COC index was used to evaluate continuous care. The total costs of diabetes treatment were measured based on the outcome evaluation period (8 years). The results of this study demonstrated that high COC significantly reduced the risk of diabetes-related complications (HR, 0.69) and medical costs (3,496 USD vs. 3,973 USD) compared with low-COC patients with T2DM.
Patients with T2DM are at significant risk for a number of complications, such as retinopathy, renal disease, and heart disease [31]. The prevalence of retinopathy is related to the duration of diabetes and is regarded as the most substantial cause of blindness among adults aged 20 to 74 years [32]. The rate of cardiovascular disease is relatively high among patients with T2DM, resulting in an increased mortality rate compared with the general population [333435]. These complications related to diabetes, however, can be reduced by continuity of care, because it may lead to escalating the likelihood of cancer screening [36] and to increasing follow-up appointments [37]. In fact, continuity of care with a primary care provider is associated with better glucose control among patients with T2DM, with a fairly high probability of detecting minor conditions at earlier stages to reduce the incidence of diabetes complications and incur fewer hospital admissions [1838]. This study also reports the positive effect of continuity of care for people with diabetes, as do previous studies. Patients who received high COC score are significantly less likely to have diabetic complications. Furthermore, patients with high COC scores have higher chances of survival. The COC score in the study was 0.83±0.24. In other studies, it was 0.84±0.17 for 3 years [15] or ranged from 0.64 to 0.66, using only diabetes-related visits between 2001 and 2006 [18].
Another issue is economic burdens on the health care system as well as on patients. Direct medical costs (91.8 billion USD in 2002) in the United States comprise 25.3% for diabetes care, and 26.8% for chronic complications attributable to diabetes [4]. The age-gender weighted average of lifetime medical costs for diabetic patients in the United States is 85,200 USD, of which 53% is due to treating diabetic complications, based on data from 2009 to 2010 from the National Health and Nutrition Examination Survey [8]. Continuity of care, however, leads to decreasing medical costs from patients with diabetes. In other words, there is a general reduction in health care costs as continuity of care improves [153940]. Moreover, patients who do not fulfill continuity of care are more likely to spend more in medical costs than those who carry out continuity of care [41]. In this study, the average medical cost is approximately 3,496 USD per patient for patients with a higher COC score, whereas it is 3,973 USD per patient for patients with a lower COC score. So the study finds results consistent with those of previous studies. Diabetics with higher COC scores had significantly lower medical expenses than those with lower COC scores after adjusting for other factors (β=−0.152).
This study is meaningful in the sense that it uses national claims-based data to verify the relationship between COC and medical costs and health outcomes for diabetes patients. However, the use of secondary data in the analysis created a few limitations. First, this research considered only available variables in the claims database, such as patients' socioeconomic status, characteristics of disease, and medical institution, that could affect diabetes patients' health outcome. It did not consider commonly addressed socio-behavioral characteristics in most studies of chronic conditions. For example, Kim et al. [42] explained that a patient's occupation, education, and family history can affect continuity of care. Ji [43] also stated that factors such as drinking and smoking habits, obesity, stress level, and average sleep hours can affect a patient's ability to control glycemic hemoglobin. However, these factors were not considered in this research. Severity of diabetes was not properly considered; this research instead applied the Charlson comorbidity score to consider the patient's overall health condition. In the study by Cho et al. [30], the prescription of hypoglycemic agents (types and number) and comorbidity index together were used to consider the severity of the disease. In this study, prescriptions of hypoglycemic agents and comorbidity score were also considered to adjust for the severity of diabetes.
Second, out of all direct costs, this research only considered medical cost to calculate the cost of diabetes. It fails to recognize that diabetes is a chronic disease that lasts for a long period of time. To manage this disease, a significant portion of the cost could be taken up by direct nonmedical costs, such as time, and transportation cost, and indirect cost such as decrease of income incurred by productivity loss and death. Even if direct medical costs had been calculated, it only considered the covered benefit costs of medical care services.
This study demonstrated, by using the National Health Insurance cohort database, that continuity of care has significant impacts on complications and medical costs of patients with T2DM. Despite the limitations of the study variables and design due to the nature of the NHI cohort data, there would be no difficulty in generalizing the results. Last, this study will be valuable for clinicians in understanding the concept and utility of care continuity.
References
1. International Diabetes Federation. IDF diabetes atlas. 5th ed. Brussels: International Diabetes Federation;2011.
2. International Diabetes Federation. IDF diabetes atlas. 4th ed. Brussels: International Diabetes Federation;2009.
3. Ogurtsova K, da Rocha Fernandes JD, Huang Y, Linnenkamp U, Guariguata L, Cho NH, Cavan D, Shaw JE, Makaroff LE. IDF diabetes atlas: global estimates for the prevalence of diabetes for 2015 and 2040. Diabetes Res Clin Pract. 2017; 128:40–50. PMID: 28437734.

