INTRODUCTION
Haemophilus influenzae is an important human pathogen and can be classified into serotypes a to f and non-typeable based on the capsular polysaccharide characteristics.
1234) It is a key etiologic pathogen in severe invasive infections, mainly among children under 5 years of age.
123) This bacterium may cause meningitis, septicemia, epiglottitis, septic arthritis, and upper and lower respiratory tract infections.
12) H. influenzae serotype b (Hib) was the most common serotype associated with severe invasive infections.
12) However, after the implementation of Hib vaccination, the incidence of invasive Hib disease decreased, particularly among children under 5 years of age.
12) With the successful introduction of Hib vaccination, invasive disease caused by non-type b
H. influenzae has emerged, particularly in individuals with underlying medical conditions, such as primary immunodeficiency, malignancy, and cerebrospinal fluid (CSF) leakage.
123)
Cerebral venous sinus thrombosis (CVST) is an uncommon, potentially life-threatening condition that may cause acute or long-term neurological deficit.
56) CVST can be complicated after a serious bacterial infection, including meningitis.
567) The prevalence of CVST, which is observed in childhood, varies, with neonates and infants being the most commonly affected.
567) CVST may present with various signs and symptoms (i.e., headache, seizure, focal neurologic deficits, encephalopathy, and coma), but they may be subtle, and thus, the diagnosis is often delayed or missed.
567) Studies have reported that precise diagnosis and treatment is an important goal to improve the outcome of patients.
6) Herein, we present a case of a child with CVST after being diagnosed with
H. influenzae serotype f (Hif) meningitis.
CASE
A 26-month-old boy was admitted with complaints of fever for 2 days and lethargy for one day. His past medical history was unremarkable. He had received all scheduled immunizations including a full course of Hib vaccine for his age. On admission, he was pale with a temperature of 38.2°C. His heart rate was 124 beats per minute, blood pressure was 96/60 mmHg, and oxygen saturation was 99%. He was alert but rather lethargic. Physical examination revealed no sign of meningeal irritation, no focal neurological deficit, and no papilledema. Laboratory tests showed a white blood cell count of 19,000/μL (71.6% neutrophils, 19.9% lymphocytes) and markedly elevated qualitative C-reactive protein (above: 300 mg/L; upper limit of normal: 5 mg/L). The CSF was turbid with 961 leukocytes/mm3 (95% neutrophils), 51.95 mg/dL protein, and 91 mg/dL glucose. Blood glucose level was 119 mg/dL, and its ratio with CSF was 0.78.
Non-contrast computed tomography (
Fig. 1) of the head performed on the 1st hospital day indicated a high-density lesion in the right transverse-sigmoid sinus area, dural sinus thrombosis, and subdural hemorrhage. Magnetic resonance imaging (MRI) and magnetic resonance venography (MRV) of the brain (
Fig. 1) performed on the 5th hospital day showed a distended right transverse-sigmoid sinus, suggesting acute dural sinus thrombosis in the right transverse-sigmoid sinus. We diagnosed CVST due to meningitis and administered empirical antibiotics (cefotaxime at 300 mg/kg/day and vancomycin at 60 mg/kg/day for 14 days and 7 days, respectively) accompanied with low-molecular-weight heparin (1 mg/kg every 12 hours for 7 days) and warfarin titrated with a target international normalized ratio of 2–3.
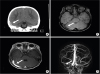 | Fig. 1 Non-contrast-enhanced computed tomography performed on the 1st hospital day showed a high-density lesion noted in right transverse-sigmoid sinus area (arrow) (A). Brain magnetic resonance images were taken on the 5th hospital day (B-D). Distended right side transverse-sigmoid sinus was hyperintense on axial contrast-enhanced T1-weighted image (B) and hypointense on susceptibility-weighted image (C). Right side transverse and sigmoid sinus obstruction is seen on venography (D).
|
After 2 days, fever subsided and lethargy was improved. He could obey and recognize his parents and the place and did not suffer from other symptoms. Blood and CSF culture indicated H. influenzae, which was identified as serotype f by standard slide agglutination typing and polymerase chain reaction-based capsule typing by Korea Centers for Disease Control and Prevention. His immunologic studies were normal, including immunoglobulins (Igs) such as total IgG, all 4 IgG subclasses, IgA, and IgM. Absolute count of T cell lymphocyte subsets and serum complement level (C3, C4, and CH50) were within the normal range. The antimicrobial susceptibility report of H. influenzae showed that it was resistant to amoxicillin/clavulanate and susceptible to cefotaxime. Therefore, treatment with cefotaxime was continued.
The patient was discharged after 15 days of hospital stay. At discharge, neurological examination and auditory screening were normal, and there were no other complications. We prescribed warfarin for 3 months; however, his parents decided to discontinue medication one month later because of an itching sensation. Consequently, we decided to schedule follow-up visits earlier than initially planned. At 2 months after discharge, the patient was neurologically normal, and follow-up brain MRI and MRV showed recanalization of CVST (
Fig. 2).
