This article has been
cited by other articles in ScienceCentral.
Abstract
Heterotrophic ossification (HO) is a reactive disease presenting the formation of mature lamellar bone in soft tissues. It is known to occur following surgery, soft tissue injury, or central nervous system anomalies. However, a definite cause has not yet been clearly addressed. During the process of approach, reduction, and fixation while conducting surgeries, partial injury of soft tissue is inevitable. Additionally, secondary injuries may be caused during the active and passive range of motion exercises that should be done for the recovery of joint motion after surgery. The authors experienced cases of HO that may occur during surgery and rehabilitation after surgery. The authors recognized that special care is required for patients complaining of severe pain during the early stage of rehabilitation immediately after surgery. This study aimed to reaffirm the principles of fracture treatment by reviewing the cases and to investigate the occurrence of HO after fracture surgery.
Keywords: Heterotrophic ossification, Surgery, Rehabilitation, Range of motion
Heterotrophic ossification (HO) is the pathologic formation of bone in soft tissues and occurs in major joints, including the hip joint, knee joint, shoulder joint, and elbow joint. HO is known to be related to trauma, such as fractures and joint dislocations, soft tissue injury due to surgery, and nervous system injury in the brain and spinal cord.
12) Based on the principles of fracture treatment, it is well understood that intra-articular fractures should be treated by performing anatomic reduction; shaft fractures should be treated by recovering the anatomic alignment, preserving the blood supply, and providing rigid fixation between fragments. Additionally, both types of fractures require early resumption of joint motility.
3)
A confliction between the two well understood principles may occur occasionally when the two cases happen simultaneously. Alternately, misunderstanding of the principles of fracture treatment may lead to immoderate joint motion and thereby to soft tissue injury. In the aforementioned circumstances, HO can be caused, ultimately resulting in joint stiffness, severe pain, and gait disorder. Hence, this study aimed to reaffirm the principles of fracture treatment by reviewing the cases and to investigate the HO occurring after fracture surgery.
Case Reports
1. Case 1
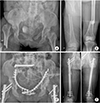
A 51-year-old female visited the trauma center with a severely injured pelvis and thigh caused by the falling of a heavy object directly on her while working. The patient complained of both hip pain and deformity of the thigh. In addition, the injury severity score was observed to be at 23 points. According to the advanced trauma life support (ATLS) guidelines, X-ray images were taken after resuscitation. Consequently, right hip posterior dislocation, pelvic bone fracture (lateral compression type II) with straddle fracture, and both femur shaft fractures were found (
Fig. 1). Although acetabular posterior wall fracture was found, it was not sufficient to meet the surgical indication as the displacement was <3 mm. Associated injuries included liver contusion and multiple rib fractures with hemothorax. There was no specific injury in the head, no special medical history was detected, and her cognition was alert.
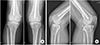
Femoral subtrochanteric fracture and associated right femoral head dislocation were unable to be reduced manually in the emergency room. Therefore, closed reduction and intramedullary nailing for the right femoral head dislocation and reduction for the femoral head were performed under general anesthesia with the consent of a caregiver. Subsequently, open reduction and plate fixation were performed for the pelvic fracture and closed reduction and nail fixation were performed for the left femoral shaft fracture upon the recovery of the general condition. The patient began active and passive hip and knee range of motion (ROM) exercises a week after the surgery. Additionally, weight bearing was resumed six weeks after the surgery in consideration of the pelvic fracture. The hip was the main site of injury and the patient showed a tolerable reaction for hip ROM exercises. However, the patient was not able to perform active knee ROM exercises and the rehabilitation involved passive ROM exercises advised by doctor and physical therapist. Since the knee was not injured, it was presumed that the reason was simple irritation caused by the interlocking screw inserted into the distal femur for antegrade nailing. Consequently, the passive ROM exercise was performed once in every three days at the time of the daily rounds by making the patient to do hip and knee flexion and extension while holding her ankle and knee. A total of five exercise sessions were continued until the patient's discharge. The patient reported severe pain (visual analogue scale [VAS] score, 7 points) every time she did the knee joint motion and rehabilitation was performed while administrating pain reliever. The patient attended the follow up sessions post her discharge two weeks after the surgery. Notably, the passive and active knee ROM measured at the time of discharge was 10° to 120° and 20° to 80°, respectively. HO around the popliteal fossa, wide enough to connect the tibia to the femur, was observed since the second month of the follow-up, and the HO was observed to expand to the medial and lateral femoral condyle and along the quadriceps (
Fig. 2). Joint stiffness was observed as the patient presented knee ROM as 20° to 30° for the right and 20° to 40° for the left side. The patient underwent surgery for HO excision and knee ROM recovery six months after the primary surgery. She did not undergo radiotherapy. However, she took Cox-2 inhibitor as it was prescribed for the treatment (
Fig. 3).