4. Hogan P, Dall T, Nikolov P. American Diabetes Association. Economic costs of diabetes in the US in 2002. Diabetes Care. 2003; 26:917–932. PMID: 12610059.
5. Brandle M, Zhou H, Smith BR, Marriott D, Burke R, Tabaei BP, Brown MB, Herman WH. The direct medical cost of type 2 diabetes. Diabetes Care. 2003; 26:2300–2304. PMID: 12882852.

6. Clarke P, Gray A, Legood R, Briggs A, Holman R. The impact of diabetes-related complications on healthcare costs: results from the United Kingdom Prospective Diabetes Study (UKPDS Study No. 65). Diabet Med. 2003; 20:442–450. PMID: 12786677.

7. Williams R, Van Gaal L, Lucioni C. CODE-2 Advisory Board. Assessing the impact of complications on the costs of type II diabetes. Diabetologia. 2002; 45:S13–S17.

8. Zhuo X, Zhang P, Hoerger TJ. Lifetime direct medical costs of treating type 2 diabetes and diabetic complications. Am J Prev Med. 2013; 45:253–261. PMID: 23953350.

9. Centers for Disease Control and Prevention: National diabetes statistics report, 2014. cited 2019 Aug 30. Available from: https://www.cdc.gov/diabetes/pdfs/data/2014-report-estimates-of-diabetes-and-its-burden-in-the-united-states.pdf.
10. Centers for Disease Control and Prevention: National diabetes statistics report, 2017. cited 2019 Aug 30. Available from: https://www.cdc.gov/diabetes/pdfs/data/statistics/national-diabetes-statistics-report.pdf.
11. Kim SA. The selection of the medical institutions by severity of disease [dissertation]. Seoul: Yonsei University;2011.
12. Kim JY. The selection of the medical institutions by motivation of medical service utilization. J Digit Converg. 2015; 13:217–230.

13. Park EJ, Jeon JA, Kim DE, Song ES, Choi SJ, Shim BR. Healthcare service utilization among Korean patients with chronic disease: focusing on hypertension and type 2 diabetes mellitus. Sejong: Korea Institute for Health and Social Affairs;2016.
14. Lin W, Huang IC, Wang SL, Yang MC, Yaung CL. Continuity of diabetes care is associated with avoidable hospitalizations: evidence from Taiwan’s National Health Insurance scheme. Int J Qual Health Care. 2010; 22:3–8. PMID: 20007170.

15. Worrall G, Knight J. Continuity of care is good for elderly people with diabetes: retrospective cohort study of mortality and hospitalization. Can Fam Physician. 2011; 57:e16–e20. PMID: 21252120.
16. Hanafi NS, Abdullah A, Lee PY, Liew SM, Chia YC, Khoo EM. Personal continuity of care in a university-based primary care practice: impact on blood pressure control. PLoS One. 2015; 10:e0134030. PMID: 26214304.

17. Tsai HY, Chou YJ, Pu C. Continuity of care trajectories and emergency room use among patients with diabetes. Int J Public Health. 2015; 60:505–513. PMID: 25779687.

18. Chen CC, Chen SH. Better continuity of care reduces costs for diabetic patients. Am J Manag Care. 2011; 17:420–427. PMID: 21756012.
19. Tom JO, Tseng CW, Davis J, Solomon C, Zhou C, Mangione-Smith R. Missed well-child care visits, low continuity of care, and risk of ambulatory care-sensitive hospitalizations in young children. Arch Pediatr Adolesc Med. 2010; 164:1052–1058. PMID: 21041598.

20. Litaker D, Ritter C, Ober S, Aron D. Continuity of care and cardiovascular risk factor management: does care by a single clinician add to informational continuity provided by electronic medical records? Am J Manag Care. 2005; 11:689–696. PMID: 16268752.
21. Younge R, Jani B, Rosenthal D, Lin SX. Does continuity of care have an effect on diabetes quality measures in a teaching practice in an urban underserved community? J Health Care Poor Underserved. 2012; 23:1558–1565. PMID: 23698670.

