Abstract
The safety and feasibility of simple coil embolization and stent deployment for the treatment of posterior inferior cerebellar artery (PICA) aneurysms, as well as their radiologic and clinical results, have not been adequately understood. Especially, if dissecting aneurysm of proximal PICA is associated with small caliber PICA and stenosis of ipsilateral vertebral artery orifice (VAO), endovascular coiling with saving of PICA is not always easy. This 64-year-old man presented with subarachnoid hemorrhage due to a ruptured dissecting aneurysm of left proximal PICA. The aneurysm was irregularly fusiform in nature with a shallow PICA orifice (1.4 mm) and narrow caliber (0.9–1.5 mm). Moreover, the ipsilateral VAO showed severe stenosis (1.8 mm). We performed bifemoral puncture and chose additional route from right vertebral artery to left vertebrobasilar junction for retrograde approach and deployment of LVIS Jr. intraluminal support at proximal PICA. And then, the antegrade approach and coiling of aneurysm was done. Despite of transient thrombus of PICA, the aneurysm was successfully secured with preservation of whole PICA course. For preservation of narrow PICA with ipsilateral VAO stenosis, the contralateral approach and deployment of LVIS Jr. intraluminal support may be considered.
Aneurysms of the proximal posterior inferior cerebellar artery (PICA) are rare. There are many obstacles to surgical approaches for this location because of their deep anatomical location and close proximity to the brain stem and lower cranial nerves. As a result, endovascular treatment (EVT) is gaining popularity as an alternative to surgery. However, the results of endovascular repair of proximal PICA aneurysms are not well reported.7) Furthermore, the safety and feasibility of stent assist coil embolization of proximal PICA aneurysms with narrow caliber are not precisely known, including their radiologic and clinical results.5) The authors present a successful but challenging case of stent-assisted coil embolization of a ruptured left proximal PICA dissecting fusiform aneurysm with left vertebral artery orifice (VAO) stenosis using the contralateral vertebral artery (VA) approach for stenting and the ipsilateral VA approach for coil embolization.
A 64-year-old man without other past medical history presented to our emergency room (St. Vincent's Hospital) with decreased mental status. A Fisher grade IV subarachnoid hemorrhage due to a proximal PICA aneurysm rupture with hydrocephalus was revealed at initial brain computed tomography (CT) angiography (Fig. 1A). On neurologic examination, the Glasgow Coma Scale score was 9 (E2 V3 M4). A left proximal PICA fusiform dissecting aneurysm with a lacerated PICA orifice was found on cerebral angiography with 3D reconstruction (Fig. 1B–D). The shape of this fusiform aneurysm was triangular and irregular, and the size of the aneurysm was 3.95 mm (anterior/posterior diameter) × 3.12 mm (height) × 4.75 mm (length) with a shallow PICA orifice (1.3 mm). The diameter of the left PICA just proximal and distal to the dissecting aneurysm was 1.2 mm and 0.9 mm and acute angulation PICA with ipsilateral VA, respectively (Fig. 1E). Furthermore, the diameter of the left VAO was very narrow, approximately 1.8 mm (Fig. 1F), so an ipsilateral VA approach for intervention seemed more likely to arrest the flow and create other complications.
Our endovascular team decided to perform a stent-assisted coil embolization with a bilateral VA approach through bilateral femoral puncture. The left side femoral artery puncture was done and using a 6 F Shuttle (Shuttle-SL, Cook Medical, Bloomington, IN, USA), 6 F Envoy guiding catheter (Codman Neurovascular, Miami Lakes, FL, USA), right side VA was selected stably. The 90 degree Excelsior SL-10 microcatheter (Striker Corp., Fremont, CA, USA) was advanced to right vertebrobasilar junction (VBJ) with antegrade manner and then, to left VBJ with retrograde manner. From left PICA orifice, to avoid violation of ruptured aneurysm wall, extremely careful advancement of Traxcess microwire (MicroVention Inc., Tustin, CA, USA) was done sufficiently distal to PICA (Fig. 2A). With this stable guidance, the 90 degree Excelsior SL-10 microcatheter (Striker Corp.) was carefully advanced for future stent deployment (Fig. 2B). At the same time, through right femoral puncture, the left VA was accessed with a 5 F Davis catheter (Cook Medical, Bloomington, IN, USA). This 5 F catheter did not violated or block left VA blood flow. The straight shaped Excelsior SL-10 microcatheter (Striker Corp.) was cautiously advanced into mid-portion of ruptured aneurysm (Fig. 2C) and partial deployment of first coil was done. Through the contralateral approach, an LVIS Jr. stent (intraluminal support: MicroVention Inc., Tustin, CA, USA; 2.5 × 23 mm) was deployed very slowly. It covered and protected the left PICA, the aneurysm neck, and a short segment of the left VA. After confirmation of stable blood flow into left PICA, embolization was performed through an ipsilateral VA approach with 4 Target Nano detachable coils (Striker Corp.), sizes 2.5 × 6 cm, 2 × 4 cm, 2 × 4 cm, and 1.5 × 3 cm (Fig. 2D). Serial angiography revealed near-complete aneurysm occlusion and preservation of the PICA and VA flow, just before last coil insertion (Fig. 2E).
After placement of the last coil, the left PICA flow was arrested totally. To prevent this complication, systemic heparin (2,000 IU) was administered intravenously after first coil deployment. Probably, the last coil might elicit dense packing of aneurysm with partial compression of woven type LVIS Jr. stent with coil (Fig. 2F). The authors removed the last coil immediately and then, via the right VA route, through LVIS Jr. stent, selection of left PICA was done (Fig. 2G). A 1 mg intra-arterial bolus injection of tirofiban for 10 minutes dissolved the thrombus totally, and complete recanalization of the occluded left PICA was confirmed on final angiography (Fig. 2H, I). The patient received dual anti-platelet therapy with aspirin and clopidogrel immediately after the procedure. Post-procedure brain CT scan showed no definite ischemic lesion but continued hydrocephalus with intraventricular hemorrhage, the patient recovered gradually with extra-ventricular drainage.
