Abstract
Ganglion cyst which originates from joint space can affect nearby nerves through an articular branch. Despite known as benign mucinous lesion, ganglion cyst can show significant fascicular invasion and expansion, resulting in compression neuropathy. Number of pathogenesis have been insisted but the most widely acknowledged one is synovial herniation hypothesis. It describes a capsular defect in joint and discharged fluid to aggregate as cyst along the epineurium of articular branch. Tarsal tunnel syndrome is an entrapment neuropathy of the tibial nerve or its branches in the tarsal tunnel of ankle. In this case report, we describe a case of ganglion cyst associated tarsal tunnel syndrome and its surgical treatment.
Ganglion cyst is a small fluid filled sac that forms over a joint or tendon sheath and can develop almost in any joint space of the body. Most cases present as a slow growing (usually over months) solitary lesion with no further symptoms. But in some patients, numbness or pain may occur and one of its mechanism can be understood as nerve compression especially in zones of anatomic nerve entrapment. Although they are benign tumors, ganglion cysts are prone to expand and cause scarring, which can devastate neighboring articular space. This would be synergistic with the confined and limited compliance of joint, thereby accelerating symptoms of compression and ischemia. When it comes to the ankle joint, one can represent it as a tarsal tunnel syndrome originated from a ganglion cyst1. Tarsal tunnel is located posterior to the medial malleolus and many structures pass through this fibro-osseous space2. Posterior tibial nerve is one of them and covered by the flexor retinaculum whose role is stabilizing its understructures. Tarsal tunnel syndrome is an entrapment neuropathy of the tibial nerve or its branches in the tarsal tunnel. Decompression with complete surgical excision has been reported as effective treatment for patients who are suffering from tarsal tunnel syndrome3. In this case, we elaborated with fascicular dissection to protect the nerve branch and provide a complete elimination of tumor. As is widely known, incomplete excision may lead to recurrence.
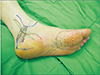
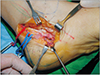
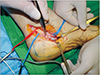
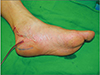
A 56-year-old male presented to our department for paresthesia and tingling sensation on the left foot. This symptom occurred spontaneously and persisted 6 months according to the patient (July 2003). He also had no significant medical or trauma history but had some experience of ankle sprain during working as a farmer. On physical examination, muscle atrophy was not noted and we found that the area of paresthesia was medial plantar nerve distribution area. We commissioned the Department of Rehabilitation Medicine to conduct an electromyography test to further clarify the sensory deterioration of this particular area4. On examination, the patient was suspected of having tarsal tunnel syndrome (Fig. 1). We concluded that release of flexor retinaculum and elimination of the occurrence factor would be the fundamental treatments. In order to directly identify what is causing the compression on the medial plantar nerve and to remove it, we decided to undergo surgical treatment with general anesthesia. On the surgical field (August 7, 2003), we noticed that there was severe medial plantar nerve compression by 3×1×1 cm3 size fusiform shaped white cyst and thickened perineural fibrous band (Fig. 2). The cyst was multinodular and had no direct connection with the posterior tibial nerve. Release of flexor retinaculum was done with surgical excision and elaborated fibrous adipose tissue dissection (Fig. 3). Both protection of the nerve branch and complete elimination of cyst were successfully carried out. The dissected cyst was presumed to be ganglion cyst, but we referred the pathology department for further confirmation (Fig. 4). They revealed it as a ganglion cyst after 4 days. After the surgery, the patient recovered immediately and no longer complained of sensory abnormality or numbness in the same area (Fig. 5).
Intrinsic or extrinsic compression of peripheral nerve can cause several symptoms like paresthesia or tingling sensation. Tarsal tunnel syndrome is entrapment neuropathy associated with the posterior tibial nerve or its branches at the tarsal tunnel5. Various factors like bony deformity of talus or calcaneus, hypertrophy of the abductor hallucis, osteochondroma, posttraumatic fibrosis or even ganglion cyst can be the cause of tarsal tunnel syndrome67. Precise cause of neural ganglia formation is still on controversy. Two different pathogenesis have been discussed considering the origin of the ganglion. One presumes that ganglion occurs in the nerve itself and the other one seeks its origin outside of the nerve. The first hypothesis insists cystic degeneration of the connective tissue of the epineurium. Ganglion presenting in restricted space may lead to compression of the epineurium and the increased pressure would induce degeneration of the epineurium8. This degeneration may form a ganglion cyst. On the other hand, the second hypothesis takes charge of invasion of ganglion cyst from the joint or surrounding tissue. However, the mechanism how the ganglion cyst penetrated into the nerve have not been thoroughly revealed.
Neural ganglia occurring in the foot and ankle are relatively rare and epineural ganglion has been reported even lesser than a ganglion cyst originated from intra-fascicular location8. For physicians, the location of ganglion is critical for treatment decision. If the ganglion is located within the nerve, complete resection of the cyst without causing damage to the nerve branch may be impossible. If the ganglion involves only the epineurium and doesn't have direct connection with the nerve fibers, excsion can be done safely.
In our case, the ganglion cyst of the posterior tibial nerve was multinodular and had no direct connection with the nerve. The patient was farmer and had history of repeated ankle sprains. It suggests that repeated minor injuries may induce cause an epineural ganglion cyst as second hypothesis mentioned above.
Though treatment of tarsal tunnel syndrome depends on the cause or physician's preference, surgical decompression is widely accepted as effective treatment nowadays910. If there is a space-occupying lesion in the tarsal tunnel, Surgical excision would be the best choice of treatment. Total resection of the lesion could be associated with sacrificing the nerve fibers, causing permanent neurologic deficit. Fortunately, the epineural ganglion cysts were not directly connected to the nerve fascicles, surgery could be performed without injury to the nerve fibers in this case. Thorough resection of the involved epineurium was necessary to reduce the recurrence rate because the cyst wall originate from the epineurium.
Figures and Tables
References
1. Singh SK, Wilson MG, Chiodo CP. The surgical treatment of tarsal tunnel syndrome. Foot. 2005; 15:212–216.

2. De Prado M, Cuervas-Mons M, Golanó P, Rabat E, Vaquero J. The tarsal tunnel syndrome. Fuß Sprunggelenk. 2015; 13:227–236.

3. Jerosch J, Schunck J, Khoja A. Results of surgical treatment of tarsal tunnel syndrome. Foot Ankle Surg. 2006; 12:205–208.

4. Cancilleri F, Ippolito M, Amato C, Denaro V. Tarsal tunnel syndrome: four uncommon cases. Foot Ankle Surg. 2007; 13:214–217.

5. Lee MF, Chan PT, Chau LF, Yu KS. Tarsal tunnel syndrome caused by talocalcaneal coalition. Clin Imaging. 2002; 26:140–143.

6. Alpar FK, Howell N, Masood I. Traumatic tarsal tunnel syndrome: the outcome of surgical decompression. Foot Ankle Surg. 2002; 8:41–44.

7. Suranigi S, Rengasamy K, Najimudeen S, Gnanadoss J. Extensive osteochondroma of talus presenting as tarsal tunnel syndrome: report of a case and literature review. Arch Bone Jt Surg. 2016; 4:269–272.
8. Fujita I, Matsumoto K, Minami T, Kizaki T, Akisue T, Yamamoto T. Tarsal tunnel syndrome caused by epineural ganglion of the posterior tibial nerve: report of 2 cases and review of the literature. J Foot Ankle Surg. 2004; 43:185–190.





 PDF
PDF ePub
ePub Citation
Citation Print
Print




 XML Download
XML Download