22. Bice TW, Boxerman SB. A quantitative measure of continuity of care. Med Care. 1977; 15:347–349. PMID: 859364.

23. Shortell SM. Continuity of medical care: conceptualization and measurement. Med Care. 1976; 14:377–391. PMID: 1271879.
24. Saultz JW. Defining and measuring interpersonal continuity of care. Ann Fam Med. 2003; 1:134–143. PMID: 15043374.

25. Fowler MJ. Microvascular and macrovascular complications of diabetes. Clin Diabetes. 2008; 26:77–82.

26. Park CM, Jang SM, Jang SH, Lee HJ. Healthcare cost and outcome affected by continuity of care (hypertension and diabetes). Seoul: Health Insurance Review and Assessment Service;2011.
27. Hodgson TA, Meiners MR. Cost-of-illness methodology: a guide to current practices and procedures. Milbank Mem Fund Q Health Soc. 1982; 60:429–462. PMID: 6923138.

28. Hong JS, Kim JY. Study on continuity of primary care for Korean elderly. Seoul: Health Insurance Review and Assessment Service;2007.
29. Chen CC, Tseng CH, Cheng SH. Continuity of care, medication adherence, and health care outcomes among patients with newly diagnosed type 2 diabetes: a longitudinal analysis. Med Care. 2013; 51:231–237. PMID: 23269110.
30. Cho KH, Lee SG, Jun B, Jung BY, Kim JH, Park EC. Effects of continuity of care on hospital admission in patients with type 2 diabetes: analysis of nationwide insurance data. BMC Health Serv Res. 2015; 15:107. PMID: 25879858.

31. Mainous AG 3rd, Koopman RJ, Gill JM, Baker R, Pearson WS. Relationship between continuity of care and diabetes control: evidence from the third National Health and Nutrition Examination Survey. Am J Public Health. 2004; 94:66–70. PMID: 14713700.

32. American Diabetes Association. Standards of medical care for patients with diabetes mellitus. Diabetes Care. 2003; 26:S33–S50. PMID: 12502618.
33. Vijan S, Stevens DL, Herman WH, Funnell MM, Standiford CJ. Screening, prevention, counseling, and treatment for the complications of type II diabetes mellitus. Putting evidence into practice. J Gen Intern Med. 1997; 12:567–580. PMID: 9294791.
34. Krolewski AS, Czyzyk A, Janeczko D, Kopczynski J. Mortality from cardiovascular diseases among diabetics. Diabetologia. 1977; 13:345–350. PMID: 913925.

35. Panzram G. Mortality and survival in type 2 (non-insulin-dependent) diabetes mellitus. Diabetologia. 1987; 30:123–131. PMID: 3556287.

36. O'Malley AS, Mandelblatt J, Gold K, Cagney KA, Kerner J. Continuity of care and the use of breast and cervical cancer screening services in a multiethnic community. Arch Intern Med. 1997; 157:1462–1470. PMID: 9224225.
37. Sweeney KG, Gray DP. Patients who do not receive continuity of care from their general practitioner: are they a vulnerable group? Br J Gen Pract. 1995; 45:133–135. PMID: 7772390.
38. Parchman ML, Pugh JA, Noel PH, Larme AC. Continuity of care, self-management behaviors, and glucose control in patients with type 2 diabetes. Med Care. 2002; 40:137–144. PMID: 11802086.

39. Raddish M, Horn SD, Sharkey PD. Continuity of care: is it cost effective. Am J Manag Care. 1999; 5:727–734. PMID: 10538452.
40. Weiss LJ, Blustein J. Faithful patients: the effect of long-term physician-patient relationships on the costs and use of health care by older Americans. Am J Public Health. 1996; 86:1742–1747. PMID: 9003131.

41. Kim J, Kim H, Kim H, Min KW, Park SW, Park IB, Park JH, Baik SH, Son HS, Ahn CW, Oh JY, Lee S, Lee J, Chung CH, Choi KM, Choi I, Kim DJ. Current status of the continuity of ambulatory diabetes care and its impact on health outcomes and medical cost in Korea using National Health Insurance Database. J Korean Diabetes Assoc. 2006; 30:377–387.

