Abstract
Purpose
This study compared the clinical and radiological results between two groups of patients with percutaneous fixation or conventional fixation after hardware removal.
Materials and Methods
The study analyzed 68 patients (43 open fixation and 43 percutaneous screw fixation [PSF] 25) who had undergone fixation for unstable thoracolumbar fractures. The radiologic results were obtained using the lateral radiographs taken before and after the fixation and at the time of hardware removal. The clinical results included the time of operation, blood loss, time to ambulation, duration of the hospital stay and the visual analogue scale.
Results
The percutaneous pedicle screw fixation (PPSF) group showed better results than did the conventional posterior fixation (CPF) group (p<0.05) in regard to the perioperative data such as operation time, blood loss, and duration of the hospital stay. There were no significant differences in wedge angle, local kyphotic angle, and the ΔKyphotic angle on the postoperative plane radiographs between the two groups (p>0.05). There were no significant differences in the wedge angle and local kyphotic angle after implant removal (p>0.05) between the two groups as well. However, there were significant differences in the segmental montion angle (p<0.001), and the PPSF group showed a larger segmental motion angle than did the CPF group (CPF 1.7°±1.2° vs PPSF 5.9°±3.2°, respectively).
Go to : 
References
1. Carl AL, Tromanhauser SG, Roger DJ. Pedicle screw instrumentation for thoracolumbar burst fractures and fracture-dislocations. Spine (Phila Pa 1976). 17(8 Suppl):S317–S324. 1992.

3. Akbarnia BA, Crandall DG, Burkus K, Matthews T. Use of long rods and a short arthrodesis for burst fractures of the thoracolumbar spine. A longterm follow-up study. J Bone Joint Surg Am. 76:1629–1635. 1994.

4. Alanay A, Acaroglu E, Yazici M, Oznur A, Surat A. Short-segment pedicle instrumentation of thoracolumbar burst fractures: does transpedicular intracorporeal grafting prevent early failure? Spine (Phila Pa 1976). 26:213–217. 2001.
5. Na HY, Choi JC, Choi JW, et al. The efficacy of the treatment of thoracolumbar spine fractures with short-segment posterior instrumentation and fusion. J Korean Fract Soc. 19:241–246. 2006.

6. Park Y, Seok SO, Lee SB, Ha JW. Minimally invasive lumbar spinal fusion is more effective than open fusion: a metaanalysis. Yonsei Med J. 59:524–538. 2018.

7. Ni WF, Huang YX, Chi YL, et al. Percutaneous pedicle screw fixation for neurologic intact thoracolumbar burst fractures. J Spinal Disord Tech. 23:530–537. 2010.

8. Phan K, Rao PJ, Mobbs RJ. Percutaneous versus open pedicle screw fixation for treatment of thoracolumbar fractures: systematic review and metaanalysis of comparative studies. Clin Neurol Neurosurg. 135:85–92. 2015.

9. Zhang W, Li H, Zhou Y, et al. Minimally invasive posterior decompression combined with percutaneous pedicle screw fixation for the treatment of thoracolumbar fractures with neurological deficits: a prospective randomized study versus traditional open posterior surgery. Spine (Phila Pa 1976). 41(Suppl 19):B23–B29. 2016.
10. Park HJ, Shim YJ, Kim WK, Cho TY, Kwon SM. Efficiency of implant removal for treatment of the thoracolumbar unstable fractures: multi segments fixationㆍsingle segment fusion. J Korean Soc Spine Surg. 18:103–110. 2011.
11. Ahn JS, Lee JK, Hwang DS, Kim YM, Kim WJ, Byun KH. The change of kyphotic angle and anterior vertebral height after posterior or posterolateral fusion with transpedicular screws for thoracolumbar bursting fractures. J Korean Soc Fract. 12:379–387. 1999.

12. Jeon CH, Lee HD, Lee YS, Seo JH, Chung NS. Is it beneficial to remove the pedicle screw instrument after successful posterior fusion of thoracolumbar burst fractures? Spine (Phila Pa 1976). 40:E627–E633. 2015.

13. Kim HS, Kim SW, Ju CI, Wang HS, Lee SM, Kim DM. Implant removal after percutaneous short segment fixation for thoracolumbar burst fracture: does it preserve motion? J Korean Neurosurg Soc. 55:73–77. 2014.
14. Chang HG, Kim YW, Jung JC, Kim HS, Lee KB. Preliminary report of temporary posterior instrumentation in stable thoracolumbar burst fractures. J Korean Soc Spine Surg. 9:364–373. 2002.

15. Lan T, Chen Y, Hu SY, Li AL, Yang XJ. Is fusion superior to non-fusion for the treatment of thoracolumbar burst fracture? A systematic review and metaanalysis. J Orthop Sci. 22:828–833. 2017.

