Abstract
Purpose
Pediatric intra-articularproximal phalangeal head fractures of the big toe are very rare and few studies on this have been published. The purpose of this study is to present the diagnostic approach and surgical management of these extremely rare fractures, which might be easily underestimated or misdiagnosed.
Materials and Methods
The study retrospectively reviewed all the patients who were diagnosed as intra-articular proximal phalangeal head fracture of the big toe and who underwent surgical intervention in our institution. The size of the bony fragment and hallux valgus interphalangeus angle were measured on the preoperative X-rays. The size and rotation of the osteochondral fragment, the presence of avascular necrosis, ligamentous injury and soft tissue entrapment were assessed on the preoperative magnetic resonance images (MRIs). The radiologic and functional evaluation were performed at 1 year postoperatively.
Results:
The average size of the bony fragments measured on the X-rays was 4.1 mm in width and 2.3 mm in length. Two cases showed hallux valgus interphalangeus. Preoperative MRI was performed in four cases and the average size of any osteochondral lesion was 5.3 mm in width, 3.9 mm in length, and 4.7 mm in height. Rotation of the osteochondral fragment was observed in one patient, and soft tissue entrapment was noted in two patients. Postoperatively, successful bony union was achieved in all the patients and the average time to union was 74.4 days.
Conclusion
Intra-articular proximal phalangeal head fractures of the big toe are very rare and often neglected due to incomplete ossification in the pediatric population. It is important to suspect the presence of this intra-articular fracture and to appropriately implement further evaluation. Nonunion of chronic cases as well as acute fractures can be successfully treated through open reduction and internal fixation using multiple K-wires.
Go to : 
References
1. Salleh R, Beischer A, Edwards WH. Disorders of the hallucal interphalangeal joint. Foot Ankle Clin. 10:129–140. 2005.

2. Maffulli N. Epiphyseal injuries of the proximal phalanx of the hallux. Clin J Sport Med. 11:121–123. 2001.

3. Kim S, Lee M, Seok S. Intra-articular fracture of proximal phalanx of great toe accompanied by valgus deformity associated with sports activities. J Orthop Surg (Hong Kong). 25:2309499017690324. 2017.

4. Kramer DE, Mahan ST, Hresko MT. Displaced intraarticular fractures of the great toe in children: intervene with caution! J Pediatr Orthop. 34:144–149. 2014.
5. Shin YW, Choi IH, Rhee NK. Open lateral collateral ligament injury of the interphalangeal joint of the great toe in adolescents during Taekwondo. Am J Sports Med. 36:158–161. 2008.

6. Van Zeeland NL, Bae DS, Goldfarb CA. Intra-articular radial head fracture in the skeletally immature patient: progressive radial head subluxation and rapid radiocapitellar degeneration. J Pediatr Orthop. 31:124–129. 2011.
7. Shimizu A, Watanabe S, Kamada K, Tsuboi I, Yamamoto H. Hallux valgus interphalangeus following osteochondral fracture of the proximal phalanx: a case report. Foot Ankle Int. 26:994–996. 2005.

8. Gong HS, Kim YH, Park MS. Varus instability of the hallux interphalangeal joint in a taekwondo athlete. Br J Sports Med. 41:917–919. 2007.

9. Kay RM, Tang CW. Pediatric foot fractures: evaluation and treatment. J Am Acad Orthop Surg. 9:308–319. 2001.

10. Bariteau JT, Murillo DM, Tenenbaum SA, Brodsky JW. Joint salvage after neglected intraarticular physeal fracture of the hallux in high-level gymnasts. Foot Ankle Spec. 8:130–134. 2015.

11. Buch BD, Myerson MS. Salter-Harris type IV epiphyseal fracture of the proximal phalanx of the great toe: a case report. Foot Ankle Int. 16:216–219. 1995.

12. Perugia D, Fabbri M, Guidi M, Lepri M, Masi V. Salter-Harris type III and IV displaced fracture of the hallux in young gymnasts: a series of four cases at 1-year follow-up. Injury. 45(Suppl 6):S39–S42. 2014.