Table 1
Characteristics of patients by groups of COC index score (%)
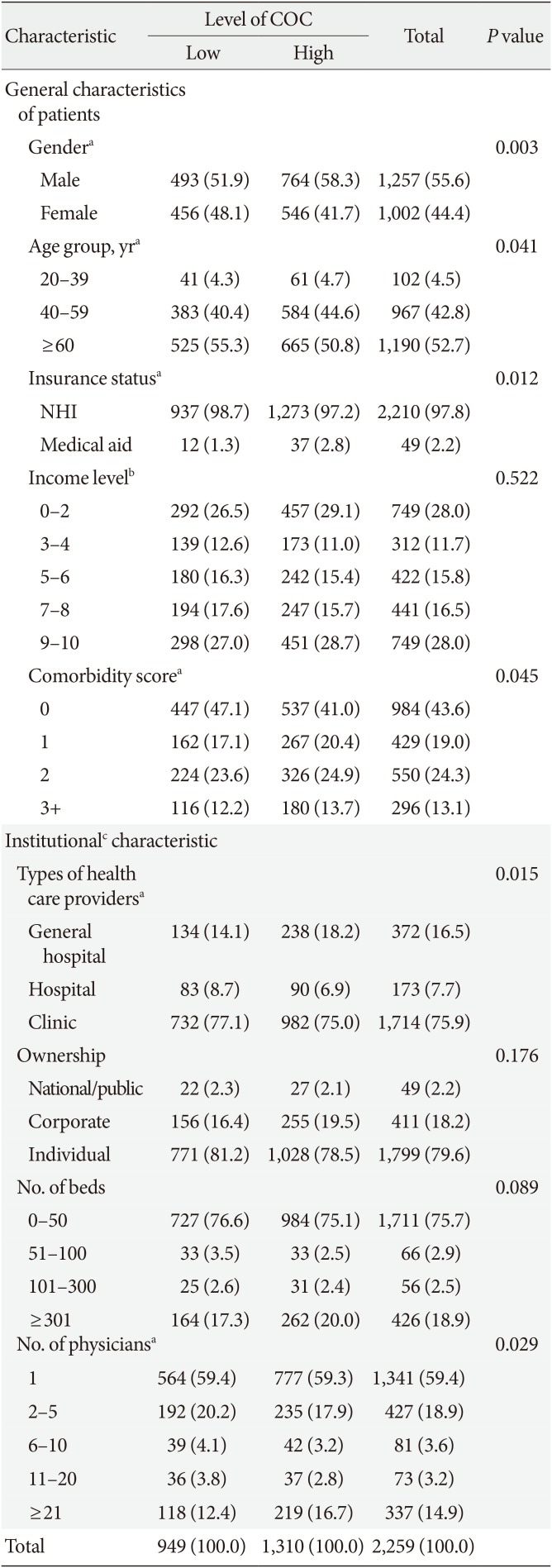
Table 2
Distribution of diabetic complications and medical costs for different COC levels
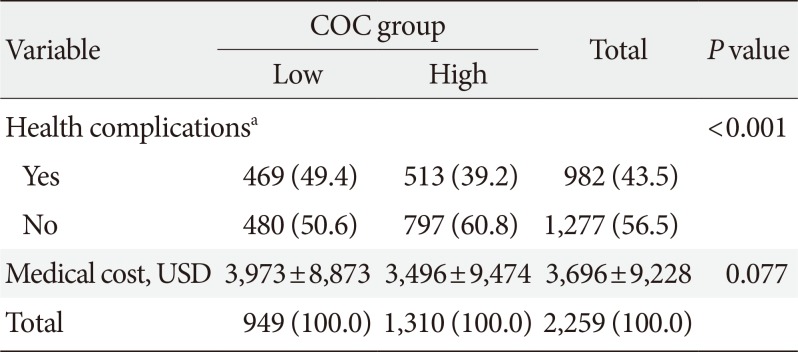
Table 3
Multivariate Cox survival analysis on risk of diabetic complications for different levels of COC, adjusting for other factorsa
| COC | HR | 95% CI |
|---|---|---|
| Low (ref) | - | - |
| High | 0.688 | 0.539–0.878 |
Table 4
Results of multiple linear regression for medical cost of treating type 2 diabetes mellitus and COC, adjusting for other factorsa
| COCb | Medical care cost | |
|---|---|---|
| Coefficient | SE | |
| Low (ref) | - | - |
| High | 0.688 | 0.539–0.878 |
COC, Continuity of Care; SE, standard error.
aOther factors include characteristics of patients (sex, age, health security type, income level, hypoglycemic agent, comorbidity) and medical care institutions (types, ownership, region, number of physicians, number of beds), bStatistically significant at α=0.05.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



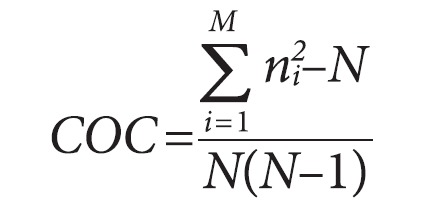

 XML Download
XML Download