Abstract
Infection of the hands is a relatively common disease that can occur after the injury of the fingers. Commonly, these common diseases can be treated with empirical antibiotic therapy within accurate and detailed information from their patients. But, some health care providers often simply think about this disease as simple infection and inflammation and just prescribe the empirical antibiotics without precise medical examination. Depending on the source of the infection, some patients will not readily fit into the standard antibiotic regimens that are commonly used for community pathogen. If accurate diagnosis within early treatment is delayed, it will cause the complications such as tenosynovitis, osteomyelitis and necrotizing fasciitis. By way of example, we describe the rare case of critically exacerbated from simple laceration to tenosynovitis caused by Shewanella algae whose infection was related to his initial injury and not the subsequent treatment.
Infection of the hands is a relatively common disease that can occur after the injury of the fingers. Commonly, these common diseases can be treated with empirical antibiotic therapy within accurate and detailed information from their patients. But, some health care providers often simply think about this disease as simple infection and inflammation and just prescribe the empirical antibiotics without precise medical examination. However, hand infections are one of the few surgical emergencies for hand surgeons and account for up to 35% of patients who treated to hand surgery1. If accurate diagnosis within early treatment is delayed, it will cause the complications such as tenosynovitis, osteomyelitis, and necrotizing fasciitis. The progression of this disease may be more severe in children with weakened immune system. Generally, Staphylococcus aureus had been reported to cause up to 80% of hand infections123. Although, S. aureus is the most common culprit of hand infection, it is helpful to consider the etiology of the infection and associate it with the possible offending microbial organism. Depending on the source of the infection, some patients will not readily fit into the standard antibiotic regimens that are commonly used for community pathogen4. By way of example, we describe the rare case of critically exacerbated from simple laceration to tenosynovitis caused by Shewanella algae whose infection was related to his initial injury and not the subsequent treatment, as well as a pertinent literature review.
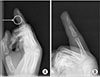
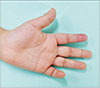
A 6-year-old boy who was healthy and never had undergone any disease was admitted with infection of his index finger. He was slipped down on the beach and got simple lacerative wound on his finger. After the injury, he was treated his finger by primary repair with the laceration and empirical antibiotics at local clinic. Although, the treatment was maintained during 4 days with simple dressing, his finger was exacerbated and seemed to be cellulitis on his finger. Five days after the initial treatment he developed pain, swelling, and redness of his index finger with small multiple blisters. When he transferred to our department for management, induration accompanied by yellowish turbid discharge progressed from fingertip to proximal phalanx of his index finger (Fig. 1). On admission, he had temperature of 37.7℃ and appeared irritable. Tenderness along the course of flexor sheath and symmetric swelling of the index finger was shown and the finger was held in a slightly flexed position. The patient experienced severe pain with active and passive flexion and extension. Flexion and extension within distal-interphalangeal joint were limited. Blood cultures, a full blood count and a wound microbiology swab were taken and he was promptly commenced on intravenous cefotaxime, analgesia, hand elevation, immobilization, and general bed rest. Radiologic inspection was carried out to confirm the presence of minute foreign body. There was tiny radiopaque densities seen as foreign body (Fig. 2). We performed wound irrigation with focal surgical debridement for removal of foreign bodies and minute debritic tissues. Foreign bodies were uncertain, but seemed like sands or seashell. The full blood count showed minor leukocytosis (11.1×109/L). There was no growth in the blood cultures. The Gram stain of the culture revealed gram-negative bacteria. The organisms grown from the tissue culture included S. algae. S. algae was sensitive to piperacillin, cefotaxime, ciprofloxacin, and resistant to amoxicillin and cefazolin. He responded well to the treatment and was discharge after 12 days of hospitalization (Fig. 3).
Hands, especially fingers, are a part of the body that people use most in their activities and are always exposed to the risk of injury and infection. A variety of causes can result in hand injuries, which can lead to the inflow of a wide variety of bacteria and the resulting infection. Hand infections are common with diverse factors; however, most are the result of direct inoculation of bacteria from penetrating trauma and lacerations567. It is important to have a high index of suspicion to diagnosis and treat hand infections expeditiously in order to prevent morbidity and maximize outcomes. If diagnosis within early treatment is delayed, it will cause the complications such as tenosynovitis, osteomyelitis, and necrotizing fasciitis. The progression of this disease may be more severe in children with weakened immune system. If the wound is worse as a complication, not a simple inflammation, surgical treatment may be necessary and may result in sequelae. In general, most of the causes of hand infection are Staphylococcus and Streptococcus species. Because it is often treated with the use of empirical antibiotics in combination with simple dressing, health care providers often consider easy and miss the golden time of treatment, often causing wounds to worsen. Especially for children, they have a weaker immune system than adults and infection can proceed easily. That is why health care provides should be able to think about the precise etiology of the infection and causes of injury. If necessary, it should be able to perform surgical debridement and bacterial examination to find the culprit of the infection rather than simple wound disinfection.
The diagnosis of flexor tenosynovitis is based on the presence of 1 or more of the 4 cardinal signs of Kanavel and then confirmed by microbiologic or histopathologic evaluation when possible. In this report, the patient showed all Kanavel signs.
S. algae is a facultative anaerobic, aquatic, gram-negative bacillus belonging to the family Vibrionaceae8. This species was first reported by Derby and Hammer9 in 1931 after being isolated from putrefied butter. This microorganism was named after Dr. James Shewan for his contributions to fishery microbiology10. Shewanella can find commonly in nations, but most found in marine environments.
Shewanella was initially termed Achromobacter putrefaciens before being reclassified as a member of the Pseudomonas family11. S. algae was also initially misidentified by phenotypic tests as Shewanella putrefaciens; correct identification relied on 16S RNA gene sequence analysis establishing a novel species in the early 199012. S. algae infections are only infrequently associated with human disease. When it is occur, those infections are most commonly due to S. algae as opposed to other Shewanella spp.11. S. algae infections range from superficial abscess, cellulitis, osteomyelitis, and bacteremia to necrotizing fasciitis11. In warm temperature including United States, South Africa, Australia, Asia, and Southern Europe, the prevalence of Shewanella infections is higher and most infections are related to contact with seawater11.
Although Shewanella species infections in humans are rare, the number of reports has significantly increased recently. In 2013, two extensive studies from Liu et al13. and Vignier et al14. were reported. In 2017, retrospective analysis of the infections of S. algae from Martín-Rodríguez et al15. were reported. These studies suggested that the manifestations of the infection of S. algae can be shown variously such as serious soft tissue infections, otitis media, spondylodiscitis, and necrotizing fasciitis. According to Fluke et al.16, pyogenic flexor tenosynovitis by S. algae has a high risk for poorer outcome if not treated. This study reported S. algae infection appears to be a much more virulent than other marine bacterium and poorer prognosis. Thus, to minimize occurring complication or morbidity, the distinction between infection by S. algae and other pathogens must be quickly when a patient presents with flexor tenosynovitis after water exposure.
As mentioned above, S. algae infections are rarely to human being, but can induce critical complication such as necrotizing fasciitis and has poor prognosis. Inadequate and delayed treatment are correlated with increased mortality. In our case, young healthy individual had undergone injury and seawater exposure. Because of its poor prognosis and high virulence, physicians should consider S. algae infections in patients with tenosynovitis to treat and minimize morbidity appropriately, especially after seawater exposure.
Figures and Tables
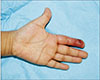 | Fig. 1A 6-year-old boy with tenosynovitis on left index finger. Immediate image on his admission. Raw surface accompanied by diffuse induration with swelling and yellowish turbid discharge. |
References
1. Tosti R, Ilyas AM. Empiric antibiotics for acute infections of the hand. J Hand Surg Am. 2010; 35:125–128.