Many articles have reported good angiographic outcomes of surgical clipping of proximal PICA aneurysms, but postoperative neurological deficits are not uncommon, as well.1) The lower cranial nerve paralysis, consequential aspiration pneumonia, and lateral medullary syndrome have been reported as postoperative complications of VA-PICA aneurysm surgery. The main obstacles to the surgical approaches to theses lesions are the jugular tubercle, the occipital condyle, and the lower cranial nerves.5) Therefore, EVT has more recently been considered the alternating treatment option for proximal PICA aneurysms. However, the PICA has a complex anatomy and a variable, tortuous course, and treatment of PICA lesions depends on the patency of the contralateral VA as well as the relationship between the VA lesion and the PICA origin.10) As a result, EVT of PICA aneurysms faces significant therapeutic challenges and has a high risk of VA-PICA thrombotic complication and occlusion. Since ischemic complications of the VA and PICA can lead to significant complications in the brainstem and cerebellum, precautions should be taken. If there are any signs of compromised PICA flow during and after the procedure, or if this situation is inevitable, sacrificing of the PICA could be a therapeutic option. However, long-term follow-up results of this catastrophic procedure are not well known and may have unexpected consequences.3) In order to maintain PICA patency in some cases, particularly where there are lesions of the VA-PICA or PICA orifice, endovascular stenting could be an option.4)
Multiple EVT techniques have been developed for adaptive occlusion of VA-PICA/PICA aneurysms with preservation of the VA-PICA flow,9) including the development of stent- or balloon-assisted techniques for treatment of wide-necked intracranial aneurysms, a retrograde approach via communicating arteries using a balloon or stent, the combined use of stent and balloon (“balloon-in-stent technique”) for fusiform aneurysms, “Y-stenting”, stenting with contralateral vertebral approach via the VBJ (“crossover technique”),8) and other techniques, such as pipeline flow diversion.6) Because of such a rapid development of various EVT techniques, indications for the use of EVT of PICA aneurysms have greatly expanded. In some cases, accessing the PICA in an antegrade approach through the ipsilateral VA is extremely difficult and risky due to multiple anatomical factors, such as VA-PICA angulation, severe hypoplasia of the ipsilateral VA, and severe stenosis of the ipsilateral VAO.3)8) In these situations, a contralateral VA approach with retrograde VBJ tracing to the ipsilateral PICA would be easier than the ipsilateral antegrade approach. A few case studies reported the “crossover technique” using the anterior or posterior communicating artery or the VBJ as an access route.3) This technique has many benefits but some disadvantages, including the potential risks associated with catheterization of a second major cerebral artery. The authors believe that, in our case, stent-assisted coil embolization would have been impossible without using the “crossover technique” due to an excessively narrow VAO size.
Recently, commonly available, self-expandable intracranial stents have become available for the treatment of posterior circulation aneurysms, and several studies recommended stent placement in small cerebral vessels less than 2 mm in diameter. However, the use of stent devices in small-diameter posterior circulation vessels of 2 mm in diameter is still controversial.4) There are some reports of stent use in cases with a small VA/PICA diameter Neuroform EZ stent (Stryker Neurovascular, Fremont, CA, USA) and the Enterprise stent (Codman Neurovascular, Raynham, MA, USA).2)3)8) LVIS Jr. stent application for a PICA fusiform aneurysm with a very shallow PICA orifice was rare, so the authors' trial with an LVIS Jr. stent with this complex anatomical case might be a meaningful attempt. That being said, this contralateral VA approach with stenting and ipsilateral VA approach with coil embolization has a high risk of thrombosis and parent artery occlusion due to narrow PICA patency and multiple device application. In this situation, PICA occlusion would have been inevitable, but long-term follow-up results of this procedure are not available. In particular, the size of the PICA is so variable that the issue of long-term stent patency remains controversial.3) Active thrombolysis is most important in this thrombolytic event. Another option in ipsilateral VAO stenosis would be an ipsilateral VA approach after creating a greater VA diameter with ipsilateral VAO stenting. But, in this type of approach, newly inserted VAO stent may hinder stable positioning of guiding catheter and may act as new thromboembolic source.
The EVT of a small-diameter PICA presents many procedural risks and challenges. The deployment of LVIS Jr. stent into a small-diameter PICA may be promising for patency maintenance, and retrograde VBJ tracing with a contralateral VA approach is a good option when multiple anatomical factors (especially ipsilateral VAO stenosis) act as obstacles.
Figures and Tables
Fig. 1
(A) The initial brain computed tomography scan shows acute subarachnoid hemorrhage on basal cistern with intraventricular hemorrhage. (B, C) The left vertebral angiography shows a left PICA dissecting fusiform aneurysm, measuring 3.95 mm (width) × 3.12 mm (height) × 4.75 mm (length). (D, E) The 3D volume rendering image shows shallow PICA orifice (1.3 mm) and narrow PICA just proximal and distal of aneurysm, giving rise to the PICA from the sac. (F) The left subclavian artery angiography shows severe stenosis of left vertebral artery orifice, about 1.8 mm (white arrow). PICA = posterior inferior cerebellar artery.
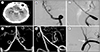
Fig. 2
The both vertebral angiography roadmap, via bifemoral puncture, enables Excelsior microcatheter from right VA to navigate left PICA, crossing aneurysm sac (A). The left VA angiography shows far distal, stable lodging of Excelsior microcatheter for future LVIS Jr. deployment (B). The both vertebral angiography roadmap shows another Excelsior microcatheter from left VA moving to fusiform aneurysm sac (C). The right VA angiography shows successful deployment of LVIS Jr intraluminal support from left VA, crossing aneurysm sac, to far distal PICA with preserved patency of PICA through contralateral VA approach (white arrow: proximal tip of deployed LVIS Jr., white dot arrow: distal tip of deployed LVIS Jr.) and left VA approach with microcatheter for detechable coil (black dot arrow: proximal tip of ipsilateral approached microcatheter for coil embolization, black arrow: distal tip of ipsilateral approached microcatheter for coil embolization) (D). Angiography shows near complete occlusion of aneurysm with preserved patency of PICA (E). After deployment of final coil, the left VA angiography revealed total thrombosis occlusion of left PICA (white arrow) (F). After reinsertion of right side microcatheter into proximal portion of PICA (through LVIS Jr. support), total 1 mg of tirofiban is injected. Rapid restroration of PICA flow is evident (G). Final angiography with 3D volume rendering image shows complete recanalization of left PICA with near obliteration of fusiform aneurysm (H, I). VA = vertebral artery; PICA = posterior inferior cerebellar artery.

