Abstract
Recently, digital health has gained the attention of physicians, patients, and healthcare industries. Digital health, a broad umbrella term, can be defined as an emerging health area that uses brand new digital or medical technologies involving genomics, big data, wearables, mobile applications, and artificial intelligence. Digital health has been highlighted as a way of realizing precision medicine, and in addition is expected to become synonymous with health itself with the rapid digitization of all health-related data. In this article, we first define digital health by reviewing the diverse range of definitions among academia and government agencies. Based on these definitions, we then review the current status of digital health, mainly in Korea, suggest points that are missing from the discussion or ought to be added, and provide future directions of digital health in clinical practice by pointing out certain key points.
Digital health has been popularized among both clinicians and patients. Accordingly, the World Health Organization (WHO) has announced a plan to create a department of digital health and has released a guideline on digital health intervention. However, definitions of digital health vary. First, the WHO digital intervention guideline states that digital health is rooted in eHealth, which uses Information and Communications Technology in support of health and health-related fields, and involves mobile health, which uses mobile wireless technologies for health. Therefore, the WHO guideline proposed the following definition of digital health: “a broad umbrella term encompassing eHealth (which includes mHealth), as well as emerging areas, such as the use of advanced computing sciences in ‘big data,’ genomics, and artificial intelligence.” In academic literature, digital health is defined as “the cultural transformation of how disruptive technologies that provide digital and objective data, accessible to both caregivers and patients, leads to an equal level doctor-patient relationship with shared decision-making and the democratization of care” [1], or “using digital tools to upgrade the practice of medicine to one that is high-definition and far more individualized” [2]. The US Food and Drug Administration (FDA) defined digital health as “The broad scope of digital health includes categories such as mobile health (mHealth), health information technology (IT), wearable devices, telehealth and telemedicine, and personalized medicine” [3].
Although there are various definitions of digital health from a variety of areas such as academia, government agencies, and international organizations, there is a common concept that covers all definitions: healthcare that utilizes new digital technologies. The current position of digital health with respect to other areas is illustrated in Fig. 1 [4]. Currently, there are medical areas that are not or cannot be digitalized, such as drug development and the wet-lab processes of genomic medicine. However, as technology advances, the role of digital health will gradually expand. A health IT company insisted that digital health will soon be synonymous with health. Furthermore, a newly established academic journal, NPJ Digit Med, stated in its first 2018 editorial, “Digital medicine, on its way to being just plain medicine” [2].
In this article, we review the current status of digital health, mainly in Korea. As in other countries, digital health is a major trend in Korea with a diverse range of synonyms such as smart health, ubiquitous health (u-Health), and medical artificial intelligence (AI). Interestingly, hospitals in Korea adopted hospital information systems much earlier than other countries [5]. Medical billing systems were popularized in the 1980s, order communication system (OCS) integrated with computerized physician order entry (CPOE), billing system, and simplified patient management system in the 1990s, electronic health record (EHR) and picture archiving and communication system (PACS) in the 2000s, and clinical data warehouse in the 2010s. Since Korea is one of the leading countries in digital health, the measures it has undertaken can assist in the adoption of digital health in other countries. Finally, we also suggest a future direction for realizing digital health.
Based on the rapid technological advancement and achievement of medical AI, current digital health is shifting focus from hospital information systems to medical AI. There have been numerous reviews or perspective articles on medical AI [6789101112131415161718], indicating that great efforts in this regard have been made in academia. Furthermore, numerous companies have attempted to implement commercial medical AI products. As a result, a diverse range of medical AI has been approved by the US FDA, European Union (EU) CE, and Korean Ministry of Food and Drug Safety (MFDS). More than 20 medical AI solutions have been approved by the US FDA, more than 17 have received EU CE markings, and 6 have been approved by the Korean MFDS.
The majority of the approved medical AI solutions target medical images in PACS. For example, all MFDS-approved medical AI solutions target computer-aided diagnosis (CAD) of radiology images. There are a number of reasons why medical image AI solutions have been popular: 1) medical images are better standardized than other clinical data due to PACS, which uses a Digital Imaging and Communications in Medicine (DICOM) standard, and 2) deep learning, such as convolutional neural networks, can analyze images proficiently. Only a few products that have been approved by the US FDA or EU CE, i.e., CardioLogs, AliveCor, and Apple, analyze electrocardiograms (ECG). CardioLogs developed 12-lead-ECG analysis software for the hospital setting, while AliveCor and Apple developed ECG analysis tools using wearables. Interestingly, ECGs are the most widely used data besides medical images, since ECGs are also better standardized than other medical data. Deep learning, such as recurrent neural networks, can also proficiently analyze such continuous signals. In Korea, there is also a diverse range of academic publications devoted to the analysis of ECG data by AI. A previous study predicted ventricular tachycardia one hour before onset [19]. Other studies predicted cardiac arrest using ICU patients' vital signs, including ECG [20]. This is a very promising approach since physicians can intervene to avoid fatal events. A substantial amount of real-time continuous monitoring data can be effectively used, not only for alerts but for other purposes as well.