Go to : 
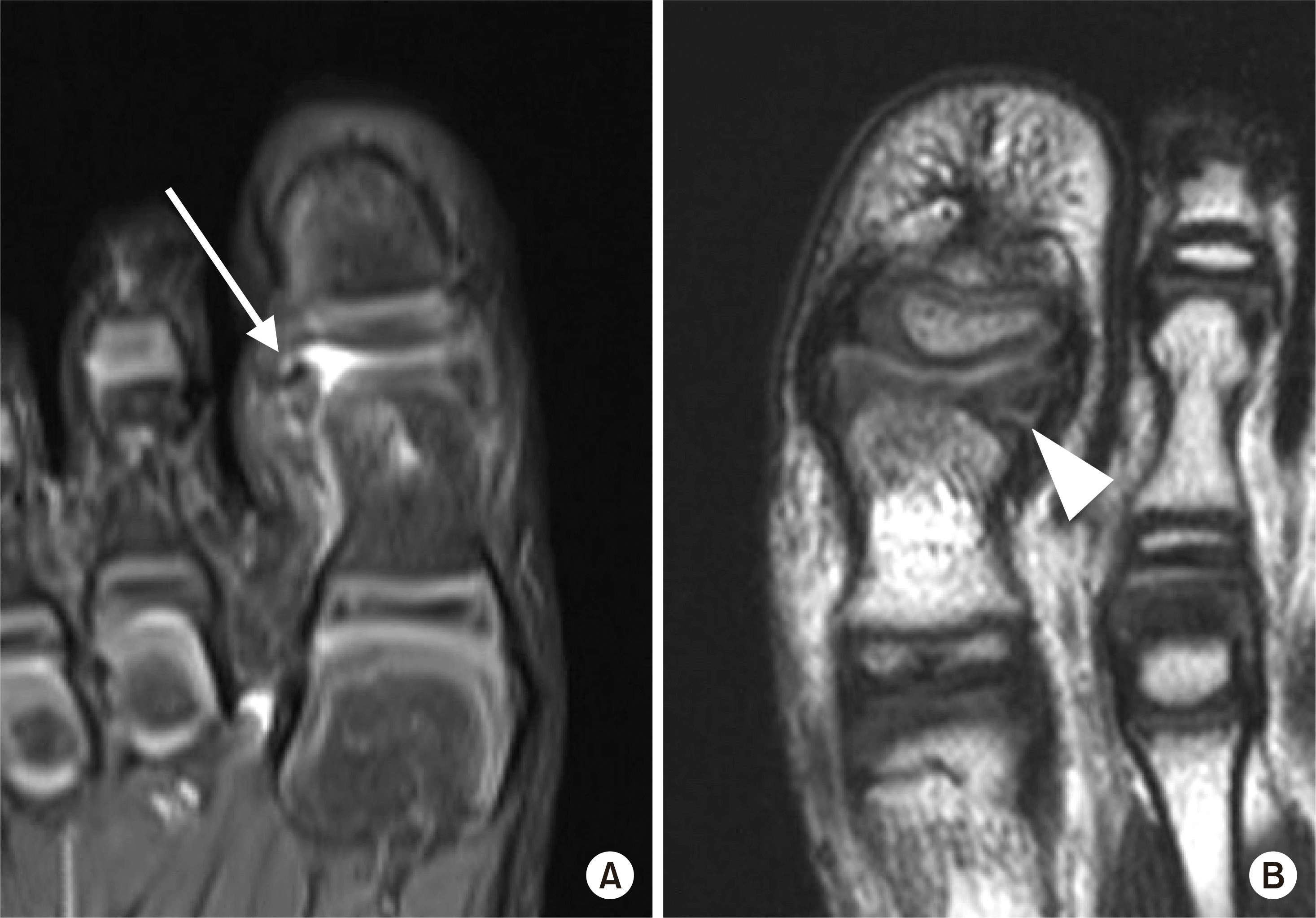 | Fig. 2.(A) Rotation of the osteochondral fragment (arrow). (B) Entrapment of the periosteum in the fracture site (arrowhead). |
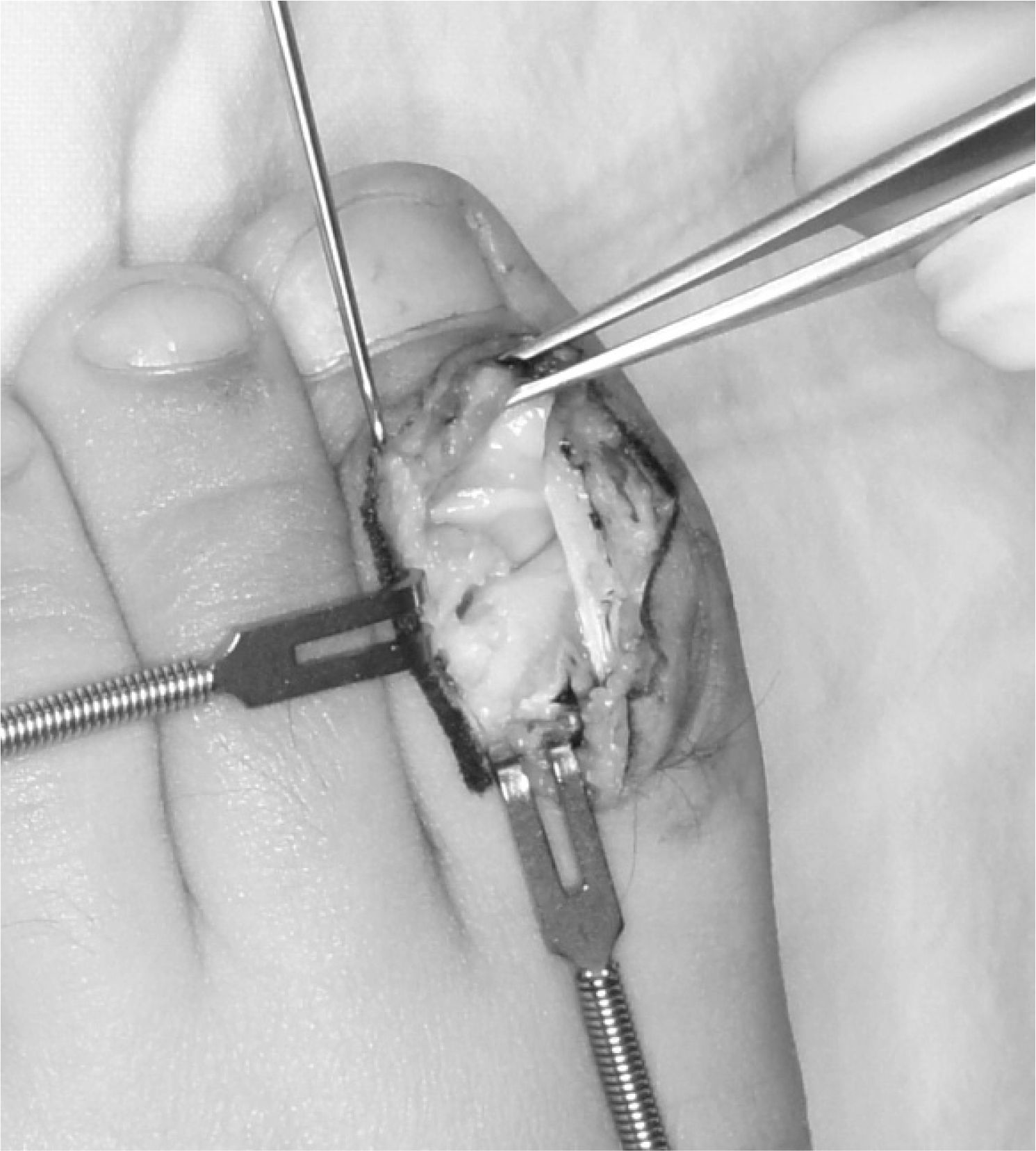 | Fig. 3.The joint surface was