2. McDonald LS, Bavaro MF, Hofmeister EP, Kroonen LT. Hand infections. J Hand Surg Am. 2011; 36:1403–1412.

3. Osterman M, Draeger R, Stern P. Acute hand infections. J Hand Surg Am. 2014; 39:1628–1635. quiz 1635.

4. Jacob-Kokura S, Chan CY, Kaplan L. Bacteremia and empyema caused by Shewanella algae in a trauma patient. Ann Pharmacother. 2014; 48:128–136.

5. Fowler JR, Ilyas AM. Epidemiology of adult acute hand infections at an urban medical center. J Hand Surg Am. 2013; 38:1189–1193.

6. Houshian S, Seyedipour S, Wedderkopp N. Epidemiology of bacterial hand infections. Int J Infect Dis. 2006; 10:315–319.

7. Türker T, Capdarest-Arest N, Bertoch ST, Bakken EC, Hoover SE, Zou J. Hand infections: a retrospective analysis. PeerJ. 2014; 2:e513.

8. MacDonell MT, Colwell RR. Phylogeny of the Vibrionaceae, and recommendation for two new genera, Listonella and Shewanella. Syst Appl Microbiol. 1985; 6:171–182.

9. Derby HA, Hammer BW. Bacteriology of butter. IV, bacteriological studies on surface taint butter. Ames: Agricultural Experiment Station, Iowa State College of Agriculture and Mechanic Arts;1931.
10. Hau HH, Gralnick JA. Ecology and biotechnology of the genus Shewanella. Annu Rev Microbiol. 2007; 61:237–258.

11. Janda JM, Abbott SL. The genus Shewanella: from the briny depths below to human pathogen. Crit Rev Microbiol. 2014; 40:293–312.
12. Nozue H, Hayashi T, Hashimoto Y, et al. Isolation and characterization of Shewanella alga from human clinical specimens and emendation of the description of S. alga Simidu et al., 1990, 335. Int J Syst Bacteriol. 1992; 42:628–634.

13. Liu PY, Lin CF, Tung KC, et al. Clinical and microbiological features of shewanella bacteremia in patients with hepatobiliary disease. Intern Med. 2013; 52:431–438.
14. Vignier N, Barreau M, Olive C, et al. Human infection with Shewanella putrefaciens and S. algae: report of 16 cases in Martinique and review of the literature. Am J Trop Med Hyg. 2013; 89:151–156.





 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download