Hurdles to the clinical adoption of digital health might be the issues of regulations and reimbursement. Since medicine deals with human life, there should a substantial number of regulations for patients' safety. This is unavoidable, and digital health companies should accept this situation. However, the problem is that most of the regulations do not align with digital health since they currently target traditional medical technologies, not digital health technologies. Regulatory bodies in each country are attempting to resolve this issue. For example, the US FDA released a digital health innovation action plan [3], including a digital health precertification program. Moreover, to support the effective implementation of digital health services, a Global Digital Health Partnership (GDHP) has been formed. The GDHP is a collaborative effort of 21 government agencies and the WHO regarding digital health in each country. Korea is one of the leading countries in digital health regulation, as shown, for example, by the Korean MFDS issuing the first medical AI software regulation guidelines in December 2017. Currently, the MFDS is developing more detailed medical AI guidelines.
The other major hurdle facing digital health in Korea is the issue of reimbursement. Korea has a single national insurance system. Unfortunately, reimbursement decisions by Korean government agencies take approximately one year. If a new digital health solution is categorized as an existing technology, then no additional fee applies to newly developed digital health technology. To date, all medical AI solutions for which application for reimbursement has been made have been categorized as existing technologies. Despite many experts' requests, the national insurance service (Health Insurance Review and Assessment Service, HIRA) does not have a plan to promote digital health technology using a reimbursement strategy. Due to the uniqueness of the Korean healthcare system (single government insurance system), this is a significant hurdle for digital health companies. The study results supported by HIRA emphasize 1) an additional retrospective or prospective study that is independent of MFDS approval, 2) a Randomized Control Trial (RCT), or 3) a cost-effectiveness study for reimbursement [21]. This is a scientifically appropriate approach; however, it is too strict.
Currently, medical AI for disease diagnosis is the most applicable component of digital health. However, digital health can be applied much more broadly in medicine, including clinical decisions of diagnosis or treatment, care management, and care delivery; for example, tele-medicine, remote patient monitoring, clinical trials, lifestyle management, in-patient care, hospital management, and drug discovery. However, much work remains to popularize digital health. For example, Topol mentions that 27 peer-reviewed articles compared the performance of AI to trained physicians, but only 4 articles were RCTs, which is the current gold standard in the medical field [17]. The necessity of RCTs will increase according to [21].
Back to the basic question, why do we need digital health? A substantial number of people have mentioned that digital health is an emerging market with immense potential. The digital health industry had reached a total value of 25 billion US dollar (USD) globally in 2017, and it could reduce healthcare costs by an estimated 7 billion USD per year in the US alone [22]. However, digital health is necessary not because of the market size but the fact that it can change the entire paradigm of health. All healthcare-related data are now being digitized, as indicated in Fig. 2. In the hospital setting, most hospitals use health information system (HIS) such as EHR, CPOE, and PACS, and laboratory information management system (LIMS). In the past, these data were created, stored, used, and archived on paper. Furthermore, the development of IT has allowed the generation of a substantial amount of patient-generated health data (PGHD) in everyday life, not in hospitals. These PGHD are collected using wearable devices or mobile health applications. There are many wearable/mobile devices to collect health-related data: 188 devices for fitness, 225 for lifestyle, and 88 for the medical domain [23]. In addition, the wearables target all possible body parts. Starting from the head to the feet, there are 84 devices for the head, 11 for the neck, 3 for the shoulder, 21 for the chest, 11 for the waist, 12 for the arm, 9 for the fingers, 26 for the torso, 14 for the legs, and 13 for the feet. There is thus a need to actively utilize PGHD, which can in particular provide insight into the management of health conditions including chronic illness management, not acute care.
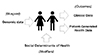
As medicine continues to develop, people are now living longer than ever. Korea was classified as an aging society in 2018, and is experiencing much faster population aging than any other Organization for Economic Cooperation and Development (OECD) country. To assist the elderly, digital health technologies should be actively adopted. All health data, including PGHD, should be integrated. As indicated in Fig. 3 [24], genomic data are the blueprints of human health, but despite their importance, extensive research is needed to explain the genetic associations of human health. Social determinants of health (SDOH) are modifiers of these blueprints, as they can modify the human genome through somatic mutation, and thus heavily affect health conditions—where to live, what to eat, and so on. Clinical data and PGHD are outcomes of health conditions. Fortunately, we can decode the human genome and collect SDOH, PGHD, and clinical data using digital technologies. Therefore, digital health will allow all the necessary data to be integrated and analyzed.