2. Case 2
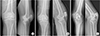
A 65-year-old male who fell down from the second floor while working, was diagnosed with patellar fracture based on the X-ray images. Consequently, he was treated by performing open reduction and plate fixation three days after the injury. The patient began aggressive passive motion three days after the surgery and complained of pain (VAS score, 8 points) during the passive ROM exercises. However, we thought that this was a normal postoperative rehabilitation process, and we proceeded with ROM exercise, ignoring the pain of the patient. The patient was discharged two weeks after the surgery and joint stiffness and HO diffusing into the patellar tendon and medial femoral condyle area were observed (
Fig. 4). The knee ROM was 10° to 40°. Therefore, we recommended that the patient should undergo surgical removal of HO. However, he refused to undergo the surgery and chose crutch gait.
Discussion
HO observed in fracture patients without central nervous system injury may be due to excessive soft tissue injury caused during surgery.
24) However, as shown in the aforementioned Case 1, the patients who did not undergo direct injury in the knee presented HO formation in the knee during the rehabilitation after the antegrade nailing in the femur. Such HO was considered to be formed due to excessive passive joint motion during the rehabilitation that may have caused micro bleeding within the muscle, which then formed hematoma and progressed through ossification. This is the first report of severe HO in the intact body regions of patients with general trauma who did not present central nervous system injury or burns. Considering that the occurrence of HO around the patella is rare and that such Case 2 has rarely been reported, HO can be predicted to occur during the postoperative rehabilitation rather than soft tissue injury during the surgery.
5)
Joints are relatively avascular regions and are nourished with the nutrients and oxygen obtained through diffusion from the joint fluid. Hence, circulation of the joint fluid is essential, and treatment for intra-articular fractures should be facilitated by beginning early joint motion to promote the circulation.
6) In addition, while performing intramedullary nailing, at least two distal screws are inserted to fix the shaft fractures and a maximum of five screws are inserted around the knee to fix the infra-isthmal fractures.
7) In the Case 1, knee stiffness may be caused if early joint motion is not initiated. Therefore, early knee joint motion is preferred. It is also required for performing weight bearing exercises early. Moreover, early mobilization after the surgery can also improve lung function, reduce the risk of deep vein thrombosis and urologic complications, and eliminate secondary risk factors, including muscular weakness and falls, which can be caused by bed rest and limited physical activity. It was also effective for the alleviation of the symptoms of delirium that may occur in elderly patients.
3)
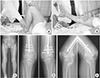
The underlying issue is that excessive joint motion will lead to soft tissue injury. However, there has been no study that has clearly defined the extent for which joint exercise is considered appropriate and when the exercise is considered immoderate/not considered suitable. Practitioners can only predict that HO occurred due to the excessive exercise. Hence, the authors propose that rehabilitation should be performed within the tolerable range of the patient rather than by forcing the patient's knee to be bent or by performing hip ROM exercises beyond the patient's tolerable range. Consequently, the authors terminated the present method of rehabilitation wherein the patient in the supine position is made to perform passive ROM exercises by a practitioner. Alternatively, patients were asked to assume a sitting position by perching on the edge of the bed, allowing for knee flexion naturally by gravity, and then asked to do quadriceps muscle strength exercise and knee ROM exercise by extending their knee by themselves (
Fig. 5). For the elbow ROM exercise, the patients were asked to hold the wrist of the injured arm with the hand of the intact arm and perform the ROM exercise within their tolerable range. Using these methods of rehabilitation, the authors confirmed considerably decreased HO incidence.
Besides, during the postoperative rehabilitation period, when the patient complains of pain that far exceeds the general pain complained (VAS score, 3-4 points), the treatment must be performed under suspicion of HO due to soft tissue injury.
12) The patient's symptoms should be monitored to reduce the intensity of the treatment or to stop rehabilitation for a while. In fact, when HO occurs, treatment becomes very difficult. HO is more prophylactic than treatment.
There are two types of existing treatments, namely, non-surgical treatments, including administration of nonsteroidal anti-inflammatory drugs (NSAIDs) and radiotherapy, and surgical removal of heterotrophic osseous tissue.
89) Cases with severe disorder of joint motion or severe pain require surgical treatment. All of the cases in this study presented joint stiffness and consequent gait disorder and required surgical treatment. The optimal timing for the removal has not been defined yet; there are controversial reports including some studies in conflict regarding the optimal timing for the removal (6 months after the onset or 12 months after the onset) and other studies recommending the early removal, regardless of the timing.
2)
The methods to prevent the relapse of HO include the administration of NSAIDs and radiotherapy.
89) NSAIDs are known to prevent HO by inhibiting the action of cyclooxygenase. Notably, indomethacin is the most frequently used NSAID. Schmidt et al.
10) reported that indomethacin exerts a preventive effect on the relapse of HO after hip joint surgery beyond a simple placebo effect. Radiotherapy is also known prevent the relapse of HO but has no preventive effect on the remaining HO tissue since bone is already formed after cell differentiation. Although the aforementioned methods for relapse after the surgery were not applied for the Case 1 in this study, relapse was not observed. This was possibly because the authors performed extensive HO removal including the removal of normal tissues.
In conclusion, appropriate ROM exercise after fracture surgery is significantly beneficial for patients in treatment of fractures as it helps the lubrication of the joint. However, immoderate passive ROM exercise may cause HO. Particular attention should be paid to patients complaining of extreme pain during postoperative rehabilitation, and ROM exercise should be performed at a gentle tolerable level.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download