exposed through the dorsal approach. Sclerotic margin of the fracture site was observed. |
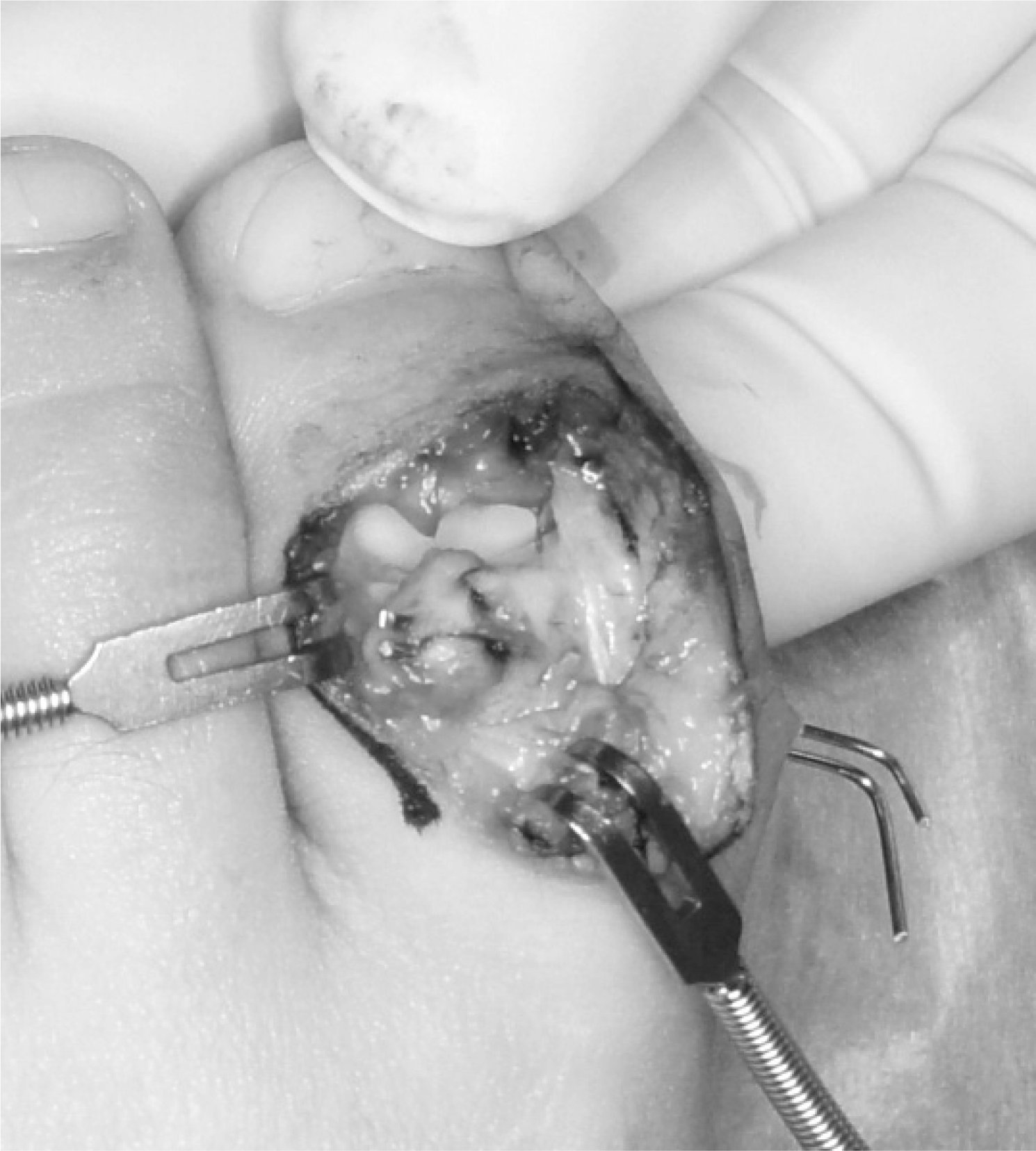 | Fig. 4.A K-wire was inserted into the fragment and retracted from the opposite side to avoid unwanted traction when removing the wire. |