For this purpose, the current healthcare system should be transformed to a learning healthcare system [25]. A learning healthcare system is defined as one in which “science, informatics, incentives, and culture are aligned for continuous improvement and innovation, with best practices seamlessly embedded in the delivery process and new knowledge captured as an integral by-product of the delivery experience [26].” From the perspective of digital health, digitalized data can accelerate this process. Thus, physicians should undertake life-long learning of new technologies. Furthermore, researchers should research the issue of digital health literacy for patients. Currently, the digital divide is the source of certain social problems. If all data or information on health are stored digitally, those who can easily utilize these data and those experiencing problems in accessing them could have very different health conditions.
However, the reliability and safety of digital health technologies must be carefully assessed. As stated in the previous section, digital health targets human life. The agile techniques mainly used in the IT field, as in software development, cannot be applied in medicine. “Agile” means characterized by the division of tasks into short phases of work and frequent reassessment as well as adaptation of plans. In software development, bugs only create an inconvenience to users; on the other hand, in digital health development, bugs can harm or even kill the patients. We should design a new mechanism to evaluate digital health solutions. Unfortunately, no reliable mechanism exists to identify validated digital health solutions [27]. As discussed by Mathews and colleagues [27], such validation can be divided into technical (performance accuracy), clinical (outcome improvement), and system validation (health IT system integration). This provides a conceptual framework for evaluating digital health products. Similarly, Stanford published the “Statement of Guiding Principles for Ethics in Digital Health” in February 2019, in which are proposed 10 principles, of which reliability, safety, and ethics could be more important than performance.
The digitalization of healthcare data has supported the generation of immense amounts of healthcare data that should transform traditional medicine. Therefore, medicine has to become a data science and doctors should be data scientists to handle digital healthcare data. For this purpose, three factors are important such as data standardization, explainable AI, and AI ethics. Great efforts have been devoted to all three of these topics. A diverse range of standards on health data have been published or are being developed. For example, in the most representative standard development organization (SDO), the International Organization for Standardization Technical Committee (ISO/TC) 215-Health Informatics, has published 188 standards and is developing 59 more. Other SDOs such as HL7, SNOMED, Logical Observation Identifiers Names and Codes (LOINC), and DICOM have also published a substantial number of standards. For explainable AI, a diverse range of research projects, including an Explainable Artificial Intelligence (XAI) project [28] funded by the US Defense Advanced Research Project Agency (DARPA), are ongoing and a substantial body of papers has been published [2930].
A digital health industry is also important. Without industry support, digital health cannot be realized. Therefore, government regulation or support is crucial, especially in the circumstances of the unique insurance system of Korea. As discussed in the previous section, medical AI software should be reviewed within a rigid scientific setting. However, Software as a Medical Device (SaMD), including medical AI, is non-invasive technology with minimal risk for patients. In addition, CAD or a Clinical Decision Support System (CDSS) does not make the final decision. Only physicians can make a clinical decision, even if with the help of an IT system. Therefore, less rigid criteria can be set than in the case of invasive medical devices or drugs. Interestingly, HIRA has a history of promoting health IT through a reimbursement plan. In 1999, HIRA started to reimburse digitalized medical images created using a PACS to speed the adoption of PACS. This approach significantly contributed to the rapid and wide adoption of PACS in Korea. As a result, 99% of tertiary hospitals in Korea use PACS. Similarly, HIRA promoted an electronic medical claim system and a Drug Utilization Review (DUR) system using a reimbursement strategy.
Finally, AI is the key component of current digital health. When discussing medical AI, we have to keep in mind the American Medical Association policy recommendation statement. AI in medicine is not Artificial Intelligence in medicine, but Augmented Intelligence in medicine. This means that in medicine, the intention of AI is not to replace human doctors. The future of digital health relies on our imagining a new practice of medicine [31].
Digital health includes the emerging health technologies that apply digital technologies, and soon will become health itself. Furthermore, digital health is an unavoidable trend in realizing precision medicine. We should carefully discuss, develop, and apply digital health in clinical practice.
Figures and Tables
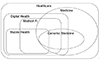 | Fig. 1Relationship between digital health and other terms.Modified from Choi YS. 2019 [4] with permission. AI, artificial intelligence.
|
ACKNOWLEDGEMENTS
This work was supported by the Technology Innovation Program (20004632, Development of industrial platform utilizing artificial intelligence analysis based on genomes) funded By the Ministry of Trade, Industry & Energy (MOTIE, Korea). I would like to thank Editage (www.editage.co.kr) for English language editing.
References
1. Meskó B, Drobni Z, Bényei É, Gergely B, Győrffy Z. Digital health is a cultural transformation of traditional healthcare. Mhealth. 2017; 3:38.