ACKNOWLEDGEMENTS
We acknowledge that the material is not published previously and would like to thank the Department of Radiology of St. Vincent's Hospital, The Catholic University of Korea, Suwon, Korea.
References
1. Al-khayat H, Al-Khayat H, Beshay J, Manner D, White J. Vertebral artery-posteroinferior cerebellar artery aneurysms: clinical and lower cranial nerve outcomes in 52 patients. Neurosurgery. 2005; 56(1):2–10.

2. Cross DT 3rd, Moran CJ, Derdeyn CP, Mazumdar A, Rivet D, Chicoine MM. Neuroform stent deployment for treatment of a basilar tip aneurysm via a posterior communicating artery route. AJNR Am J Neuroradiol. 2005; Nov-Dec. 26(10):2578–2581.
3. Jeon SI, Kwon BJ, Seo DH, Kang HI, Park SC, Choe IS. Bilateral approach for stent-assisted coiling of posterior inferior cerebellar artery aneurysms - two cases. J Cerebrovasc Endovasc Neurosurg. 2012; 09. 14(3):223–227.

4. Kim MJ, Chung J, Kim SL, Roh HG, Kwon BJ, Kim BS, et al. Stenting from the vertebral artery to the posterior inferior cerebellar artery. AJNR Am J Neuroradiol. 2012; 02. 33(2):348–352.

5. Lv X, Jiang C, Li Y, Wu Z. Clinical outcomes of ruptured and unruptured vertebral artery-posterior inferior cerebellar artery complex dissecting aneurysms after endovascular embolization. AJNR Am J Neuroradiol. 2010; 08. 31(7):1232–1235.

6. Mazur MD, Kilburg C, Wang V, Taussky P. Pipeline embolization device for the treatment of vertebral artery aneurysms: the fate of covered branch vessels. J Neurointerv Surg. 2016; 10. 8(10):1041–1047.

7. Peluso JP, van Rooij WJ, Sluzewski M, Beute GN, Majoie CB. Posterior inferior cerebellar artery aneurysms: incidence, clinical presentation, and outcome of endovascular treatment. AJNR Am J Neuroradiol. 2008; 01. 29(1):86–90.

8. Roh HG, Chun YI, Choi JW, Cho J, Moon WJ, Solander S. Retrograde stent placement for coil embolization of a wide-necked posterior inferior cerebellar artery aneurysm. Korean J Radiol. 2012; Jul-Aug. 13(4):510–514.





 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download