Background
Ethics is a generic term dealing with diverse ways of considering and understanding moral life. Morality refers to a system of ideas with regard to right and wrong human conduct that is so widely shared, albeit incomplete, that it constitutes a stable social agreement. Professional morality is a particular type of morality that includes moral codes of practice. The ethics of a profession comprises the obligations determined by the accepted role of professionals [
1].
As occupational health (OH) professionals, the role of occupational physicians (OPs) is to protect and promote workers’ health and working ability; this role varies among countries depending on national legislation and the relationships among employers, employees, and the general public [
2,
3]. Responsibilities to these parties may conflict. For example, ethical problems are most likely to arise if one party does not perceive that the OPs have other responsibilities [
4]. Some ethical codes have been produced by professional societies and organizations for OPs [
4–
8], and provide guidance on what is considered right or wrong in terms of practice [
9]. However, these do not cover the ethical conflicts facing OPs in Korea, due to the limited ability to extend specific approaches beyond general ethics to consider Korean contextual issues.
Despite this, there have been few studies on the necessity of an ethical code for Korean OPs with respect to the ethical conflicts faced, solutions employed, knowledge of the ethical code, and attitude toward implementation of ethical principles. Only one survey of 107 Korean OPs on perception of ethical issues during their practice was conducted in 2010. OH practice is constantly changing and OPs need guidelines to address new ethical challenges. Therefore, this study aimed to investigate the ethical conflicts, the practical resolutions, the ethical principles, and core professional values for the Korean OPs.
Discussion
Medical professionalism is the promise and duty of a professional group of physicians to fulfill social expectations based on a social contract, and can also be a belief in the need for professional behavior under social regulation [
14]. A society expects the medical profession to fulfill their guarantee of competence, altruism, morality, truthfulness, promotion of public benefit, transparency, accountability, and self-regulation, as opposed to granting autonomy and providing exclusive rights. Because the medical profession is responsible for duties necessary to society, the standard required is high both practically and morally [
15,
16]. In other words, medical professionalism is based on expertise and ethics and on the premise that professional autonomy as a physician exists within a professional standard and code of ethics [
17]. Because OPs have complicated relationships with employees, employers, and the general public, they may have simultaneous obligations towards a third party, which could lead to adverse effects and ethical conflicts [
18]. In this context, ethical consideration during OH practice is regarded as an important core competency for OPs [
2,
11,
19,
20]. As a result, many countries establish and improve their own ethical code in accordance with their circumstances [
4,
6–
8].
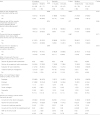
This study showed that Korean OPs, 91.3% of specialists and 63.4% of residents (70% of senior residents), experienced many work-related ethical conflicts; these percentages are likely due to differences in levels of authority and responsibility between specialists and residents. Many respondents experienced ethical conflicts with employees and employers during OH examinations and evaluations of fitness for work. Korean OPs conduct OH examinations and industrial healthcare management in SMEs based on the Occupational Safety and Health Acts [
21]; as such, Korean OPs are closely connected with the Ministry of Health and Welfare and the Ministry of Employment and Labor. Moreover, as their customers are commonly not patients but healthy employees and most OPs are hired instead of being in private practice, decision-making processes usually involve consultation with all parties concerned [
22]. Many respondents claimed that they experienced ethical conflicts with related parties during decision-making for work-related diseases (especially with workers diagnosed with an occupational disease, D1). Also specialists had more frequent conflicts with employers than residents, likely because specialists have more responsibilities and contact with employers, such as in industrial healthcare management and OH examinations. Specialists resolve such conflicts through their personal beliefs and consultation with colleagues, while residents mostly do so with colleagues; few respondents used available ethical codes. This differed from the studies by Brandt-Rauf’s in American OPs, in which 22% of respondents ‘always’ and 33% ‘frequently’ resolved ethical conflicts using professional codes of ethics [
13]. Thus, professional codes of ethics can assist in resolution of ethical conflicts during OH practice. In this study, 81% of specialists and 76.1% of residents recognized the necessity for a code of ethics for OPs in Korea, particularly those more experienced. Additionally, those with more experience also tended to more frequently agree that systematic training for ethical decision-making and a higher sense of ethics are needed for OPs, compared with other physicians.
Most of the participants experienced ethical conflicts at work, but few were aware of other codes of ethics for OPs. The level of recognition was not significantly different from that of a survey performed in 2010 [
10]. This may be because many Korean OPs resolve ethical conflicts based on their personal beliefs and consultation with an experienced colleague. However, the study by Aw of recognition of ethical codes involving OPs from the UK, the Netherlands, and Singapore reported that all but one of the physicians were unaware of codes formulated by organizations outside of their own country [
9]; it is thus possible that Korean OPs believe that ethical codes from other countries are not relevant to the Korean context. Also, compared with national guidelines targeting OPs in the country of origin, such as the Guidance on Ethics for Occupational Physicians by the UK Faculty of Occupational Medicine [
7] or the Code of Ethics for the Practice of Industrial Hygiene by ACGIH in the United States [
8], the International Code of Ethics for Occupational Health Professionals by the ICOH, which targets international OPs [
5], was recognized by only 20% of the participants in this study. This may be because the general description and instructions for each ethical principle are inadequate to resolve ethical conflicts in practice. Indeed, the American Medical Association Code of Medical Ethics sets out in detail the ethical and legal problems physicians may face [
23], and the British Medical Association’s Medical Ethics Today provides a detailed explanation and common cases of ethical problems [
24]. Therefore, a suitable Korean ethical code for OPs is required.