2. Steinhubl SR, Topol EJ. Digital medicine, on its way to being just plain medicine. NPJ Digit Med. 2018; 1:20175.

3. Digital health innovation action plan. U.S. Food & Drug Administration. 2019; 8.
4. Choi YS. Digital healthcare: the future of medicine. Seoul: Cloud9;Forthcoming 2019.
5. Kim CY, Kang G, Lee JS, Kim BY, Kim YI, Shin Y. Introduction and the current status of hospital information systems. J Korean Soc Med Inform. 1999; 5:27–35.

6. Payne PRO, Bernstam EV, Starren JB. Biomedical informatics meets data science: current state and future directions for interaction. JAMIA Open. 2018; 1:136–141.

7. Shortliffe EH, Sepúlveda MJ. Clinical decision support in the era of artificial intelligence. JAMA. 2018; 320:2199–2200.

8. Goldhahn J, Rampton V, Spinas GA. Could artificial intelligence make doctors obsolete? BMJ. 2018; 363:k4563.

9. Maddox TM, Rumsfeld JS, Payne PRO. Questions for artificial intelligence in health care. JAMA. 2019; 321:31–32.

11. Saria S, Butte A, Sheikh A. Better medicine through machine learning: what's real, and what's artificial? PLoS Med. 2018; 15:e1002721.

12. Challen R, Denny J, Pitt M, Gompels L, Edwards T, Tsaneva-Atanasova K. Artificial intelligence, bias and clinical safety. BMJ Qual Saf. 2019; 28:231–237.

13. Medicine in the digital age. Nat Med. 2019; 25:1.
14. Norgeot B, Glicksberg BS, Butte AJ. A call for deep-learning healthcare. Nat Med. 2019; 25:14–15.

15. Gottesman O, Johansson F, Komorowski M, Faisal A, Sontag D, Doshi-Velez F, Celi LA. Guidelines for reinforcement learning in healthcare. Nat Med. 2019; 25:16–18.

16. He J, Baxter SL, Xu J, Xu J, Zhou X, Zhang K. The practical implementation of artificial intelligence technologies in medicine. Nat Med. 2019; 25:30–36.

17. Topol EJ. High-performance medicine: the convergence of human and artificial intelligence. Nat Med
. 2019; 25:44–56.

19. Lee H, Shin SY, Seo M, Nam GB, Joo S. Prediction of ventricular tachycardia one hour before occurrence using artificial neural networks. Sci Rep. 2016; 6:32390.

20. Kwon JM, Lee Y, Lee Y, Lee S, Park J. An algorithm based on deep learning for predicting in-hospital cardiac arrest. J Am Heart Assoc. 2018; 7:e008678.

21. Park SH, Do KH, Choi JI, Sim JS, Yang DM, Eo H, Woo H, Lee JM, Jung SE, Oh JH. Principles for evaluating the clinical implementation of novel digital healthcare devices. J Korean Med Assoc. 2018; 61:765–775.

22. Duggal R, Brindle I, Bagenal J. Digital healthcare: regulating the revolution. BMJ. 2018; 360:k6.

23. Kourtis LC, Regele OB, Wright JM, Jones GB. Digital biomarkers for Alzheimer's disease: the mobile/ wearable devices opportunity. NPJ Digit Med. 2019; 2:9.

24. Park YR, Shin SY. Status and direction of healthcare data in Korea for artificial intelligence. Hanyang Med Rev. 2017; 37:86–92.

25. Budrionis A, Bellika JG. The learning healthcare system: where are we now? a systematic review. J Biomed Inform. 2016; 64:87–92.

26. Institute of Medicine. A continuously learning health care system. In : Smith M, Saunders R, Stuckhardt L, editors. Best care at lower cost: the path to continuously learning health care in America. Washington (DC): National Academies Press (US);2013. p. 136.
27. Mathews SC, McShea MJ, Hanley CL, Ravitz A, Labrique AB, Cohen AB. Digital health: a path to validation. NPJ Digit Med. 2019; 2:38.

28. Gunning D, Aha DW. DARPA's explainable artificial intelligence (XAI) program. AI Mag. 2019; 40:44–58.

29. Adadi A, Berrada M. Peeking inside the black-box: a survey on explainable artificial intelligence (XAI). IEEE Access. 2018; 6:52138–52160.

30. Towards trustable machine learning. Nat Biomed Eng. 2018; 2:709–710.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download