Abstract
Purpose
To investigate the clinical characteristics of spontaneous separation of idiopathic epiretinal membrane (ERM) patients without any surgical treatment.
Methods
Retrospective medical records analysis was performed for patients with spontaneous separation of the idiopathic ERM without treatment. The patients' age, average time until ERM separation, best-corrected visual acuity (BCVA), refractive error, intraocular pressure (IOP), optical coherence tomography (OCT) data, central macular thickness (CMT), and the presence of posterior vitreous detachment (PVD) were evaluated and recorded.
Results
Twenty-two eyes of 22 patients were included in the study. The mean age of patients was 52.0 ± 8.6 years, and the average time until ERM separation was 14.1 ± 16.2 months. The average BCVA (logMAR) was 0.12 ± 0.12 before separation and improved (p = 0.032) to 0.07 ± 0.08 after separation. The average CMT before separation was 386.1 ± 63.2 μ m, after sepa-ration, the average CMT decreased (p < 0.001) to 299.1 ± 46.7 μ m. The differences in IOP and refractive error before and after ERM separation were not statistically significant. Not all patients experienced PVD before ERM separation, however, they all showed PVD after the separation.
Go to : 
References
1. Kim SH, Song SJ, Bae JH. The incidence and risk factors of abdominal membrane in a screened Korean population. J Korean Ophthalmol Soc. 2018; 59:922–9.
2. Hwang DJ, Na KI, Kwon SI, Park IW. abdominal changes in visual acuity and foveal thickness after vitrectomy for idiopathic abdominal membrane. J Korean Ophthalmol Soc. 2012; 53:434–9.
3. Byon IS, Pak GY, Kwon HJ, et al. Natural history of idiopathic abdominal membrane in eyes with good vision assessed by spectral-abdominal optical coherence tomography. Ophthalmologica. 2015; 234:91–100.
4. Fraser-Bell , Guzowski M, Rochtchina E, et al. Five-year abdominal incidence and progression of epiretinal membranes: the Blue Mountains Eye Study. Ophthalmology. 2003; 110:34–40.
5. Lee CH, Kweon EY, Cho NC, Kim WJ. Analysis of leading abdominals causing epiretinal membrane and comparison of prognosis after epiretinal membrane peeling. J Korean Ophthalmol Soc. 2015; 56:1586–90.
6. Kwon JM, Lee JH, Kim KH, et al. Reproliferation of idiopathic abdominal membrane after spontaneous separation. J Korean Ophthalmol Soc. 2016; 57:682–5.
7. Cakir M, Cekiç O, Bayraktar S, Yilmaz OF. Spontaneous abdominal of epiretinal membrane in a child with Stargardt macular dystrophy. J AAPOS. 2007; 11:618–9.
8. Gupta A, Gopal L, Biswas J. Spontaneous separation of abdominal epiretinal membrane in a patient with toxoplasmic retinochoroiditis. Oman J Ophthalmol. 2012; 5:64–5.
9. Greven CM, Slusher MM, Weaver RG. Epiretinal membrane abdominal and posterior vitreous detachment. Ophthalmology. 1988; 95:902–5.
10. Sachdev N, Gupta V, Gupta A, Singh R. Spontaneous separation of idiopathic epiretinal membrane in a young patient. Int Ophthalmol. 2008; 28:301–2.

11. Lim YC, Au Eong DT, Wagle AM, Au Eong KG. Spontaneous abdominal of epiretinal membrane: a report of three cases. Clin Exp Optom. 2018; 101:299–301.
12. Andreev AN, Bushuev AV, Svetozarskiy SN. A case of secondary epiretinal membrane spontaneous release. Case Rep Ophthalmol Med. 2016; 2016:4925763.

13. Noh JH, Kim HA, Park TK, Ohn YH. Spontaneous separation of idiopathic epiretinal membranein an elderly patient. J Korean Ophthalmol Soc. 2014; 55:459–64.
14. Cho SY, Hwang YH. Comparison of macular retinal thickness among four optical coherence tomography devices in healthy young subjects. J Korean Ophthalmol Soc. 2019; 60:434–9.