16. Oh HS, Seo HY. Percutaneous pedicle screw fixation in thoracolumbar fractures: comparison of results according to implant removal time. Clin Orthop Surg. 11:291–296. 2019.

17. Lee JK, Jang JW, Kim TW, Kim TS, Kim SH, Moon SJ. Percutaneous short-segment pedicle screw placement without fusion in the treatment of thoracolumbar burst fractures: is it effective?: comparative study with open short-segment pedicle screw fixation with posterolateral fusion. Acta Neurochir (Wien). 155:2305–2312. discussion 2312,. 2013.

18. Vanek P, Bradac O, Konopkova R, de Lacy P, Lacman J, Benes V. Treatment of thoracolumbar trauma by short-segment percutaneous transpedicular screw instrumentation: prospective comparative study with a minimum 2-year follow-up. J Neurosurg Spine. 20:150–156. 2014.

19. Wang HW, Li CQ, Zhou Y, Zhang ZF, Wang J, Chu TW. Percutaneous pedicle screw fixation through the pedicle of fractured vertebra in the treatment of type A thoracolumbar fractures using Sextant system: an analysis of 38 cases. Chin J Traumatol. 13:137–145. 2010.
Go to : 
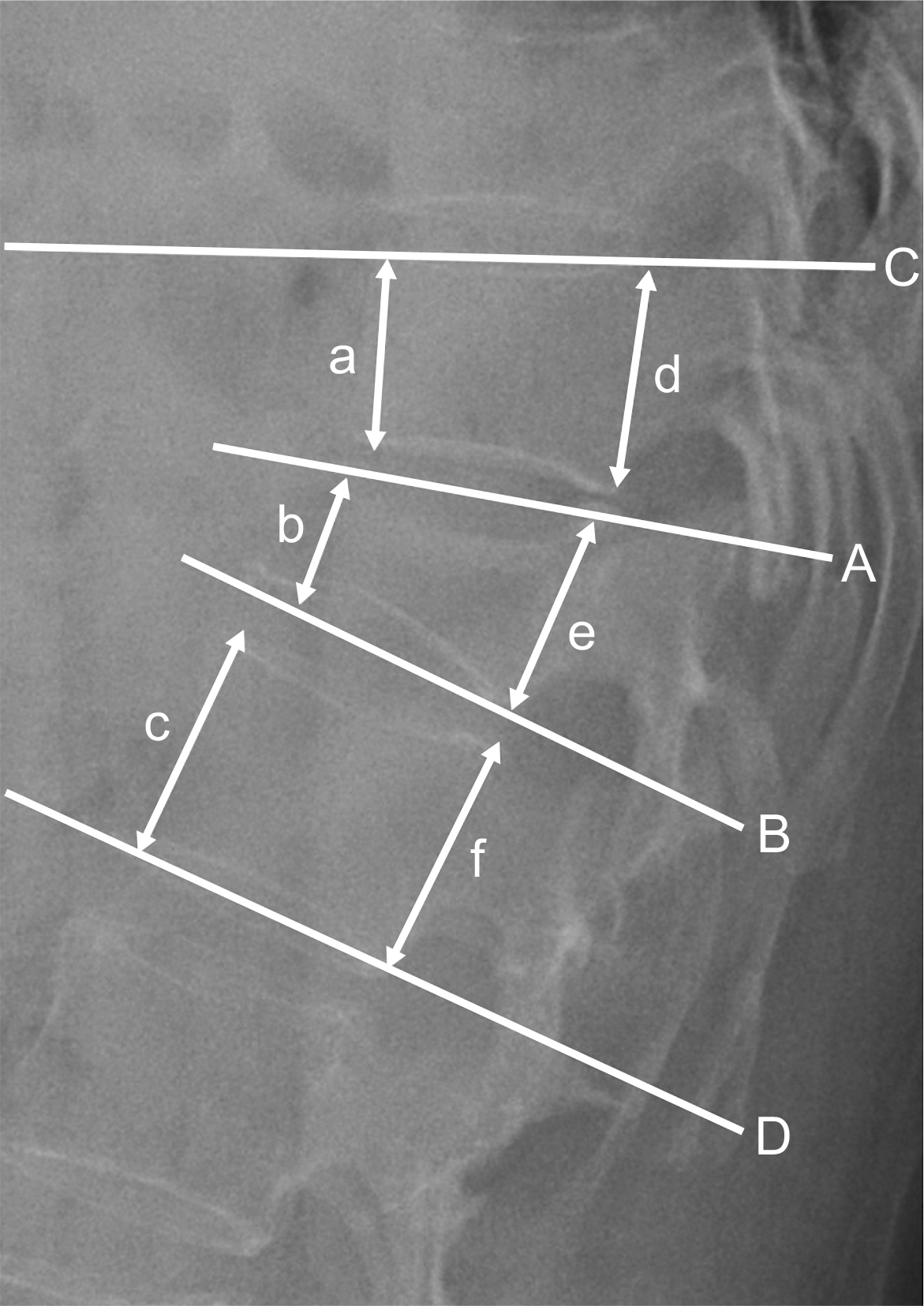 | Fig. 1.Radiography showing linear and angular measurement. Wedge angle (∠AB°), local kyphotic angle (∠CD°), anterior body height (200× b/(a+c) %), posterior body height (200×e/(d+f) %). |
 | Fig. 2.The segmental motion angle (SMA) was calculated as the difference between the local kyphotic angle on the flexion (FLEX) and extension (EXT) plain radiograph. |
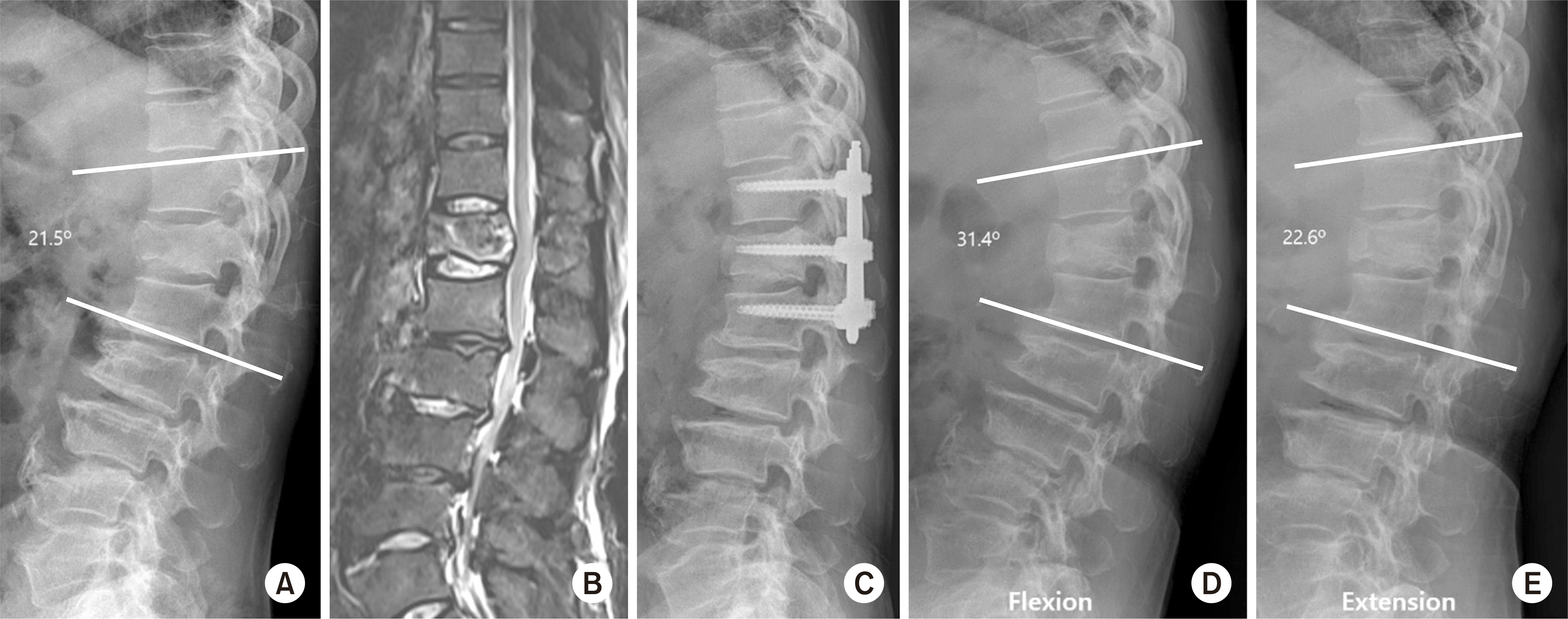 | Fig. 3.A 64-year-old male with flexion-distraction injury on T12. (A) The preoperative lateral X-ray shows fracture of the T12 body and spinous process. (B) On the magnetic resonance imaging (T2 weighted fat suppression), there was acute compression fracture with a spinous process fracture. (C) The lateral radiograph, taken immediately after surgery, shows anatomical reduction. (D, E) Lateral X-ray of the flexion (D)/extension (E) views that show the range of motion of no fusion segment. |
Table 1.
Demographic Note
Table 2.
Perioperative Data for Fixation
Table 3.
Radiologic Results after Posterior Fixation
Table 4.
Radiologic Results 3 Months after Implant Removal




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download