The four core professional values, ‘consideration of workers’ health and safety’, ‘neutrality’, ‘effort to maintain expertise’ and ‘maintenance of professional independence’, did not differ from the configuration items in Kim’s study [
10], except for ranking; specifically, OPs in Korea regarded the following to be important obligations: 1) to protect worker’s health, respect their human dignity, and maintain their well-being; 2) to judge based on scientific knowledge and fact, and refrain from any judgment and action against integrity and impartiality; 3) to continue to develop competence, be aware of scientific/technical knowledge, and aim to achieve the best recognized standard of quality; and 4) not be affected by a conflict of interest in any situation during judgment and decision-making [
5,
25,
26].
Compared with Martimo’s study, in which ‘expertise’ and ‘confidentiality’ were selected as the core ethical characteristics of OH, our results differed [
12]. Confidentiality, a key factor in several ethical codes [
4–
8], is defined as the protection of medical data. Disclosure and transmission of medical information should be controlled by national laws or regulations and ethical codes for medical practitioners [
5]. Confidentiality is supposed to be strictly guaranteed in OH practice; however, it is not an absolute principle [
27]. OPs have dual (or multiple) loyalties; thus, they are put in the position of assessing the risk-benefit of all parties concerned. As such, it is inevitable that OPs are concerned over what and how much information should be provided. Korean OPs judged confidentiality to be of low importance in this study, possibly due to cultural differences. A specialist responded to an open-ended question that he experienced a conflict with the confidentiality of workers’ medical information when he reported to the employer. Thus, more attention should be paid to confidentiality.
Residents and specialists with >10 years’ experience selected neutrality as their first and second choices, respectively. However, neutrality was ranked fourth by specialists with ≤10 years’ experience. This could reflect their priorities but could also be due to confusion over the concepts of neutrality and independence. A limitation of this study was that these terms were not defined in the survey.
The mock cases enable identification of the ethical principles used by Korean OPs in practice. The four-principle (beneficence, nonmaleficence, respect for autonomy, and justice) approach to biomedical ethics by Beauchamp and Childress is widely accepted in current biomedical theory [
28]. The principles of nonmaleficence (to do no harm to others) and beneficence (to provide benefit) have been important in medical ethics from ancient times. However, the principles of respect for autonomy (the right of self-determination) and justice (fair distribution of benefit, risk, and cost) have emerged since the mid-twentieth century. This is because decision-making has been progressively transferred from the physician to the patient, and the distribution of medical resources has become an important issue [
1,
15].
The principle of beneficence and justice were selected for assessment of fitness for work (cases 1, 4, and 5) and confidential information acquired while on duty (cases 3, 7, and 8). As assessment of fitness for work aims to ensure that workers are in an occupational environment appropriate for their psychological and physical capability; OPs judge whether a worker’s health is suitable. Ethical conflicts can occur in this process because the worker and employer may have different perspectives. OPs can also experience ethical conflicts due to their having multiple loyalties. For example, OPs have revealed that a hazardous material has been used or an event has been harmful to the health of the worker or the general public. In this study, many OPs acted from the perspective of beneficence, especially paternalism, which is intentional intervention in another person’s preference or actions with the purpose of either preventing or reducing harm to or benefiting that person. This was because Korean OPs already operate within a social context that takes good deeds for workers and public health for granted.
In terms of a pre-placement examination, beneficence was preferred in case 6, and respect for autonomy in case 2. Pre-placement examination is an assessment of fitness for work based on the health condition of the individual, the job description, and harmful factors [
29]. There can be a conflict between the right to work (respect for autonomy) and health (beneficence). In case 2, both specialists (61.3%) and residents (56.3%) chose respect for autonomy as the preferred ethical principle. As the second choice, beneficence (30.0%) was chosen by specialists, and beneficence (21.1%) and nonmaleficence (12.7%) by residents. Nonmaleficence is a passive duty to do no harm to others, while beneficence actively promotes and preserves health [
15]. The difference is likely due to the different responsibilities of specialists and residents.
This is the first study of supplication of four moral principles to resolve ethical conflicts. According to Westerholm, it is necessary to clarify the facts needed for a decision, to identify which of the ethical values mentioned above are involved, and to confirm whose interests are concerned and the consequences of an action by the OP [
30]. This study revealed the preferred ethical values of Korean OPs. Further studies are required to assess the contributions and limits of the ethical principles.
Some of the items can be understood differently due to the absence of ethical training for Ops and ambiguity of the ethical terms between ‘neutrality’ and ‘maintenance of professional independence’. The numerator of the response rate could be identified because information on the name, age, year acquired (for specialists), and grade of residency (for residents) were available. However, we were unable to confirm the denominator of total contacted persons, due to the three surveys used, personal information protection, and the potential for duplication among the three survey methods (e.g., sending an email to several alumni associations through administrators, attendance at the annual autumn meeting of Korean Association of Occupational and Environmental Clinics, and survey via the online community). The inability to calculate the response rate is a weakness of this study. However, this approach enabled collection of a more diverse range of opinions.








 PDF
PDF Citation
Citation Print
Print



 XML Download
XML Download