15. Kim SI, Park SW, Byon IS, Lee JE. Surgical outcomes of abdominal epiretinal membrane with good visual acuity. J Korean Ophthalmol Soc. 2014; 55:686–92.
16. Banach MJ, Hassan TS, Cox MS, et al. Clinical course and surgical treatment of macular epiretinal membranes in young subjects. Ophthalmology. 2001; 108:23–6.

17. Mansour AM, Mansour HA, Arevalo JF. Spontaneous release of epiretinal membrane in a young weight-lifting athlete by presumed central rupture and centrifugal pull. Clin Ophthalmol. 2014; 8:2243–50.
18. Yang HS, Hong JW, Kim YJ, et al. Characteristics of spontaneous idiopathic epiretinal membrane separation in spectral domain abdominal coherence tomography. Retina. 2014; 34:2079–87.
19. Chung SE, Lee JH, Kang SW, et al. Characteristics of epiretinal membranes according to the presence or absence of posterior abdominal detachment. Eye (Lond). 2011; 25:1341–6.
20. Nomoto H, Matsumoto C, Arimura E, et al. Quantification of changes in metamorphopsia and retinal contraction in eyes with spontaneous separation of idiopathic epiretinal membrane. Eye (Lond). 2013; 27:924–30.

21. Meyer CH, Rodrigues EB, Mennel S, et al. Spontaneous separation of epiretinal membrane in young subjects: personal observations and review of the literature. Graefes Arch Clin Exp Ophthalmol. 2004; 242:977–85.

22. von Hanno T, Lade AC, Mathiesen EB, et al. Macular thickness in healthy eyes of adults (N = 4508) and relation to sex, age and abdominal: the Tromsø Eye Study (2007–2008). Acta Ophthalmol. 2017; 95:262–9.
23. Kim M, Kim HE, Lee DH, et al. Intraocular lens power estimation in combined phacoemulsification and pars plana vitrectomy in eyes with epiretinal membranes: a case-control study. Yonsei Med J. 2015; 56:805–11.