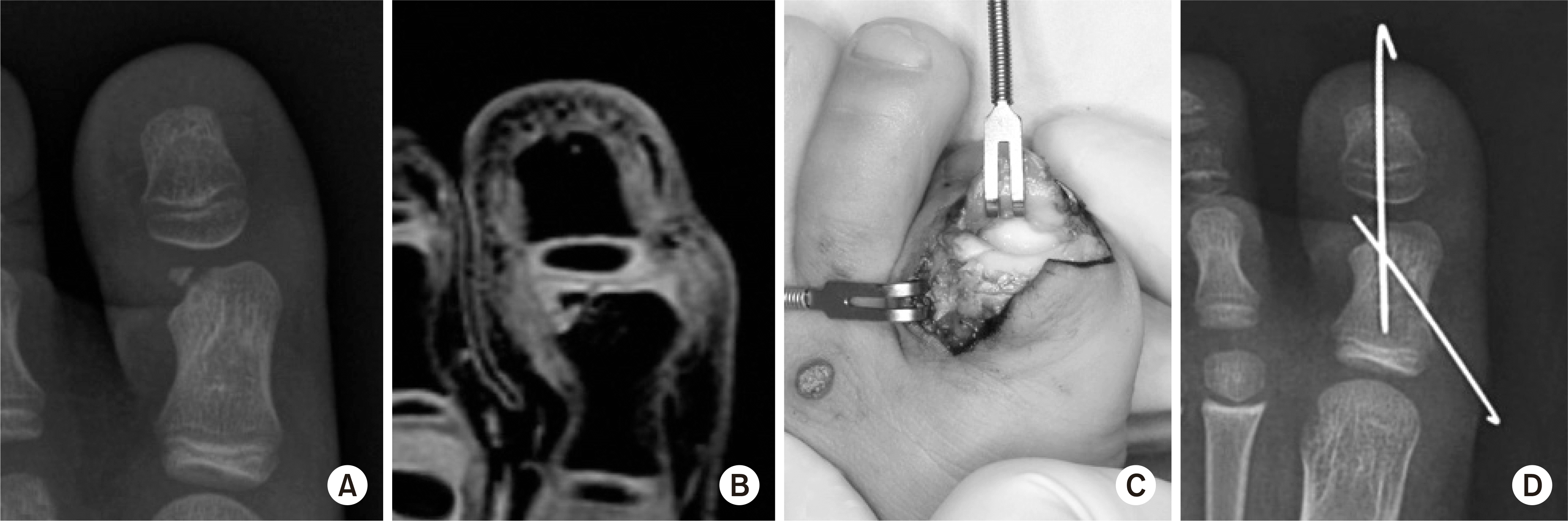 | Fig. 5.(A, B) The size of the osteochondral fragment might be underestimated on the plain X-ray. (C, D) Minimally displaced osteochondral fracture was fixed with two K-wires. |
