Abstract
Neurosyphilis is an infection of the brain or spinal cord that is caused by the bacterium Treponema pallidum. Syphilitic myelitis, which involves the spinal cord, is a very rare form of neurosyphilis seen in patients with syphilis. It requires differentiation from other diseases of the spinal cord, including idiopathic transverse myelitis and spinal cord infarction. Herein, we describe the presentation and diagnosis of syphilitic myelitis in a 43-year-old woman, based on a flip-flop sign and candle guttering appearance depicted in magnetic resonance imaging and laboratory tests.
Neurosyphilis can occur at any time during the course of syphilis. Its early forms occur within the first few months or years following the infection. They affect the meninges or blood vessels, whereas the late forms occur years or decades later, and mainly affect the brain and spinal cord parenchyma (1). Syphilitic myelitis is a rare spinal cord infection caused by the bacterium Treponema pallidum (2). Although it may be difficult to distinguish spinal cord lesions from acute transverse myelitis, viral myelitis and spinal cord infarction, clinical findings and cerebrospinal fluid (CSF) abnormalities can assist in the diagnosis. Herein, we describe the diagnosis of a case of syphilitic myelitis by using magnetic resonance imaging (MRI) and laboratory tests.
The patient was a 43-year-old woman with mental disability and had exhibited impulsive pronunciation since childhood. Despite her disability, she was capable of managing her daily and work life well. Two days before coming to the hospital, she suddenly felt weakness in her left lower leg while climbing stairs. Although she had more strength in her right leg than the left one, her ability to walk was compromised. The day before she was admitted to the hospital, the feeling of weakness in her left lower leg worsened on waking up in the morning. The weakness progressed over time and she was unable to lift her left leg while lying down since that afternoon. These symptoms persisted and she visited the emergency room. There was no history of surgery or trauma to her back or legs. Physical examination revealed rigidity in her left leg. The motor function tests revealed a decrease in the elevation, extension, abduction and adduction of the left leg, knee flexion, knee extension, ankle plantar flexion and ankle dorsiflexion. The sensations of pain, touch and temperature below the right nipple (below T5 level) decreased, as well as the anal sphincter tone. The laboratory investigations revealed increased CSF IgG (38.55 mg/dL; normal range, 0.63–3.35 mg/dL) and CSF albumin (101.90-mg/dL; normal range, 13.4–23.7 mg/dL). She also tested positive (1:16) for CSF venereal disease research laboratory (VDRL) test and CSF fluorescent treponemal antibody (FTA) absorption IgG. The results of the polymerase chain reaction tests for the cytomegalovirus, herpes simplex virus and varicella zoster virus were all negative. The blood tests for T. palladium latex agglutination, FTA absorption IgG, VDRL (1:32) and VDRL rapid plasma reagin were all positive. The plain radiography did not reveal any specific findings other than spondylosis in the thoracic and lumbar spine. The T2-weighted axial MRI of the thoracic spine depicted a 1.6-cm ill-defined and heterogeneous low signal intensity lesion at the T6–T7 spinal cord level and in the intramedullary space (Fig. 1a). Edema throughout the thoracic spinal cord was depicted in the T2-weighted sagittal images (Fig. 1b). The T1-weighted axial and sagittal images depicted an iso-signal intensity lesion that could not be clearly visualized. The T1-weighted contrast-enhanced axial imaging depicted a round nodular enhancement, suggesting that the lesion was in contact with the superficial intramedullary space (Fig. 1c). The T1-weighted contrast-enhanced sagittal imaging depicted a half-moon nodular enhancement (Fig. 1d). No restriction was evident in the axial or sagittal diffusion-weighted MRI (Fig. 1e, f).
Syphilis is a sexually transmitted infectious disease caused by the spirochete bacterium T. pallaidum (2). It is divided into primary, secondary and tertiary stages according to its clinical course. In most cases, the central nervous system is only affected in the tertiary stage. Neurosyphilis occurs in one third of the patients who progress to the tertiary stage and in approximately 5–10% of untreated patients (3). Neurosyphilis is classified into early and late forms. In the early form, the spinal cord and mesodermal structure of the brain are invaded, while in the late form, the parenchyma is invaded (1). Syphilitic myelitis is a rare type of neurosyphilis. It is a form of meningo-vascular syphilis that is confined to the spinal cord (4). It is diagnosed via treponemal antibody tests, such as the VDRL, FTA absorption and TPH tests, which have high specificities but low sensitivity (27%) (56). Tashiro et al. (7) were the first to report MRI findings associated with syphilitic myelitis, in 1987. In their report, there was a high signal intensity in the short segment of the T2-weighted imaging of the thoracic spinal cord. Moreover, in the superficial part of the spinal cord, there was mainly an abnormal enhancement. Tsui et al. (4) reported non-specific MRI findings, including a diffuse high-signal lesion in the whole spinal cord in the T2-weighted imaging and discrete nodular enhancement located dorsally at the T8–T9 level of the spinal cord. Kikuchi et al. (8) reported MRI features of syphilitic myelitis, including the characteristic “flip-flop sign,” which is caused by abnormal enhancement of the parenchyma depicted as hypo-intensity in the T2-weighted imaging and a “candle guttering appearance” that is a superficial enhancement of the spinal cord parenchyma beneath the pia mater. Yuan et al. (9) reported MRI findings, which showed the characteristic “flip-flop sign.” Pandey (1) described a diffuse high-signal lesion with atrophy of the spinal cord at the thoracic level depicted through a non-enhanced MRI of the spinal cord. Such lesions in the spinal cord are thought to be caused by meningeal inflammation and spinal cord ischemia. They disappear completely with therapy, indicating that ischemic or inflammatory lesions are reversible (710). Therefore, given the lack of characteristic MRI findings, it is necessary to differentiate syphilitic myelitis from idiopathic transverse myelitis, spinal cord infarction, acute disseminated encephalomyelitis (ADEM) and intramedullary spinal cord metastasis. The characteristic MRI findings associated with idiopathic transverse myelitis include diffuse swelling and long-segment involvement of the spinal cord. The idiopathic transverse myelitis does not exhibit consistent enhancement. However, it sometimes exhibits patch enhancement. The spinal cord infarction is an elongated “pencil-like” lesion in the anterior spinal cord or a triangular lesion in the posterior spinal cord. Diffusion-weighted imaging depicts high signal intensity with low apparent diffusion coefficient values at the site of the lesion. ADEM is associated with swelling of the spinal cord and long-segment involvement, as is idiopathic transverse myelitis. However, it does not exhibit enhancement and can invade the brain. Intramedullary spinal cord metastasis is also associated with long-segment involvement of the spinal cord and may exhibit nodular enhancement. The identification of the primary cancer can assist in its diagnosis (11).
In the present case, the MRI findings were non-specific, with nodular enhancement at the thoracic spinal cord level and a diffuse high-signal lesion across the thoracic spinal cord level on the T2-weighted imaging. The abnormal intramedullary parenchymal enhancement was relatively reduced on the T2-weighted images, which showed the “flip-flop sign.” The T1-weighted enhanced imaging depicted superficial intramedullary enhancement, which was described as a “candle guttering appearance” at the T6–T7 spinal cord level. The diffusion-weighted imaging did not depict any restriction. These are considered as the characteristic findings of syphilitic myelitis.
In conclusion, we reported the MRI findings in the case of syphilitic myelitis, a rare form of neurosyphilis. Serum and CSF VDRL tests and MRI findings can be helpful in the diagnosis of syphilitic myelitis.
Figures and Tables
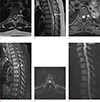 | Fig. 1Magnetic resonance imaging of the thoracic spine of a 43-year-old woman who experienced sudden weakness of the left lower leg while climbing stairs. The T2-weighted (a) axial and (b) sagittal images depicting high signal intensity lesions throughout the thoracic spinal cord level and heterogeneous low signal intensity lesions (arrows) at the T6–T7 spinal cord level. Superficial intramedullary enhancement (arrowheads), which shows a “candle guttering appearance”, can be seen in the enhanced fat-suppressed T1-weighted (c) axial and (d) sagittal images. The “flip-flop sign” (arrow and arrowhead) is seen, which shows that the abnormal enhancement is reduced on the T2-weighted images. The diffusion-weighted (e) axial and (f) sagittal images do not depict restriction. |
Acknowledgments
This study was supported by a 2018 research grant from Pusan National University's Yangsan Hospital in the Republic of Korea.
References
1. Pandey S. Magnetic resonance imaging of the spinal cord in a man with tabes dorsalis. J Spinal Cord Med. 2011; 34:609–611.