24. Yonemoto J, Noda Y, Masuhara N, Ohno S. Age of onset of abdominal vitreous detachment. Curr Opin Ophthalmol. 1996; 7:73–6.
Go to : 
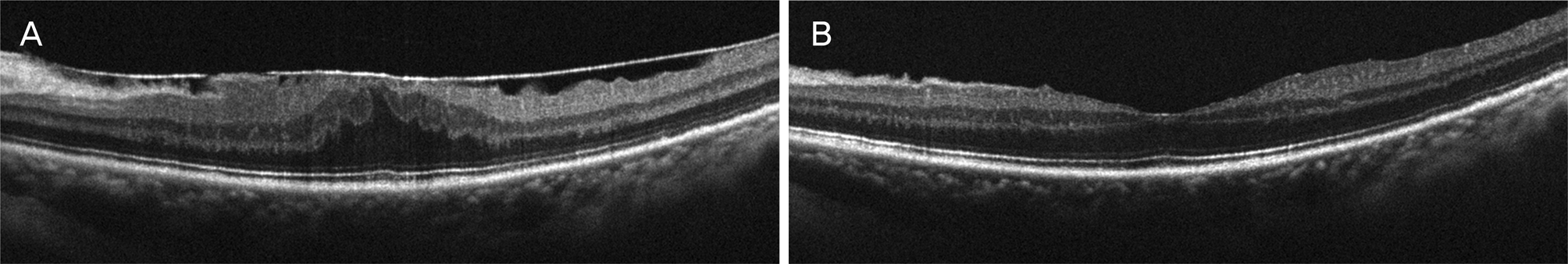 | Figure 1.Opticalcoherence tomography images of macula with epiretinal membrane (A), and after spontaneous separation of epiretinal membrane in same eye (B). The central macular thickness decreased from 491 μ m to 297 μ m, and the patient's visual acuity (logMAR) was improved from 0.4 to 0.05. logMAR = logarithm of minimal angle of resolution. |
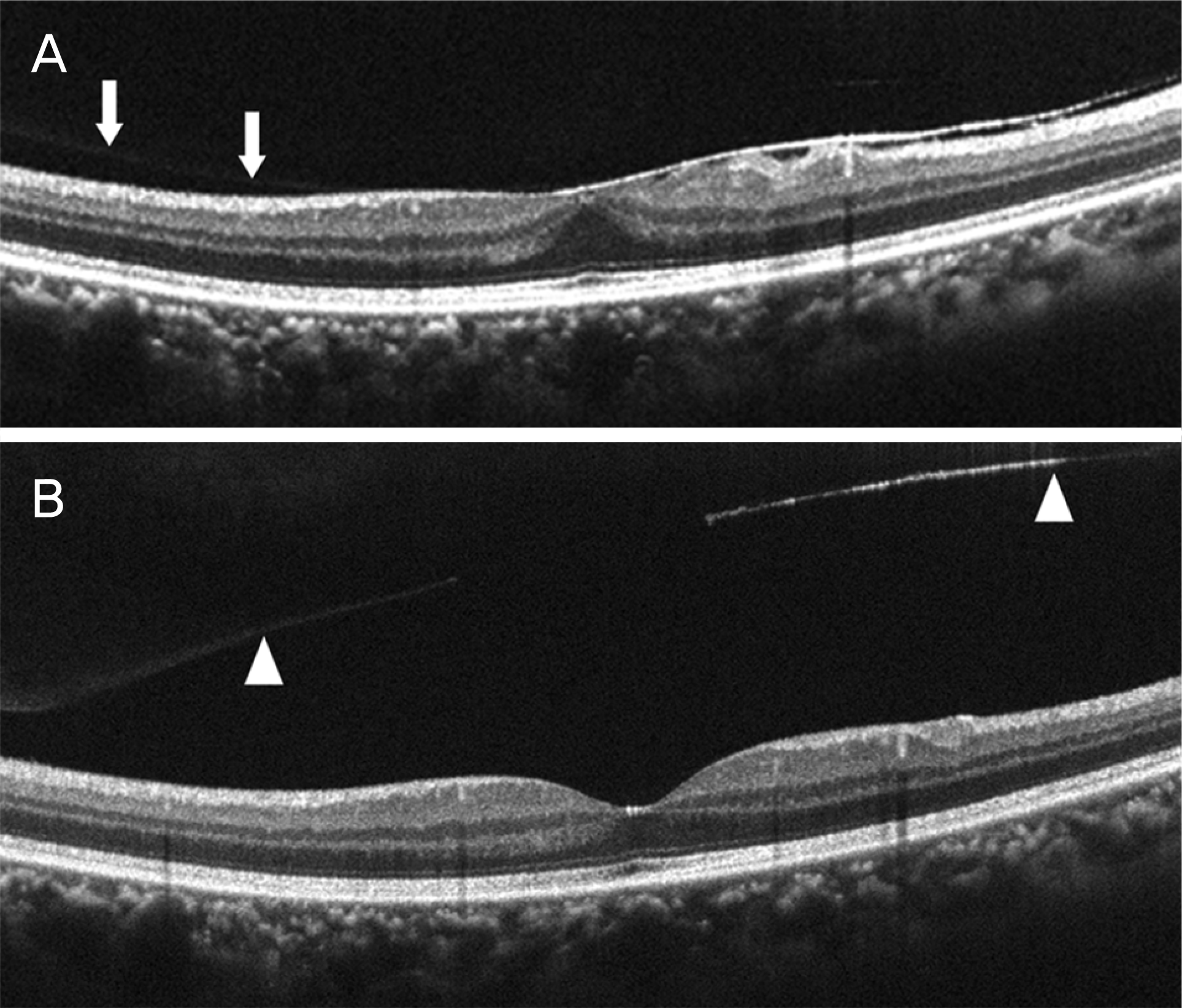 | Figure 2.Opticalcoherence tomography images of macula with posterior vitreous adhesion (arrows) and epiretinal mem-brane (A), and posterior