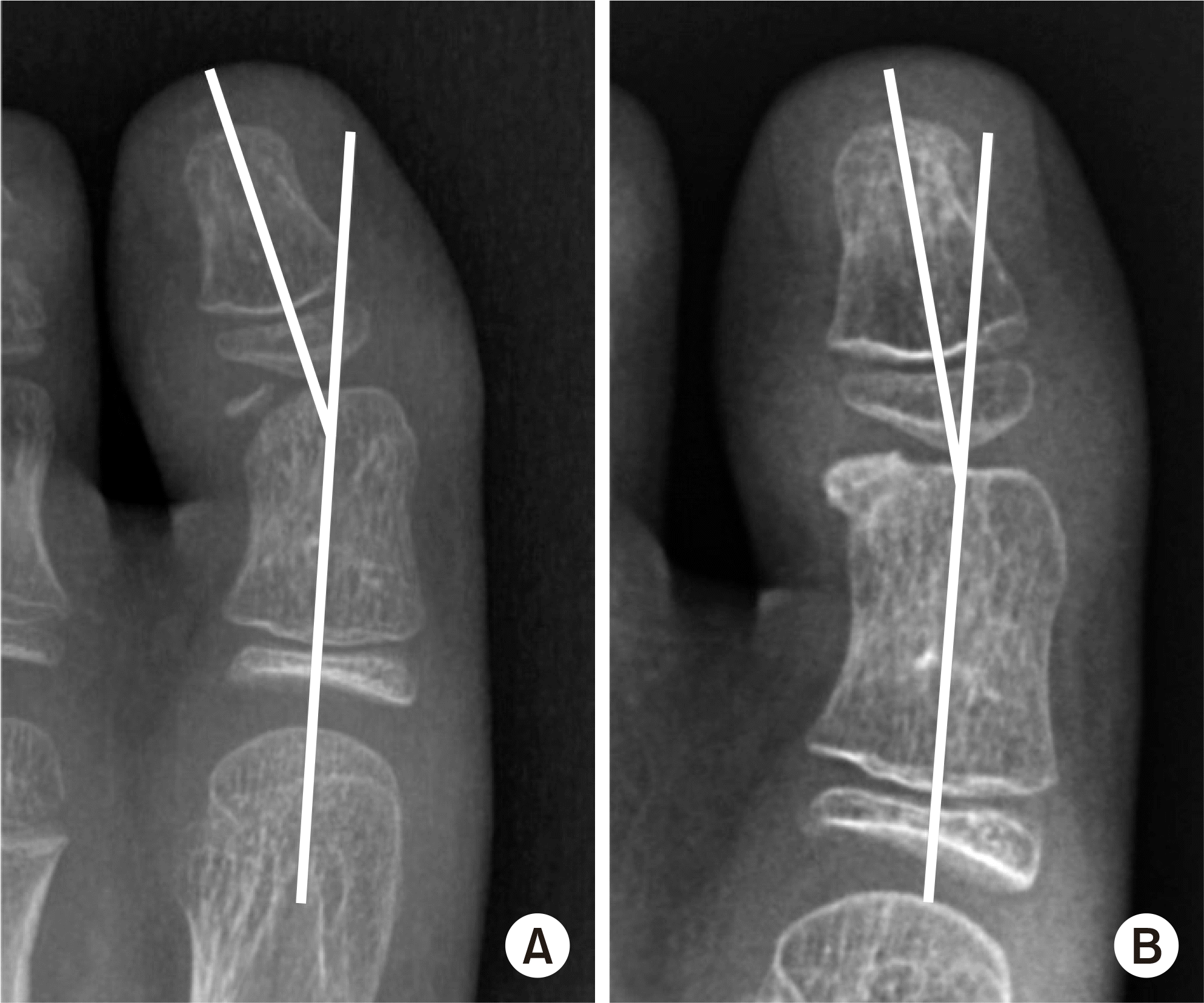 | Fig. 6.Preoperative X-ray (A) and X-ray at 2 months postoperatively (B). The hallux valgus interphalangeus angle was reduced after the surgery. |
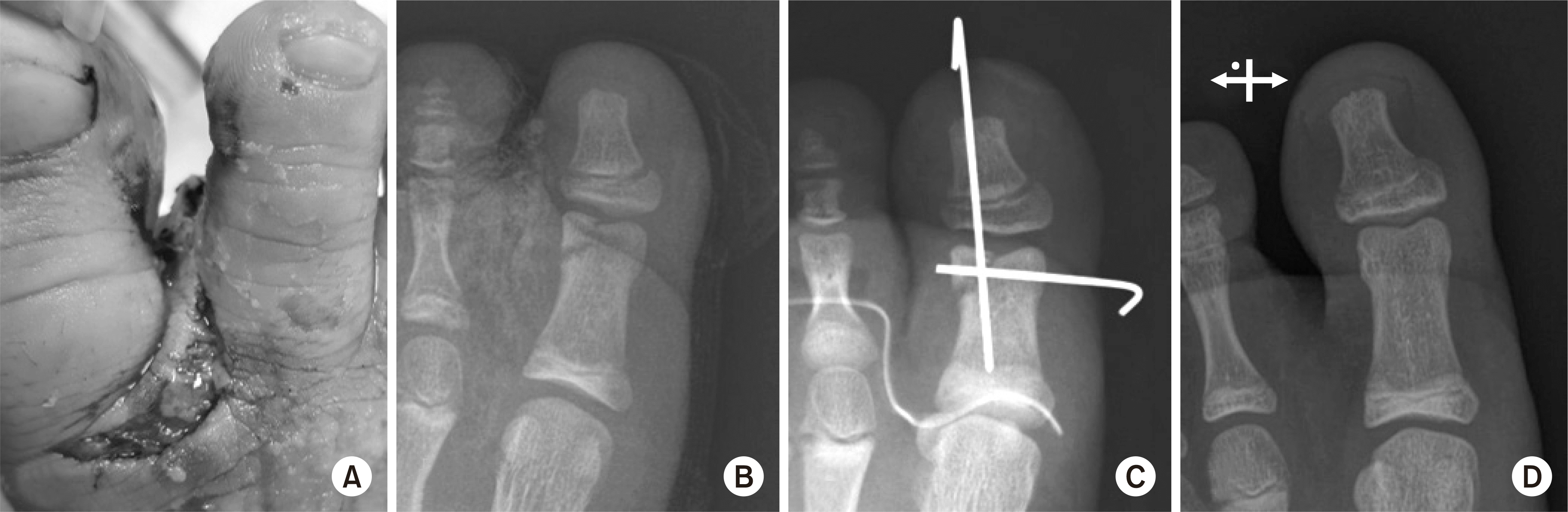 | Fig. 7.(A, B) A case of acute fracture with forefoot laceration. (C) Stable fixation was achieved using two K-wires. (D) Follow-up X-ray at 2 years postoperatively. |
Table 1.
Demographics and Preoperative Radiologic Evaluations




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download