2. Dattner B, Thomas EW, De Mello L. Criteria for the management of neurosyphilis. Am J Med. 1951; 10:463–467.

3. Harris DE, Enterline DS, Tien RD. Neurosyphilis in patients with AIDS. Neuroimaging Clin N Am. 1997; 7:215–221.
4. Tsui EY, Ng SH, Chow L, Lai KF, Fong D, Chan JH. Syphilitic myelitis with diffuse spinal cord abnormality on MR imaging. Eur Radiol. 2002; 12:2973–2976.

5. Tien RD, Gean-Marton AD, Mark AS. Neurosyphilis in HIV carriers: MR findings in six patients. AJR Am J Roentgenol. 1992; 158:1325–1328.

6. MacLean S, Luger A. Finding neurosyphilis without the venereal disease research laboratory test. Sex Transm Dis. 1996; 23:392–394.

7. Tashiro K, Moriwaka F, Sudo K, Akino M, Abe H. Syphilitic myelitis with its magnetic resonance imaging (MRI) verification and successful treatment. Jpn J Psychiatry Neurol. 1987; 41:269–271.

8. Kikuchi S, Shinpo K, Niino M, Tashiro K. Subacute syphilitic meningomyelitis with characteristic spinal MRI findings. J Neurol. 2003; 250:106–107.

9. Yuan JL, Wang WX, Hu WL. Clinical features of syphilitic myelitis with longitudinally extensive myelopathy on spinal magnetic resonance imaging. World J Clin Cases. 2019; 7:1282–1290.





 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download