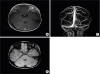 | Fig. 2 The follow-up brain magnetic resonance images performed 2 months after the initial study. The aforementioned hyperintense lesion appears to have resolved on contrast-enhanced T1-weighted image (A) and the hypointense lesion has almost disappeared on susceptibility-weighted image (B). Recanalization of thrombosis was seen in right side transverse and sigmoid sinus on venography (C).
|
This case was reviewed and approved by Institutional Review Board of Hallym University Sacred Heart Hospital (IRB No. 2018-11-016). Requirement for informed consent was waived.
DISCUSSION
To our knowledge, this is the first case report of Hif meningitis complicated with CVST in Korea. Beyond the neonatal period,
H. influenzae is one of the major organisms causing bacterial meningitis. In Korea, Hib vaccine was introduced to prevent invasive infections in 1993 and was included in the national immunization program in 2013.
89) The proportion of cases of childhood invasive infections caused by
H. influenzae has decreased from 20.1% in 1996–2000 to 4.5% in 2001–2005; it has further decreased to 1.9% in 2006–2010 in Korea.
1011) Several other countries have also reported substantially decreased incidence of Hib infections after the introduction of Hib vaccine. However, concerns have been raised about the possibility of changes in serotype distribution as other serotypes and/or non-typeable strains may replace the ecological niche of Hib.
1234) In fact, some in vitro data suggest that Hib suppresses the growth of other encapsulated and nonencapsulated strains by producing a bactericidal factor.
4) However, the incidence of invasive disease associated with Hif is low, and most published reports are individual case reports of meningitis, pneumonia, or sepsis.
1234) In general, information about the clinical, microbiological, and epidemiological significance of Hif infection is limited.
1234) Therefore, further studies are needed to support the hypothesis of Hif replacement after Hib vaccination.
123)
Hif meningitis is rare and may be related to a predisposing condition.
1234) Predisposing conditions to Hif infection, including impaired immunity, have been reported for more than two-thirds of patients with pneumonia, sepsis, or meningitis.
3) Immunodeficiency is usually presented with severe signs and symptoms of infection, and it may initially be recognized with the occurrence of Hif meningitis.
3) Hence, a patient presenting with Hif meningitis should undergo immunological evaluation. However, Hif may show significant virulence and cause infection even in an individual with no clear evidence of immunodeficiency.
3) In our case, the patient had no prior history of recurrent infections or other signs that could indicate a pre-existing immunodeficiency, and immunological evaluation revealed no evidence of immunodeficiency.
Infections of the central nervous system (CNS) can cause various cerebrovascular diseases. The pathological processes involved are para-infectious processes (immune-mediated) causing vasospasm or thrombosis, vasculitis primarily affecting the vessels at the base of the brain in meningitis, or a hypercoagulable state with endothelial dysfunction resulting from the activation of inflammatory and procoagulant cascades.
1213) CVST is a cerebrovascular disease that is relatively rare and potentially life-threatening among children.
5) Although there have been reports of meningitis complicated with CVST caused by pneumococcus, to our knowledge, there was no previous report related to Hif in Korea.
14) The 2 encapsulated bacteria differ in terms of the bacterial cell wall components.
H. influenzae is a gram-negative bacterium, and it has lipooligosaccharide as its cell wall component, whereas
Streptococcus pneumoniae is a Gram-positive bacterium, and it has lipoteichoic acid as its cell wall component.
15) These produce meningeal inflammation and activate complement system causing hypercoagulable states.
1315) The relationship between CVST and CNS infection from
H. influenzae is unclear. Nevertheless, we assume that its pathophysiology is similar to that of other encapsulated bacterial infections, i.e., disseminated intravascular coagulopathy and vascular thrombosis due to high levels of circulating procoagulant microparticles from platelets or granulocytes and disordered protein C activation in endothelial cells.
612) Although infection is not considered a prominent cause of CVST currently, in developing countries, sepsis and CNS infections remain a vital cause of CVST.
16)
CVST treatment includes supportive measures, such as hydration, empirical antibiotics, anticonvulsants, antithrombotic therapy, symptomatic treatment of increasing intracranial pressure (e.g., headache, confusion, and visual deficit), and etiological treatment to manage related conditions and risk factors.
16) The aims of antithrombotic therapy in CVST are to recanalize the occluded vessels, prevent thrombus proliferation, prevent pulmonary embolism, and treat the underlying prothrombotic state.
16) Warfarin sodium was administered as an antithrombotic agent, and its adverse reactions include fatal and nonfatal hemorrhage from tissues or organs.
17) Dermatological allergic reactions, such as urticarial, maculopapular, vesicular, and pruritic skin eruptions, are rarely reported.
17) In this case, the patient could not tolerate warfarin due to itching. Although our clinicians did not examine the lesions and symptoms, allergic reactions manifesting as an itching sensation can occur.
After the introduction of Hib vaccine, the rate of infections caused by Hib has dramatically decreased and the proportion of infections caused by non-type b H. influenzae has increased. We report a case with Hif meningitis complicated with CVST, which was diagnosed by brain MRI and MRV and successfully treated with appropriate antibiotics and anticoagulation therapy. In the Hib vaccination era, non-type b H. influenzae can be a cause for serious invasive infection.






 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download