vitreous detachment (arrowheads) with spontaneous separated epiretinal membrane (B). The central macular thickness decreased from 337 μ m to 275 μ m. |
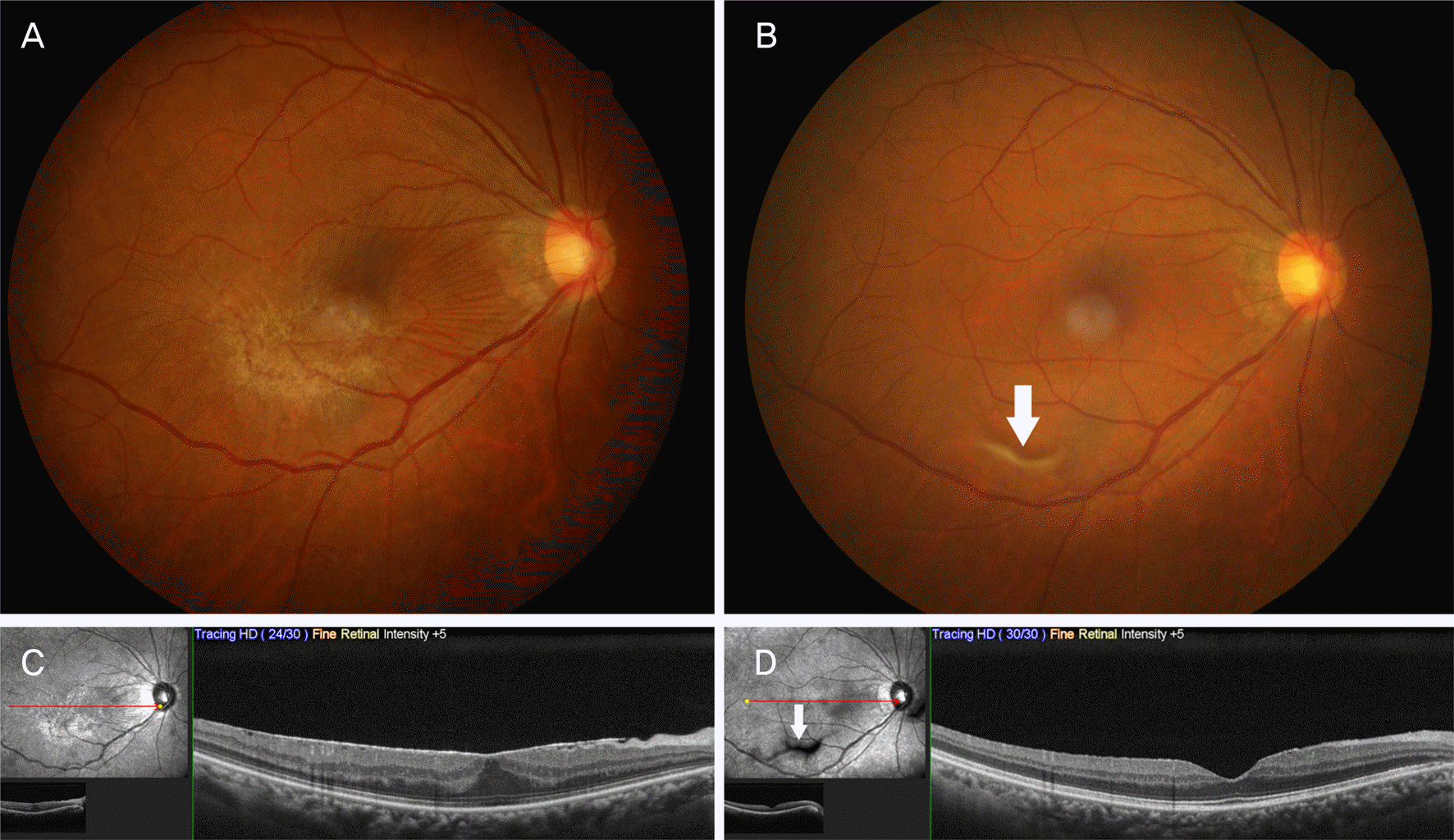 | Figure 3.Fundus photograph (A, B) and opticalcoherence tomography images (C, D). Epiretinal membrane was shown at baseline images (A, C), and large floater (arrows) appeared after spontaneous separation of epiretinal membrane (B, D). The central macular thickness decreased from 401 μ m to 298 μ m. |
Table 1.
Baseline characteristics of patients (n = 22)
Table 2.
BCVA and CMT at first visit, before spontaneous separation, and after spontaneous separation




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download